A Comparison of Automated Refractions Using Plusoptix S04 Photoscreener, Nidek AR-20 Handheld Autorefractor and Nidek ARK-510A Auto Ref-Keratometer
Tania Baban A, Fady Sammouh K, Haytham El Ballouz M and Elias Warrak*
Department of Ophthalmology, University of Medical Center, Lebanon
Submission: January 26, 2017; Published: April 04, 2017
*Corresponding author: Elias Warrak L, FASCRS, Advanced Eye Care Hospital Naccach, Lebanon, Tel: +961-3-310828; Fax: +961-1-424221; Email: advancedeyecare.ew@gmail.com
How to cite this article: Tania A B, F K Sammouh, Haytham M El B, Elias L W. A Comparison of Automated Refractions Using PlusoptiX S04 Photoscreener, Nidek AR-20 Handheld Autorefractor and Nidek ARK-510A Autoref-005 keratometer. JOJ Ophthal. 2017; 2(4): 555594. DOI: 10.19080/JOJO.2017.02.555594
Abstract
Purpose: To evaluate automated refraction measurements using the Plusopti X S04 photo screener (OP), Nidek AR-20 hand held auto refractor (NAR) and compare them to the more traditional Nidek ARK-510A (ARK).
Methods: 102 patients aged 3 to 81 years were included. All patients underwent on-cycloplegic automated refraction using the PlusoptiX S04 photo screener, Nidek AR-20 handheld auto refractor and the Nidek ARK-510A. This was followed by measuring Cyclo plegic auto refraction using the Nidek AR-20 handheld auto refractor and Nidek ARK-510A.
Results: Without Cyclo plegia, the mean sphere values were significantly different for both the OP (-0.41 D, SD±2.39D) versus ARK (-0.60D, SD±2.24) groups with a p=0. 008, and for NAR (-0.48, SD±2.01) Versus ARK groups with a p=0.029. With cycloplegia, there was no significant difference in the mean sphere values between the OP versus ARK groups as compared to the OP versus NAR and NAR versus ARK groups (p=0.049 and p=0.001 respectively).
Conclusion: Our study indicates similarities between the OP photo screener and the traditional table-mounted ARK results after cycle plegia. These results were not reflected when comparing the NAR handheld auto refractor to the ARK. Although efficient as screening tools, we recommend caution when using handheld instruments.
Keywords: Refractometer; Refractive errors; Myopia; Hyperopia; Astigmatism; Cycloplegia; Middle east; Lebanon
Introduction
Refraction is a clinical test used to determine the refractive state of the eye and to assess the individual's need for visual aid. Although hretinoscopy is still considered the gold standard for determining the refractive state of the eye, it is subject to interobserver variability [1,2]. Over the past few decades, new advancements have introduced the auto refractors which have gained a popular routine use among ophthalmologists [3,4]. Auto refractors are easy to use, time saving and relatively accurate in measuring the amount and type of refractive error. Today, many auto refractors are available in the market (Canon, Nikon, Topcon, Carl Zeiss Meditec, Nidek etc.). A disadvantage of most auto refractors is they need to be mounted on a table due to their relatively large size. As such, ametropia measurements may therefore be difficult in bed ridden patients, disabled persons and very young or handicapped children. Handheld auto refractors or photo screener scans are useful in such scenarios.
Plusopti XS04 (OP) (Plusoptix GmbH; Nuremberg, Germany), is a third generation vision screener designed to screen for refractive errors, anisocoria, and strabismus in children starting at the age of 6 months [5]. Screening is quick with both eyes screened simultaneously and can be performed by non-medical personnel, with a screening distance of 1 meter [5]. The device measures refraction, pupil size, and corneal reflexes. Results with abnormal limits are displayed as "refer". Referral criteria include anisometropia, astigmatism, hyperopia, myopia, anisocoria and corneal reflexes [5].
To date, multiple studies show that the OP vision screener is useful when used in screening for amblyopia oramblyogenic risk factors [6-10] small-angle strabismus [11] is considered effective when compared to cycloplegic pediatric ophthalmic evaluation [9,10] and can be used to screen patients with intellectual disability foramblyogenic risk factors with 95% sensitivity and 50% specificity [12].
