Corneal Perforation after Uneventful Cataract Surgery Associated with Sjögren’s Syndrome
Mandel L*, Pe’er L, Karmona L, Avizemer H and Achiron A
Department of Ophthalmology, The Edith Wolfson Medical Center, Israel
Submission: December 03, 2016; Published: January 04, 2017
*Corresponding author: Liat Mendel Department of Ophthalmology, The Edith Wolfson Medical Center St. Holon, Israel, Tel: ; Fax: +972-3-5028706; Email: liat.veig@gmail.com
How to cite this article: Mandel L, Pe'er L, Karmona L, Avizemer H, Achiron A. Corneal Perforation after Uneventful Cataract Surgery Associated with Sjogren's 004 s Syndrome. JOJ Ophthal. 2017; 1(4): 555570. DOI: 10.19080/JOJO.2017.01.555570
Case Report
A 77 year old female approached our clinic due to a progressive visual acuity deterioration lasting several years. She has been diagnosed with primary Sjögren’s Syndrome for the last 5 years, with keratoconjunctivitis sicca, Xerostomia and arthritis. Other medical history included ischemic heart disease and hypertension. Her regular medications included Amlodipine, Tritace, Cadex, Cardiloc, Plaquenil 400 mg and artificial eye lubricants (saline tears x6/d and Viscotears® Liquid Gel x1/d). She denied use of punctal plugs or topical cyclosporine use. On her initial examination best corrected visual acuity was 6/30 in the right eye and 6/20 in the left eye. Slit lamp examination showed diffuse superficial punctate ephithelial erosions (SPK). Intraocular pressure (IOP) was 10 in both eyes. The lens had nuclear sclerosis and anterior capsular opacity. The retina showed peripapillary atrophy with mild retinal pigmented epithelium changes. On April 2015 she underwent uncomplicated right eye cataract phacoemulsification with posterior chamber intra-ocular lens (IOL) insertion. First day post operative exam showed no change in visual acuity, cornea with diffuse SPKs, mild descemet membrane folds with +1 cells in the anterior chamber (AC). Postoperative treatment was topical Diclofenac (a local NSAID) and Maxitrol (Neomycin sulphate, polymyxin B sulphate and dexamethazone) drops, 4 times a day each. Artificial tear drops were continued.

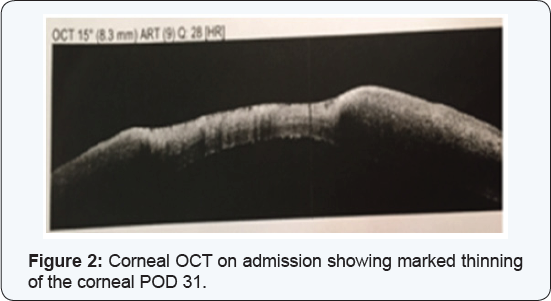
Seven days post operatively, examination revealed that visual acuity remained 6/60 PH 6/30. The cornea had diffuse dense SPKs with epithelial edema and a small bulla appeared on the lower half. The patient was asked to gradually lower the medical treatment dosage. At the next routinely scheduled postoperative examination (post-operative day 30), a large inferior para-central corneal erosion was observed (Figure 1) and corneal OCT showed a significant thinning in the erosion area (Figure2). The patient reported no pain and didn’t notice any vision deterioration. On further history, the patient misunderstood her medical regime and continued both steroidal and NSAIDs drops without lowering the dosage. She was admitted for hospitalization.
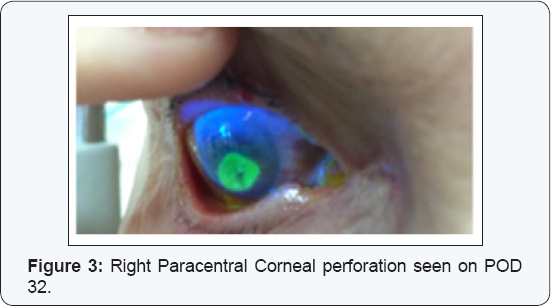
On admission exam visual acuity was 1 meter finger count (FC), the erosion size was 4.5 mm X 4.2 mm, no infiltrate was seen, the AC was clear without cells or flare and the PC-IOL was in place. Serum 20% drops every hour, Erythromycin ointment 4 times a day and oral Doxycycline 100 mg per day were administered. Maxitrol and Diclofenac were discontinued. PCR for Herpes Simplex and bacterial cultures were performed with a negative result. On the second day of admission visual acuity deteriorated to hand motion. Slit lamp examination demonstrated a slightly inferior paracentral corneal perforation (Figure 3). The AC was shallow and the iris prolapsed through the corneal perforation.
