A Study to Assess the Prevalence of Antipsychotics Non-Adherence and it's Associated Factors Among Patients with Schizophrenia in Hiwot Fana Specialized University Hospital, Harar, Ethiopia, 2017
Sumesh k, Dr Sanjay T* and Henock A
School of Nursing and Midwifery, College of Health and Medical Sciences, Haramaya University, Harrar, Ethio
Submission: December 12, 2017; Published: March 22, 2018
*Corresponding author: Dr Sanjay T, School of Nursing and Midwifery, College of Health and Medical Sciences, Haramaya University, Harrar, Ethiopia, Email: thomassanjay994@gmail.com
How to cite this article: Sumesh k, Dr Sanjay T, Henock A.A Study to Assess the Prevalence of Antipsychotics Non-Adherence and it's Associated Factors Among Patients with Schizophrenia in Hiwot Fana Specialized University Hospital, Harar, Ethiopia, 2017. JOJ Nurse Health Care. 2018; 6(5): 555700. DOI: 10.19080/JOJNHC.2018.06.555700
Abstract
Non adherence to antipsychotic medication severely affects the efficacy of the treatment and acts as important modifier of health system effectiveness. It has significant negative economic and clinical effects which are manifested by frequent relapses and re-hospitalizations. The aim of this study is to assess the prevalence of antipsychotics medications non adherence and its associated factors among the patients with schizophrenia in Hiwot fana specialized university hospital from February to march 2017 Institutional based cross sectional study was conducted at Hiwot fana specialized university hospital on schizophrenic patients. A total 154 of patients were selected by non-probability convenient sampling technique. Self-Structured and interviewer administered MARS (medication adherence rating scale) questionnaires were used by data collectors. A total of 154 schizophrenic patients were included in this study and all of them were analyzed. This study found a prevalence of antipsychotics medication non adherence in HFSUH was 39.6%. 66.88% were male and 33.12% were females and 57.79% of participants were lived in urban and the rest were in rural. The factors significantly associated with non-adherence are, forgetfulness (OR=5.85), carelessness (OR=11.24), stop if better (OR=6.51), stop if worse (OR=15.87), take when only sick (OR=6), feeling weird like zombie (OR=3.4) and medication side effect (OR=3.85). This study found a prevalence of antipsychotic medication non adherence among patients with schizophrenia which is a significant high value. The findings of this study imply that psycho education could be helpful to improve adherence to antipsychotic medication in schizophrenia.
Keywords: Anti-psychotic medication; Non- adherence; Schizophrenia and Ethiopia
Abbreviations: MARS: Medication Adherence Rating Scale
Introduction
Non adherence is a poly faceted problem but triadic model relating therapeutic relationship between the patient and clinician, factors related to the medications and factors related to patients and their illness help to explain non adherent behavior Golin CE et al. [1]. The consequences of non-adherence are mainly manifested and expressed through clinical and economic indicators. Clinically it means an increase in the rate of relapse and re-hospitalization. As per one study non adherent patients have about a 3.7 times high risk of relapse within 6 months to 2 years as compared to patients who are adherent Fenton Ws et al. [2]. Unfortunately, there is no agreed consensual standard to define non-adherence. Problems with adherence can include taking excess medication, but this is less common, and this review is concerned with those who take less medication than prescribed. Schizophrenia is a clinical syndrome of variable, but disruptive, psychopathology that involves cognition, emotion, perception and other aspects of behavior Kaplan Saddocks [3]. Although non-adherence is a problem throughout medicine. There are several factors that make it especially challenging in schizophrenia. These includes lack of illness awareness (insight), direct impact of symptoms includes depression, cognitive impairment and positive and negative symptoms, social isolation, co morbid substance misuse and stigma Cramer JA et al. [4]. A burden of non-adherence in Africa is also high, for example, a study from Nigeria reported that the prevalence of non-adherence is 40.3% in schizophrenic patients Abiodun O et al. [5]. A study from Ethiopia in Jimma University reported that the prevalence of non-adherence among adult psychiatric outpatients is 41.2%, non-affective psychosis contributing the highest rate (44.5%) from total non-adherent respondents Kenfe Tesfaye et al. [6]. According to available evidences, non-adherence to psychiatric medication is high and is one of the priorities of public health problems needing attention. Therefore, the purpose of this study is to assess the prevalence of antipsychotic non-adherence and its associated factors among schizophrenic patients at HFSUH in harar To assess the prevalence of antipsychotics non adherence and associated factors among patients with schizophrenia at HFSUH, Harar Ethiopia from February to March 2016 [7-10].
