- Review Article
- Abbreviations
- Introduction
- Background
- Problem Statement
- Justification and Rationale
- Objectives
- Need for Cross-Border Malaria Initiative (Zambia & Namibia)
- Partnership, Harmonization and Alignment
- Components and Activities for Malaria Prevention and Control (Zam Nam)
- Challenges of CBMI-Zambia and Namibia
- Expected Out-Comes for Cross-Border Malaria Initiative-Zambia & Namibia
- Organization and Program Management of CBMI
- Monitoring and Evaluation Indicators
- Summary and Conclusion
- References
Ministry of Health, Zambia and the Ministry of Health and Social Services, Namibia
Emmanuel Kooma*
Texila American University, USA
Submission: December 01, 2017; Published: December 15, 2017
*Corresponding author: Emmanuel Kooma, Texila American University, USA, Email: emmanuel.kooma@gmail.com
How to cite this article: Emmanuel K. Ministry of Health, Zambia and the Ministry of Health and Social Services, Namibia. JOJ Nurse Health Care. 2017; 5(5): 555673. DOI: 10.19080/008 JOJNHC.2017.05.555673
- Review Article
- Abbreviations
- Introduction
- Background
- Problem Statement
- Justification and Rationale
- Objectives
- Need for Cross-Border Malaria Initiative (Zambia & Namibia)
- Partnership, Harmonization and Alignment
- Components and Activities for Malaria Prevention and Control (Zam Nam)
- Challenges of CBMI-Zambia and Namibia
- Expected Out-Comes for Cross-Border Malaria Initiative-Zambia & Namibia
- Organization and Program Management of CBMI
- Monitoring and Evaluation Indicators
- Summary and Conclusion
- References
Abbreviations
Abbreviations: ANC: Antenatal Care; FANC: Focused Ante Natal Care; HMIS: Health Management Information System; IEC: Information, Education and Communication; IVM: Integrated Vector Management; MACEPA: Malaria Control and Evaluation Partnership in Africa; MIS: Malaria Information System; MOU: Memorandum of Understanding; MOZIZA Area: South-Africa-Zimbabwe-Musina-Beitbridge Border; NCMPs: National Malaria Control Programs; NMCC: National Malaria Control Centre; NMVC: National Malaria Vector-Borne Diseases Control Program; PMI: President's Malaria Initiative; RBM: Roll Back Malaria; SADC: South African Development Community; SARN: Southern African Roll Back Malaria Network; SFH: Society For Family Health; UNAM: University of Namibia
- Review Article
- Abbreviations
- Introduction
- Background
- Problem Statement
- Justification and Rationale
- Objectives
- Need for Cross-Border Malaria Initiative (Zambia & Namibia)
- Partnership, Harmonization and Alignment
- Components and Activities for Malaria Prevention and Control (Zam Nam)
- Challenges of CBMI-Zambia and Namibia
- Expected Out-Comes for Cross-Border Malaria Initiative-Zambia & Namibia
- Organization and Program Management of CBMI
- Monitoring and Evaluation Indicators
- Summary and Conclusion
- References
Introduction
The Trans-Zambezi Region covers 5 countries (Angola, Namibia, Botswana, Zambia and Zimbabwe) at the narrow Caprivi Strip with a total of 16 districts; (4) Angola, (3) Botswana (2) Namibia, (5) Zambia, (2) Zimbabwe with a population of 1.5 million people at risk of malaria. Malaria burden has been ranging between <10 and 349 malaria cases per 1000 people at risk, and the death rate of under fives (5) averaged at 3-51 per 1000. While some communities in these countries experience epidemics.

A consultative meeting (Cross-Border Malaria Initiative- CBMI) for Zambia and Namibia was held in Sesheke district on the 4th of December, 2015 to promote sustainability in the reduction of malaria across the borders for the two countries. The Zambia -Namibia CBMI is being implemented in the area of Sesheke,Katima Mulilo, Mwandi, Livingstone and Kazungula and on the Zambezi Region on the Namibian Side, in order for each of the two countries to achieve their individual and collective goals of malaria elimination across-borders (Figure 1).
- Review Article
- Abbreviations
- Introduction
- Background
- Problem Statement
- Justification and Rationale
- Objectives
- Need for Cross-Border Malaria Initiative (Zambia & Namibia)
- Partnership, Harmonization and Alignment
- Components and Activities for Malaria Prevention and Control (Zam Nam)
- Challenges of CBMI-Zambia and Namibia
- Expected Out-Comes for Cross-Border Malaria Initiative-Zambia & Namibia
- Organization and Program Management of CBMI
- Monitoring and Evaluation Indicators
- Summary and Conclusion
- References
Background
The Trans-Zambezi Cross-Border Malaria Initiative (TZMI) was launched by the SADC Health Ministers in Ondangwa, Namibia in November, 2006 and a consultative meeting was held at the Elephant Hills Hotel in Victoria Falls, Zimbabwe from the 1st to the 3rd of February, 2011. Participants were drawn from Malaria National Control Program and Military Malaria Managers, SADC and SARN Secretariat, Research and academic institutions, WHO- National Program Officers from five TZMI countries; (Angola, Namibia, Botswana, Zambia and Zimbabwe.
The meeting included also partners from the Region (WHO- IST-ESA, MACEPA, Clinton Access to Health, SANOFI-AVENTS and HEDEC, The Globe RBM Secretariat, Global Malaria Program, Global Health Group and International Federation of the Red Cross and four SARN Steering Committee Members).
The objective was to contribute to the implementation of the SADC Malaria Control and Malaria Elimination Frame Works, E8 Resolutions and the SARN Work Plan through a joint TZMI Action Plan and establishment of vibrant TZMI and MOZIZA Cross-Border Initiatives to get funding from the Global Fund.
