Decreasing Falls in the Emergency Department by Implementing the use of Voice Activated Stretcher Alarm Pads.
Denise Cadle Rhew1* PhD,RN,CNS,CEN and Jason Upham2 MSN,RN,CEN
1Clinical Nurse Specialist, Cone Health, USA
2Department of Emergency, Cone Health, USA
Submission: December 28, 2018; Published: January 23, 2019
*Corresponding author: Denise Cadle Rhew, Clinical Nurse Specialist, Research Chair Cone Health, USA
How to cite this article: Denise C R, Jason U. Decreasing Falls in the Emergency Department by Implementing the use of Voice Activated Stretcher Alarm Pads. .JOJ Nurse Health Care. 2019; 10(2): 555785. DOI:10.19080/JOJNHC.2019.10.555785.
Keywords: Falls; Stretcher alarm; Voice Activated alarm; Emergency department; Emergency nurses
Introduction
Over 3 million emergency department (ED) visits are from older adults aged 65 and older due to having a fall [1]. Just in the emergency department alone patient falls have sky rocketed with increase in the number visits, especially those patients being treated aged 65 and older. Approximately 17% of adults living in the community age 65 and older have at least one treat-and-release ED visit each year. Data has shown that one in three older adults recently discharged from the ED, that return to the ED, are admitted to the hospital, sent to a nursing home, or die within 90 days after being treated and released from their ED visit [2]. Falls have huge impact within the emergency departments regarding injury, length of stay, health care cost, and quality of life [3]. In the emergency department there are many times where patients arrive with some form of altered mental state, this can be due to various reasons such as intoxication, impaired by drugs/medications, or medical diagnosis. In this, mental state patients are at a high risk for falls with or without injury.
Currently the practice is to attempt to find a staff member to sit with the patient to prevent patient from falling. The Agency for Healthcare Research and Quality 2016 identified that one-third of fall events can be prevented with appropriate screening tools and the use of appropriate safety intervention devices [4]. Since 2008, the Centers for Medicare & Medicaid Services eliminated payment to hospitals for costs incurred in treating injuries resulting from falls during hospitalization. The Joint Commission has prompted organizations to implementing fall safety interventions for all patient settings [5]. One study by McErlean & Hughes (2016) [6] identified drug use (73.9%), impaired mobility (58.7% and altered mental status (56%) as being factors that increase the risk for falls in the emergency department [6]. As mentioned in the article by Ward (2014) [7], effectiveness of a bed alarm system to predict falls have been explored in the acute care setting and interventions have been mostly targeted for the acute impatient areas to prevent falls [7]. Falls tend to occur in acute inpatient care settings in the patient room area; generally, around the bed and/or in bathrooms and majority of these falls are not observed [7,8]. Emergency departments are becoming more of a holding area for many patients who are waiting to be admitted due to lack of bed availability and staffing shortage. With ED nurses, having the burdened to care for patients holding to be admitted, there is a greater need to address interventions to prevent falls in the emergency department. In this same study, it was suggested that there is a need for more research to identify when the use of a bed alarm system is appropriate for the patient, and helpful to the nurse [8].
Emergency Department nurses are primarily responsible for the patient while they are being seen and treated. In addition, ED nurses are held to making sure that their patients are kept safe and receive the appropriate care while waiting in a noisy, busy, overcrowded ED [9]. The purpose of this article is to present the impact of a pilot study with the implementation of voice/alarm activated stretcher pads to decrease falls in the emergency department. In addition, this article will share staff perception for patient’s safety pre and post study and the perception of family member’s perception of the use of emergency department specific stretcher voice/alarm intervention. Stretcher voice/alarm pad use in the emergency setting to prevent falls have not been previously studied. Bed alarms are common in the in-patient world, but not in emergency department settings. The primary reason is the use of stretchers not electric hospital beds in the ED setting
The pilot study took place in a community hospital, which is part of a private, not for profit healthcare system located in the Southeastern United States. Specifically, the study was conducted in a 25 bed Emergency Department, nine triage/minor care, and eight transition rooms that sees approximately 65,000 patients a year. All ED nurses and any patient that was consider a high fall risk during their stay in the ED were included in the study. The purpose of this pilot study was to keep patient safety first, utilize innovation with new advancements in technology of stretcher bed alarms, while transforming the way we monitor our patient’s safety.
Method
The pilot study did received approval from the hospital Institutional Review Board (IRB) prior to implementation. Patients were assessed upon their arrival to the ED and throughout their visit for their risk for fall using our current approved fall assessment tool located in the electronic medical record. Patients with a high fall risk score were provided a stretcher alarm/ voice activated pad. The stretcher alarm pad was placed under the patient and then connected to the Hill-Rom bed/nurse call monitoring system, which was attached to the bed. Patients were assessed for any potential skin breakdown before, during and after use of these pads.
