Comparison of pupil diameter measurements: Binocular infrared stand-alone unit vs. monocular Placido-based Keratograph
Anastasios John Kanellopoulos*
Laservision.gr Clinical and Research Eye Institute, Greece
Submission: February 24, 2017; Published: March 20, 2017
*Corresponding author: Anastasios John Kanellopoulos, The Laservision Clinical and Research Eye Institute, Athens, 17 Tsocha Str., 11521, Greece, Tel: , Fax: ; Email: ajk@brilliantvision.com
How to cite this article: Anastasios J K. Comparison of pupil diameter measurements: Binocular infrared stand-alone unit vs. monocular Placido-based Keratograph. JOJ Ophthal. 2017; 2(2): 555585. DOI: 10.19080/JOJO.2017.02.555585
Abstract
Purpose: The purpose of this work is to investigate the repeatability of PROCYON and VARIO while measuring pupil diameter in various situations.
Methods: The pupil diameter of 10 healthy subjects was examined using PROCYON, for scotopic, mesopic high and mesopic low options and VARIO for wide and small pupil. The measurements were repeated 2 times for both eyes of each subject. The contemporary and accurate method of Bland-Altman was used to investigate the repeatability of each device.
Results: According to Bland-Altman diagrams, PROCYON has 0.12±0.37 mean of differences between two tests while Vario 0.061±0.17. From the diagrams it is clear that Variois more stable as a result having better repeatability.
Conclusion: VARIO has been proven to be more trustworthy than PROCYON for measuring pupil diameter.
Keywords: Repeatability; PROCYON; VARIO; Pupil diameter
Introduction
Pupil measurement has been found clinically and has been reported to be a significant modulator in the quality of vision after cornea laser vision correction procedures. With the advent of excimer laser treatments in order to reshape cornea power, the initial broad-beam lasers had a fixed diameter of ablation zone and it was a one-size-fits-all for the different pupillary apertures in photopic, mesopic, and scotopic conditions of patients that had this procedure [1,2].
After several years of experience, it was evident that mismatch of ablation zone to a mesopic and scotopic pupil may have been a significant contributing factor in halos and ghosting experienced by the patients, as well as a mismatch between the pupillary aperture in mesopic and scotopic, and the diameter of ablation on the cornea may exacerbate more decentration issues as a smaller pupil would “forgive” mild and moderate decentrations, where a larger pupil would not forgive even moderate decentrations [3,4].
There are several pupillometry devices dedicated in documenting preoperative and postoperative pupillary size, some of them are monocular such as the Colvard pupillometer, which uses infrared technology for the examiner to manually determine whether the scotopic pupil size of the patient matches a certain circle present in the optics of the examiner. We have for many years employed the Procyon P3000 stand alone desktop binocular pupillometer technology, which measures binocularly the pupil size in photopic, mesopic and scotopic conditions by video photography and digital calculation of the pupillary size produced in a report where the average pupillary size of each eye of the patient evaluated is Schallenberg M et al. [5], Rosen E [6]. We have also been using for the last six years the Vario Keratograph, which is a Oculus 4 Keratograph to adapt with the Wavelight refractive laser suite and provide topography-guided data for the EX500 and 400Hz excimer lasers. This device has the ability to capture the cornea topography and the pupillary parameters in low light and high light illumination, therefore producing two different pupillary sizes, photopic and mesopic, and also to be able to document centroid shift as well. So the purpose of this study was to compare our golden standard up to now over the last 13 years to the Vario pupillometry and try and find possible correlations between the measurements by the two devices [7-10].
Materials and Methods
20 healthy patients were randomly selected, in order to measure their pupil diameter using PROCYON and VARIO. Each eye was measured 2 times forscotopic (0.04 lux), mesopic Low (0.4 lux) and mesopic high (4.0 lux) high using PROCYON and for wide and small pupil option using VARIO. So we created 2 measurement groups, groupl and group2, that were compared using Bland-Altman method. This is a contemporary method for comparing the differences of 2 groups of paired measurements [11-13]. (Figure 1)
