Pediatric to Adult Care Transition for Chronically Ill Patients: Introducing the PACT Mobile App
Kimberly Campbell1, Kathryn K Hyatt2 and Olcay Y Jones3*
1Clinic Manager, Pediatric Specialty Service, Department of Pediatrics, Walter Reed National Military Medical Center, USA
2Pediatric Cardiology/Rheumatology RN Coordinator, Pediatric Specialty Clinic, Department of Pediatrics, Walter Reed National Military Medical Center, USA
3Chief, Division Pediatric Rheumatology, Department of Pediatrics, Walter Reed National Military Medical Center, USA
Submission: April 13, 2022; Published: June 14, 2022
*Corresponding author: Olcay Y Jones, Chief, Division Pediatric Rheumatology, Department of Pediatrics, Walter Reed National Military Medical Center, USA
How to cite this article: Kimberly Campbell, Kathryn K Hyatt, Olcay Y Jones. Pediatric to Adult Care Transition for Chronically Ill Patients: Introducing the PACT Mobile App. JOJ Nurse Health Care. 2022; 12(3): 555837. DOI:10.19080/JOJNHC.2022.12.555837
Abstract
Pediatric subspecialties care for chronically ill children that often requires long term treatment and monitoring. In many cases, it can be challenging to successfully prepare the youngster and parent and complete the transfer of care to adult care specialist. We developed a mobile app, Pediatric to Adult Care Transition or PACT, to promote practice and skills building that can be personalized for the patient and supervised by a medical provider.
Abbreviations: WRNMMC: Walter Reed National Military Medical Center; DHA: Defense Health Agency
Introduction
The transition of care for adolescent and young adult patients from pediatric care providers to adult care providers is many times a complex process. This process is further confounded in patients with chronic illnesses. Currently over 90% of children with special health care needs require transition services as their life expectancy continues to grow [1]. During this precarious time of transitioning healthcare, patients tend to have problems establishing care with adult providers. This in turn can result in poor medication compliance and appointment no shows which may ultimately result in direct health impacts including disease flares, dangerous infections, health complications and even death [1].
The American Academy of Pediatrics along with an endorsement from the American Academy of Family Physicians and the American College of Physicians published a report on the process of Health Care Transition and the importance of supporting patients throughout this transition process. This report emphasized nine different principles to facilitate successful transition and from this a variety of tools were developed to help aid in transition including the Six Core Elements of Health Care Transition [2]. These Core Elements provide a structured process that healthcare clinics can use to implement the transition process for pediatric patients while also allowing for customization based on patient and family needs.
The Core Elements, provide a variety of tools to help in the transition process. These tools include questionnaires and handouts to be given to patients and their parents at in person visits throughout the transition process. Accordingly, the transition process begins around the age of 12 where patients are initially introduced to care transition and it should then be reviewed regularly to prepare patients and their parents. The current practice is based on screening patients regularly to assess their readiness for the transition to adult healthcare. In addition, patients undergo education on their disease process, disease management as well as self-management and advocating for themselves in their future healthcare appointments. During this critical time of transition, it is imperative to prepare not only patients but their parents as well they prepare for this change [3]. Thus, the transition process itself involves patients, parents, and a broad interdisciplinary team.
Conclusion
It is widely recognized that the transition process by the medical team has high impact on many children to become productive adults after experiencing long term health problems. For the limited work-force available within the pediatric subspecialties, however, it is practical to utilize digital and reliable open-source resources to maximize the efficacy of interventions. In the adolescent population, mobile, on-the-go, applications are extremely helpful in promoting self-management, especially in the technology focused generation going through the transition process [4]. Based on this observation, we designed the Pediatric to Adult Care Transition (PACT) app to introduce the transition process to patients and parents (Figure 1). It includes a screening questionnaire to assess user readiness for transition that is organized under four domains, i.e., foundation, knowledge, communication, and ownership. This allows personalized schedule and training that can be guided in practice by a medical provider. Assignment of to-do items under each domain can be customized based on the need-gap followed by a progress review during a return visit. The data on readiness assessment overtime is important to provide feed-back to the family and tailor the support. The end goal is to assist patients in skill development and confidence building.
