Problem Solving Ability and Working Memory Capacity of Patients with Schizophrenia: The Effect of Problem-Solving Training Intervention
Eweida RS*, Mekail MN and Ramadan FH
Department of Psychiatric Nursing and Mental Health, Alexandria University, Egypt
Submission: November 02, 2017; Published: December 09, 2017
*Corresponding author: Eweida RS, Department of Psychiatric Nursing and Mental Health, Alexandria University, Egypt, Email: dr_rashapsych@hotmail.com
How to cite this article: Eweida RS, Mekail MN, Ramadan FH. Problem Solving Ability and Working Memory Capacity of Patients with Schizophrenia: The Effect of Problem-Solving Training Intervention. JOJ Nurse Health Care. 2017; 5(5): 555671. DOI: 10.19080/JOJNHC.2017.05.555671
Background: Problem solving and working memory were determined as the most important cognitive domains that affect the ability of patients with schizophrenia to learn, maintain or perform the skills required for everyday functioning and grossly one's resilience in handling the encountered problems. Acquiring interpersonal problem-solving skills acts as a shield in protecting against relapse, reduced quality of life, and difficulties in psychosocial and occupational functioning. Interestingly, there is a tremendous need for equipping patients with schizophrenia with interpersonal problem-solving competencies that they can use in their everyday interactions and empower them to attain more of their personal goals. Objective: This study aimed to assess the effect of a problem-solving training intervention on interpersonal problem-solving ability and working memory capacity among patients with schizophrenia. Method: A quasi-experimental design was used in this study. The training intervention was conducted through 10 training sessions 4 times/ week for three weeks. Results: The study implies statistical significant differences in favor of the study group regarding problem solving ability and working memory capacity as compared to the control one. Conclusion: Problem-solving training intervention contributed positively in the enhancement of the interpersonal problem-solving ability and working memory capacity among patients with schizophrenia. The findings should merit more extensively for longer period on a larger sample; including female patients to ensure proper generalization. Keywords: Problem solving ability; Working memory capacity; Interpersonal problem-solving skills; Schizophrenia
By reviewing the existing large body of literature, problem solving and working memory were determined as the most important cognitive domains that affect the ability of patients with schizophrenia to learn, maintain or perform the skills required for everyday functioning and grossly one's resilience in handling the encountered problems [1-4]. Furthermore, these two dominant cognitive abilities are intimately encompassing all cognitive abilities; that enable individuals to solve their encountered problems and reduce many adverse effects such as anxiety, depression, and interpersonal conflict that may arise from unproductive attempts [5]. Green et al. [6] confirmed that the deficits in any of these cognitive areas may lead to ineffective interpersonal problem solving and limit social and work functioning among patients with schizophrenia. The inability to handle interpersonal problem situations effectively and compromised working memory in patients with schizophrenia were found to be the main causes of relapse, reduced quality of life, and difficulties in psychosocial and occupational functioning [7,8]. It was hypothesized that training patients with schizophrenia in interpersonal problem-solving skills will be of benefit for building cognitive strength to cope with daily frustrations and interpersonal conflicts, and to diminish the risk of serious interpersonal dysfunction. Increasingly, training patients how to actively solve typical, everyday interpersonal problems, could provide them with opportunities of increasing their confidence and self- control to approach problems in a systematic way, not only for their immediate problems but also with the future problems on their own. It will also help them to understand the link between their emotional symptoms and current everyday problems. Hence, it helps in improving a problematic situation, reducing or modifying the negative emotions generated by the problems, or both of these outcomes [9,10]. Based on the cognitive-behavioral frame of reference which emphasizes the interaction of thoughts, feelings and behaviors in an attempt to facilitate self-control for broadening behavior changes, Spivack & Siegel [11] developed ICPS program for patients with schizophrenia to train them about the general cognitive strategies in coping more successfully with other people, and deal with their problems that arise within the interpersonal matrix. This program is based on the assumption that the ability to recognize and resolve everyday problems will contribute to lower recidivism rates of admission to hospitals and better adjustment in the community [11]. The common goal of ICPS program is to enhance adjustment, not by direct modification of behavior themselves, but by altering an individual's ability to think through and solve typical, everyday problems that come up when interacting with others. In this program, patients are guided to develop the habit of generating multiple options, evaluating these options, and planning the step by step means to reach a stated goal [12]. Therefore, acquiring interpersonal problem-solving skills acts as a shield in protecting against such devastating consequences and, ultimately helps them successfully return to society. Interestingly, there is a tremendous need for equipping patients with schizophrenia with interpersonal problem-solving competencies that they can use in their everyday interactions and empower them to attain more of their personal goals. Moreover, it can actively stimulate their working memory abilities through manipulation or processing of what has been previously learned and execute it into the real- life tasks. Such abilities, in fact, have a bearing on successful community adjustment. Accordingly, psychiatric nurses need to pursue more active studies and acquire the necessary abilities needed to enhance the interpersonal problem-solving skills for patients with schizophrenia.