The main outcomes were: Redefined TZMI goal and objectives, a Draft Joint Action Plan with timelines to be finalized by the draft teams, development of the TZMI Business Plan, Establishment of TZMI District Committees in all the 16 districts made up of the District Health Teams, the Business and Local Community Leaders (Figure 2).
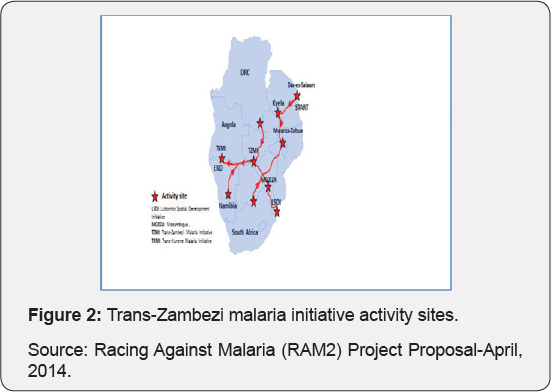
Social economic profile
The Trans-Zambezi Region (Zambia-Namibia) has over 90,000 people. The population has been mostly composed of subsistence farmers who make their living on the banks of the Zambezi, Kwando, Linyati and Chobe Rivers. The region is dominated by the Lozi ethnic group that live in Western Zambia, North West Zimbabwe (70,000) and Northern Botswana (14,000) and around Katima Mulilo. There are dynamics of mobility along the borders for these countries, making the prevention of imported and exportation of malaria a challenge for both countries [1-4].
The region has been described as an attractive destination for international tourism and as the largest Trans-Frontier Park in Southern Africa that has significant potential in agriculture, fishing and mining. In fact the Caprivi Strip is an economic and conservation corridor inscribed in the SADC economic and tourism integration strategies.
Cross-border population (target group)
A wide range of activities have long been adopted to protect and support livelihoods for many such as pastoralists, fishermen, businessmen, general travelers, tourists etc. However, there remains limited understanding of the nature, magnitude and value of cross-border livelihood activities in relation to diseases such as malaria and other communicable diseases. The TZMI along its borders experiences seasonal out-breaks of malaria between November and April each year.
The health system for Zambia and Namibia
Both countries have similarities in health service delivery systems as SADC member countries and as developing countries. The health system use has been imperative for optimal out comes, health and otherwise, for individuals and communities. As national borders become increasing porous, harmonized and coordinated efforts between the two countries is quite essential for malaria prevention and control.
Best practices and challenges have been identified across transmission zones and interventions, as well as cross cutting categories such as policies, funding, human resources, procurement and supply, monitoring and evaluation (M&E), partner coordination and integration, gender and equity and including Cross-Border Initiatives. Thus modern health systems are a rich and complex net work of interactions that cross national borders along with merits and demerits.
Pathway to malaria elimination
The current focus on resources and support has been on sustained control and countries taking different paths to malaria elimination. Countries in low/unstable transmission may move to elimination stage after reaching the milestones and those in high/stable transmission to remain in sustained control until new tools/approaches make elimination feasible. This pathway can also be categorized by level of transmission (Figure 3).
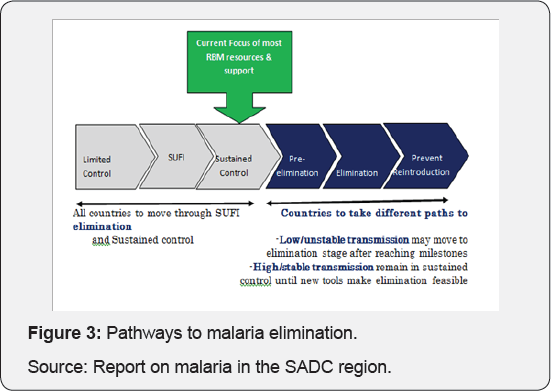
Major transmission zones and interventions
There are three transmission zones, (high, stable and mixed transmission, Low, unstable transmission, and no current transmission). Zambia still falls under the high, stable transmission zone that constitute areas where malaria cases occur throughout the year with or without seasonal peaks (WHO). The full WHO interventional package of Indoor Residual Spraying (IRS), Insecticide Treated Nets or Long lasting Insectide Treated Nets (ITNs/LLITNS), Rapid Diagnostic Tests (RDTs) and Artemisin in Combination Therapy (ACTs) have been adopted by member states.
In 2014, Zambia recorded 4.6 million cases of malaria and its malaria incidence increased from 330 per 1000 in 2010 to 407/1000 in 2014. However, case fatality rates have been indicating a reduction. Zambia still records clinical cases of malaria in some districts and institutions despite the availability of Rapid Diagnostic Tests (RDTs). However, overall case fatality has been going down.
The Zambian National Malaria Control Program include: clear National Policy and Guidelines providing a full package of malaria core interventions such as Intermittent Presumptive Treatment (IPT), Long Lasting Insecticide Treated Nets (LLINS), Indoor Residual Spraying (IRS). The country revised its malaria diagnosis and treatment guidelines (2014) and adopted the new WHO guidelines as for Sulphadoxine Pyrimethamine (SP).
Namibia falls in the low, unstable transmission zone characteristically having low incidence rates of malaria that are now continuous and are prone to epidemics. All interventions from high transmission zones (except IPTp) are applied in low transmission zones. Namibia has low, unstable transmission and has prepared for malaria elimination.
However, the challenge it faces is that it shares borders with Zambia that is still in high, stable and mixed transmission coupled with high volumes of population movement occurring across the borders. For Namibia, strong cross-border malaria control activities have to be supported by solid surveillance systems such as:
A. Availability of general principles that govern surveillance systems, including strengthened case definitions, procedures for case detection and investigation.