In our manuscript, we explore the accuracy of both the OP vision screener when used as suggested in noncyclopleged patients, the Nidek AR-20 (NAR) (NidekCo. Ltd, Gammagori; Aichi, Japan) handheld auto refractor on non cyclopleged and cyclopleged patients and compare the results with those obtained before and after cycloplegia using a more traditional table- mounted NidekARK-510A (ARK) autorefractor/keratometer (NidekCo. Ltd, Gammagori, Aichi, Japan).
Materials and Methods
We prospectively evaluated 102 consecutive patients presenting to the outpatient clinic during August 2013, without any bias to their age, gender, diagnosis or previous medical history. Patients were excluded if they could not be refracted because of poor cooperation or any ocular pathology. After the initial history was taken, a trained ophthalmology fellow (H.B) and professional optometrist (J.H) used all 3 instruments to obtain non Cyclo plegic automated refraction. This was followed bycycloplegia using 1 drop of Mydriacyl (tropicamide 1%, Alcon, Puurs, Belgium) in each eye twice (10 minute interval). Twenty to 30 minutes later, Cyclo plegic auto refraction was obtained using the ARK, and NAR auto refractors.
Data entry and statistical analysis were performed using SPSS 22.0 for Windows (SPSS Inc, Chicago, IL, USA). Analysis variables included:gender, age (years), auto refraction (sphere, cylinder, axis) and spherical equivalent for both eyes. For each of the 3instruments, the data were divided into 4 main categories: sphere, cylinder, axis and spherical equivalent. Spherical equivalent (sphere power+(0.5 x cylinder power)) measured in diopters was calculated from the auto refraction measurements. For the ARK and NAR handheld auto refractor, data were further divided into non cycloplegic and Cyclo plegic auto refractiCases with missing variables were excluded from the analysis. Two types of statistical testing were used to determine differences or similarities between the OP, NAR handheld auto refractor, and the ARK. Analysis of variance (ANOVA) testing was performed to compare the 3 groups. A variable ratio (F) was calculated to determine overall statistical differences. Paired-samples t-tests were performed to compare means between 2 groups. Significance was defined as p values less than or equal to 0.05.
Results
One hundred two patients (204 eyes) were initially recruited. Nineteen eyes (9.3%) could not be refracted by OP (one patient could not be refracted for both eyes by neither OP nor the NAR) and were excluded from the analysis. A total of 185 eyes completed the study on all 3 instruments and were included in the analysis (45.7% males, 54.3% females). The patients ranged in age from 3 years to 81 years (mean 41.02±19.7years, median 43 years).Using OP, the mean recorded sphere on 185 eyes was -0.41 diopters, mean cylinder was +1 diopters, and mean axis were measured at 90.6° (Table 1). The median spherical value was Plano (range -6.75 to +10). The mean spherical equivalent determination of the OP group was +0.09 diopters (range -6.125 to +10.5). A myopic spherical value was found in 47.6% of the eyes 42.7%were hyperopic and 9.7% were plano. Astigmatism was identified in 96.8%
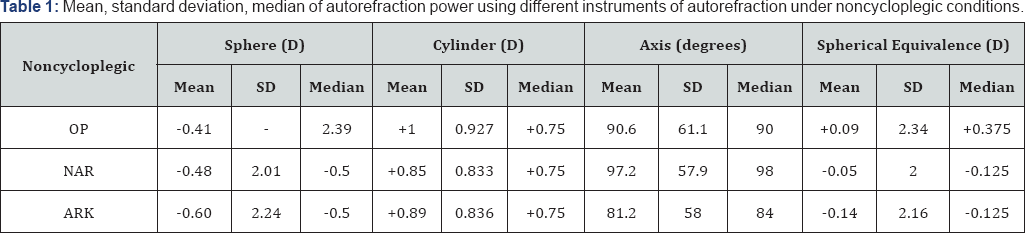
OP:PlusoptiX S04 (Plusoptix GmbH; Nuremberg, Germany); NAR: Nidek AR-20 (Nidek Co.Ltd, Gammagori; Aichi, Japan); ARK: Nidek ARK-510A (NidekCo.Ltd, Gammagori; Aichi, Japan).
