Post-Operative Steroid Response in Fellow Eye Ameliorated by Loteprednol
Mohammed Abusayf, Rizwan Malik*
Department of ophthalmology, King Khaled Eye Specialist Hospital, Saudi Arabia
Submission: July 24, 2017; Published: September 22, 2017
*Corresponding author: Rizwan Malik, Consultant Ophthalmologist, King Khaled Eye Specialist Hospital, Riyadh, Saudi Arabia, Tel: +966114821234; Fax: +966114821234; Email: rizimalik@googlemail.com/ rmalik@kkesh.med.sa
How to cite this article: Mohammed A, Rizwan M. Post-Operative Steroid Response in Fellow Eye Ameliorated by Loteprednol. 2017; 5(1): 555652. DOI: 10.19080/JOJO.2017.05.555652
Abstract
Introduction: Steroid-induced glaucoma is a form of secondary open angle glaucoma that usually results from the chronic use of topical steroids. Whilst steroid response in the eye being treated has been well-documented, a contralateral steroid response is less common. We report a patient with a fellow-eye steroid response following glaucoma surgery which was abolished by switching the patient to loteprednolol.
Case report: A 20-year-old gentleman presented with advanced bilateral steroid-induced glaucoma. His intraocular pressure (IOP) remained poorly controlled in the right eye despite maximum medical therapy and controlled in the left eye. He underwent non-penetrating deep sclerectomy in the right eye with satisfactory post-operative IOP on the first post-operative day. However, his IOP elevated markedly in the fellow left eye 5 days after commencement of prednisolone 1% drops to his right eye. This IOP elevation was ameliorated by switching him to loteprednol 0.5%.
Conclusion: A steroid response should be considered in any patient who develops high IOP in the fellow eye post-operatively. The use of loteprednolol may be an effective way to abolish this steroid response whilst maintaining control of post-operative inflammation in the operated eye.
Keywords: Steroid induced glaucoma; Deep sclerectomy; Decompression retinopathy; Fellow-eye steroid response; Loteprednolol
Introduction
Topical steroids have widespread use in the treatment of ophthalmic disease. Side effects include cataract formation and high intraocular pressure. Steroid-induced glaucoma is a form of secondary open angle glaucoma that usually results from the chronic use of topical steroids. Whilst steroid response in the eye being treated has been well-documented, a contralateral steroid response is less common. Loteprednol is an ester steroid which may cause less steroid response than other topical steroids. Here, we report a patient with a fellow-eye steroid response with prednisolone acetate 1% following glaucoma surgery which was abolished by switching the patient to loteprednolol 0.5%.
Case Report
A 20-year-old myopic gentleman was referred to our hospital with bilateral advanced glaucoma. He started to use topical FML drops 3 years previously without any prescription or medical supervision for symptoms of allergic conjunctivitis. He had a myopic glasses prescription in both eyes. He was using Duotrav (Timolol 0.5% / Travaprost 0.004% fixed combination) once daily and Azopt (Brinzolamide 1%) twice daily to both eyes. He had no family history of glaucoma. On examination, his best corrected visual acuity was 20/25 in each eye. He had deep anterior chamber angles with quiet eyes. There was no signs of pigment dispersion. The intraocular Pressure (IOP), as measured with Goldmann applanation tonometry was 41mmHg in the right eye and 42mmHg in the left eye. Gonioscopy revealed open angles (Shaffer grade 3 to 4 both eyes). Both optic discs were small in size and exhibited advanced cupping, with a cup-to-disc ratio of 0.9.
The patient's corneal thickness was 530 microns in each eye. Humphrey visual field examination with the 10-2 test grid showed advanced visual field loss in both eyes, with a Mean Deviation of -26dB and -17dB in the right and left eyes respectively (Figure 1). The most likely diagnosis in this patient was steroid-induced glaucoma from the chronic use of steroid drops. The main differential diagnosis in this patient was juvenile open angle glaucoma. In view of the severity of glaucomatous damage, young age of the patient and level of IOP in the right eye, intervention in the form of filtration surgery was planned. Due to the success of deep sclerectomy in young patients with steroid- induced glaucoma in the author's experience, deep sclerectomy was planned for the right eye. The patient was switched to Lumigan (Bimatoprost 0.03%) and Cosopt.

