Application Strategies and Drawbacks of Biomaterials in Ocular Implants
Adityateja KG, and Mukty Sinha*
Department of Medical Devices, India
Submission: August 09, 2017; Published: September 06, 2017
*Corresponding author: Mukty Sinha, Department of Medical Devices, National Institute of Pharmaceutical Education and Research-Ahmedabad, Gujarat, India, Tel: +91-9327671224; Fax: +91-79-27450449; Email: muktys@gmail.com
How to cite this article: Adityateja KG, Mukty S. Application Strategies and Drawbacks of Biomaterials in Ocular Implants. 2017; 4(3): 555639. DOI: 10.19080/JOJO.2017.04.555639.
Abstract
Eye is highly sensitive organs with primary role in vision and the main responsible parts for the vision are cornea, lens, and retina. Any refractory error leads to blurred vision or blindness. In order to rectify the disorders of each organelle of our eye various biomaterials are used for the fabrication of implants. The present review mainly focuses on the criteria of selection of various types of biomaterials used for fabrication of implants which are used to rectify various ocular problems arises due to age, trauma and diseased condition.
Keywords: Contact lens; Corneal implants; PMMA; PHEMA; PVA; Hydrogel
Introduction
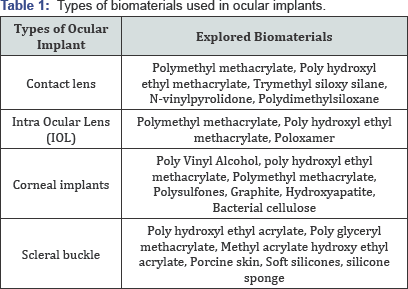
Out of all the sense organs eye is considered as the most important and sensitive sense organ. It is not only sensitive but also equally complex system. Eye is a soft organ and most of the part is a vascular. It is housed in an eye socket, orbit. Light travels through the eye by crossing various layers, the outer most is tear layer and subsequent layers in order of appearance are corneal, aqueous humor, lens, vitreous humor, and retina. Finally image is formed at retina and it is sensed through lens optics which is connected to the brain through macular part. Any obstruction in any of the layer leads to blurred vision or blindness. The transplantation of the part is reported, but the supply is less than the demand. Therefore, there is great need of artificial support for the systems. A number of biomaterials has been tried for the purpose and many of the artificial transplants are been used successfully (Table 1). The current review evaluates all the biomaterials which has been explored for the applications with their drawbacks and advantages.
Contact Lens
Contact lenses are used to correct refractive error in eye. Therapeutic contact lenses are being used nowadays to deliver drug to treat various ocular diseases [1]. Leonardo da Vinci et al. [2], is the person who has invented the use of contact lenses for the first time in 1508 [2]. There are two types of lenses, hard contact lens and soft contact lens. Initially they were made up of glass taking moulds of rabbit or cadaver eyes. The discoveryof polymethyl methacrylate (PMMA) led to the idea of usage of polymers for the development of contact lenses. However, PMMA lenses are hard and are difficult to wear for longer durations as these lenses do not permeate oxygen to pass through them. Wearing PMMA lenses obstructed oxygen diffusion hence there is a need for other alternative material [3,4]. To address this an attempt was made in the form of rigid gas permeable contact lenses which are made by copolymerising methyl methacrylate (MMA) with trymethyl siloxy silane (TRIS) which have been licensed to extended wear up to 7 days [5]. In subsequent years, the synthesis of poly hydroxyl ethyl methacrylate (PHEMA) led to the manufacturing of soft contact lenses in 1961 [6]. PHEMA gives excellent comfort and is having greater elastic modulus, higher water content upto 38% of water. In addition to this various hydrogel based lenses were also made from polymers like N-vinylpyrrolidinoneand glyceryl methacrylate [7, 8]. Although these lenses were comfortable to wear the main drawback is that these hydrogel based lenses must be very thin and permeable of oxygen, but reduction in thickness led to loss in strength [9,10]. Another type of soft contact lenses were made up of polydimethylsiloxane (PDMS), it is having higher oxygen permeability. But the problem with PDMS is its low surface energy results in poor wetting [11]. Research is being carried out to increase the wet ability of the lens by grafting with hydrophilic polymers. Till date, PHEMA is most commonly used in contact lens with upto 90% water content for extended use.