Non cycloplegic auto refraction results for nidek AR-20 handheld autorefractor and nidek ARK-510A
The mean sphere value recorded by the NAR for 185 eyes was -0.48 diopters, mean cylinder was+0.85 diopters, and mean axis were 97.16°. The median spherical value was -0.5 diopters (range -6.75 to+8.5). The mean spherical equivalence for the NAR group -0.05 diopters (range -6.125 to+9.12). A myopic spherical value was identified in 60.5%; 33.5% were hyperopic, and 5.9% were Plano. Astigmatism was identified in 91.9% (Table 3). The mean spherical value recorded using the ARK on 185 eyes was -0.604 diopters, mean cylinder was +0.89 diopters, and mean axis measurement was 81.2° (Table 1). The median spherical value was -0.5 diopters (range -6.25 to+10.5). The mean spherical equivalence measured in this group was -0.136 diopters (range -4.875 to+1G.875). A myopic spherical value was diagnosed in 61.1%, 3G.3% were hyperopic, and 8.6% were Plano. Astigmatism was identified in 95.7% of 185 eyes (Table 3).
Cycloplegicautorefraction results for nidek AR-20 handheld autorefractor and nidek ARK-510A
The mean sphere value recorded by the NAR for 185 eyes was -0.266 diopters, mean cylinder was +0.837 diopters, and mean axis were 91.3° (Table 2). The median spherical value was Plano (range -5.75 to+10.5). The mean spherical equivalence for the NAR group +0.145 diopters (range -4.75 to+10.875). A myopic spherical value was diagnosed in 48.6%, 41.6% were hyperopic, and 9.7% were Plano. Astigmatism was identified in 97.3%. The mean spherical value recorded using the ARK on 185eyes was -0.40 diopters, mean cylinder was +0.86 diopters, and mean axis measurement was 79.95° (Table 2). The median spherical value was -0.25 diopters (range -6.25 to+10.5). The mean spherical equivalence measured in this group was +0.05 diopters (range -4.875 to+10.875). A myopic spherical measurement was diagnosed in 52.4% of eyes, 35.1% were hyperopic, and 12.4% were Plano. Astigmatism was identified in 95.7% of eyes (Table 4).
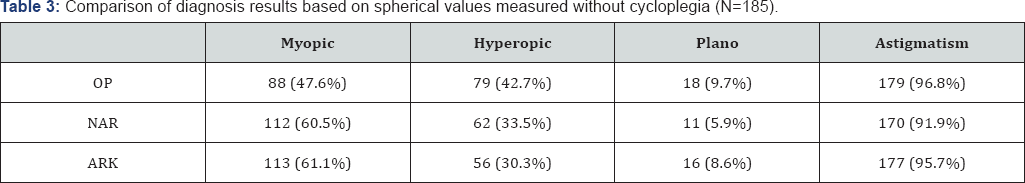
OP: PlusoptiX S04 (Plusoptix GmbH; Nuremberg, Germany); NAR: Nidek AR-20 (NidekCo.Ltd, Gammagori; Aichi, Japan); ARK: Nidek ARK-510A (NidekCo.Ltd, Gammagori; Aichi, Japan).