B. Data recording, reporting and analysis
C. Factors to be considered in establishing malaria surveillance systems.
With the availability of inexpensive, quality-assured rapid diagnostic tests for malaria means that parasite-based diagnosis is now possible not only at peripheral health care facilities but also at the community level. Thus malaria surveillance can be based on confirmed rather than suspected cases at all levels of the health system. As transmission is progressively reduced, it becomes increasingly possible and necessary, to track and respond to individual cases. If not well managed cases of malaria can surprisingly increase within a week to alarming levels.
The Health System in Namibia has become stronger and stronger than in the high transmission settings (Zambia) and there should be strengthened wide spread availability of parasitological diagnosis and appropriate treatment. Namibia has to concentrate more in the marginalized populations such as those living in the remote border areas, migrant workers and tribal populations and innovative ways have to be found to reach these groups [5].
The country has to strongly observe the feature of malaria surveillance systems in the control and elimination phases: low transmission settings. Namibia reported a decline of 98% in cases of malaria in the last decade (UCSF, 2004). The country is on track to be malaria free by 2020 after seeing cases in 2003 (450,000 dropping to just 2,500 in 2013.
Zambia is also on track towards malaria elimination with 50%- 75% decrease in case incidence from 2000-2015. They both have committed to the elimination 8 goal and despite the efforts in both countries, their borders continue to thwart the efforts,therefore there is urgent need to collaborate and coordinate the malaria prevention and control activities (Figure 4).
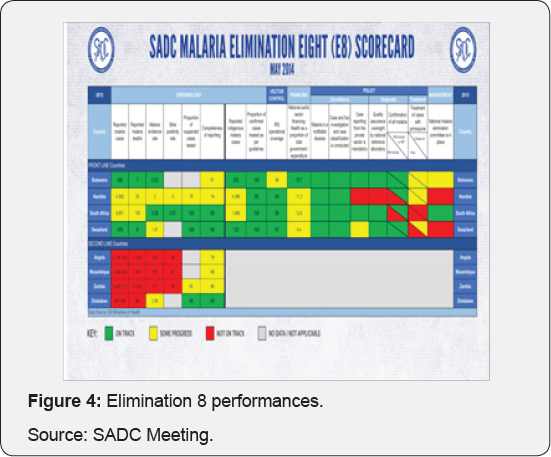
- Review Article
- Abbreviations
- Introduction
- Background
- Problem Statement
- Justification and Rationale
- Objectives
- Need for Cross-Border Malaria Initiative (Zambia & Namibia)
- Partnership, Harmonization and Alignment
- Components and Activities for Malaria Prevention and Control (Zam Nam)
- Challenges of CBMI-Zambia and Namibia
- Expected Out-Comes for Cross-Border Malaria Initiative-Zambia & Namibia
- Organization and Program Management of CBMI
- Monitoring and Evaluation Indicators
- Summary and Conclusion
- References
Problem Statement
Despite positive intervention results, Zambia and Namibia still have communities cut-off from effective malaria protection and treatment by geographical barriers, lack of physical infrastructure and resources (financial and human). The burden of malaria in the Zambezi and Sesheke areas has been borne by resource-poor communities, with limited access to health care and other social services, as well as low levels of literacy and a mobile population. The terrain of swamps, wetlands and woodlands are breeding grounds for malaria causing mosquitoes [6].
Malaria burden in the Trans-Zambezi Region has been reported to range between 1 and 400 malaria cases per 1000 population. A number of contributing factors to these incidences have been realized such as: Intermittent floods along the basin and around rivers, inadequate service delivery due to gaps in the six building blocks of the health system. Barriers exist to service access/delivery due to stringent customs and immigration laws and enforcement of public health regulations coupled with poor communication.
Highly mobile population transfer cross border infections (people with malaria parasite move across the borders). There has been lack of harmonization of policies, synchronization of activities and optimization of cross border interventions.
- Review Article
- Abbreviations
- Introduction
- Background
- Problem Statement
- Justification and Rationale
- Objectives
- Need for Cross-Border Malaria Initiative (Zambia & Namibia)
- Partnership, Harmonization and Alignment
- Components and Activities for Malaria Prevention and Control (Zam Nam)
- Challenges of CBMI-Zambia and Namibia
- Expected Out-Comes for Cross-Border Malaria Initiative-Zambia & Namibia
- Organization and Program Management of CBMI
- Monitoring and Evaluation Indicators
- Summary and Conclusion
- References
Justification and Rationale
There many productive hours of work lost due to malaria illness or funerals leading to low productivity. Without malaria as a public health problem across the border more tourists will be attracted and boost economic recovery and poverty alleviation in the region, the cross-border malaria initiative has risen due to migration of people between Zambia and Namibia influenced by the economic boom, employment potential population explosion along the Zambezi basin, infrastructure development and education between the two countries. Diseases like malaria and others have been widely prevalent along the border areas causing human suffering to under serviced populations [7-10].
A formal consultative malaria initiative meeting held between Sesheke and Zambezi health authorities in Sesheke district on the 4th of December, 2015 discussed issues related to cross-border disease prevention and control. Sesheke and Zambezi areas were selected for action process and further discussions were with NMCPs for both countries. Collaboration and commoditization of health care have contributed to increased patient mobility as patients cross borders to access health services in neighboring jurisdictions.
The Cross-Border Initiative has accelerated efforts to eliminate malaria in the Trans-Zambezi region with focused intervention supported by cooperating partners. The initiative will accelerate coordination of cost-effective malaria control activities and act as an accelerator of transmission from malaria control to malaria elimination, paving way for poverty alleviation and social economic prosperity in the region. Many lives can be saved through this initiative.
In Western Province of Zambia, malaria has become the highest cause of morbidity with an increase rate of 472/1000 (2014). Districts of Kaoma, Luampa, Lukulu and Nkeyama contribute largest burden of malaria cases for the province. The province has experienced an increase in the incidence of malaria from the year 2010 to the year 2015. The case fatality was 28/1000 admissions in the year 2014. Pregnant women have wide access to ant malaria prevention. Delivery of commodities and health services to remote river communities, however, remains a major challenge [11].
