A Rare Presentation of Ocular Tuberculosis: A Case Report
Ashutosh*
Department of Ophthalmology, SS Institute of Medical Sciences, India
Submission: August 24, 2017; Published: September 22, 2017
*Corresponding author: Ashutosh, Department of Ophthalmology, SSIMS and RC Davangere-577005, karnataka, India, Tel: 919901727048; Email: ashu02ashutosh29@gmail.com
How to cite this article: Ashutosh. A Rare Presentation of Ocular Tuberculosis: A Case Report. 2017; 5(1): 555653. DOI: 10.19080/JOJO.2017.05.555653
Introduction
Tuberculosis is a serious infectious disease that affects about a third of the world population [1,2]. Ocular tuberculosis is a rare but known complication of tuberculosis [3]. Ocular TB is re- emerging as a major challenge all over the world [4]. This disease can involve any tissue of the eye and the orbit. Ocular involvement can occur through either direct entry or as an immunological reaction to the organism. The occurrence is more common in immune compromised individual. The organism can enter the eye from both the epithelial and the haematogenous route. The latter being the favourable route of spread [3,4]. The commonest manifestation is in the uveal tract and usually presents as a posterior uveitis. Tuberculous uveitis still represents a minority of uveitis cases, with varying prevalence ranging from 2-4% to 12-25% in different areas of the world. Despite significant research over the past decades, the diagnosis of ocular TB is difficult to both ophthalmologists and physicians due to lack of gold standard criteria to diagnose ocular TB & clinical signs and symptoms can mimic other conditions [3]. A definite diagnosis of tuberculous uveitis can be confirmed by certain specific investigations like by performing acid-fast smears, culture of mycobacteria or polymerase chain reaction (PCR)-based assays on ocular fluids i.e. vitreous or aqueous humour. However, the sensitivities & specificity of these tests are not fairly high, making definitive diagnosis difficult. Occurrence of ocular TB is more common in immune compromised individuals while it is rare in immuno competent persons [4]. We are presenting a 28-year-old immune competent male, a very rare case of ocular tuberculosis.
Objective
To report a case of rare presentation of ocular tuberculosis.
Materials & Methods
Case Report
A 28year old male patient presented in Ophthal OPD with complains of diminution of vision in both eyes for past 1 month, which was insidious in onset, gradually progressive in nature & was associated with on & off floaters since 15 days in both eyes. There was no history of metamorphopsia, flashes, or field Loss in any eye. Patient also gave the history of fever & headache for past 1 week. Fever was sudden in onset, continuous type, associated with severe throbbing headache & doesn't relieve with medications. Patient had developed altered sensorium for Past 3 days. There was no history of any ocular surgery or trauma.
No significant medical history or any associated comorbid conditions in past.
On examination: Patient was febrile, had fever (39 °C), Brudzenski and Kernig signs were positive. CNS examination revealed no cranial nerve function abnormality.CSF analysis revealed clear fluid, elevated protein level, increased number of cells (2% polymorphs, 98% lymphocytes).CSF ADA( Adenosine deaminase)-15.7 U/L.
Ocular examination: On examination, his visual acuity of RE was 6/36, no improvement with pin hole, LE was CF@3 meter, no improvement with pin hole. Ocular motility-normal ocular movement of BE. Adnexa- normal in both eyes. Conjunctiva was normal. Cornea, was clear AC was normal in depth and contents. Pupils were brisk and reactive. Lens was clear in both eyes.