A. Explore the interpersonal problem-solving ability and working memory capacity of patients with schizophrenia. B. Assess the effect of a problem-solving training intervention on interpersonal problem- solving ability and working memory capacity among patients with schizophrenia.
A quasi-experimental design was used in this study. This study was conducted at EL-Maamoura Hospital for Psychiatric Medicine, in Alexandria, Egypt. The hospital is affiliated to the Ministry of Health and Population. 60 Male patients diagnosed with schizophrenia constituted the subjects of this study. They were randomly divided into control and study groups (30 patients each). A. Definite diagnosis of schizophrenia with no co-morbidity. B. Duration of illness not more than 5 years since diagnosis. C. Able to communicate in a coherent and relevant manner. D. Not under ECT treatment (in order to avoid the adverse effects of ECT on cognitive functioning). E. Able to read and write. F. Agreed to participate in the research after understanding the purpose of the study. Tool I: Means-Ends Problem-Solving Procedure (MEPS): Means-Ends Problem-Solving Procedure (MEPS) is an instrument developed by Spivack et al. [13]. The MEPS procedures are intended to measure the ability of a person to conceptualize the means or sequence of steps that may be necessary to carry one from a point of having an interpersonal problem that require a resolution, to the point where the need is satisfied or the problem is solved. The MEPS consists of 10 story roots that describe an interpersonal problem or conflict situation. There are three story roots recommended for children 9-12 years of age, and seven story roots applicable to adolescents and adults. Spivack et al. [13] recommended that at least three story roots (vignettes) could be used to achieve minimum reliability. The tool was applied on patients with schizophrenia and demonstrated high test-retest reliability (Pearson r=0.92). The task presented to the subjects is to make up a story that connect the beginning of the story as given, with the end (resolution) as given (i.e: to make up the middle). It's working assumption is that better adjusted individuals are more able means- ends thinkers. Such thinking incorporates the following components: (a) the ability of the subjects to conceptualize the means or the sequential steps that are necessary to solve the interpersonal problem (b) the ability to anticipate obstacles that may potentially hinder or block the successful completion of a plan, and (c) the ability to appreciate that such problem solving takes time or the fact that appropriate timing may be an essential ingredient of a workable plan [13]. Stories are scored for (a) the number of means given by the subjects in order to reach the story goal, (b) the number of obstacles that might prevent the hero from reaching that goal, and (c) any indication of the passage of a specific amount of time before reaching the goal. The subjects were given one point for each score. For the overall vignettes, a mean score was calculated pre and post intervention. Tool II: Forward and backward digit span test: The forward and backward digit span test was developed by Weschler [14] to measure the storage capacity of working memory. The digit span test includes two components namely; digits forward and digits backward in a single subtest. Digits forward is considered to assess the short term- memory and digits backward considered with assessment of the executive working memory. The test comprised seven levels and each level consisted of a number of digits that increased with a rate of one number per each level. The subjects are given one point for each series of digits that was correctly recalled. If the subjects do errors for two consecutive trials of the same length of digits, the test is stopped. Scoring of the digit span test was based on the sum of the forward and backward correctly repeated items. The total score ranged between 0-28 based on the sum of successful repeated items of both forward and backward tasks. The scores are categorized as follows: 0-9 indicate low working memory capacity, 10-19 represent moderate working memory capacity and 20-28 reflect high working memory capacity. The test was valid, applied on patients with schizophrenia and demonstrated high test-retest reliability (Pearson r =0.88) [14]. Tool III: Socio-demographic and clinical data interview schedule: A socio-demographic and clinical data interview schedule was developed by the researcher to elicit data about patients' age, martial status, educational level, duration of illness, and number of previous psychiatric hospitalization. The problem- solving training intervention was conducted according to the following phases: Preparation phase: A. A jury composed of five experts in the field of psychiatric nursing was consulted to select three stories suitable to the Egyptian