In Namibia, highest cases of malaria are reported in the Zambezi and Okavango hot spots along the Zambezi area of Namibia that are concentrated along the border with Angola. The malaria trend has reduced from 2001 to 2012. Namibia has interventions in place: case management, robust malaria surveillance system which conducts active and passive treatment of cases, IVM, IEC. The country has stopped treating clinical malaria cases.
- Review Article
- Abbreviations
- Introduction
- Background
- Problem Statement
- Justification and Rationale
- Objectives
- Need for Cross-Border Malaria Initiative (Zambia & Namibia)
- Partnership, Harmonization and Alignment
- Components and Activities for Malaria Prevention and Control (Zam Nam)
- Challenges of CBMI-Zambia and Namibia
- Expected Out-Comes for Cross-Border Malaria Initiative-Zambia & Namibia
- Organization and Program Management of CBMI
- Monitoring and Evaluation Indicators
- Summary and Conclusion
- References
Objectives
Main objective
To agree on coherent technical policies relating to crossborder malaria interventions (Policy direction, goals, guidelines, protocols, synchronization, collaboration, coordination, interventions and treatment regimes of activities).
Specific objectives
A. To review current cross-border malaria interventions between Zambia and Namibia.
B. To identify opportunities for CBMI in border districts.
C. To identify operational strategic direction towards CBMI(Administrative Structure & Composition).
D. To establish a surveillance, monitoring and evaluation system that informs planning and implementation of TZMI strategies in Zambezi and Sesheke areas.
- Review Article
- Abbreviations
- Introduction
- Background
- Problem Statement
- Justification and Rationale
- Objectives
- Need for Cross-Border Malaria Initiative (Zambia & Namibia)
- Partnership, Harmonization and Alignment
- Components and Activities for Malaria Prevention and Control (Zam Nam)
- Challenges of CBMI-Zambia and Namibia
- Expected Out-Comes for Cross-Border Malaria Initiative-Zambia & Namibia
- Organization and Program Management of CBMI
- Monitoring and Evaluation Indicators
- Summary and Conclusion
- References
Need for Cross-Border Malaria Initiative (Zambia & Namibia)
In accordance with Article 11 (SADC Health Protocol, August, 1999), there has been realization by the National Malaria Control Programs for both Zambia and Namibia that multi country border complexities pause challenges to individual country malaria efforts and to malaria elimination. In the 21st century people are increasingly mobile for numerous reasons, including seeking health care [12].
Highly mobile population with parasites has created the need for minimization of cross border infections (Import & Export of Parasites). The multi-country border complexities do not only isolate or deny services to communities at boundaries but sustain malaria reservoirs for the populations that are poised for disease elimination. The high population movement across the border promotes high circulation of parasites in and out of both countries. This is a key motivation for collaboration and coordination for Zambia and Namibia. Malaria deters economic growth especially in tourism, mining, fishing and agriculture which are the main economic activities in TZMI Region [13].
The Trans-Zambezi region has several geographical characteristics such as rough and rugged terrain as well as underdeveloped road infrastructure that limit equity of access to quality health care. The delivery of logistics and other supplies is also difficult due to the geographical terrain of the region [14]. Further, the region has inadequate health facilities and human resources for health to support a complete six building blocks for the health system.
- Review Article
- Abbreviations
- Introduction
- Background
- Problem Statement
- Justification and Rationale
- Objectives
- Need for Cross-Border Malaria Initiative (Zambia & Namibia)
- Partnership, Harmonization and Alignment
- Components and Activities for Malaria Prevention and Control (Zam Nam)
- Challenges of CBMI-Zambia and Namibia
- Expected Out-Comes for Cross-Border Malaria Initiative-Zambia & Namibia
- Organization and Program Management of CBMI
- Monitoring and Evaluation Indicators
- Summary and Conclusion
- References
Partnership, Harmonization and Alignment
Each of the two countries has collaborating and coordinating partners. Zambia's stakeholders being government and partners are: NMCC, SFH, MACEPA, USAID, PMI: ISdell Flowers- Anglican Church. While Namibian has NMVC, Global Fund, UCSF Global Health, Research, Research Centre at University of Namibia(UNAM), the Novartis Foundation for Sustainable Development, the London School of Hygiene and Tropical Medicine, the Clinton Health Access Initiative, Anglican Church; ISdell Flowers and other Community -Based Volunteers.
- Review Article
- Abbreviations
- Introduction
- Background
- Problem Statement
- Justification and Rationale
- Objectives
- Need for Cross-Border Malaria Initiative (Zambia & Namibia)
- Partnership, Harmonization and Alignment
- Components and Activities for Malaria Prevention and Control (Zam Nam)
- Challenges of CBMI-Zambia and Namibia
- Expected Out-Comes for Cross-Border Malaria Initiative-Zambia & Namibia
- Organization and Program Management of CBMI
- Monitoring and Evaluation Indicators
- Summary and Conclusion
- References
Components and Activities for Malaria Prevention and Control (Zam Nam)
1. Integrated Vector Management (IRS, LLINS, Larviciding & Environmental Management
2. Disease surveillance involving weekly monitoring system
3. Case management alignment to country needs and WHO & SADC Guidelines
4. Health education (SBCC)-Improving awareness and knowledge about malaria play a major role in increasing intervention coverage and reducing malaria cases and mortality
5. Strengthening IPT via FANC and ANC services (Zambia)
6. Surveillance (Zambia) to maintain sentinel surveillance sites and data to be submitted on weekly basis
7. Case detection and management (Zambia)- Parasitological confirmation of malaria to be strengthened prior to treatment of clients in order to limit the misuse of the anti malarias
8. Strengthening HMIS and MIS in both countries
9. Document good practices for dissemination between the two countries
10. Mobilize funds to close the gap for universal coverage across the borders
11. Strongly address hard-to-reach marginalized or other vulnerable groups
12. Replace and or dispose damaged nets
13. Build capacity for monitoring the efficacy of insecticides and drugs, as appropriate
14. Fully engage the private sector and create opportunities
15. Build human resource capacity to support the rapid scale -up of malaria control and advancement along the elimination path way