Intra Ocular Lens
Cataract is one of the most dreadful diseases that lead to blindness by clouding of the lens. The removal of natural lens leads to withdrawal of cloudiness. Later, to reinstate the natural vision, an intra ocular lens (IOL) is placed. Typically IOL have two parts: optic and haptic [12]. Haptic may be made up of same material or different material. PMMA is the widely used material for manufacturing of IOL. It is selected because of its high bio-compatibility and less weight. Though PMMA has been used for 40 years it has its own disadvantages like less surface energy results to damage of corneal endothelium [13]. Polymeric coatings of NVP and HEMA are being coated to improve the bio-compatibility and to increase the surface energy [14,15]. In addition to PHEMA hydrogels, collagen fibers and acrylic polymers are used for manufacture of foldable IOL [16]. Recently, thermo sensitive polymer, poloxamer hydrogel has been studied for IOL and the pilot study showed satisfactory results [17].
Corneal Implants
In order to alter the refractive state of the eye permanent implants are inserted into cornea. Previously the implant completely replaces the entire thickness of cornea but recent advancements are available where only selected layers can be replaced. Initially corneal implants were made from flint glass later they were replaced by PMMA. Though PMMA is a good polymer, it obstructs nutrition transport in the cornea and there are reports of mechanical irritation [18] and thinning of epithelial layer above the cornea. Later, polysulfones were selected for making thin and high refractive index film to replace natural cornea, but polysulfones is impermeable to aqueous solutions and results in poor nutrient transport. So the surfaces are made porous with a pore size of 10|im [19]. In order to improve the design, hydrogel based corneal implants came into picture [20], but, they were unable to match the refractive index of natural cornea [21, 22]. To improve the mechanical feature and bio adhesion of the artificial cornea, the design has further improved by using core-skirt approach. The material which has been studied in the design is Poly vinyl alcohol, PHEMA, graphite [23, 24]. Other hydrogel systems are also tried like bacterial cellulose [25], but clinical trials are required to prove the efficacy. Myopia can also be corrected by altering the surface area of the cornea. A specialized ring is surgically inserted into the corneal surface to flatten the surface and adjusting the focal point on to fovia [26]. PMMA rings are approved by FDA in 2004 for treatment of keratoconus [27]. These are also exempted under humanitarian device exemption.
Scleral Buckle
Retinal detachment is a severe condition where retina gets peeled off from its basement membrane. Scleral buckle pushes the sclera and brings chroid back in contact with retina [28]. A wide variety of materials are used for the formulation of scleral buckles, in early days tendons of the same patient were used; though they eliminate out foreign body reactions but it required double surgery. The elasticity of implants is the major drawback as the exact required dimensions of the buckle cannot be achieved. Many other biodegradable materials are being used but the most accepted and widely used substance is gelatin derived from porcine skin [29]. The main problem with the absorbable buckles is inefficient buckling effect. Therefore, non absorbable buckles came into picture which is made up of soft silicones and silicone sponges [30]. The buckles are soft even after implantation thereby preventing the erosion of underlying sclera. In addition to soft silicones various materials like poly glyceryl methacrylate (PGMA), poly hydroxyl ethyl acrylate (PHEA), and methyl acrylate hydroxy ethyl acrylate (MAI). Out of the three, MAI possess better bulk properties while PHEA breaks on swelling and PGMA has poor tensile strength.
Concluding Remarks
There are many biomaterials has been for various types of ocular implants. Some have proven efficacy in in-vitro and preclinical studies. The materials must be scaled up to clinical level for human applications. Additionally, there is scope of newer polymer with nano materials approach. Moreover, these implants can be used as drug delivery depot for the treatment of various ocular diseases like age related macular degeneration, glaucoma, etc.
References
- Costa VP, Braga ME, Duarte CM, Alvarez LC, Concheiro AG, et al (2010) Anti-glaucoma drug-loaded contact lenses prepared using supercritical solvent impregnation. J Supercrit Fluid 53:165-173.
- Heitz R, Enoch J, Leonardo DV (1987) An assessment on his discourses on image formation in the eye. Advances in Diagnostic Visual Optics 19-26.
- MacRae SM, Matsuda M, Yee R (1985) The effect of long-term hard contact lens wear on the corneal endothelium. Eye Contact Lens 11: 322-326.
- Thean JH, Mcnab AA (2004) Blepharoptosis in RGP and PMMA hard contact lens wearers. Clin Exp Optometry 87: 11-14.
- Khoo C, Chong J, Rajan U (1999) A 3-year study on the effect of RGP contact lenses on myopic children. Singapore Med J 40: 230-237.