culture and to examine also the content validity of the selected vignettes, and they revealed to be valid. B. Reliabilities of the study tools MEPS and The forward and backward digit span test were tested using the Pearson Chi-Square test on a sample of 15 patients with schizophrenia meeting the criteria of the study sample. The tools proved to be reliable. C. The researcher was trained on how to conduct the problem solving training interventions. D. The researcher followed the Spivack & Siegel [13] problem solving training intervention as a guide [11]. With some modifications to fit with the Egyptian culture. E. Contents of the problem solving training intervention were prepared by the researcher under the direction of the supervisors including; pictures, CD, slides, videotapes, flip charts, etc.... These activities were designed by a professional person from the faculty of Fine Arts. F. Male wards were ranked using simple randomization by picking their names up from a pool. The first selected ward from the pool was the starting one for data collection, and then the second the next one and so on. G. The first two-selected wards were assigned for the control group and the second two for the study group. The process was repeated till the required number is obtained. H. Study tools were applied on both groups using the interview method on an individual basis (pre-test). The study subjects were presented by the selected 3 vignettes and the forward and backward digit span test. A. The study group was divided into subgroups. Each subgroup ranged between 6 and 8 patients. B. The training intervention was conducted through 10training sessions, 4 times/week for three weeks. The intervention was conducted by covering the following four stages with a series of 12 training exercises: Stage 1: Recognition of problems. (2 sessions) This stage comprised four exercises that were conducted into 2 sessions. Each session covered 2 exercises. The first and the second exercise intended to give the subjects some practice in paying attention to what they see as a mean of being better able to recognize problems when they occur. The third exercise intended to give the subjects practice in recognizing interpersonal problems concerning others' feelings. The fourth exercise in stage 1, aimed to give the subjects practice in the actual recognition of problems. Stage 2: Definitions of problems. (3 sessions) This stage consisted of two exercises. Exercise (5) was covered in two sessions and intended to teach the subjects the art of intelligent information gathering as one aspect of the ability to define problems. While, exercise (6) was conducted in one session and intended to teach the subjects how to seek information about other people as part of the ability to define problems. Stage 3: Alternative Ways of Solving Problems. (2 sessions) This stage comprised two exercises. Each exercise was covered in one session. Exercise (7) aimed to give the subjects practice in recognizing that there are different solutions to the same problem. Exercise (8) intended to give the subjects practice in thinking of alternative solutions to solve the problem. Stage 4: Deciding Which Solution is the Best Way to Solve the Problem. (3 sessions) The final stage involved four exercises. Exercise 9 & 10 were conducted in the first session. Exercise 11 in the second session and, exercise 12 in the last session. Exercise (9) aimed to demonstrate to the subjects that the initial, frequently impulsively chosen solution to a problem is often not the best and that it is better to wait and reflect before taking action. Exercise (10) intended to give the subjects practice on how to make a decision between two choices and considering the advantages and disadvantages of each alternative solution to the problem. Exercise (11) is essentially the same as exercise 10 but is on a cassette tape for variety and further practice via an audio rather than a visual modality. Exercise (12) intended to give the subjects practice in all four stages of the problem-solving. Five problem situations are presented. The researcher used the following learning strategies; Modeling, Role play/ behavioral rehearsal, Getting participants feedback, and Positive reinforcement. A. At the end of the intervention, post test was done using the study tools for both the study and control groups. B. According to the baseline scores on the study tools, comparison was done between pre and post tests in both the study and the control groups.
A. Study procedure was revised and approved by the Ethical Committee of the Faculty of Nursing, Alexandria University and by Human Rights Protection Committee of the General Secretariat of Mental Health in Cairo. B. Throughout the study steps informed oral consent was obtained from each patient participated in the study. C. Data confidentiality was assured. D. Patient’s privacy and anonymity were respected.