16. Prevent cross-border leakage of drugs including malaria drugs
17. Provide guidelines at all levels of health facilities
18. Strengthen planning, monitoring and evaluation and general administration of the initiative.
- Review Article
- Abbreviations
- Introduction
- Background
- Problem Statement
- Justification and Rationale
- Objectives
- Need for Cross-Border Malaria Initiative (Zambia & Namibia)
- Partnership, Harmonization and Alignment
- Components and Activities for Malaria Prevention and Control (Zam Nam)
- Challenges of CBMI-Zambia and Namibia
- Expected Out-Comes for Cross-Border Malaria Initiative-Zambia & Namibia
- Organization and Program Management of CBMI
- Monitoring and Evaluation Indicators
- Summary and Conclusion
- References
Challenges of CBMI-Zambia and Namibia
Cross-Border malaria activities and economic exchanges have been significantly constrained by the lack of a common institutional frame work to enable harmonization of policies, synchronization of activities, collaboration and coordination within administrative and malaria activities implementation structures, regulation and promotion of cross-border issues in the Trans-Zambezi Region of Zambia and Namibia. The common challenges for the two countries have been:
Indoor Residual Spraying (IRS)
Zambia's IRS program has been affected by late implementation of the program while Namibia has done well and start the IRS program at the right time but refusals towards the program in some communities are reported. Both countries have difficulties in covering mobile populations and lack of synchronization of activities where Namibia conducts IRS before Zambia does it and done at end of peak season (2 years now).
ITNs
There has been non compliance to the use of LLITNs for both countries and misuse for both countries have been recorded. There could also be insufficient supplies of LLITNs. Trainings for new commodity roll outs not well organized or timed. Distribution of LLITNs has also faced challenges due to high turnover of community volunteers generally due to lack of incentives for motivation.
Case management
Shortage of qualified staff in facilities of the bordering districts has been a big challenge. The staff attrition rate has been a big challenge due to many causes. There has been insufficient IEC for dispelling myths and emphasizing the need for prompt diagnosis and treatment. There also exist "Push and Pull Factors" in seeking health care services for the cross border population.
Despite our inadequate understanding about the precise number and nature of patients seeking health care abroad, several factors have facilitated the movement of patients between the two countries. Some of the factors are the new developments of information about foreign providers. With the global village in place, coupled with lowered transportation costs and reduced language barriers, trade liberization efforts in health care service delivery are another driving force of enhanced medical travel [14].
Patients have also specific reasons for seeking health care abroad within the two countries. Patients might want to seek treatment not available in their own country done better in another country. While doing this malaria parasites can be transmitted from one end to another end. Furthermore, patients faced with long waiting lists for certain procedures sometimes decide to seek treatment abroad.
Some patients look for more affordable health care and might also travel to neighboring district that offer health services of similar quality but at significantly lower price. The clinical diagnosis was still practiced in some parts of Sesheke health care facilities. This calls for harmonization, and where appropriate standardization of policies in areas of case definitions for diseases, notification systems, treatment and management of major communicable disease (Article 9 SADC Health Protocols, 1999).
Disease surveillance and reporting
There has been reporting systems not linked across the health system levels or regions/districts between the two countries. In some parts of the two districts passive case detection in the public sector has been strengthened to identify new malaria infections but less is said about the private sector. Sesheke and Zambezi Region rely on HMIS, where reporting was often infrequent, delayed and sometimes lacks adequate case information. Weekly surveillance system has been enhanced. Vector control data is usually kept separate from case data preventing comprehensive analysis of all program activities [15].
Monitoring cross border activities have little or no involvement of district programs and Port Health (IHR, 2005) not well policed to support resource availability and personnel at Points of Entry (POEs). In Cross-Border Malaria Initiative, Port Health Officers are not brought distinctively in Cross-Border Malaria strategies and activity implementation.