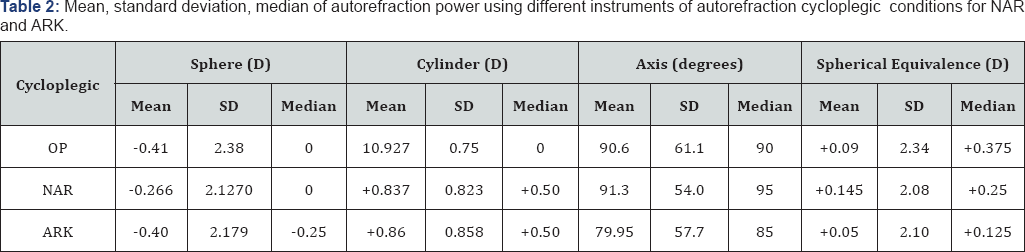
Optix: PlusoptiX S04 (Plusoptix GmbH; Nuremberg, Germany); C-NAR: cycloplegic-Nidek AR-20 (NidekCo.Ltd, Gammagori; Aichi, Japan); C-ARK: cycloplegic- Nidek ARK-510A (NidekCo.Ltd, Gammagori; Aichi, Japan).
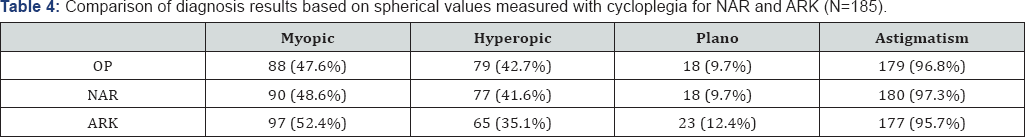
Optix: PlusoptiX S04 (Plusoptix GmbH; Nuremberg, Germany); C-NAR: Cycloplegic- Nidek AR-20 (NidekCo.Ltd, Gammagori; Aichi, Japan); C-ARK: Cycloplegic- Nidek ARK-510A (NidekCo.Ltd, Gammagori; Aichi, Japan).
Except, of the axis value, ANOVA testing for auto refraction parameters of all instruments before cycle plegia revealed no significant difference among the 3 groups (Table 5). While paired-samples t-test comparisons of OP and NAR sphere values showed no statistical significance (p=0.34). Comparisons of sphere values for OPversus ARK and NAR versus ARKwere statistically significant (p=0.008 and 0.03 respectively) (Table 5) . Paired-samples t-test comparisons of cylinder values of NAR versus ARK showed similar results. However, the OP versus NAR and OP versus ARK groups showed a significant difference (p= 0.002 and p=0.025 respectively) (Table 5). The axis value analysis by ANOVA revealed a significant p-value (p= 0.034), indicating an overall significant difference between the 3 groups. Conversely, paired-samples t-test results were only significant between the NAR and ARK groups (p=0.001) (Table 5).
Calculated spherical equivalence measurements did correlate with our initial sphere measurements in the NAR versus ARK groups. Paired-samples t-test comparisons between the OP versus ARK demonstrated a difference with a p= 0.002. When comparing the OP versus NAR and the NAR versus ARK groups, no statistical difference was observed (Table 5).
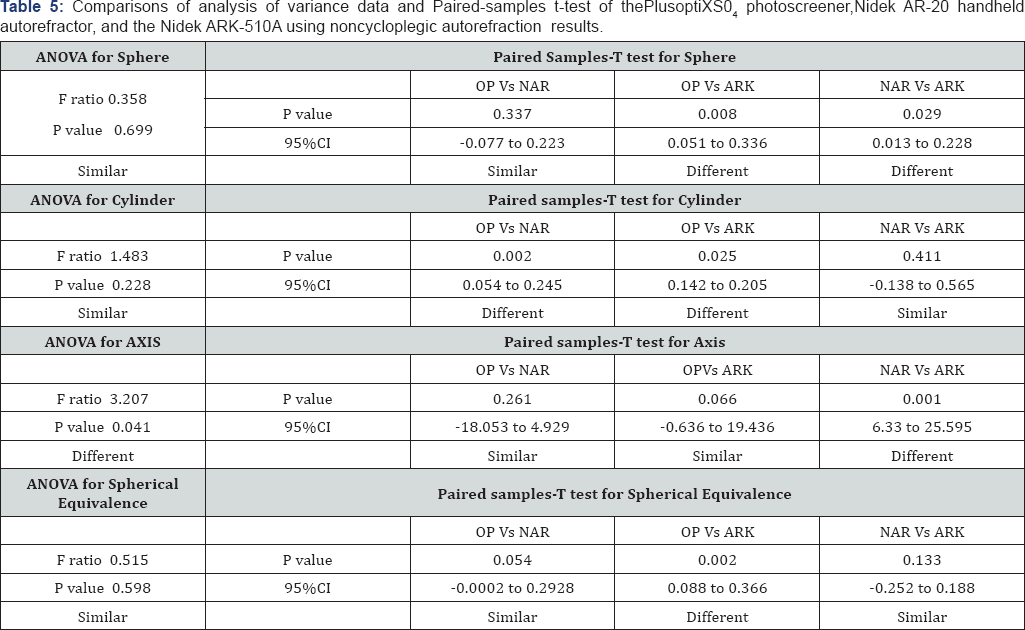
ANOVA: analysis of variance test; CI: confidence interval; F: Variance ratio; OP: PlusoptiX S04 (Plusoptix GmbH; Nuremberg, Germany); NAR: Nidek AR-20 (NidekCo.Ltd, Gammagori; Aichi, Japan); ARK: Nidek ARK-510A (NidekCo.Ltd, Gammagori; Aichi, Japan).