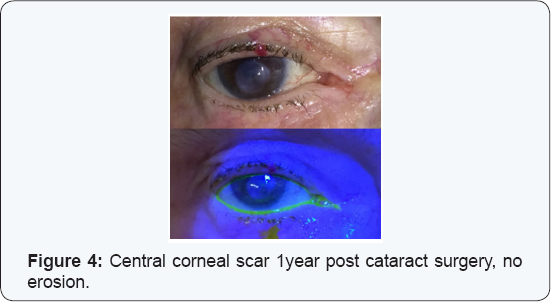
The cornea was glued with cyanoacrylate and a therapeutic contact lens was placed. Considering corneal melting due to an inflammatory systemic disease systemic Prednisone 60 mg per day was initiated. During clinic follow-up the glue remained on the cornea for about 10 months and a therapeutic contact lens was replaced several times. After 10 months the glue fell off, at first with a positive Seidel test but at the concurrent visit there was no more leakage. The cornea remained with a central corneal scar with no erosion (Figure 4) and visual acuity did not improve. The patient and her family were not interested in performing rehabilitative corneal procedures, due to her system illness.
Discussion
Sjögren’s Syndrome is a progressive autoimmune disease characterized by lymphocyte infiltration of the exocrine glands resulting in their fibrosis causing keratoconjunctivitis sicca (dry eyes; 85% of patients) and xerostomia (dry mouth; 90% of patients) with several systemic manifestations, [1]. The disease affects mostly women (9:1 ratio) with median age of 54 years. Positive serum serology for Anti SSA (RO) or Anti SSB (LA) is found in about 60% of patients. The current diagnostic criteria for Sjögren’s syndrome include ocular or oral symptoms and 2 out of 3 the following: Positive serum serology (antiSSA and/or antiSSB or positive rheumatoid factor and antinuclear antibody titer >1:320), salivary gland biopsy showing tipical lymphocytic sialadenitis (with a focus score >1 focus/4 mm2) and keratoconjunctivitis sicca (ocular staining score >3) [1] (Table 1).

The disease is slowly progressing, taking about 10 years from onest until the complete clincal expression is demonsterd[2]. From the ophthalmic point of view the most important symptom is keratoconjunctivitis sicca, secondary to the lack of tears in the eye tear film, with destruction of the corneal and conjunctival epithelium. Treatment is mainly sympthomatic with lubrication or nasolacrimal duct occlusion. Immunomodulatory treatment as local Cyclosporine has also been suggested in difficult cases. For systemic manifastations, treatment may incude Hydroxychloroquine, Methotrexate and Prednisone [2].
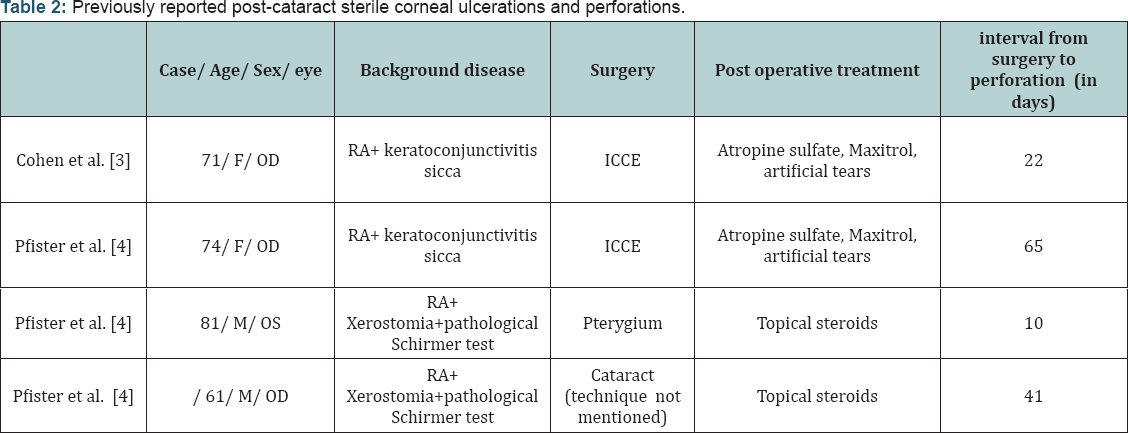
F- Female; ICCE- Intracapsular cataract extraction; RA- Rheumatoid arthritis.
