Eplerenon as Adjunctive Therapy for Choroidal Neovascularisation with Serous Pigment Epithelial Detachment and Subretinal Fluid in Age Related Macular Degeneration
Ceklic Lala* and Latinovic Slobodanka
Eye Clinic, Vidar Orasis, Serbia
Submission: February 16, 2017; Published: February 17, 2017
*Corresponding author: Lala Ceklic, Vidar Orasis, Bulevar Cara Lazara 79b21000 Novi Sad, Serbia, Email: lala@oftalmolog.ba
How to cite this article: Ceklic L, Latinovic S. Eplerenon as Adjunctive Therapy for Choroidal Neovascularisation with Serous Pigment Epithelial Detachment and Subretinal Fluid in Age Related Macular Degeneration. JOJ Ophthal. 2017; 1(5): 555574. DOI: 10.19080/JOJO.2017.01.555574
Abstract
Objective: To investigate possible effect of eplerenon 50 mg in serous pigment epithelial detachment (sPED) and subretinal fluid (SF) resolution after initial intravitreal application of 2 mg aflibercept in treatment of neovascular age-related macular degeneration (nAMD).
Method: Case presentation of two females with occult choroidal neovascularisation with sPED due to the nAMD treated with three consecutive intravitreal injections of 2 mg aflibercept. On control check up 6 weeks after last injection, per oral 50 mg Eplerenon (Inspra) once daily is prescribed. For follow up we used visual acuity, intraocular pressure, Amsler grid test, color fundus (CF), optical coherence tomography (SD OCT) baseline, 6 weeks after last intravitreal injections, 6 weeks after initiation of eplerenon as well as potassium serum concentration 6 weeks after initiation of eplerenon therapy is monitored.
Results: Morphologic improvement evident in reduction of central macular thickness and height of sPED >10% followed with stabile visual acuity was registered in both patients after 6 weeks of eplerenon prescription.
Conclusion: Eplerenon given as adjunctive therapy for treatment of sPED in nAMD could have beneficial effect but further more detailed and more controlled clinical investigations are recommended.
Keywords: Serous pigment epithelial detachment; Eplerenon; Neovascular age related macular degeneration
Introduction
Serous pigment epithelial retinal detachment (sPED) is sharply demarcated, smooth, dome shaped elevation of retinal pigment epithelium (RPE) [1]. SPEDs are manifestation of neovascular age related macular degeneration (nAMD), polypoidal choroidal vasculopathy (PCV) and central serous chorioretinopathy (CSR). Controversy remains about etiology of sPEDs [2-5]. The over activation of the mineralocorticoid receptor (MR) pathway has been shown to cause fluid accumulation in the retina, choroidal vasodilation, and to promote retinal neovascularization in hypoxic conditions [1-4,6-8]. According the role of mineralcorticosteroid receptors in retina, eplerenon has shown beneficial effect in treatment of CSR [5].
A well-known complication of PED is a RPE tear caused by contraction of the elevated PED and retraction of RPE resulting in absence of RPE underneath the neurosensory retina [5,6]. RPE rip could be serious vision threating complication of laser photocoagulation, photodynamic therapy and anti-VEGF therapy. There is an evidence that sPED with height > 350 ?m are more high risk for development of RPE and consecutive macular atrophy [7]. Anti VEGF is nowdays the main therapeutic approach for nAMD and despite chronic presence of sPED and subretinal fluid in regular and continuous anti-VEGF regimes have comparable and benefitial effect in visual and functional outcome [8]. Due to the costs of antiVEGF and patient compliance with intravitreal injections alternative treatments are rational approach to those cases [5].
Case Presentation
Case series of 2 patients with occult choroidal neovascularisation (CNV) due to the nAMD with sPED >350 чm,treated with three initially consecutive intravitreal injections of 2 mg aflibercept (EYLEA®) in private practice. After 6 weeks after last intravitreal aflibercept therapy per oral Eplerenon 50 mg (INSPRA®) once daily was prescribed as persistent sPED exists and relatively large collection of subretinal fluid (>50 чm) presented in macular region. Both patients are females, age of 71 and 64. Visual acuity baseline 30 ETDRS (Early treatement diabetic retinopathy) letters.
