Hay-Wells Syndrome: Case Report
Cristina Sousa1*, Jorge Breda1, Goretti Silva2 and Fernando Falcao-Reis1,3
1Ophthalmology Department, Centro Hospitalar de Sao Joño, Portugal
2Pediatrics Department, Centro Hospitalar de Sao Joño, Portugal
3Órgñose Sentidos Department, University of Porto, Portugal
Submission: March 02, 2017; Published: May 04, 2017
*Corresponding author: Cristina Sousa, Ophthalmology Department, Centro Hospitalar de Sao Joao, Alameda Professor Hernani Monteiro, 4200319 Porto 22-551-21-00, Portugal, Email: Cris.sousa.med@gmail.com
How to cite this article: Cristina S, Jorge B, Goretti S, Fernando F. Hay-Wells Syndrome: Case Report. JOJ Ophthal. 2017; 3(1): 555603. DOI: 10.19080/JOJO.2017.03.555603
Abstract
Introduction: Hay-Wells Syndromeis a rare disease with an autosomal dominant transmission. It is a type of ectodermal dysplasia, leading to impaired development of hair, nails, teeth and glands, usually in association with cleft palate and/or lip and ankyloblepharon. This syndrome is present at birth and diagnosis is made based on child phenotypic features. This study aims to describe a case of this syndrome.
Case report: Authors describe a case of a newborn with no history of parental consanguinity or other similar cases in the family. At birth alopecia, ankyloblepharon, cleftpalate, micrognatia and absent nails were detected. Surgical correction of ankyloblepharon was done. Postoperative period had no complications and after 12 months of follow-up lid edges are completely free.
Discussion: As a genetic disease, treatment is symptom-oriented. Antibiotic ointments can be used in skin lesions. Surgery is reserved for correction of cleft palate/lip and ankyloblepharon. Genetic counseling is recommended.
Keywords: Syndrome; Ectodermal dysplasia; Ankyloblepharon cleft palate and lip
Introduction
Hay-Wells Syndrome, also known as AEC syndrome (ankyloblepharon-ectodermal dysplasia- clefting syndrome), is a rare genetic disease [1], with an autosomal dominant transmission. Sporadic cases have, however, also been described. First described by Hay and Wells in 1976 [2], it was later found that it is caused by a p63 gene mutation, a known regulator of epithelial development/differentiation and homologous of the TP53 oncosupressor gene [3,4]. It is a type of ectodermal dysplasia, leading to impaired development of hair, nails, teeth and glands, usually in association with cleft palate and/or lip and ankyloblepharon. These are considered the cardinal signs of the syndrome by most authors. This syndrome is present at birth and diagnosis is made based on the child's phenotypic features. The authors aim to describe a case of a male newborn with the cardinal signs of this syndrome at birth, as it is a very rare syndrome with just a few cases reported worldwide.
Case Report
Male white newborn with no history ofparental consanguinity or other similar cases in the family. The baby was born by spontaneous vaginal delivery after an uneventful pregnancy with good prenatal care. At birth alopecia, ankyloblepharon, cleft palate, micrognathia and absent nails were detected (Figure 1a,1b & 1c- Phenotypic features). Anterior segment was normal, with no detected anomalies in the lacrimal apparatus. The rest of the physical examination was normal.
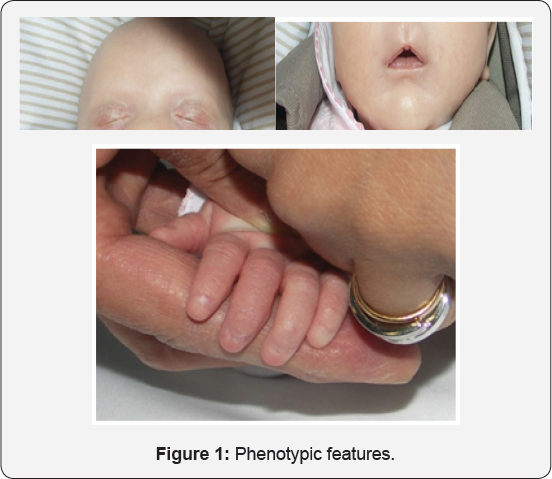
Ophthalmic ultrasound revealed a normal posterior segment. Abdominal and pelvic ultrasound were normal. Head ultrasound showed a small cyst in the pellucid septum and an apparent thickening in optic chiasmal area. Further study with Cranial MRI was normal, thus excluding a septum-optic dysplasia. Blood tests (CBS, electrolytes, hepatic function, kidney function, imunophenotyping and immunoglobulin levels) revealed a decrease in immunoglobulin A (X; normal range X), with no other changes. Hearing tests were normal.