Methodology
An institutional based cross sectional study was conducted at HFSUH located in Harrar regional state from February to March 2017.The study population was schizhophrenic patients who attended outpatient unit at HFSUH. The sample size was 154 patients and Non-probability convenient sampling technique was used. A structured questionnaire was used to collect the data on socio demographic characteristics (age, sex, residence to home, marital status, religion, ethnicity, education level, occupation, living circumstance and income per month) [1120]. The Medication Adherence Rating Scale (MARS) used to provide simple and reliable tool in non-adherence. This standard questionnaire was used to measure the level of non-adherence and attitude towards medications.
Results
Results Section 1: Sociodemographic Information
A total of 154 schizophrenic patients were interviewed ,among them 66.88% were male and 33.12% females,33.12% and 25.97% were aged between 26-33 and 18-25 respectively. 45.45% were single and 38.11% are married, 32.47% of them had primary education and 27.27% secondary education. Muslims accounted 48.05% and 34.42% orthodox. Majority of the ethnicity was Oromo which accounted 52.60% and Amhara was 28.57%. 37.01% are unemployed, 24.68% were private employers and 23.38% are farmers. 61.69% of them lived with parents, 20.78% was with spouse and 12.34% of them lived with sibling. 57.79% of participants are lived in urban and the rest of them in rural. 55.19% of the participants had <500 birr per month [21-32]. Among 154 schizophrenic patients , 61(39.6%) are non adherent to antipsychotics medication and 93(60.4%) were adherent to antipsychotic medication. Among this 13.38% had medication side effect 10.3% of them had forgetfulness , carelessness accounted 9.14%, feeling weird like zombie marked 8.49%, stop if worse and stop if better accounted 7.59 % and 7.46% respectively[33-39].
Section 2: Substance Use (Table 1)
Section 3: Medication Adherence Rating Scale(MARS)(Figure 1)
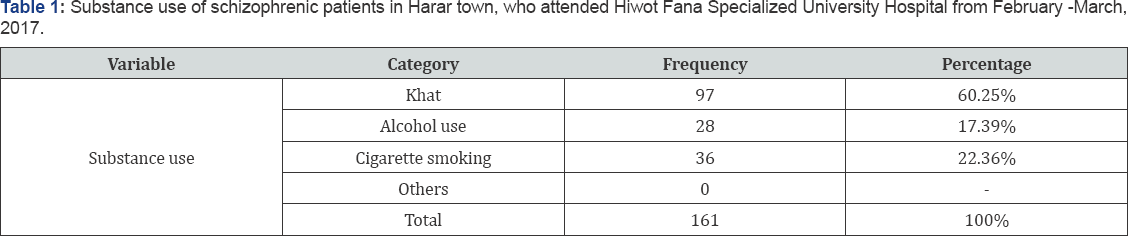
Among 154 patients 60.25 % were Khat chewers, 17.39 % drinks alcohol and 22.36% are cigarette smokers.