After 12 weeks of last treatment with anti VEGF and 6 weeks after Eplerenon prescription visual acuity was 70 and 75 ETDRS letters respectively. Intraocular pressure was with normal limits during all controls (less than 21 mmHg). Both patients had detailed ophthalomologic examination on all consecutive visits. It included complete anterior segment of the eye exam which was within normal limits in both cases. Fundoscopic exam in mydriatic conditions show soft drusen on both eyes, complete resolution of the blood on eplerenon baseline visit and no blood on consecutive visit in treated eye. Both patients had incomplete posterior vitreous detachment, no vitreoretinal changes. Fellow eye has high risk AMD in younger patient (presence of large soft drusen in macula). In other patient fellow eye has soft drusen and occult juxtafoveal CNV. Both patient were treatment naive.
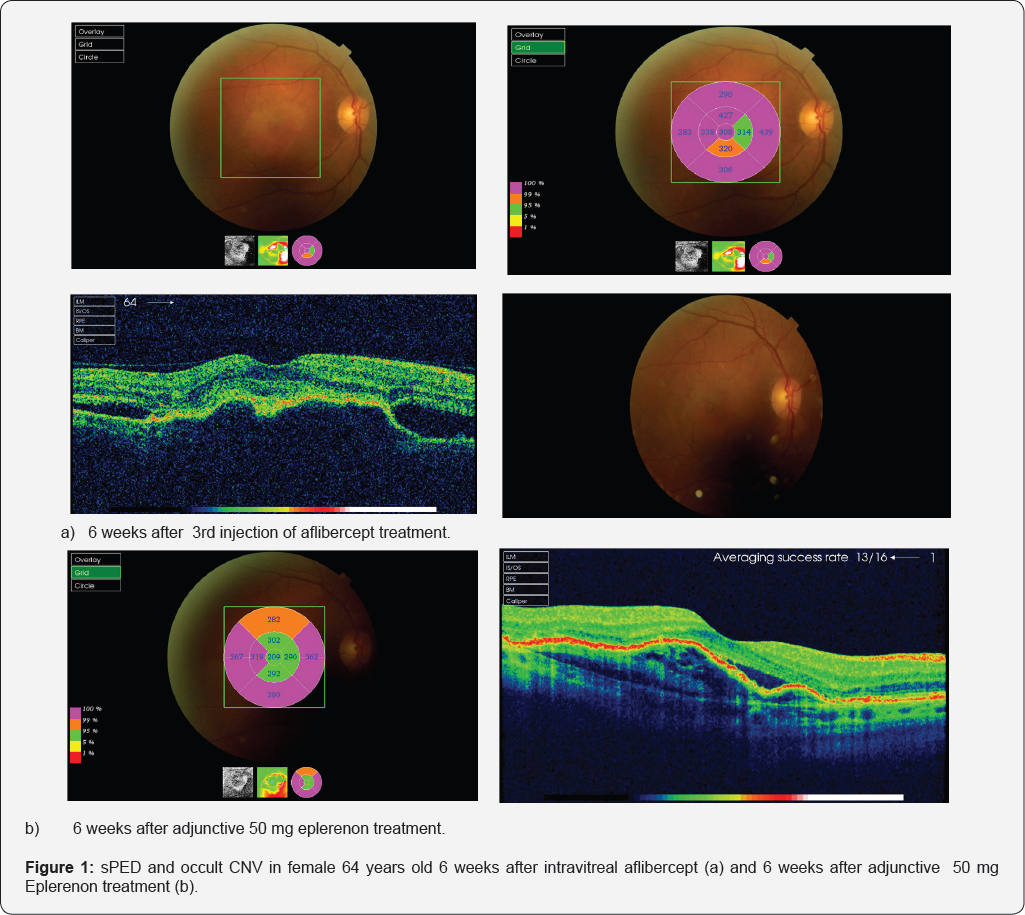
Both patients were previously for 5 years treated with oral beta blockers (metoprolol 25 mg once daily) and ACE inhibitors (enalapril 10 mg twice daily) for arterial hypertension and received statins (atorvastatin 10 mg once daily) for regulation of hyperlipoproteinemia type IIa. Other systemic and ocular health problems were not present. Both patients presented type A personality. Central retinal thickness and central sPED height measured 6 weeks after eplerenon 50 mg treatment and 12 weeks after last intravitreal injection of 2 mg aflibercept seemed to be evidently reduced. Visual acuity during treatment with eplerenon 50 mg was stable through 6 weeks 70 and 75 ETDRS letters respectively. Both patients are educated for self testing Amsler grid, and Amsler grid tests performance was stable and unchanged during all follow up period. Potassium plasma level was monthly monitored in both patients (within normal limits <4,1 mmol/L). Younger patient is now switched to pro re nata (PRN) anti VEGF therapeutic regime, as signs of CNV activity in both cases considered are visual acuity, Amsler grid test, signs of hemorrhage on clinical exam, increase in retinal thickness due to the intraretinal edema on OCT (Figure 1). Other patient refuse further antiVEGF treatment and she is still taking eplerenon combined with antioxidant and vitamin supplements.