Dermatology consultation recommended topical streoids in scarceeczematous areas and daily mineral ointments. Later hair prosthesis was discussed with the parents. Surgical correction of ankyloblepharon was carried out by ophthalmologists. Tearing of lid bridges was done in the operating room, under general anesthesia, using an electric scalpel in both eyes (Figure 2- Surgical correction of ankyloblepharon). Careful tearing with gentle pulling of the eyelids was carried out in order not to damage the underlying cornea. Post-operative period had no complications and after 12 months of follow-up lid edges are completely free (Figure 3 - After 12 months of follow-up).
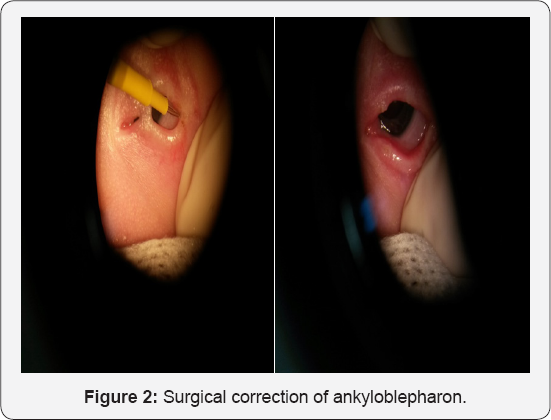
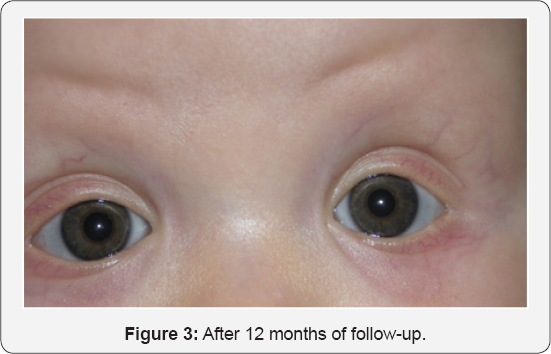
Cleft palate was complete, type III. Surgical correction was performed according to Furlow and Von Langenbeck procedures by pediatric surgeons. Blood molecular analysis of TP63 mutations and deletions/duplications was normal; we are still waiting for molecular analysis of mouth mucosa specimen. Unfortunately, it was not possible to have parental authorization to carry DNA analysis in their cells. Speech therapy was also prescribed.
Discussion
Hay-Wells Syndrome, also known as AEC Syndrome (ankyloblepharon-ectodermal dysplasia-clefting), is a rare autosomal dominant disease [1]. Ankyloblepharon, ectodermal dysplasia signs and cleft palate are considered cardinal signs of this syndrome [5]. All of these features were present in our case.
Ankyloblepharon results from fusion, partial or total, of superior and inferior lid edges. In general, eyelids remain closed until the 5th week of gestation, when they open spontaneously. The mechanism underlying this phenomenon is still on debate, but many author point out keratinization as the key [6]. Accordingly, any kind of anomaly occurring between 7th and 15th week of gestation can result in eyelid anatomy changes [6]. Ankyblepharon can also be present in Trisomy 18 and CHAND Syndrome (Curly hair-Ankyblepharon-Nail Dystrophy), being associated with heart malformations, hydrocephaly, imperforated anus and glaucoma. Ankyblepharon should then be a warning sign for the possibility of other important simultaneous diseases [7].
Ectodermal dysplasias are a group of diseases in which there is impaired development of hair, teeth, nails, sweet glands and other structures originating from ectoderm [8,9]. These anomalies, when associated with other malformations, correspond to a group of ectodermal dysplasia syndromes that includes EEC Syndrome (ectodactilia-ectodermal dysplasia- clefting), Rapp-Hodgkin Syndrome and Chand Syndrome, the most important differential diagnosis of Hay-Wells Syndrome [9]. In our case, none of the other malformations were identified, so that Hay-Wells Syndrome diagnosis was straight forward.