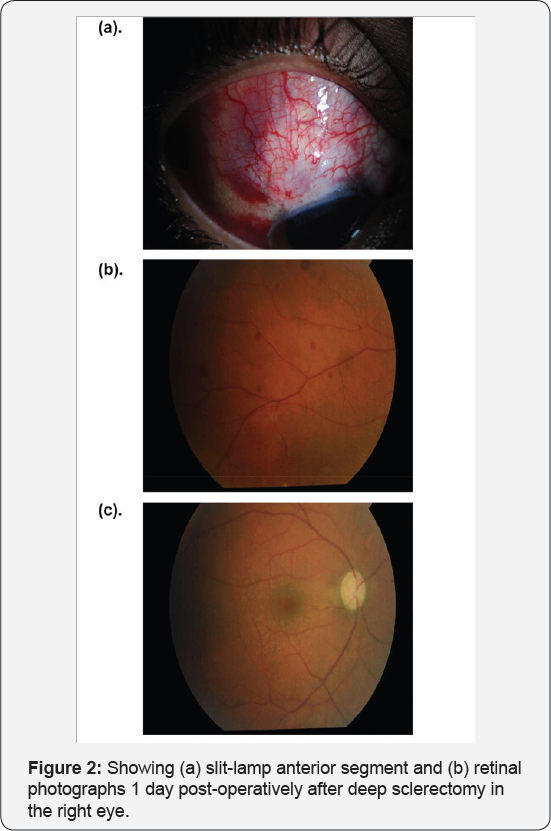
Timolol 0.5%/Dorzolamide 2% combination) twice daily to both eyes prior to surgery. The surgery was uneventful and post-operatively the patient was placed on prednisolone acetate 1% every 1 hour for the right eye for the control of intraocular and conjunctival inflammation. There was no change to the medication for the left eye. As the patient lived outside the city and was unable to return for a one-week follow-up appointment, he was admitted for post-operative treatment. On the first post-operative day, the right eye was injected, with a small subconjunctival haemorrhage, a deep anterior chamber and an IOP of 05mmHg (Figure 2a). Small mid-peripheral fundal retinal haemorrhages were noted (Figure 2b), most likely as a result of decompression retinopathy [1]. The optic nerve appearance was unchanged (Figure 2c). The IOP in the left eye was 15mmHg.
Five days post-operatively, the patient's condition remained stable in the operated right eye. However, he developed markedly high IOP in the left eye (40mmHg) whilst still on cosopt and lumigan to the left eye. During this post-operative period, the patient remained in the hospital, with all medication administered by the nursing staff.
A contralateral steroid response was considered likely and topical prednisolone forte was changed to loteprednol every 2 hours. Four days later, the IOP was 09mmHg in the right eye and had normalised to 10mmHg in the left eye. The patient was discharged 1 week after surgery. The loteprednol was tapered and discontinued over 2 months. Over the subsequent six months following surgery, the patient remained stable, with visual acuity of 20/25 in each eye and an IOP of 11mmHg in the right eye and 27mmHg in the left eye as a likely result of noncompliance of glaucoma drops in the left eye. Deep sclerectomy has been planned for the left eye.
Discussion
Whilst steroid response in the eye being treated with steroid drops is well recognised, a steroid response in the fellow eye is less well recognized. Further, to our knowledge this is the first case documenting an amelioration of steroid response in the contra lateral eye after switching to loteprednol. It has long been recognized that, in the general adult population, about one-third will experience 6-15mmHg elevation in the level of IOP which defined as moderate responders, while around 5% will experience IOP elevations of 15mmHg which defined as high responders following 4-6 weeks of topical corticosteroid therapy. 1 Family history of glaucoma, diabetes mellitus, young age and myopia are recognized risk factors in those of individuals [1,2]. Our patient exhibited the latter 2 risk factors. As evident in our patient, patients may develop glaucomatous optic nerve damage and irreversible vision loss, with either topical, periocular or oral steroid use [5-8].
Post-operatively, our patient developed a steroid response in the fellow eye, rather than the operated eye, presumably due to the surgical fistula, which prevented such a rise in the operated eye. Systemic absorption resulted in a steroid response in the fellow eye, which took 5 days to develop [9,10]. Although classically steroid-induced rise takes weeks to develop, some patients can have elevated IOP within days of starting topical steroid therapy [11].