If a patient attempted to get out of bed, the alarm made a loud audible sound via the alarm system box as well as through the nurse call bell system. In addition, a voice activated alarm would say to the patient lay back down, do not get up. This voiceactivated alarm could be a generic voice or a recording of a family member’s voice.
ED staff responded immediately to the room to assess and maintain patient safety. The staff member completed the survey tool at the disposition of the patient. This survey tool consists of four parts: a) Demographics. b) Capture the patient and staff experience of using the stretcher alarm system. c) Staff will survey family regarding their perception of how safe did using the stretcher alarm make them feel about their potential for falling. d) Product utilization questions prior to implementation of the study. A group of five ED RN’s was selected to assist in validating if the education provided to staff and the stretcher alarm evaluation tool was appropriate.
Results
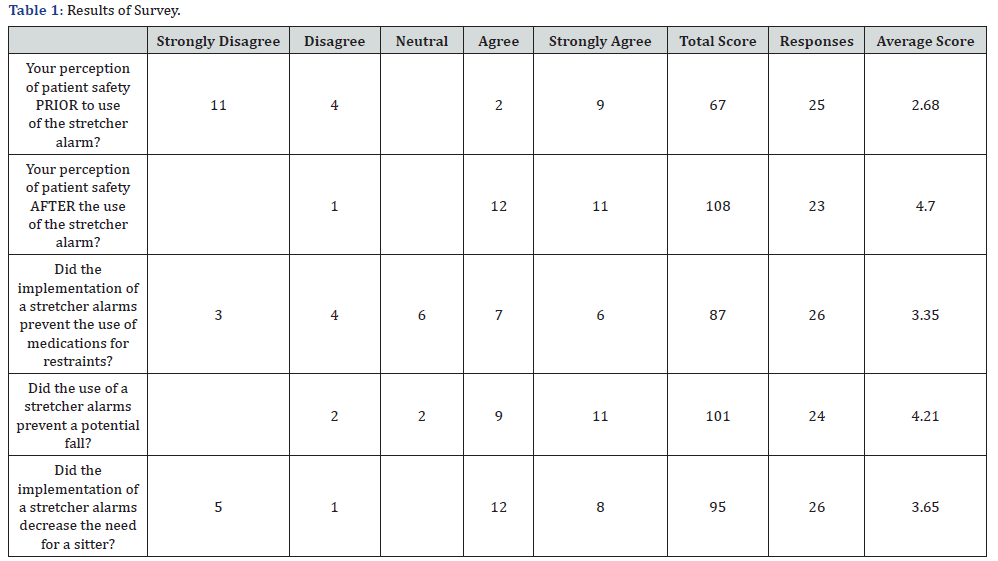
This pilot study was prompted due to an increase in falls with injuries from FY 2015 total falls were 7 falls with injury and in FY 2016 we had a total of 35 falls for our five-system emergency department. Falls rate for FY 2017 with injury was 11 and FY 2018 was 10 classified as an injury. Our pilot was done within one of our community hospitals. Due to our positive results from our study, the alarm pads were implemented in all of our emergency departments system-wide. We had a total number of 25 responses received from our pilot survey over a 4-week period. Nurse perception of patient safety prior to the use of the stretcher alarm using a Likert scale of strongly agree to strongly disagree was 2.68 and their perception after the use of the stretcher alarm showed to improve significantly with a score 4.70.
Family members were asked an open ended question prior to patient’s disposition in regards to their perception of did they feel the use of the alarm/voice activated pad provided an extra safety net for their love’s ones. All family members responded with a definite yes. Their response to the question did the implementation of the stretcher alarm prevent the use of medications for restraints 13 out of 25 answered agreed or strongly agreed with total score of 3.35. The response to the question did the stretcher alarm prevent a potential fall and 20 out of 25 reported agree or strongly agreed with a total score of 4.21. The last question asked did the utilization of the stretcher alarm decrease the need for a sitter and 20 out of 25 reported agreed or strongly agreed with a total score of 3.65. There were no falls with injury during the pilot study in the ED where the study was held. The results also showed there were no alterations noted in skin integrity while using the pad. See table 1 for the summary of the results
Implications to staff
Employee’s perception regarding patient safety prior to inception of this study was 2.68 and post study significantly improved to 4.70. The key finding showed that by providing an additional resource (stretcher alarm pads) for the staff it has shown to be beneficial in decreasing medication use and provided another safety net for staff to help to prevent fall potential. The pilot study also encouraged the other emergency departments in our system to provide stretcher alarms pads for staff to initiate on their high-risk fall patients. The main limitations of our study were that it was only piloted in one of our Emergency departments.
