Simple Ocular Colobamata in Two Generations of a Family
Tarun Sood1*, Mandeep Tomar3, Shilpa Sood2 and Nishant Vardhan4
1Department of ophthalmology, Civil hospital, India
2Department of ophthalmology, Roatry eye hospital Kullu
3Department of ophthalmology, India
4Deprtment of ophthalmology, civil hospital, India
Submission: August 04, 2017; Published: September 18, 2017
*Corresponding author: Tarun Sood, Department of ophthalmology, Eye surgeon, civil hospital sarkaghat, himachal pardesh, India,Tel: 9418436544; Email: tarunsood_86@yahoo.co.in
How to cite this article: Tarun S, Mandeep T, Shilpa S, Nishant V. Simple Ocular Colobamata in Two Generations of a Family. 2017; 4(5): 555647. DOI: 10.19080/JOJO.2017.04.555647
Abstract
Generally, colobomata are contemplated as clefts caused by absence of tissue in the inferonasal quadrant of the eye. Failure of the ectodermal optic vesicle fissure to close is regarded as basic etiology of coloboma [1]. Prevelance of ocular colobomata is calculated to be 0.5 to 2.2 cases per 10000 live births. The typical, most frequent location of ocular coloboma is the inferonasal quadrant [2,3]. The author tends to report the presence of simple iris coloboma in female members comprising three generations of a indian family. The Grand mother had simple iris coloboma in right eye, mother in left eye, and daughter in Left eye .
Introduction
A 27 year old female presented with her 8 year old girl and 58 year old mother for routine eye checkup . simple iris coloboma was noted in all three of them
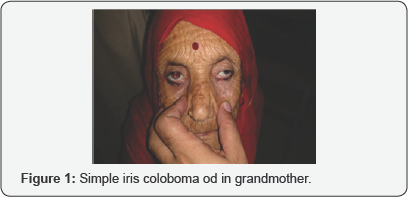
Figure 1: Grandmother with controlled hypertension .visual acuity was recorded as od 6/6 ,os 6/6 s.PCIOL was implanted in both eyes. Fundus examination was unremarkable in both eyes
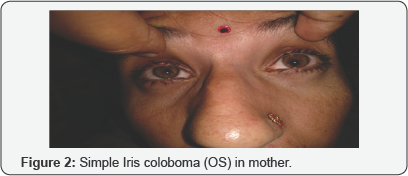
Figure 2: Best corrected Visual acuity in case of mother was 6/9 and 6/12. OD-9.00 DSPH -3.00 DCYL AT 90 6/9 OS: -11.00 ,-3.00 DCYL AT 90 6/12. Typical iris coloboma was present in left eye. Slit lamp examination was unremarkable .fundus examination revealed myopic fundus 0U.

Figure 3: Granddaughter had uncorrected visual acuity of 6/6 0U. Typical iris coloboma was present in left eye. Slit lamp examination and indirect ophthalmoscopy were unremarkable. The mother gave a history of uneventful pregnancy, birth and neonatal history. She was given 'routine' drugs, namely fersolate tablets, folic acid tablets, and vitamin B complex tablets
Discussion
The term coloboma was coined by WALTHER in 1921, to describe a condition wherein a portion of structure of eye is lacking. Congenital ocular colobomata (derieved from the Greek word koloboma meaning mutilated or curtailed) is supposed to be consequence of defective embryogenesis. Subsequently, ocular colobomas were categorised as typical or atypical, depending on their location in eye. By definition [4], the typical coloboma is found in region of embryonic cleft (inferonasally) and is due to disturbance of mechanism of closure. Atypical coloboma is located elsewhere and is of different etiology [5]. A typical iris coloboma is characterised by concurrent presence of choroidal coloboma in region of embryonic cleft. Simple iris coloboma or atypical iris coloboma is condition where occurrence of iris coloboma is not accompanied by existence of a typical choriodal coloboma. A complete iris coloboma involves the pigment epithelium and stroma leading to keyhole pupil, which can be unilateral or bilateral. Although isolated iris coloboma is observed, it is often associated with colobomata in other parts of the eye. Chorioretinal coloboma, colobomata affecting the posterior segment of the eye can be unilateral or bilateral. In case the fetal fissure fails to close posteriorly, then a coloboma affecting the retinal pigment epithelium (RPE), neurosensory retina, or choroid may occur. The defect is essentially a bare sclera with the overlying RPE, retina, or choroid missing. Typically occurring in the inferonasal quadrant. Usually, chorioretinal colobomata are asymptomatic despite significant upper visual field defects. Majority patients with Coloboma are clinically asymptomatic. Complications such as retinal detachment and Cataract are associated with retinochoroidal Coloboma. Cataracts of multiple varieties are associated with coloboma including pigment deposits, sub capsular, cortical, anterior and posterior polar and total opacification.
Conclusion
The most common mode of inheritance of isolated colobomatous malformation is autosomal dominant, although autosomal recessive inheritance, x linked inheritance has also been observed in some families [4]. Mitochondrial Inheritance needs to be strongly suspected if the Coloboma runs only in female members of generations.
References
- Sheetal B, Gopal KM (2015) Ocular Colobamata in a Family. Journal of Evidence based Medicine and Healthcare 2(17): 2420-2423.
- Warburg M (1993) Classifi cation of microphthalmos and coloboma. J Med Genet 30(8): 664-669.
- Stoll C, Alembik Y, DoJ B, Roth MP (1992) Epidemiology of congenital eye malformations in 131,760 consecutive births. Ophthalmic Paediatr Genet 13(3): 179-186.
- Hornby SJ, Dandona L, Jones RB, Stewart H, Gilbert CE (2003) The familial contribution to non-syndromic ocular coloboma in south India. Br J Ophthalmol 87(3): 336-340.
- Tantri AP, Johnson AT (2006) Retinochoroidal coloboma: 54-year-old female with blurred vision. Eyerounds.org.






