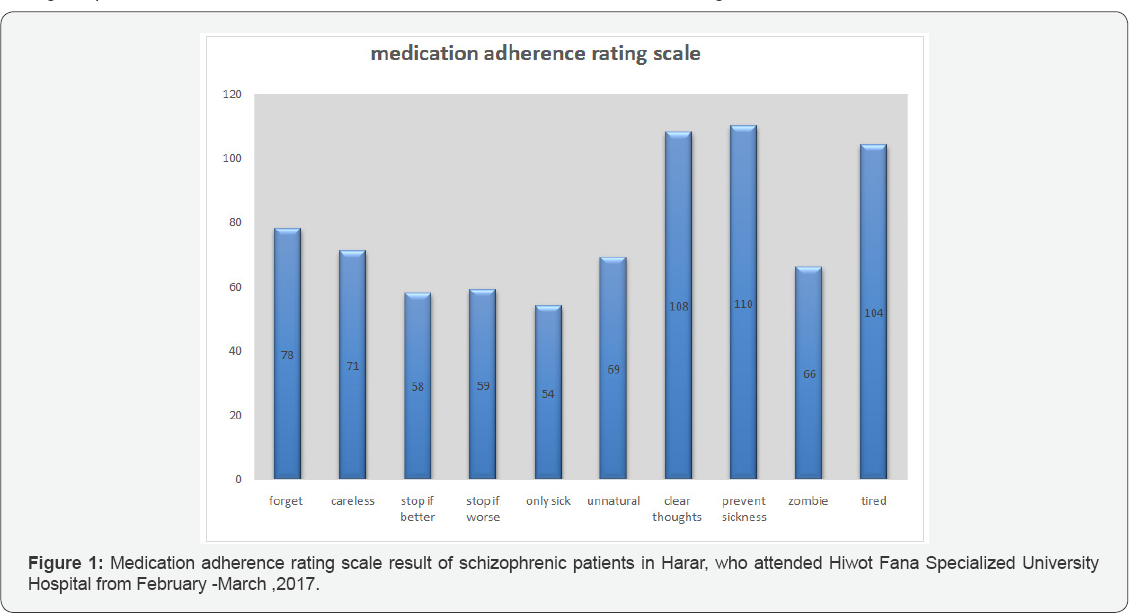
Section 4: Factors Associated with Antipsychotic Medication Non Adherence
Sociodemographic Characteristics: Among the total schizophrenic patients those who were male had 1.03 times increased risk of non-adherence than females and being from rural were also 1.15 times increased risk of antipsychotic medication non adherence than urban residence. Factors such as age, marital status, religion, ethnicity, educational status, occupation and income per month had no significant association with antipsychotic medication non adherence according to this finding [40-42].
Substance Use (Table 2)
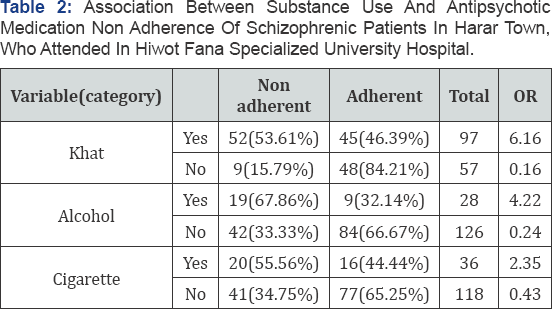
Medication Adherence Rating Scale Association (Table 3)

Conclusion
The study analyzed the prevalence of antipsychotic medication non adherence among patients with schizophrenia attending at HFSUH was 39.6%, which is a significantly higher than the other studies. The associated factors found to have link with antipsychotic medication non adherence are forgetfulness, carelessness, stop if better, stop if worse, take when only sick, feeling weird like zombie and medication side effect. The other positively factors are include being male, rural residence and substance use .The findings of this study implies that psycho education would be helpful to improve adherence towards antipsychotic medication in schizophrenia.
References
- Golin CE, Liu H, Hays RD, Miller LG, Beck ck, et al. (2002) A prospective study of predicators of adherence to combination antiretroviral medication. Gen intern med 17(10): 756-765.
- Fenton Ws, Blyler CR, Heinssen RK (1997) Determinants of medication compliance in schizophrenia. Emperical and clinical findings, schizophrenia Bulletin 23(4): 637-651.
- Kaplan Sadocks' (2007) synopsis of psychiatry behavioral sciences/ clinical psychiatry (10th edn) 51(4): 331.
- Cramer JA, Rosenheck R (1998) compliance with medication regimens for mental and physical disorder. phsychiatr serv 49(2): 196-201.
- Abiodun Adewuya, AdebayoErinfolami, Owoeye Olugbenga, Etop Etim (2009) Prevalence and correlates of poor medication adherence amongst psychiatric outpatient and south western Nigeria. General hospital psychiatry 31(2): 167-174.