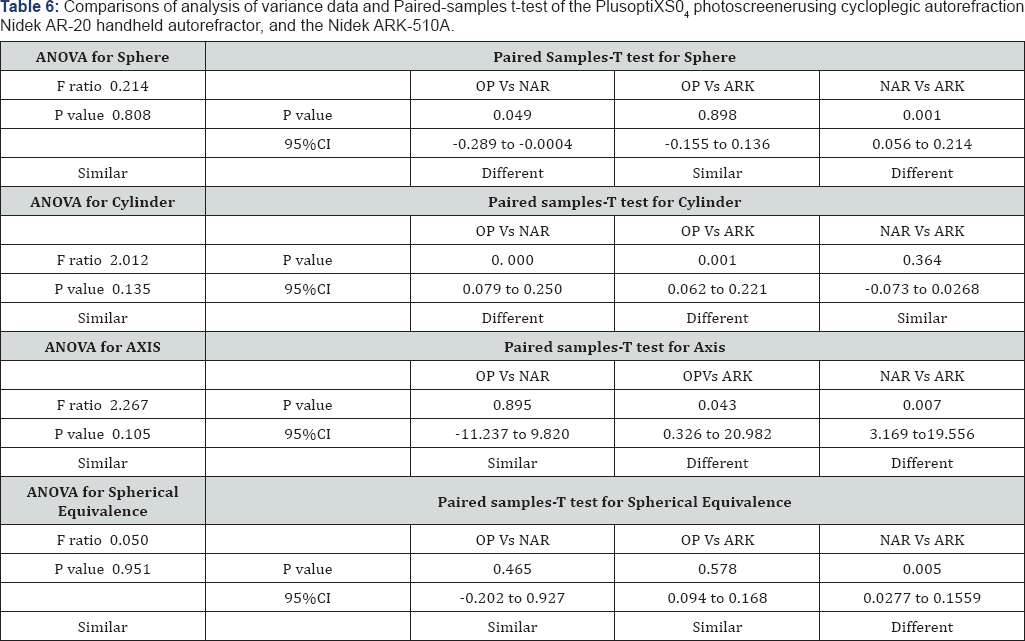
Data from the NAR and ARK instruments were reassessed using Cyclo pelagic autorefractions (C-NAR and C-ARK); ANOVA testing for all refraction parameters did not indicate any statistical differences (Table 6). Similarly, paired-samples t-test comparisons showed comparable results among the OP versus C-ARK groups. However, there was a statistical significance in OP versus C-NAR and C-NAR versus C-ARK groups (p= 0.049 and 0.001 respectively) (Table 6). Paired-samples t-test for the cylinder values of the OP versus the C - NAR group and OP versus C-ARK indicated statistical differences (p=0. 000 and p =0. 001) (Table 6).