- Review Article
- Abbreviations
- Introduction
- Background
- Problem Statement
- Justification and Rationale
- Objectives
- Need for Cross-Border Malaria Initiative (Zambia & Namibia)
- Partnership, Harmonization and Alignment
- Components and Activities for Malaria Prevention and Control (Zam Nam)
- Challenges of CBMI-Zambia and Namibia
- Expected Out-Comes for Cross-Border Malaria Initiative-Zambia & Namibia
- Organization and Program Management of CBMI
- Monitoring and Evaluation Indicators
- Summary and Conclusion
- References
Expected Out-Comes for Cross-Border Malaria Initiative-Zambia & Namibia
A. Situational analysis conducted periodically along the border (Sesheke & Zambezi)
B. Increased understanding of current malaria burden across the borders
C. Mapped opportunities for Cross-Border Malaria Initiative synergies between Zambia and Namibia
D. Community Volunteers trained in use of Rapid Diagnostic Tests (RDTs)
E. Malaria Test, Treat and Track (T3) conducted at Points Of Entry for both countries (Zambia and Namibia)
F. High number of Community Health Workers/Malaria Agents trained in case management
G. Improved parasitological confirmation of malaria cases
H. Strengthened active and passive surveillance of malaria cases in Sesheke and Zambezi Region (Katima Mulilo)
I. Number of planned review meetings held between Zambia and Namibia
J. Number of exchange visits conducted between Sesheke and Zambezi Region (Management level & Health care facilities along the border)
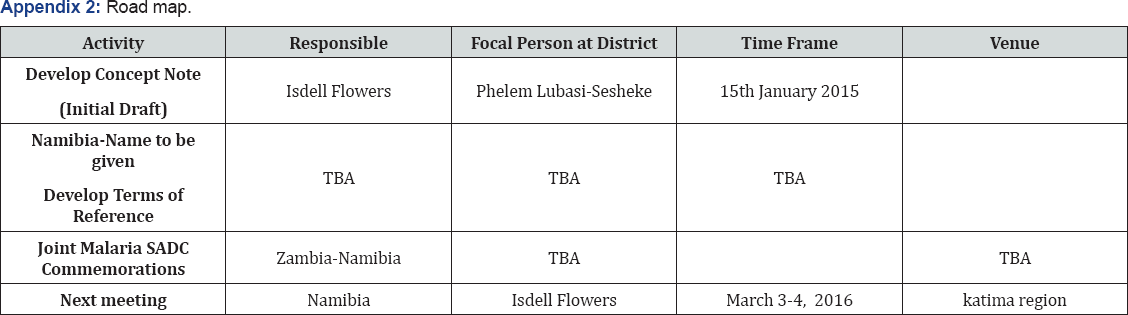
K. Road Map drawn for Sesheke and Zambezi areas
L. Joint Malaria SADC Commemoration Action Plans developed and implemented
M. Strengthened communication and advocacy activities
N. Strengthened stakeholders analysis and engagement in CBMI
O. Synchronization and harmonization of policies implemented
P. Strengthened community engagement in CBMI
- Review Article
- Abbreviations
- Introduction
- Background
- Problem Statement
- Justification and Rationale
- Objectives
- Need for Cross-Border Malaria Initiative (Zambia & Namibia)
- Partnership, Harmonization and Alignment
- Components and Activities for Malaria Prevention and Control (Zam Nam)
- Challenges of CBMI-Zambia and Namibia
- Expected Out-Comes for Cross-Border Malaria Initiative-Zambia & Namibia
- Organization and Program Management of CBMI
- Monitoring and Evaluation Indicators
- Summary and Conclusion
- References
Organization and Program Management of CBMI
The CBMI is between Ministry of Health-Zambia and Namibia through their NMCP implemented by the health system structures for the two countries. The aim is to reduce and eliminate malaria transmission in the targeted border districts in order to identify gaps, mobilize leaders through public and privates sectors, malaria structures and empowering communities for malaria elimination for multi-sect oral action at all levels [16].
The cross-border regional malaria surveillance system has to be developed to identify transmission foci (parasitological and entomological) and coordinate, monitor, evaluate and report on surveillance activities in the communities through active and passive case detection, notification, investigation and follow up within 24hrs of notification by searching for parasites in and around the foci and treating infected people in accordance with T3: Test, Treat and Track strategy as supplementary elimination interventions.
There is need for mapping of foci and villages along the border where a focus on malaria control is identified in mobile populations such as migrants, travelers, traders and tourists. Social Behavior Change and Communication (SBCC) has to be strengthened among the communities and reinforcement of community participation and ownership to achieve universal access to malaria control services and improved health status of both residents and mobile populations and partners.
Stakeholders have to be mapped to support cross-border malaria control and elimination. The health systems management of the two areas (Sesheke and Zambezi) has to strongly support the malaria programs through strengthened information, education and communication (IEC) and SBCC for communities along the borders.
The system has to help programs increase health promotion levels and expand community and home-based malaria control. The multi-sect oral collaboration has to promote community mobilization among cross-border populations, while making sure isolated populations-river valley communities, illegal border jumpers, migrants, travelers and tourists (hospitality) are also reached. The Health Management Information System (HMIS) has to support programs to strengthen districts and community level ownership of malaria elimination activities. All the activities have to be reported through the system and meetings [17].
- Review Article
- Abbreviations
- Introduction
- Background
- Problem Statement
- Justification and Rationale
- Objectives
- Need for Cross-Border Malaria Initiative (Zambia & Namibia)
- Partnership, Harmonization and Alignment
- Components and Activities for Malaria Prevention and Control (Zam Nam)
- Challenges of CBMI-Zambia and Namibia
- Expected Out-Comes for Cross-Border Malaria Initiative-Zambia & Namibia
- Organization and Program Management of CBMI
- Monitoring and Evaluation Indicators
- Summary and Conclusion
- References
Monitoring and Evaluation Indicators
There is need to implement the potential indicators (Existing and newly developed)
Passive surveillance
The surveillance systems detect infections:
A. Human Blood Examination Rate (ABER)-Passive, Active, Passive-Active (Reactive)
B. Completeness and Timeliness-Passive surveillance reporting (inclusion of the Private sector) and Village/ Community Health Workers reports. Proportion reported within x time period
C. Proportion of suspected malaria cases tested for malaria
D. Proportion of cases of malaria which are parasitological confirmed
E. Proportion of facilities with microscopy with an active Quality Assurance System.
Active surveillance and response
A. Proportion of malaria cases fully investigated
B. Proportion of cases investigated within x time period
C. Proportion of foci full investigated
D. Proportion of case investigation response conducted within x time period:
a) Reactive Case Detection (RACD), Focal, IRS, Targeted Presumptive Treatment (TPE)
Differential surveillance indicators by strata (district, facility)
A. Proportion of cases confirmed by RDT/Microscopy
B. Proportion of facilities reporting in 7 days
C. Proportion of confirmed cases reported in 2 days
D. Proportion of confirmed cases investigated
E. Proportion of confirmed cases within 3 days
F. Proportion of responses (RACD,etc ) within 7 days
Case management
A. Proportion of confirmed cases treated appropriately as per national guidelines
B. Inpatient malaria deaths per 1000 per year
Vector control
A. Proportion of targeted households that have been sprayed(IRS)
B. Proportion of population at risk potentially covered by nets distributed (Equal or greater than 80%)
C. Proportion of targeted risk groups receiving ITN (equal or greater than 80%)
D. Proportion of HHs with at least one ITN
E. Insecticide resistance monitoring conducted
Policy framework indicators
A. Official National commitment to elimination (MOU)
B. National, Provincial, District, Facility, Case Register in place
C. Proportion of funding from domestic sources(Budget Plans)
D. Malaria is a modifiable disease with less or equal to 48 hours
E. Mandatory case reporting in private sector
F. Cross border agreement and or collaboration(MOU & Concept Note):
a. Different indicators are for different stages?