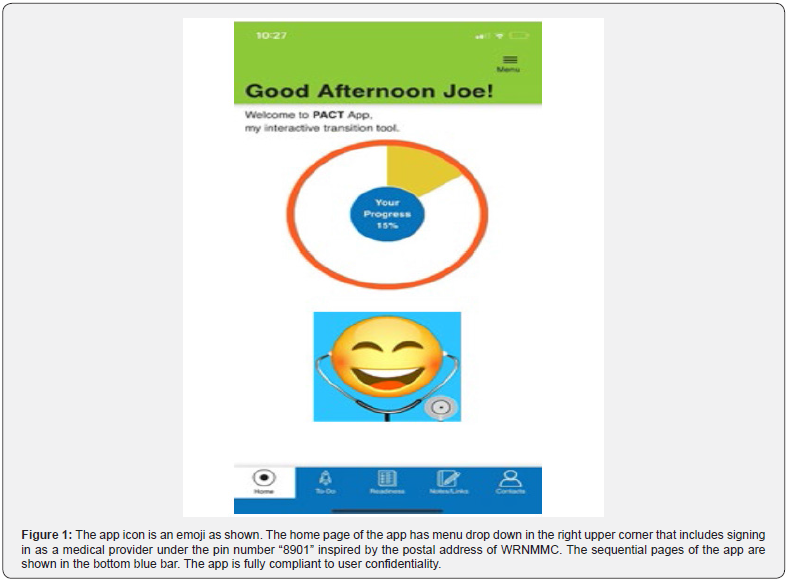
Technology adaptation is helpful, but it is critical to accomplish the training based on a solid foundation through well-structured clinical practice. To our experience, nursing staff has been the backbone of the transition program providing a friendly, but assertive, environment for both the youngster and the parent to understand the process and engage in productive communications. Initial face to face review of core concepts of transition process is essential and continuing one to one engagement remains as the key element for successful outcomes.
In summary, mobile apps are promising tools to promote self-learning and real-life practice while the youngster is still under the supervision and guidance by the parent and medical team. Digital tools may also allow adaptations of telemedicine blended within the transition process to circumvent access to care. Future research is needed on cross-disciplinary and cross-cultural perspectives of transition to improve the mobile tools and therefore end-user experience. This, in turn, can contribute to large scale data collection on quality of control measures for successful completion of the transition process in collaborations with the adult care providers.
Acknowledgement
We extend our thanks to Ms. Catherine Myrick at WRNMMC Office of Command Communications and the DHA Mobile Technology Program Group at Joint Base Lewis-McChord for their crucial contributions in developing this mobile app. We also thank Dr. Patience White for her critical review of the manuscript and thank Autoinflammatory Alliance for kindly promoting the App among the families. We sincerely appreciate the support and funding of this manuscript by Next Generation Medicine, a nonprofit dedicated for the advancement of technology in patientcentered care.
Conflict of Interest
No potential conflicts of interest to disclose
PACT MOBILE APP
Disclaimer
The views expressed in this article are those of the author(s) and do not necessarily reflect the official policy of the Department of Defense or the U.S. Government.
References
- Sabbagh S, Ronis T, White PH (2018) Pediatric rheumatology: Addressing the transition to adult-oriented healthcare. Open Access Rheumatol 10: 83-95.
- White Ph, Cooley WC (2018) Transition Clinical Report Authoring Group, American Academy of Pediatrics, American Academy of Family Physicians, American College of Physicians. Supporting The Health Care Transition from Adolescence to Adulthood in The Medical Home. Pediatrics 142(5).
- Katz JD, Mamyrova G, Agarwal S, Jones OY, Bollar H, et al. (2011) Parents’ perception of self-advocacy of children with myositis: an anonymous online survey. Pediatr Rheumatol Online J 9(1): 10.
- Virella Perez YI, Medlow S, Ho J, Steinbeck K (2019) Mobile and web-based apps that support self-management and transition in young people with chronic illness: Systematic review. J. Med. Internet Res 21(11).






