For Axis values, paired-samples t-test comparisons of OPversus C-NAR values were statistically similar, whereas those of OP versus C-ARK showed a significant difference (p= 0.04). The C-NAR axis value compared to that of the C-ARK also showed a significant difference (p= 0.07) (Table 6). Finally, when analyzing spherical equivalence, paired-samples t-test comparisons showed similar results except for the C-NAR versus C-ARK group which showed a significant difference with a p=0. 005 (Table 6).
Discussion
Although considered as the gold standard for measuring refractive status, Cyclo pelagic refractions can be time consuming, cause patients discomfort and adds additional costs. As amblyopia is one of the leading causes of visual impairments in adults [13] developing accurate, easy to use, friendly autorefractors that do not require the use of cytoplegic agents could help in identifying significant refractive errors more rapidly and efficiently while avoiding the drawbacks of cycloplegia.As new instruments for refractive error measurements become available, it is of critical importance to evaluate and compare their validity to that of existing reliable technology. The OP photo screener has been marketed toward health care providers as a tool to assess refractive errors in young children without cycloplegia [5,9,10]. Although many studies showed that the OP vision screener is useful as a screening tool for amblyopia or amblyogenic risk factors [6-10] Dahlmann-Noor et al argue that the use of OP as a single screening test in children may miss a significant number of children with amblyopia or amblyogenic risk factor [14].
As in other studies, we found that both the OP vision screener and NAR handheld auto refractor were simple and user friendly, as well as quick in reporting refraction result without the need for direct contact or patient compliance. However, limitations that we encountered while using the OP included the need for a dimly lit room to obtain proper measurements, and its inability to obtain measurements in patients with a number of ophthalmologic conditions. Of the 19 eyes that failed autorefraction by the OP, 6 had a high refractive errors (more than -5), 4 had a history of cataract surgery, 2 had a history of cataract surgery and corneal rings for keratoconus (also failed autorefraction by NAR), 2 had a history of diabetic retinopathy, 1 had a history of a corneal ring for keratoconus, while the remaining 4 had no known ocular problems but were read as "pupil undetected". Disadvantages similar to those claimed by Rajavi et al which may have limited our use included: pupil size, fixation problems and posterior segment pathologies [15]. Limitations with the NAR were mostly a failure of patient cooperation resulting in no measurements being taken especially in children. A child's ability to hold the head still limited our ability to produce repeatable measurements.
The ARK table-mounted auto refractor readings were more frequently myopic compared to the OP and NAR (Table 3 & 4). This may be explained by the fact that it is well known that auto refractive instruments tend to overestimate myopia and underestimate hyperopia [10]. Except for the axis value prior to cycloplegia, when comparing all 3 instruments using ANOVA, our data indicated that there was no significant difference in auto refraction results before and after cyloplegia (Table 5 & 6). Comparing the OP spherical values with values obtained before cycloplegia using the NAR and the ARK indicated that there was a significant difference between the OP and the ARK groups as well as the NAR and ARK groups. This may lead us to conclude that the two handheld instruments may not be as reliable as the well established ARK for diagnosing refractive errors. In contrast, however, the results from both handheld instruments were similar (Table 5). Although the above mentioned results were reflected in the calculated spherical values for both the OP versus ARK and OP versus NAR groups, the NAR versus the ARK group showed similar results.
After cycloplegia on NAR and ARK, our spherical values indicated a difference between OP versus C-NAR and the C-NAR versus C-ARK groups (Tables 6). However, there was no difference between the OP and C-ARK values. Our study results are consistent with data from other studies that claim the OP to be a screening tool to assess refractive without the need cycloplegia [5,9,10]. While in both the cyclopleged and non cyclopleged groups, the OP recorded myopia less often than those recorded by the NAR and the ARK, astigmatism recordings were more comparable in all 3 groups (Table 3 & 4). The astigmatic (cylinder) readings were statistically similar between all 3 instruments by ANOVA however, paired samples-T test detected a difference between the OP and both the NAR and ARK groups before and after cycloplegia (Table 5 & 6). These results could mean that with regards to diagnosing astigmatism (measuring cylinder values) the OP may not be as reliable as the ARK as compared to the NAR.