Epidemiology (ZAMNAM reporting indicators)
A. Reported malaria cases (All ages)
B. Reported malaria deaths (All ages)
C. Slide positivity rate (All ages)
D. Proportion of suspected cases tested (All ages)
E. Completeness and timeliness of reporting (Agreed time of reporting)
F. IRS operational coverage (Seasonal/foci)
G. LLITN operational coverage (All year round/replenishment/replacement)
- Review Article
- Abbreviations
- Introduction
- Background
- Problem Statement
- Justification and Rationale
- Objectives
- Need for Cross-Border Malaria Initiative (Zambia & Namibia)
- Partnership, Harmonization and Alignment
- Components and Activities for Malaria Prevention and Control (Zam Nam)
- Challenges of CBMI-Zambia and Namibia
- Expected Out-Comes for Cross-Border Malaria Initiative-Zambia & Namibia
- Organization and Program Management of CBMI
- Monitoring and Evaluation Indicators
- Summary and Conclusion
- References
Summary and Conclusion
Our understanding of public health has been challenged by the current global trend of a more integrated world. As national borders become increasingly porous, public health experts need to explore new ways of managing national health systems. In the 21st century, more and more patients have decided to seek medical treatment in countries where they are not residents. There are many reasons for this increasing international mobility of patients, due to many individual needs. Affluent patients might search for the highest possible quality of health care, and whereas others might be looking for quality and less expensive treatment abroad. In any case, patient mobility is increasingly observed in developed and developing countries, both of which serve as source and destination countries.
The planning and implementation of malaria cross -border activities as response to disease transmission remain largely unexplored much in both policy and practice. Given the regional nature of malaria and the challenges it poses, there is an urgent need to develop a better understanding of cross border dynamics and take full advantage of their potential to contribute to strategic and more appropriate interventions to malaria situation along the borders of Zambia and Namibia.
This response needs to be premised by both countries (Zambia and Namibia) on the recognition that the existence of cross border linkages makes bordering communities likely to be exposed to similar risks and have interdependent or correlated vulnerabilities. It is imperative therefore to undertake comprehensive cross-border situational analysis in the early program planning stages as the basis of appropriate strategies and activities. Assumptions will misguide strategies and finally activities implemented and this will not give good responses to the situation existing.
Notwithstanding the unexplored potential to work across the long and porous borders between Zambia and Namibia, more significant and strategic engagement necessarily requires substantial technical and operational capacity, not least because of the remoteness and size of the border areas for Sesheke and Zambezi border population [18].
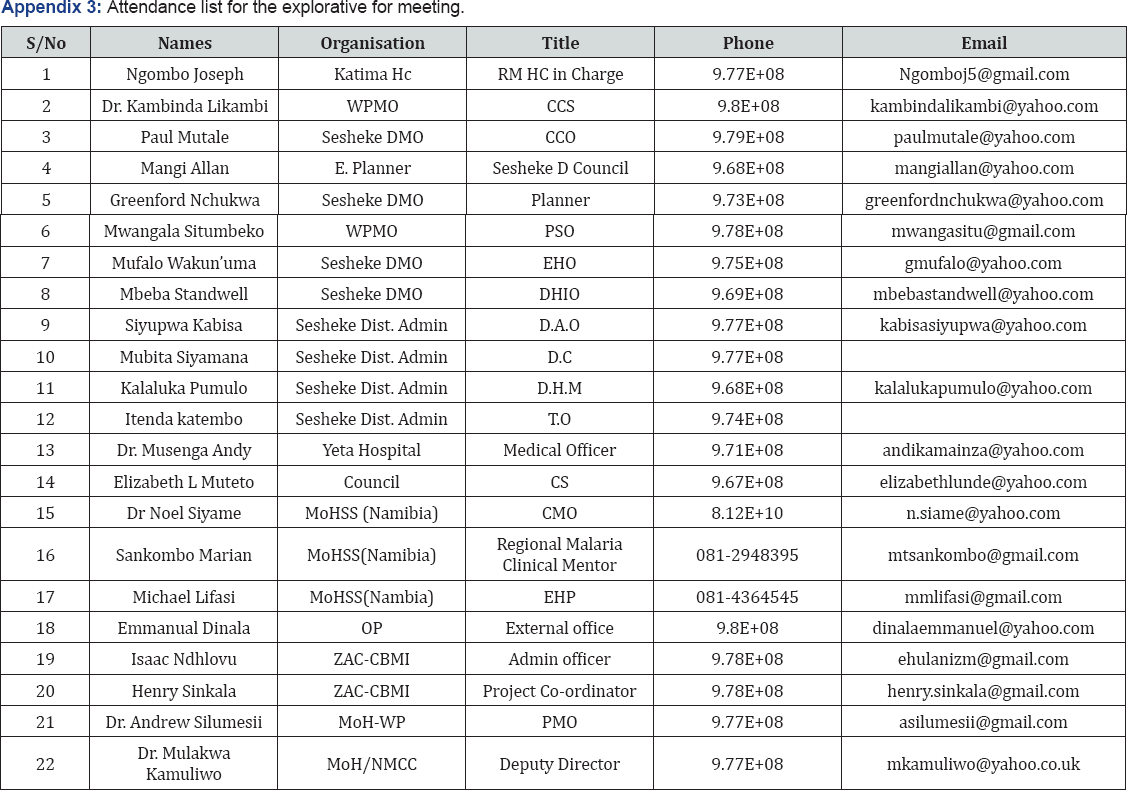
It is very important to redress the negative perceptions and trans-border activities so that the national and provincial partners explicitly recognize and support the available and sizeable opportunities that these areas offer in terms of malaria out-breaks and epidemic preparedness. Given the inevitability of cross border exchanges, Zambia and Namibia should also take urgent steps to monitor malaria activities pertaining to cross border health systems service delivery gaps (Appendix 1-3).