Post-cataract sterile corneal ulcerations and perforations in Sjögren’s patients has been previously reported in only two articles, (Table 2) [3,4]. Cohen et al. [3] reported two females with a prolonged history of rheumatoid arthritis and keratoconjunctivitis sicca that developed painless sterile corneal ulceration and perforation following an uneventful cataract surgery (Intracapsular extraction) [3]. Both patients received postoperative topical steroid drops. As in our case report, perforations occurred within 3 to 8 weeks following surgery. Pfister & Murphy [4] reported on 18 eyes of 14 rheumatoid arthritis and Sjögren’s patients who had spontaneous corneal ulceration and perforation. Two of the case occurred following an anterior segment surgery and topical steroid treatment, one occurred 10 days post Pterygium excision, and the other cases occurred 42 days post cataract extraction (technique not mentioned) [4]. Reasons for the perforations in these cases may be divided to:
- A basic anterior segment disease.
- Surgical damage.
- Post-operative injury by topical corticosteroid/ NSAIDS treatment. Strategies for the timely diagnosis and proper management of dry eye syndrome in the face of cataract surgery patients will be emphasized.
A basic anterior segment disease
Patients with Sjögren’s Syndrome may be at a high risk for complications due to the chronic inflammatory state in the anterior segment. Sjögren’s Syndrome is characterized by tear film abnormality and epithelial damage; both are risk factors for post-operative complications. A study that analyzed corneal innervations and morphology in primary Sjögren’s Syndrome showed that in comparison to controls the corneas of Sjögren’s patients had an irregular and patchy surface epithelium, stromal thinning and that their sub-basal nerve fiber bundles revealed abnormal morphology [5].
Moreover, in a study following 163 Patients with Sjögren’s Syndrome, 13% had vision threatening symptoms- 4.5% had spontaneous corneal melting or perforation during median 3 years follow up, without any ocular surgery [6]. A chronic ocular inflammation state such as in Sjögren, scleritis or uveitis patients should be controlled pre-operatively to minimize the chance of scleral or corneal necrosis. The ophthalmologist can work in conjunction with other physicians involved in the patient’s care to consider systemic therapy with systemic corticosteroid and immunosuppressive agents.
Surgical damage
Anterior segment surgery may cause corneal dryness and damage by mechanism of post-operative corneal denervation and reduced blinking rate. During surgery the cornea is exposed for a long time without blinking which can also contribute to its dryness. Adding ocular surgery to essentially dry eyes was found as a risk factor for complications post anterior segment operations [7,8].
Post operative Topical corticosteroid and Non Steroidal treatment
Severe stromal melting has been reported with the postoperative use of several topical nonsteroidal anti-inflammatory drugs (NSAIDs). The melting is due in part to the epithelial toxicity and hypoesthesia that these drugs can induce. In addition topical steroids suppress corneal wound healing by reducing collagen synthesis [9].
Management of corneal perforation
Persistent epithelial defects accompanied by stromal lysis require intensive treatment with non-preserved topical lubricants. The use of topical medications, particularly preserved medications, should be minimized to reduce epithelial toxicity. Additional treatment modalities to encourage epithelialization and to arrest stromal melting include punctal occlusion, bandage contact lenses, tarsorrhaphy, botulinum injections to induce ptosis, autologous serum eye drops and systemic tetracycline antibiotics [10]. If the disease continues to progress in spite of medical therapy, an amniotic membrane graft or lamellar or penetrating keratoplasty should be considered. Corneal melting may recur even with grafted tissue. For the treatment of any underlying autoimmune disease, systemic immunosuppressive therapy may be needed. To note, the prophylactic use of topical antibiotics must be monitored closely; after a week of application, many topical antibiotics begin to cause secondary toxic effects that may inhibit epithelial healing.