Whilst the possibility of non-compliance of glaucoma medication should normally be considered as a cause of raised IOP, this patient was admitted in hospital during his post-operative course and the nursing staff were meticulously administering all medication during this period [12-15]. Lotemax and Predforte share the same chemical structure except that lotemax contains an ester instead of a ketone molecule at the carbon 20 (C-20) position. This makes lotemax metabolically labile at C 20 to be hydrolyzed by endogenous esterase into an inactive metabolite. Additionally lotemax is highly lipophilic. All these factors give lotemax high ocular penetration for potent anti-inflammatory effects and less IOP elevation. In our patient, the steroid response diminished with the introduction of lotemax instead of prednisolone 1%. Studies have shown a lesser effect of lotemax on intraocular pressure compared to many others topical steroids used in ophthalmic diseases on the short term and long term such as FML, Dexamethasone and Prednisolone acetate and similar clinical effects [16-18], regardless of formulation, dosage regimen, or treatment duration, including in known steroid responders. Post operatively, the treating physician should remember to check IOP in both eyes particularly in steroid responders because of the possibility of a rise in IOP in the contra lateral eye. The use of loteprednol may help ameliorate a fellow eye steroid response whilst maintaining control of intraocular conjunctival inflammation in the operated eye'.
References
- Jones R, Rhee DJ (2006) Corticosteroid-induced ocular hypertension and glaucoma: a brief review and update of the literature. Curr Opin Ophthalmol 17(2): 163-167.
- Kersey JP, Broadway DC (2006) Corticosteroid-induced glaucoma: a review of the literature. Eye 20: 407-416.
- Bodor N (1993) Design of novel soft corticosteroids. Current problems in dermatology 21: 11-19.
- Kozobolis VP, Kalogianni E, Katsanos A, Dardabounis D, Koukoula S, et al. (2011) Ocular decompression retinopathy after deep sclerectomy with mitomycin C in an eye with exfoliation glaucoma. European journal of ophthalmology 21: 324-327.
- Sahni D, Darley CR, Hawk JL (2004) Glaucoma induced by periorbital topical steroid use-- a rare complication. Clinical and experimental dermatology 29: 617-619.
- Aggarwal RK, Potamitis T, Chong NH, Guarro M, Shah P, et al. (1993) Extensive visual loss with topical facial steroids. Eye 7 (Pt 5): 664-666.
- Fat CL, Leslie T (2011) Irreversible visual loss secondary to excessive topical steroid use in eczema. The British journal of general practice : the journal of the Royal College of General Practitioners 61(590): 583584.
- Chadha V, Cruickshank I, Swingler R, Sanders R (2008) Advanced glaucomatous visual loss and oral steroids. Bmj 337: a670.
- Levene R, Wigdor A, Edelstein A, Baum J (1967) Topical corticosteroid in normal patients and glaucoma suspects. Archives of ophthalmology 77(5): 593-597.
- Spiers F (1965) Topical steroids and intraocular pressure. II. An evaluation of the intraocular pressure in 93 outpatients divided according to their response to monocular steroid provocation and studies on the reaction of the control eye. Acta ophthalmologica 43(6): 812-820.
- Armaly MF (1963) Effect of Corticosteroids on Intraocular Pressure and Fluid Dynamics. I. The Effect of Dexamethasone in the Normal Eye Arch ophthalmology 70: 482-491.
- Bodor N, El-Koussi AA, Kano M, Khalifa MM (1988) Soft drugs. 7. Soft beta-blockers for systemic and ophthalmic use. J Med Chem 31(8): 1651-1656.
- Bodor N (1994) Designing safer ophthalmic drugs by soft drug approaches. Journal of ocular pharmacology 10(1): 3-15.
- Bodor N, Buchwald P (2005) Ophthalmic drug design based on the metabolic activity of the eye: soft drugs and chemical delivery systems. The AAPS J 7(4): E820-833.
- Druzgala P, Wu WM, Bodor N (1991) Ocular absorption and distribution of loteprednol etabonate, a soft steroid, in rabbit eyes. Current eye research 10(10): 933-937.
- Comstock TL, DeCory HH (2016) Loteprednol Etabonate 0.5%/Tobramycin 0.3% Compared with Dexamethasone 0.1%/Tobramycin 0.3% for the Treatment of Blepharitis. Ocular immunology and inflammation 1-8.
- Jung HH, Ji YS, Sung MS, Kim KK, Yoon KC (2015) Long-Term Outcome of Treatment with Topical Corticosteroids for Severe Dry Eye Associated with Sjogren's Syndrome. Chonnam medical journal 5(1): 26-32.
- Lane SS, Holland EJ (2013) Loteprednol etabonate 0.5% versus prednisolone acetate 1.0% for the treatment of inflammation after cataract surgery. Journal of cataract and refractive surgery 39(2): 168-173.






