- Kenfe Tesfay, Eshetu Girma, Alemayehu Negash, Markos Tesfaye, Sandra Dehning (2011) Medication non adherence among adult psychiatric out patient in Jimma University specialized hospital, southwest Ehiopia. Ethiop J Health Sci 23(3): 227-236.
- Abyot Endale, Esileman Abdela, Basher allele, Ermias Cheru, Bemnet Amogne (2014) Rate of non-adherence to antipsychotic medication and factors leading to non-adherence among psychiatric patients in Gonder university hospital. Advances in Psychiatry
- AO Adelufos, TO Adebowale, Abayomi O,Mosanya JT (2012) Medication adherence and quality of life among Nigerian out patient with schizophrenia. Gen Hosp Psychiatry 34(1): 72-79.
- Black HR (1999) Will better tolerate anti-hypertensive agents improved blood pressure control?JNC VI revisited. AmJ hypertens 12(12): 225s-230s.
- Caserio O, Perez Iglesias R, Mata I, Martinez Garcia O,Pelayo Teran JM, et al. (2012) Predicting relapse after first episode of non-affective psychosis: a three years follow up study. J psychiatry Res 46: 10991105.
- Dassa D, Boyyer L, Benoit M, Bourset S, Rayemonet P, et al. (2010) Factors associated with medication nonadherence inpatients suffering schizophrenia in French public hospital. Aust NZJ psychiatry 44(10): 921-928.
- Dibonaventura M, Gabriel S, Dupclay L, Gupta S, Kim E (2012) A patient perspective of the impact of medication side effects on adherence results of a cross sectional nationwide survey of patients with schizophrenia. BMC psychiatry 12:20.
- D King, Knapp M, A patel, Amaddeo F, M Tansella, et al. (2013) The impacts of non-adherence to medication in patients with schizophrenia onhealth, social care and societal costs. Analysis of the QATRO study Epidemiology and psychiatric sciences 23(1): 61-70.
- Mamo Belayneh, Kefale Gelaw, Tegegn GT (2016) medication adherence among patients with schizophrenia treated with antipsychotic at adama hospital, east showa zone oromia regional state 5(2).
- Fawad Taj, Mansoor Taanwir, Zarmeneh Aly, AA khowajah, Asma Tariq, et al. (2008) Factors associated with non-adherence among Psychiatry patients at a tertiary care hospital. Karachi, Pakistan. A questionnaire based cross-sectional study. Journal of the Pakistan medical association in 58(8): 432-436.
- Gilmer TP, Dolder CR, Lacro JP, Folsom DP, Lindamer L, et al. (2004) Adherence to treatment with antipsychotic medication and health care costs among Medicaid beneficiaries with schizophrenia. AMJ psychiatry 161(4): 692-699.
- Harar Bulletin of health science (2011) Master's thesis research extract number two Haramaya university
- Haynes RB, MC Donald H, Garq AX, Montaque P (2001) Interventions for helping patients to follow prescriptions for medications. Cochrane Database of Systematic Review.
- IbrahimAW,Pindar SK, yerima MM, Rabbebe IB, Shehu SJ, et al. (2015) Medication related factors of non-adherence among patients with schizophrenia and bipolar disorder, outcome of cross sectional survey in Maiduguri, north-eastern Nigeria 7: 31-39.
- Jombo H Efflong, K Albert Umoh (2015) Medication non-adherence in schizophrenia prevalence and correlates among outpatients in tertiary health care facility in UYO south Nigeria 5(6): 107-113.
- Karves S, cleves MA, Helm M, Hudson TJ, west DS, et al. (2009) Good and poor adherence: optimal cut point for adherence measures using administrative claims data. curr med Res opin 25(9): 2303-2310.
- Lacro JP, Dunn LB, Dolder CR, Leck band SG, Jeste DV (2002) prevalence of and risk factors for medication non adherence in patients with schizophrenia. J Clain psychiatry 63(10): 892-909.