Managing patients with high risk for perforation prior to surgery
Abnormalities in the tear film may have an impact on the ocular surface and thus adversely affect postoperative recovery if not addressed in advance. Bringing the patient to the optimal epithelial state prior to surgery will reduce future post-operative complications. Preoperative excessive lubrications, punctual plugs and even temporal tarsorrhaphy should be considered[11]. During the surgery itself, we suggest frequent hydration the cornea with an irrigating solution or by coating the cornea with a topical viscoelastic agent, in order to reduce such complications. Close observation of these patients during the weeks following surgery is warranted to identify and treat toxic keratoconjunctivitis and corneal ulceration from collagenase activation by postoperative corticosteroid therapy. Topical NSAID should be used with caution and with close monitoring for these patients because they have the effect of reducing corneal sensitivity and thus associated with high risk for corneal melting [9]. In extreme cases, persistent epithelial defects may require a bandage (therapeutic) contact lens, tarsorrhaphy, or amniotic membrane transplant.
Optimizing dry-eye therapy prior to cataract surgery improves visual outcomes [7]. A variety of aqueous layer supportive treatments can be personalized for each surgical candidate, including topical preserved and non-preserved liquid tear preparations, gels, and ointments, topical cyclosporine and punctum plugs. In addition, when planning cataract surgery, the surgeon must evaluate the patient’s ability to comply with the postoperative care regimen.
Conclusion
In this report we have discussed the possible factors for corneal perforation following cataract removal surgery in a patient suffering from Sjögren’s Syndrome. The effects of severe dry eye may be potentiated postoperatively due to interference with lid mobility and corneal denervation, reducing blink rate and post operative treatment with topical NSAIDS and steroids. We hope to raise surgeon’s awareness about the importance of proper evaluation of a high risk patient before, during and after surgery. Meticulously caring for the epithelia may guarantee good results in high risk patients.
Take home message:
- The effects of severe dry eyes may be potentiated postoperatively due to interference with lid mobility and corneal denervation, reducing blink rate and post operative treatment with topical NSAIDS and steroids.
- It is important to consider close observation of patients with any severity of dry eyes.
- Educate patients about the importance of complying with eye drops and attending follow-up.
References
- Shiboski SC, Shiboski CH, Criswell L, Baer A, Challacombe S, et al. (2012) American College of Rheumatology classification criteria for Sjogren's syndrome: a data-driven, expert consensus approach in the Sjogren's International Collaborative Clinical Alliance cohort. Arthritis Care Res (Hoboken) 64(4): 475-487.
- Kassan SS, Moutsopoulos HM (2004) Clinical manifestations and early diagnosis of sjogren syndrome. Arch Intern Med 164(12): 1275-1284.
- Cohen KL (1982) Sterile corneal perforation after cataract surgery in Sjogren's syndrome. The Br J Ophthalmol 66(3): 179-182.
- Pfister RR, Murphy GE (1980) Corneal ulceration and perforation associated with Sjogren's syndrome. Arch Ophthalmol 98(1): 89-94.
- Tuominen IS, Konttinen YT, Vesaluoma MH, Moilanen JA, Helinto M, et al. (2003) Corneal innervation and morphology in primary Sjogren's syndrome. Invest Ophthalmol Vis Sci 44(6): 2545-2549.
- Akpek EK, Mathews P, Hahn S, Hessen M, Kim J, et al. (2015) Ocular and systemic morbidity in a longitudinal cohort of Sjogren's syndrome. Ophthalmology 122(1): 56-61.
- Afsharkhamseh N, Movahedan A, Motahari H, Djalilian AR (2014) Cataract surgery in patients with ocular surface disease: An update in clinical diagnosis and treatment. Saudi J Ophthalmol 28(3): 164-167.
- Chaudhary R, Mushtaq B (2011) Spontaneous corneal perforation post cataract surgery. BMJ Case Rep.
- Aragona P, Di Pietro R (2007) Is it safe to use topical NSAIDs for corneal sensitivity in Sjogren's syndrome patients? Expert Opin Drug Saf 6(1): 33-43.
- Jhanji V, Young AL, Mehta JS, Sharma N, Agarwal T, et al. (2011) Management of Corneal Perforation. Surv Ophthalmol 56(6): 522-538.
- Cosar CB, Cohen EJ, Rapuano CJ, Maus M, Penne RP, et al. (2001) Tarsorrhaphy: clinical experience from a cornea practice. Cornea 20(8): 787-791.






