Discussion
The purpose of this case presentation is to show effect of eplerenone, a mineralocorticoid receptor antagonist, as a treatment option for reduction of SRF and sPED in cases with nAMD. The role of mineral corticosteroid receptors (MR) in retinal disorders is emerging and the potential association with physiological traits are investigated in CNV. The place of MR antagonists for retinal diseases treatment are discussed [1-4].
Central subfield thickness at follow-up visit after eplerenon initiation significantly decreased more than 10% from baseline which was previously reported in cases with chronic CSR [5]. Following therapy with eplerenon, there was a significant reduction in SF, reduction in CST, and improvement visual acuity in eyes with chronic CSR [5]. A majority of eyes with CSR presented by Singh and al [5] (47.1%) demonstrated stable SRF on treatment, while 35.3% had complete resolution of SRF. Results of this study indicate that eplerenone could be beneficial in the treatment of unresolved CSR. Considering that some cases in nAMD morphologically reminds on CSR could be rational approach to treat those patients with mineralcorticosteroid antagonists with the goal of serous transudation reduction and to reduce number of intravitreal injections which could be serious burden for patients. Also, presence of subretinal and sub RPE fluid is still not mandatory indication for continuous and strict anti VEGF regime. There are evidences that antiVEGF therapy in cases with large serous PED are prone to RPE rip [7,8]. As it is still controversial, there could be some benefit of anatgonists of mineralcorticosteroid receptors in some cases with resistent and non compliant patients with sPED. Further more precise conclusions and role of mineralcorticosteroid receptors in nAMD request more controlled and precise clinical investigations.
References
- Singh RP, Sears JE, Bedi R, Schachat AP, Ehlers JP, et al. (2015) Oral eplerenone for the management of chronic central serous chorioretinopathy Int J Ophthalmol 8(2): 310-314.
- Gruszka A (2013) Potential involvement of mineralcorticoid receptor activation in the pathogenesis of central serous chorioretinopathy: a case report. Eur Rev Med Pharmacol Sci 17(10): 1369-1373.
- Bousquet E, Beydoun T, Zhao M, Hassan L, Offret O, et al. (2013) Mineralcorticoid receptor antagonism in the treatment of chronic central serous chorioretinopathy: a pilot study. Retina 33(10): 2096-2102.
- Behar Cohen F, Zhao M (2016) Corticosteroids and the retina: a role for the mineralocorticoid receptor. Curr Opin Neurol 29(1): 49-54.
- Shaikh AH, Toussaint BW, Miller DM, Petersen MR, Foster RE, et al. (2015) Cost comparison of intravitreal aflibercept with bevacizumab and ranibizumab for the treatment of wet age-related macular degeneration. Ophthalmic Surg Lasers Imaging Retina 46(1): 62-66.
- Chang LK, Sarraf D (2007) Tears of the retinal pigment epithelium: An old problem in a new era. Retina 27(5): 523-534.
- Lehmann B, Heimes B, Gutfleisch M, Spital G, Pauelikhoff D, et al. (2015) Serous vascularized pigment epithelial detachments in exudative AMD. Morphologic typing and risk of tears in the RPE. Ophthalmologe 112(1): 49-56.
- Arora S, McKibbin M (2011) One-year outcome after intravitreal ranibizumab for large, serous pigment epithelial detachment secondary to age-related macular degeneration. Eye (Lond) 25(8): 1034-1038.






