- Lieberman JA, Koreen AR, Chakos M, Sheitman B, Woerner M, et al. (1996) Factors influencing treatment response and outcome of first episode schizophrenia: implications for understanding the pathophysiology of schizophrenia's clin psychiatry 57(9): 5-9.
- Lerner BH (1997) From careless consumptives to recalcitrant patients, the historical construction of non-compliance. Socsci med 45(9): 1423-1431.
- M Olfson, David mechanic, steplen Hansel, Carol A Boyer, peter J weiden (2000) predicting medication noncompliance after hospital discharge 51(2): 216-222.
- MC Donnell PJ, Jacobes MR (2002) Hospital admission resulting from preventable adverse drug reactions. Ann pharmacotter 36(9): 13311336.
- Meguid EL, Marwa A, Eissawy, Heba, Sabry, et al. (2015) Understanding medication nonadherence in a sample of Egyptian patients with schizophrenia in relation to illness severity and insight. J psychiatry 23(4): 161-167.
- Mohler DN, Wallin DG, Dreyfus EG (1955) Studies in the home treatment of streptococcal disease I. failure of patients to take penicillin by mouth as prescribed. N Engl J med 252(26): 1116-1118.
- (2009) Medicines adherence involval patients in decisions about prescribed medicines and supportical adherence. National institute for health and clinical excellence, UK.
- Nose M, Barbui C, Tansella M (2003) How often do patients with psychosis fail to adhere to treatment program? in systemic review, psyco med 33(7): 1149-1160.
- Novick D, Haro JM, Suarez D, Perez V, Dittmann RW, et al. (2010) predictors and clinical consequences of non-adherence with antipsychotic medication in the outpatient RX of schizophrenia. psychiatry res 176(2-3): 109-113.
- Perkins DO, GUH, weieden PJ, MC Evoy JP, Hamer RM, Lieberma (2008) compassion of atypical in first episode study group. Predictors of treatment discontinuation and medication non adherence in pts recovering from a 1st episode of schizophrenia, schizophreniform disorder, or schizoaffective disorder; a randomized, double bind, flexible-dose, multicenter study. I clin psychiatry 69: 106-113.
- Rana NH, Ayub M (2002) Noncompliance to medication in psychiatric patients. pak J med sci 63(12): 1121-1128.
- Robinson D, Woerner MG, Alvir JM, Bilder R, Goldman R, et al. (1999) Predictors of relapse following response from a first episode of schizophrenia or schizoaffective disorder. Arch Gen psychiatry 56(3): 241-247.
- Senst BL, Achusim LE, Genest RP, cosentino LA, Ford CC, et al. (2001) practical approach to determining costs and frequency of adverse drug events in a health care network. AmJ Health syst pharm 58(12): 1126-1132.
- Svestka J, Bitter I (2007) Nonadherence to antipsychotic treatment in patients with schizophrenic disorders.Neuroendocrino Lett 28(1): 95116.?
- Tadele Eticha, Amha Tekelu, Dagim Ali, GebremedhinSolomon, Adisu Alemayehu (2015) factor associated with medication adherence among patients with schizophrenia in mekele, northern Ethiopia 10(3): e0120560.
- Thompson K, Kulkarni J, Sergew AA (2000) Reliablity and validity of a new medication adherence rating scale (MARS) for the psychosis. Schizophr Res 42(3): 241-247.
- Valestein M, Granoczy D, Mc carthy JF, Myra kim H, Lee TA, et al. (2006) Antipsychotic adherence over time among patients receiving treatment for schizophrenia. I clin psychiatry 67(10): 1542-1550.
- Young JL, Zonana HV, Shepler L (1986) Medication noncompliance in schizophrenia : Codification and update. Bulletin of the American Academy of Psychiatry and the Law 14(2): 105-122.
- Wiersma D, Nienhuis FJ, Sloof CJ, Giel R (1998) Natural course of schizophrenia disorders: a five years follow ups of a dutch incidence cohort. schizo phr Bull 24: 75-85.
- WHO (2003) adherence to long term therapies. Evidence for action Genera, Switzerland.






