Fundus examination
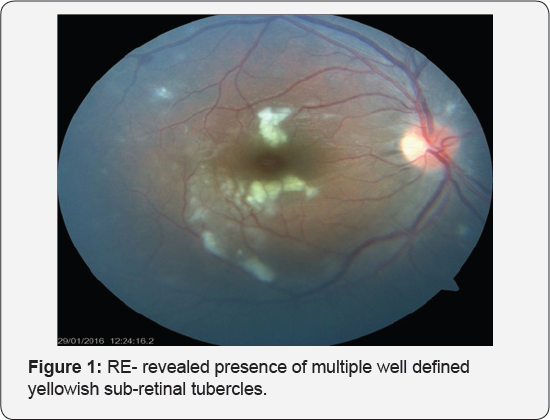
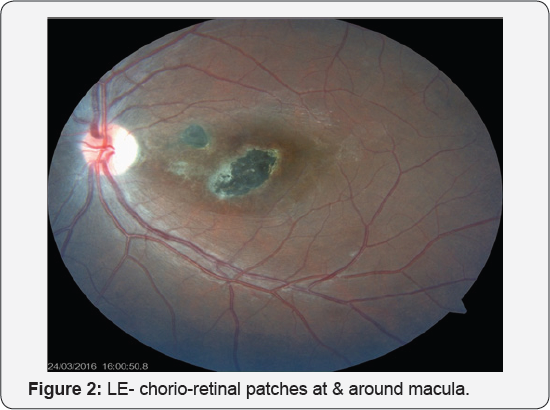
RE- revealed presence of multiple well defined yellowish sub-retinal tubercles (Figure 1). LE- chorio-retinal patches at & around macula (Figure 2). Based on clinical history & investigations a suspicion of tuberculous meningitis with ocular involvement was made. CT brain did not show any cerebral lesion correlating with TB. PPD skin testing was positive and the induration was 23mm. HIV-Negative. After the above mentioned clinical test & investigations the diagnosis of tuberculous meningitis with associated tuberculous choroiditis was established. In view of the vision-threatening consequences, the patient was advised a depot steroid (triamcinolone) injection in the left eye immediately but patient denied for that & then, after consulting the physician patient was put on oral steroid & on full anti-TB treatment with Isoniazid 300mg/day, Rifampicin 600mg/ day, Pyrazinamid 1200mg/day and Ethambutol 1600mg/day for 2 months as intensive phase & with Isoniazid 300mg/day, Rifampicin 600mg/day for next 6 months as continuation phase. Patient was advised regular follow ups.
Results
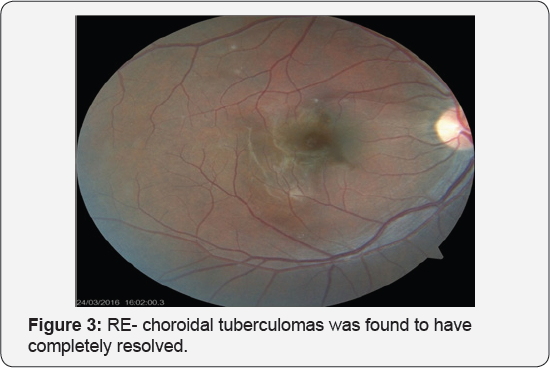
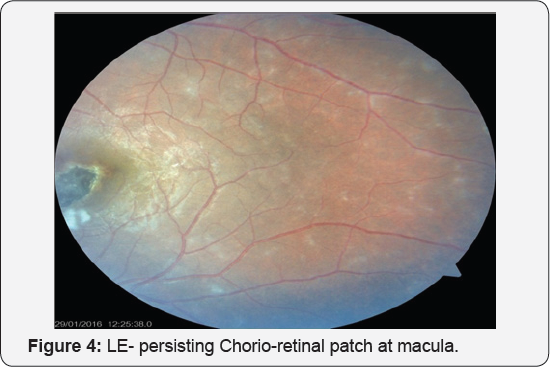
Patient had significantly improved with the treatment (Oral steroid & ATT). On review after 3 months patient showed improved visual acuity to 6/9 in right eye & 6/36 in left eye. On fund us examination choroidal tuberculomas was found to have completely resolved in right eye (Figure 3) while the chorioretinal patch in the left eye was persisting (Figure 4).