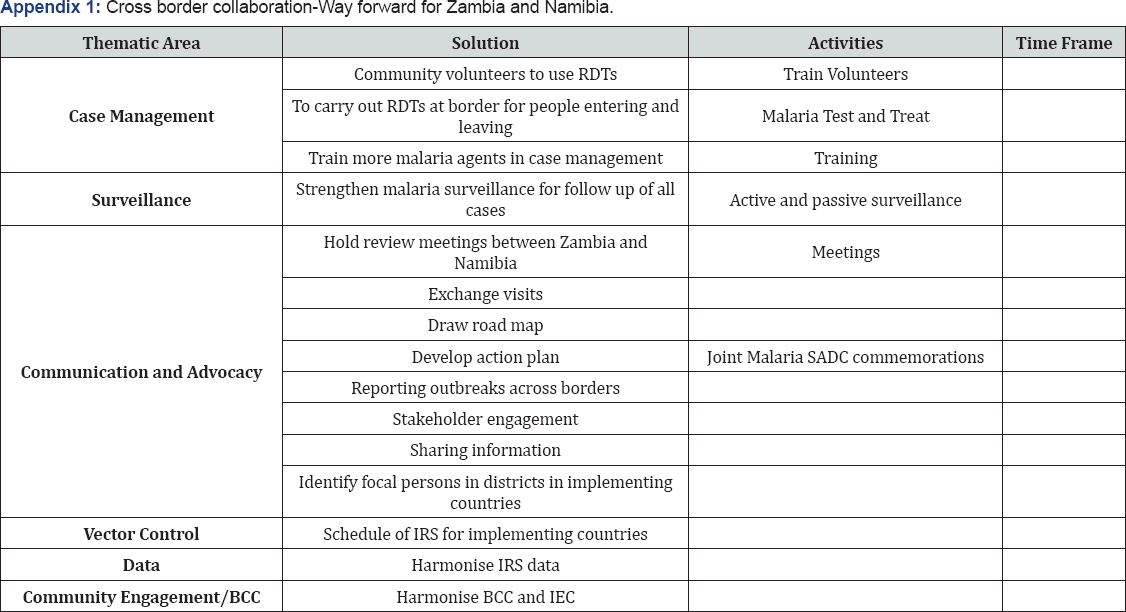
- Review Article
- Abbreviations
- Introduction
- Background
- Problem Statement
- Justification and Rationale
- Objectives
- Need for Cross-Border Malaria Initiative (Zambia & Namibia)
- Partnership, Harmonization and Alignment
- Components and Activities for Malaria Prevention and Control (Zam Nam)
- Challenges of CBMI-Zambia and Namibia
- Expected Out-Comes for Cross-Border Malaria Initiative-Zambia & Namibia
- Organization and Program Management of CBMI
- Monitoring and Evaluation Indicators
- Summary and Conclusion
- References
References
- (2017) Adapted from Guidelines on the elimination of residual foci of malaria transmission, WHO Regional Office for East Mediterranean, Cairo, Egypt.
- African Union (2007) Declaration on the African Union Border Program and its implementation modalities as Adopted by the Conference of African ministers in charge of border issues. Addis Ababa, Ethiopia.
- Gueye CS, Gerigk M, Newby G, Lourenco C, Uusiku P, et al. (2014) Namibia's path toward malaria elimination: a case study of malaria strategies and costs along the northern border. BMC Public Health 14: 1190.
- (2009) Guidelines for treatment of malaria. (3rd edn), World Health Organisation, Geneva, Switzerland.
- http://www.rollbackmalaria.org/files/files/countries/TZMI_ RMMCCmeeting2011feb.pdf
- Little P (2006) Working across borders: Methodological and policy challenges of cross-border livestock trade in the Horn of Africa.
- (2007) Malaria Elimination. A field manual for low and moderate endemic countries. WHO, Geneva, Switzerland.
- Pavenello S. Cross border policy and practice in East and West Africa drylands. A Literature review. HPG working paper.
- https://photos.state.gov/libraries/zimbabwe/231771/PDFs/ Racing%20Against%20Malaria%20Sept%2018.pdf
- (1999) SADC Health Protocol.
- http://alma2030.org/sites/default/files/sadc-elimination-scorecard/ elimination-scorecard-placemat.pdf
- SARN Secretariat (2011) Report of the Trans-Zambezi Cross-border Malaria Program consultative Meeting, Elephant Hills Hotel, Zambia.
- https://www.ucsf.edu/news/2014/04/113841/ucsf-work-namibia- contributes-sharp-drop-malaria-cases
- UCSF-Global Health Sciences: Indicators for malaria elimination: What is new, what is needed. Tulane University, USA.
- http://www.moh.gov.zm/docs/nhsp.pdf
- (2011) Universal access to malaria diagnostic testing. World Health Organization, Geneva, Switzerland.
- University's work already has contributed to 98 percent drop in malaria cases in Namibia.
- http://www.who.int/malaria/publications/country-profiles/profile_ zmb_en.pdf






