Hay-Wells Syndrome patients can have various degrees of alopecia, thin and scarce hair, onicodystrophies, palmoplantar hyperkeratosis, cutaneous pigment changes [10], hypohidrosis, hypodontia, teeth malformations and ear anomalies. Lacrimal canal obstruction is common. Other described features include super numerary nipples, otitis media, hypospadia, middle-facial hypoplasia, hypertelorism, low height, mental retardation, deafness and other ocular deformities.
At birth, a descamative erythrodemia can be seen, with superficial erosion and crusts. Scalp area usually shows an erosive dermatitis, which is a common source of infection, putting these patients at an increased risk of bacterial superinfection and sepsis; this leads to an increase in mortality and morbidity rate in newborns with this syndrome. A lot of Hay-Wells Syndrome cases are erroneously diagnosed as bullous epidermolysis due to the presence of erythrodermia and extensive areas of erosion. It is thought that scalp lesions can disappear with age or lead to alopecia [3].
Although concerns exist about wound healing in patients with this syndrome, there have been no reported instances of wound healing complications. Cleft lip and palate repair can then be performed safely in patients with Hay-Wells syndrome.
This syndrome is caused by a p63 gene mutation, an homologous of p53 oncosupressor gene [3,4], which has a central role in epidermal stratification process, regulating basal keratocyts proliferative capacity. Evidence showing that changes in this gene can be associated with other diseases like EEC and Rapp-Hodgkins syndrome reveal the high pleomorphic effect of p63 gene mutations. Hay-Wells Syndrome results specifically from amino-acid substitution in SAM domain (sterile alpha motif) [3,4].
Timely diagnosis is essential. As a genetic disease with multiple phenotypic features, multidisciplinary action is of main importance and treatment is symptom-oriented. Antibiotic ointments can be used in skin lesions. Surgical treatment is reserved for correction of cleft palate/lip and ankyloblepharon. Genetic counseling is recommended.
Disclosure statement
No sponsorship or funding arrangements relating to research and no conflicts of interest to declare.
References
- Rosa EJ, Ronaldo FM, Marcelino PMN, Alessandra AM, Aloisio G (2010) Hay-Wells Syndrome- A Case Report. An Bras Dermatol 85(2): 365596.
- Hay RJ, Wells RS (1976) The Syndrome of Ankyblepharon, Ectodermal D and Cleft Lip and Palate: An Autosomal Dominant Condition. Br J Dermatol 94(3): 277-289.
- Payne AS, Yan AC, Ilyas E, Li W, Seykora JT, Young TL, et al. (2005) Two novel TP63 mutations associated with the ankyloblepharon, ectodermal defects, and cleft lip and palate syndrome: a skin fragility phenotype. Arch Dermatol 141(12): 1567-173.
- McGrath JÄ, Duijf PH, Doetsch V, Irvine AD, de Waal R, et al. (2001) Hay- Wells syndrome is caused by heterozygous missense mutations in the SAM domain of p63. Hum Mol Genet 10(3): 221-229.
- Macias E, de Carlos F, Cobo J (2006) Hay-Wells syndrome (AEC): a case report. Oral Dis 12(5): 506-508.
- Mohamed YH, Gong H, Amenyra T (2003) Role of apoptosis in eyelid development. Exp Eye Res 76(1): 115-123.
- Sharkey D, Marlow N, Stokes J (2008) Ankyloblepharon filiforme adnatum. J Pediatr 152(4): 594.
- Tsutsui K, Asai Y, Fujimoto A, Yamamoto M, Kubo M, et al. (2003) A novel p63 sterile alpha motif (SAM) domain mutation in a Japanese patient with ankyloblepharon, ectodermal defects and cleft lip and palate (AEC) syndrome without ankyloblepharon. Br J Dermatol 149(2): 395-399.
- Pinheiro M, Freire-MN (1994) Ectodermaldysplasias: a clinicalclassificationand a causal review. Am J Med Genet 53(2):153- 162.
- Drut R, Pollono D, Drut RM (2002) Bilateral nephroblastoma in familiar Hay-Wells syndrome associated with familial reticulate pigmentation of the skin. Am J Med Genet 110(2): 164-169.






