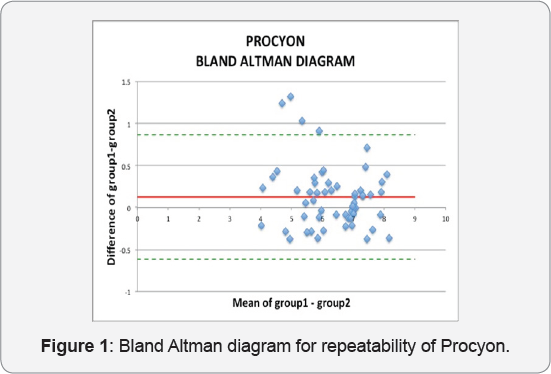
Results
According to Bland-Altman plots, PROCYON has 0.12±0.37 mean of differences comparing two groups while Vario 0.061±0.17 [11,12]. (Figure 2)
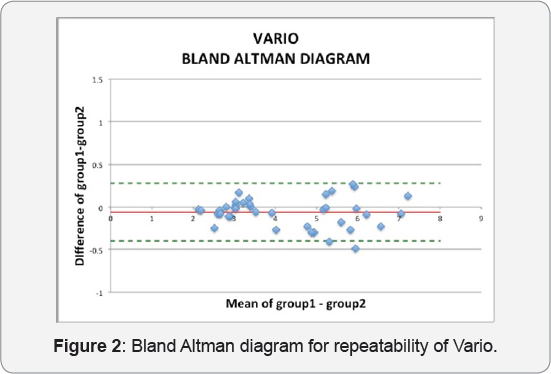
Discussion
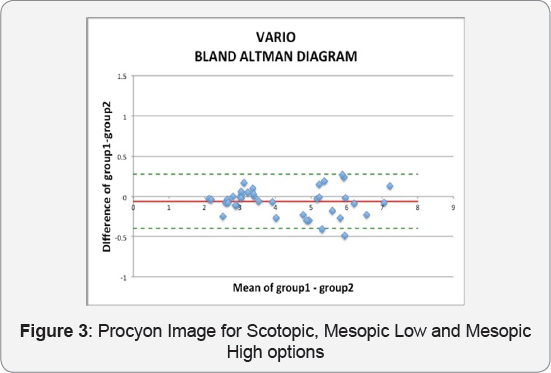
We are very pleased to document in this study that there was a strong correlation found between the scotopic Procyon and the mesopic Vario measurement. We also found, by checking inter-exam accuracy, that the Vario was more stable and had a higher repeatability, and we would suggest that future pupillometry devices would potentially share the same technology with the Vario Keratograph in, ideally a binocular fashion, in order to be able to document both pupillary apertures in these two or even more illumination settings, document centroid shift with the same high repeatability. (Figure 3)
The clinical relevance for the clinician is that since corneal topography with this placido-based device is a cornerstone of evaluation, treatment, and postoperative management of laser cornea refractive surgery patients, these data can be extrapolated by the clinician to also give accurate pupillometry measurements and therefore potentially help with the surgical planning and/or postoperative assessment of potential visual complaints of the patients. (Figure 4)
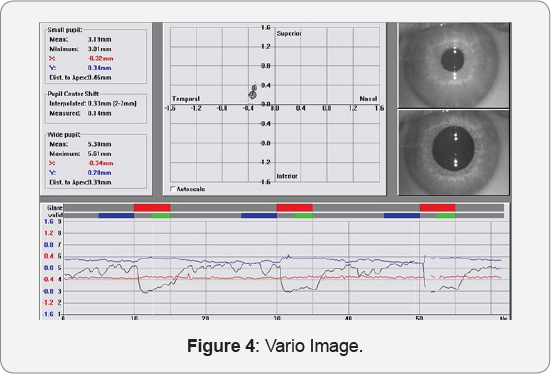
Conclusion
In this work we investigated the repeatability of Procyon and Vario concerning the repeatability in measuring pupil diameter. According to the results presented, Vario has a better repeatability that means that is more trustworthy measuring pupil diameter in order to make more accurate treatment plans for refractive or cataract operations.
References
- Schmitz S, Krummenauer F, Henn S, Dick HB (2003) Comparison of three different technologies for pupil diameter measurements. Graefe’s Arch Clin Exp Opthalmol 241(6): 472-477.
- Wickremasinghe SS, Smith GT, Stevens JD (2005) Comparison of dynamic digital pupillometry and static measurements of pupil size in determining scotopic pupil size before refractive surgery. J Cataract Refract Surg 31(6): 1171-1176.
- Bootsma S, Tahzib N, Eggink F, de Brabander J, Nuijts R (2007) Comparison of two pupillometers in determining pupil size for refractive surgery. Acta Ophthalmol Scand 85(3): 324-328.
- Michel AW, Kronberg BP, Narváez J, Zimmerman G (2006) Comparison of 2multiple-measurement infrared pupillometers to determine scotopic pupil diameter. J Cataract Refract Surg 32(11): 1926-1931.
- Schallenberg M, Bangre V, Steuhl KP, Kremmer S, Selbach JM (2010) Comparison of the Colvard, Procyon, and Neuroptics pupillometers for measuring pupil diameter under low ambient illumination. J Refract Surg 26(2): 134-143.
- Rosen E (2010] Pupillometry using the procyon pupillometer. J Refract Surg 26(8]: S44.
- Altan C, Kaya V, Basarir B, Celik U, Azman E, et al. (2012) Comparison of 3 pupillometers for determining scotopic pupil diameter. Eur J Ophthalmol 22(6): 904-910.
- Brown SM, Bradley JC (2011) Comparison of 2 monocular pupillometers and an autorefractor for measurement of the dark-adapted pupil diameter. J Cataract Refract Surg 37(4): 660-664.
- McDonnell C, Rolincova M, Venter J (2006) Comparison of measurement of pupil sizes among the colvard pupillometer, procyon pupillometer, and NIDEK OPD-scan. J Refract Surg 22(9Suppl): S1027-S1030.
- Kanellopoulos AJ, Asimellis G (2015) Distribution and Repeatability of Corneal Astigmatism Measurements (Magnitude and Axis) Evaluated With Color Light Emitting Diode Reflection Topography. Cornea 34(8): 937-944.
- Kanellopoulos AJ, Asimellis G, Georgiadou S (2015) Digital pupillometry and centroid shift changes after cataract surgery. J Cataract Refract Surg 41(2): 408-414.
- Kanellopoulos AJ, Asimellis G (2013) Comparison of high-resolution Scheimpflug and high-frequency ultrasound biomicroscopy to anterior-segment OCT corneal thickness measurements. Clin Ophthalmol 7: 2239-2247.
- Kanellopoulos AJ, Asimellis G (2013) Comparison of Placido disc and Scheimpflug image-derived topography-guided excimer laser surface normalization combined with higher fluence CXL: the Athens Protocol, in progressive keratoconus. Clin Ophthalmol 7: 1385-1396.






