Although handheld refractors are proving to be more practical, time efficient and provide a value as screening tools, we suggest that they should be used with caution when determining automated refractions especially in children. In the era of refractive surgery, it is important to assess the reliability and reproducibility of newer instruments when compared to existing technology and should not compromise the accuracy of the refractive state of a patient at the expense of practicality and time saving. We do not recommend the use of the hand held instruments for diagnostic purposes, with the exception of remote or inaccessible areas where portable instruments are essential and cycloplegia is difficult.
A positive aspect of our study setup is that our study population was non bias to age during recruitment. To our knowledge the Optixphotoscreener has only been extensively studied in screening younger population groups. This study may give us a better analysis of the use of the open adult patients. Several limitations are inherent in our study. In view of the time constraints and the difficulty of getting young children and elderly patients to cooperate and concentrate for long durations, repeated measurements on all 3 instruments were not documented. Furthermore, and for the same reason of time constraint, two separate individuals obtaining measurements on the handheld instruments may have introduced inter-observer bias. Finally, the same observer documenting measurements from both the handheld and table-mounted auto refractor was not masked to subjective refraction readings, introducing possible observer bias.
References
- Bharadwaj SR, Malavita M, Jayaraj J (2013) A psychophysical technique for estimating the accuracy and precision of retinoscopy. Clin Exp Optom 97(2): 164-170.
- Zadnik K, Mutti DO, Adams AJ (1992) The repeatability of measurement of the ocular components. Invest Ophthalmol Vis Sci 33(7): 2325-2333.
- Decarlo DK, Mc Gwin G, Searcey K, Gao L, Snow M, et al. (2013) Trial frame refraction versus auto refraction among new patients in a low- vision clinic. Invest Ophthalmol Vis Sci 54(1): 19-24.
- Wesemann W, Dick B (2000) Accuracy and accommodation capability of a handheld autorefractor. J Cataract Refract Surg 26(1): 62-7G.
- https://plusoptix.com/en/vision-screener
- Matta NS, Singman EL, Silbert D (2008) Performance of the Plusoptix vision screener for the detection of amblyopia risk factors in children. J AAPOS 12(5): 49G-492.
- Matta NS, Arnold RW, Singman EL, Silbert DI (2009) Comparison between the plusoptix and MTI Photoscreeners. Arch OphthalmolDec 127(12): 1591-1595.
- Arthur BW, Riyaz R, Rodriguez S, Wong J (2GG9) Field testing of the plusoptix SG4 photoscreener. J AAPOS 13(1): 51-57.
- Matta NS, Singman EL, Silbert DI (2010) Performance of the plusoptix SG4 photoscreener for the detection of amblyopia risk factors in children aged 3 to 5. J AAPOS 14(2): 147-149.
- Matta NS, Singman EL, McCarus C, Matta E, Silbert DI (2010) Screening for amblyogenic risk factors using the PlusoptiX SG4 photoscreener on the indigent population of Honduras. Ophthalmology 117(9): 1848185G.
- Strauss R (2006) Off-label use of the Visionscreener® to detect small angle strabismus. Z Prakt Augenheilkd 27: 367-37G
- Ugurbas SC, Alpay A, Tutar H, Sagdik HM, Ugurbas SH (2011) Validation of plusoptiX SG4 photoscreener as a vision screening tool in children with intellectual disability. J AAPOS 15(5): 476-479.
- Simons K (2GG5) Amblyopia characterization, treatment and prophylaxis. Surv Ophthalmol 5G(2): 123-166.
- Dahlmann-Noor AH, Vrotsou K, Kostakis V, Brown J, Heath J, et al. (2009) Vision screening in children by Plusoptix Vision Screener compared with gold-standard orthoptic assessment. Br J Ophthalmol 93(3): 342-345.
- Rajavi Z, Parsafar H, Ramezani A, Yaseri M (2G12) Is noncycloplegicphotorefraction applicable for screening refractive amblyopia risk factors? J Ophthalmic Vis Res 7(1): 3-9.






