Discussion
A dearth of literature on stretcher alarm use in the emergency department; exists our findings confirm that the use of stretcher alarms in the ED setting can have an impact on falls and falls with injury. Nurses shared that the alarm allowed them to return to patient’s room quicker and prevent the patient from getting out of bed or to intervene to prevent them from falling. The findings also showed that staff felt that using the stretcher alarm pad decreased medication usage which sometimes was a reason a patient would fall due altering their cognitive ability. This study also adds evidence that the use of the stretcher alarm pad with its connection to the Hill-Rom nurse call system allowed them to respond to patients quicker to prevent a potential fall. Staff felt that with the audible voice alarm system providing commands to the patient to lay back down or to tell the patient to use their nurse call button helped to keep patient safe.
Conclusion
Patient safety is vital in order to achieve quality health care outcomes. Undesirable events such as falls, together with mortality and morbidity, are considered as negative outcomes associated with poor quality of care. Falls have been reported to be among the most common type of inpatient accidents and now with the increase need to hold patients in the ED falls have increased in this patient care setting that compromises patient safety. The use of a stretcher alarm in the ED setting are needed due to several reasons; patients’ reluctance to bother nurses, 50% of patients presenting with acute delirium symptom, 45% patients presenting with dementia with cognitive decline and healthcare staff being very busy and may not be able to respond to their call lights promptly.
The use of a stretcher alarm system is therefore an additional safety measure to ensure that ED nurses are alerted to patients trying to get up from high ED stretchers when the patient does not call for assistance. Our study has however demonstrated objectively, an overall reduction in nurses’ workload, provided an extra resource fall intervention in the ED, received positively by family members and shown to be beneficial in decreasing the amount of sedation medications given as a restraint, with the introduction of the stretcher voice/alarm pads (Table 1).
Method
Patients were assessed upon their arrival to the ED and throughout their visit for their risk for fall using the John Hopkin’s approved fall assessment located in the electronic medical record. Patients with a high fall risk score were provided a stretcher alarm pad. The stretcher alarm pad was placed under the patient and then connected to the Hill-Rom bed/nurse call monitoring system, which was attached to the bed. Patients were assessed for any potential skin breakdown before, during and after use of these pads. If a patient attempted to get out of bed, the alarm made a loud audible sound via the alarm as well as through the nurse call light system. ED staff responded immediately to the room to assess and maintain patient safety. The staff member completed the survey tool at the disposition of the patient.
Results
Nurse perception of patient safety prior to the use of the stretcher improved significantly from 2.68 score to 4.70 with implementation of the Stretcher Alarm/pad. Thirteen out of 25 respondents agreed that the use of medications decrease its use as a restraint. Twenty out of 25 staff shared that the stretcher alarm prevented a potential fall with a score of 4.21 and that a sitter was not need with a score of 3.65. The findings also showed no alteration noted in skin integrity while using the pad.
Conclusion
The key finding is that the pilot study has showed that with providing an additional resource (stretcher alarm pads) for the ED nurse has shown to be beneficial in decreasing medication use as a restraint and provided another safety net for staff to help to prevent potential falls. This pilot study also encourages the other EDs within our system to provide stretcher alarms pads for staff to initiate on their high risk fall patients.
References
- Take Stand of Falls. CDC Centers for Disease Control and Prevention.
- Centers for Disease Control and Prevention (2013) The state of aging and health in America.
- Ruby Z, Chu, RN, CCRN (2017) Preventing In-patient Falls, The Nurse Pivotal role. Nursing 47(3): 24-30.
- Wong C, Recktenwald AJ, Jones ML, Waterman BM, Bollini ML, et al. (2011) The Cost of serious fall-related injuries at three midwestern hospitals. Jt Comm J Qual Patient Saf 37(2): 81-87.
- The Joint Commission (2015) Preventing falls and fall-related in health care facilities. Sentinel Alert Event 55: 1-5.
- Mc Erlean DR, Hughes JA (2016) Who falls in an adult emergency department and why – A Retrospective Review. Australas Emerg Nurs J 20(1): 12-16.
- Smith-Ward P, Barrett L, Rayon K, Govro K (2014) Effectiveness of a bed alarm system to predict falls in an acute care setting. Sciedu 3(1).
- Subermaniam K, Welfred R, Subramanian P, Karauthan C, Fatimah I, et al. (2016) The Effectiveness of a Wireless Modular Bed Absence Sensor Device for Fall Prevention among Older Inpatients. Front Public Health 4: 292.
- Rhew DC, Letvak S, McCoy TP (2017) The Effects of an Educational Intervention on Emergency Nurses’ Attitudes, Knowledge, and Care Behaviors toward Older Adults. BJSTR 1(7): 1-7.






