Discussion
Tuberculosis is a serious infectious disease primarily affecting the lungs. TB is caused by acid-fast bacteria belonging to Mycobacterium tuberculosis complex [4]. Other than lungs it can affect any other tissue of body also. Ocular TB is one of vision threatening variant of TB [3,4]. The ocular manifestations of tuberculosis vary from involvement of the lid and adnexa, orbital cellulitis, dacroadenitis, periocular lymphadenopathy to phlyctenules, conjuctival granuloma, scleritis , iridocyclitis in the anterior segment [3]. The posterior segment can be involved in the form of vitritis, pars planitis, chorio-retinitis, choroiditis and optic neuritis [3]. Sometimes ocular TB can be the only manifestation of the serious underlying systemic active tuberculosis. In certain cases Ocular TB helps physician to make appropriate early diagnosis with the help of an ophthalmologist & to decide further treatment. Thus a thorough knowledge of the possible ocular manifestations is very important to the treating ophthalmologist. Ocular TB (Extrapulmonary TB) is more difficult to diagnose than pulmonary disease. It often needs more Sophisticated laboratory techniques like the PCR and Gold TB-quantiFERON. Since HRCT scan detects subtle, early, and small lesions, it is very useful in detecting mediastinal lymphadenopathy [3-6]. A definitive diagnosis requires an interspeciality interaction and a high clinical suspicion [3,4,7,8].
Conclusion
Tuberculosis can present with variable clinical manifestations. Ocular TB is one of the varied manifestation of systemic TB. This case highlights the facts that a seemingly innocuous eye involvement could be associated with significant systemic tuberculosis & thus requires thorough investigation & timely prompt treatment. Early diagnosis & timely intervention helps in preventing the occurrence of vision threatening complications in case of ocular TB [9-12].
References
- Oluleye TS (2013) Tuberculous uveitis. J Multidiscip Healthc 6: 41-43.
- Agrawal R, Gonzalez LJJ, Nobre CJ, Gupta B, Grant R, et al. (2016) Predictive factors for treatment failure in patients with presumed ocular tuberculosis in an area of low endemicprevalence. Br J Ophthalmol 100(3): 348-355.
- Bharti G, Dewan T, Vashisth S, Shrivastav D, Singh MD (2013) A rare presentation of definitive ocular tuberculosis in a health-care worker. JIACM 14(1): 66-8.
- Marrakchi W, Aouam A, Kooli I, Brahim HB, Loussaief C, et al (2016) Atypical Clinical resentation of Ocular Tuberculosis in an Immunocompetent Patient. J NeurolTranslNeurosci 4(1): 1061.
- Sahu GN, Mishra N, Bhutia RC (1998) Manifestations in ocular tuberculosis. Ind J Tub 45: 153.
- Albini TA, Rao NA, Karakousis PC (2008) Interferon-ã Release Assays in the Diagnosis of Tuberculous Uveitis. American Journal of Ophthalmology 146: 486-488.
- Sheu SJ, Shyu JS, Chen LM (2001) Ocular manifestations of tuberculosis. Ophthalmology 108(9): 1580-1585.
- Goyal JL, Jain P, Arora R, Dokania P (2015) Ocular manifestations of tuberculosis. Indian J Tuberc 62: 66-73.
- Hase K, Namba K, Saito W, Ohno S, Ishida S (2015) A case of tuberculous endophthalmitis successfully treated with vitrecto my followed by anti tuberculous agents. J Ophthalmic Inflamm Infect 5: 14.
- Agrawal R, Gupta B, Gonzalez-Lopez JJ, Rahman F, Phatak S, et al. (2015) The Role of Anti-tubercular Therapy in Patients with Presumed Ocular Tuberculosis. Ocul Immunol Inflamm 23: 40-46.
- Al-Fraikh H, Al-Dahmash S (2010) Rare presentation of definitive ocular tuberculosis in an immunocompetent young patient. Saudi J Ophthalmol 24: 31-33.
- Albini TA, Rao NA, Karakousis PC (2008) Interferon-a Release Assays in the Diagnosis of Tuberculous Uveitis. American Journal of Ophthalmology 146: 486-8.






