- Wichterle O, Lim D (1960) Hydrophilic gels for biological use. Nature 185: 117-118.
- Kunzler JF, Friends GD (1991) Polymer compositions for contact lenses. Google Patents.
- Vanderlaan DG, Nunez IM, Hargiss M, Alton ML, Williams S (1999) Soft contact lenses. Google Patents.
- Dohlman CH, Rejojo MF, Rose J (1967) Synthetic polymers in corneal surgery: I. Glyceryl methacrylate. Arch Ophthalmol-Chic, 77: 252-257.
- Evans CH (1980) Hydrogel contact lens. Google Patents.
- Nicolson PC, Vogt J (2001) Soft contact lens polymers: an evolution. Biomaterials 22(24): 3273-3283.
- Cumming JS (2009) Accommodating 360 degree sharp edge optic plate haptic lens. Google Patents.
- Obstbaum SA (1992) The Binkhorst Medal Lecture Biologic relationship between poly (methyl methacrylate) intraocular lenses and uveal tissue. J Cataract Refr Surg 18: 219-231.
- Yao K, Huang XD, Huang XJ, Xu ZK (2006) Improvement of the surface biocompatibility of silicone intraocular lens by the plasma-induced tethering of phospholipid moieties. J Biomed Mater Res A 78(4): 684692.
- Lowe AB, Vamvakaki M, Wassall MA, Wong L, Billingham, et al. (2000) Well-defined sulfobetaine-based statistical copolymers as potential antibioadherent coatings. J Biomed Mater Res Part A 52(1): 88-94.
- Feng Y, Borrelli M, Reichl S, Schrader S, Geerling G (2014) Review of alternative carrier materials for ocular surface reconstruction. Curr Eye Res 39(6): 541-552.
- Kwon JW, Han YK, Lee WJ, Cho CS, Paik SJ, et al. (2005) Biocompatibility of poloxamer hydrogel as an injectable intraocular lens. J Cataract Refract Surg 31: 607-613.
- Loughnan MS, Robinson D, Sullivan L (1996) Mechanical methods in refractive corneal surgery. Curr Opin Ophthalmol 7(4): 41-46.
- Grendhal DT (1986) Corneal inlay with holes. Google Patents.
- Mcdonald MB, Mccarey BE, Storie B, Beuerman RW, Salmeron B, et al. (1993) Assessment of the long-term corneal response to hydrogel intrastromal lenses implanted in monkey eyes for up to five years. J Cataract Refract Surg 19(2): 213-222.
- Werblin TP, Peiffer RL, Binder PS, Mccarey BE, Patel AS (1992) Eight years experience with Permalens® intracorneal lenses in nonhuman primates. Refract Corneal Surg 8(1): 12-22.
- Mulet ME, Alio JL, Knorz MC (2009) Hydrogel intracorneal inlays for the correction of hyperopia: outcomes and complications after 5 years of follow-up. Ophthalmology 116(8): 1455-1460.
- Liu K, Li Y, Xu F, Zuo Yi, Zhang Li, et al. (2009) Graphite/poly (vinyl alcohol) hydrogel composite as porous ringy skirt for artificial cornea. Mater Sci Engg C 29: 261-266.
- Sinha M, Gupte T (2017) Design and evaluation of artificial cornea with core-skirt design using polyhydroxyethyl methacrylate and graphite. Int Ophthalmol.
- Wang J, Gao C, Zhang Y, Wan Y (2010) Preparation and in-vitro characterization of BC/PVA hydrogel composite for its potential use as artificial cornea biomaterial. Mat Sci Engg C 30(1): 214-218.
- Alio JL, Salem TF, Artola A, Osman AA (2002) Intracorneal rings to correct corneal ectasia after laser in situ keratomileusis. J Cataract Refract Surg 28(9): 1568-1574.
- Feldman BH, Kim T (2010) Enhanced effect of double-stacked intrastromal corneal ring segments in keratoconus. J Cataract Refract Surg 36 : 332-335.
- Fraser S, Steel D (2010) Retinal detachment. BMJ Clin Evid.
- Chen T, Janjua R, Mcdermott MK, Bernstein SL, steidl SM, et al. (2006) Gelatin-based biomimetic tissue adhesive. Potential for retinal reattachment. J Biomed Mater Res B Appl Biomater 77(2): 416-422.
- Tsui I (2012) Scleral buckle removal: indications and outcomes. Surv Ophthalmol 57(3): 253-263.






