The collected data were tabulated and statistically analyzed using the Statistical Package for Social Sciences (SPSS) software package version 16.0. Number and percentage were used for describing and summarizing qualitative data. Minimum and maximum were used for describing and summarizing quantitative data. Mean and Standard deviation were calculated. It was used for measuring the degree of variability in a set of scores. The distribution of quantitative variables was tested for normality using Kolmogorov-Smirnov test, Shapiro-Wilk test. The tests' result revealed that the data were abnormally distributed, non- parametric tests were used. For qualitative data, Chi-square test, Fisher's Exact test, and Monte Carlo test were used. Intra group comparisons of the MEPS within the study group and control groups were performed using Marginal Homogeneity and Wilcoxon Signed Ranks Test. Mann-Whitney Test (Z) was used to compare means between the study group and control one. Correlation between two quantitative variables were assessed using Spearman coefficient test.
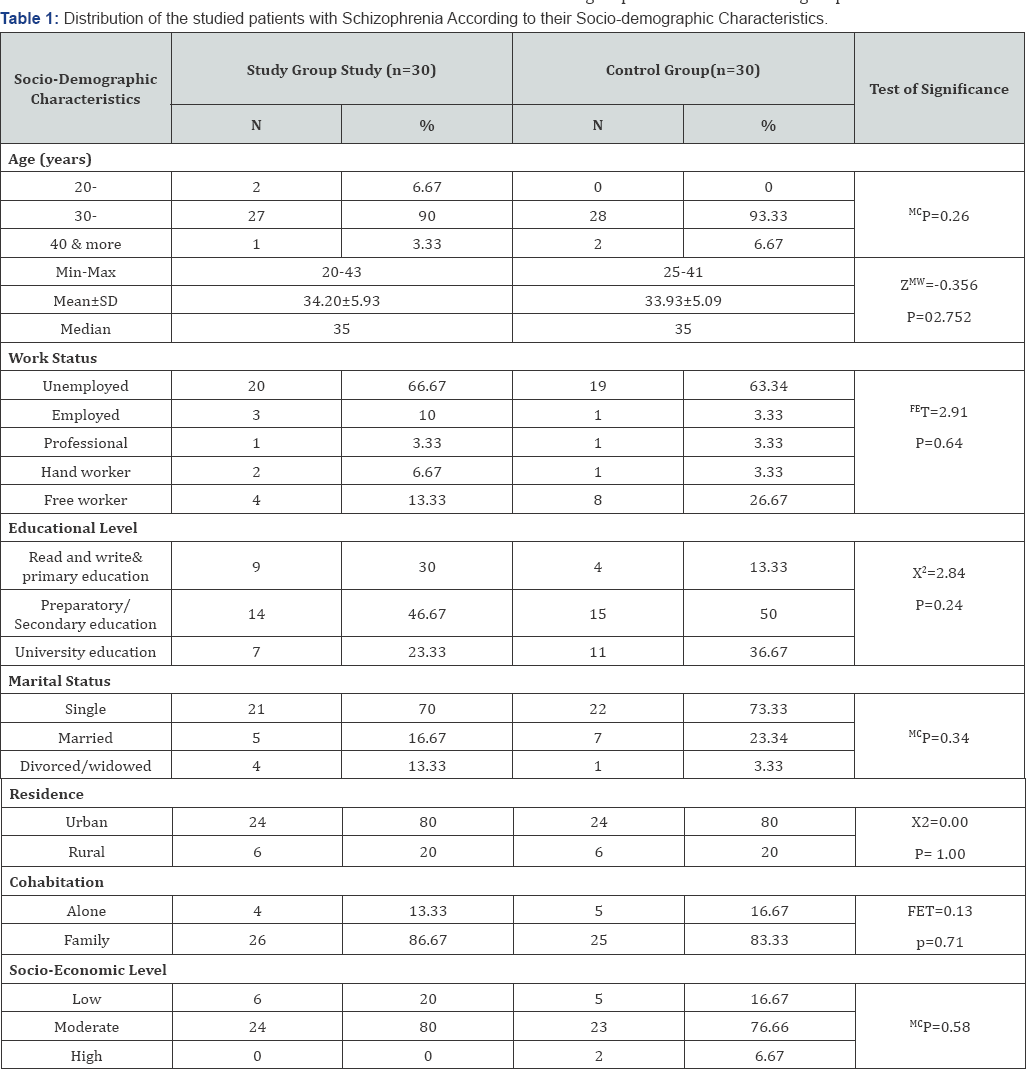
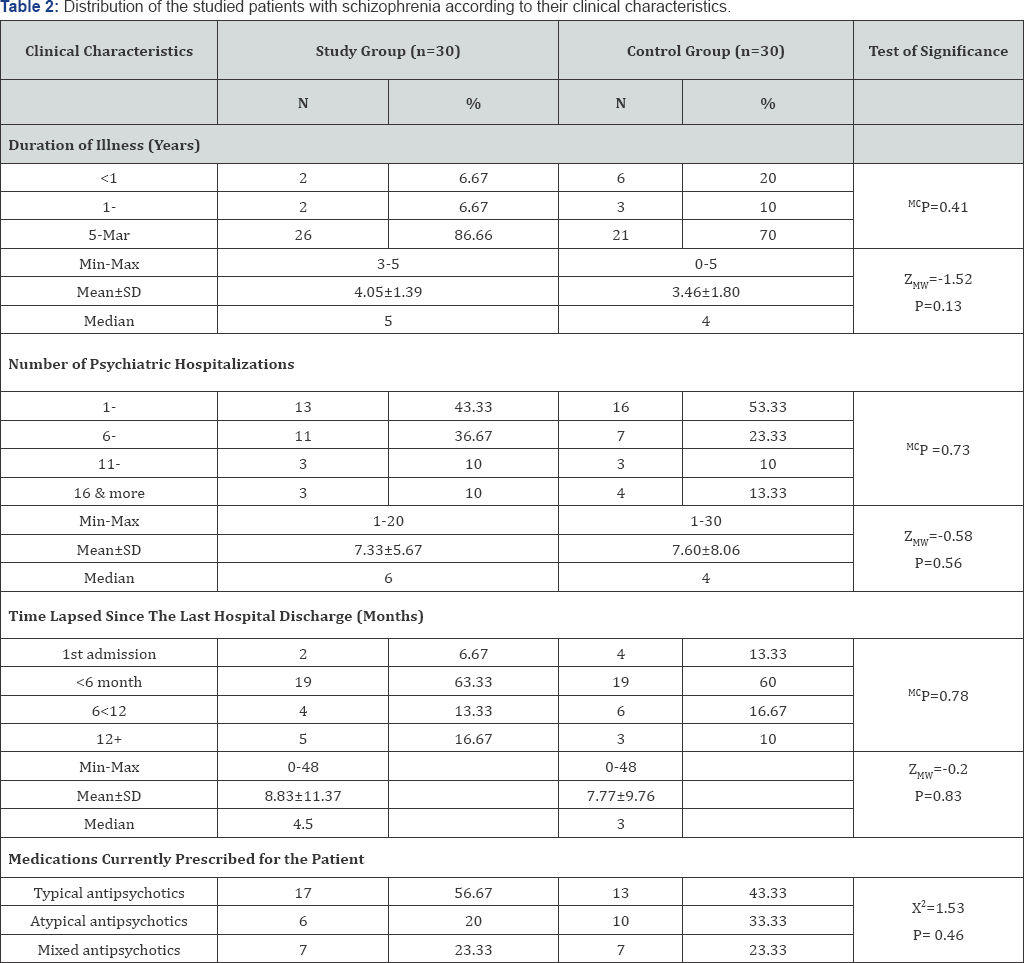
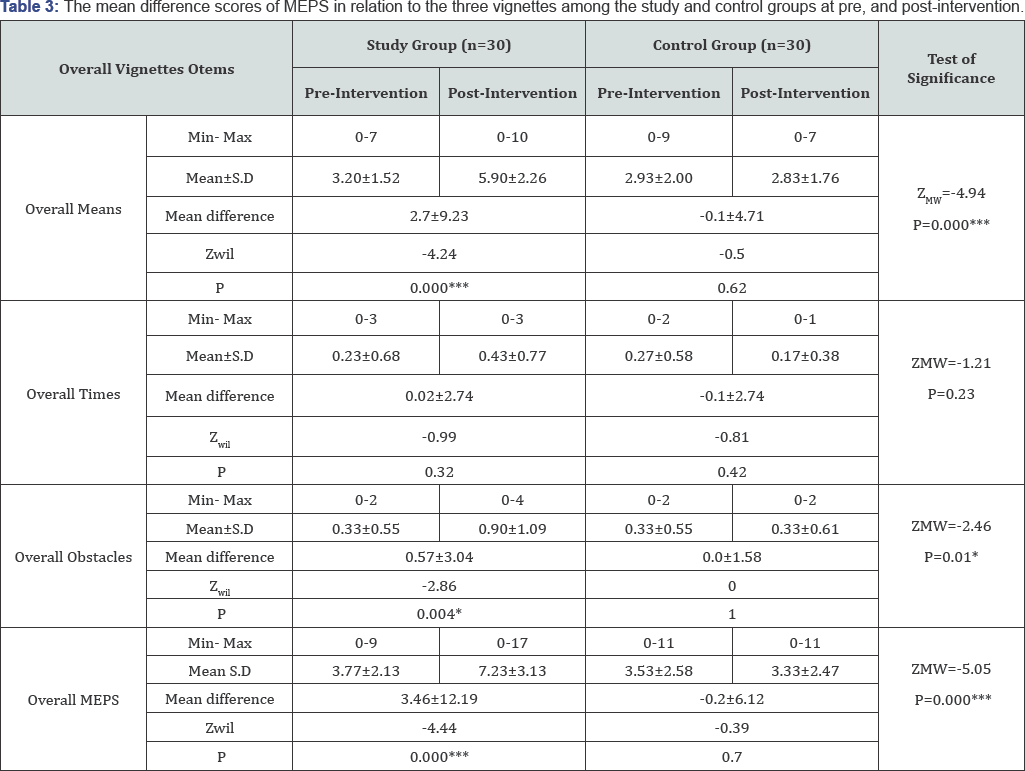
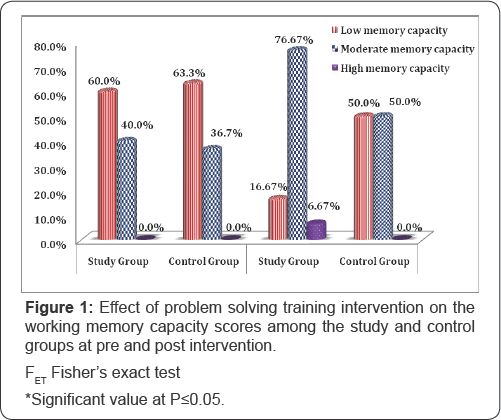
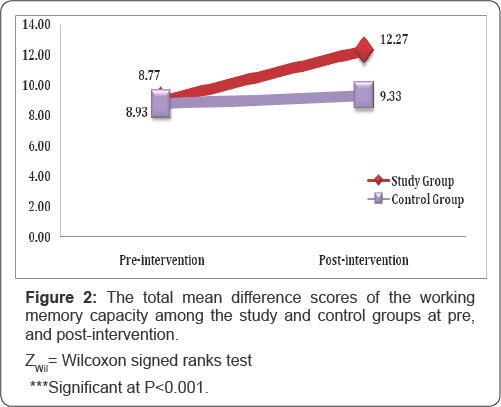
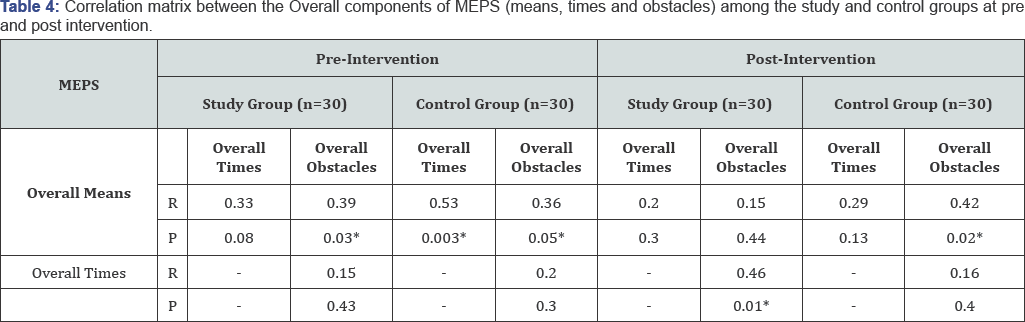
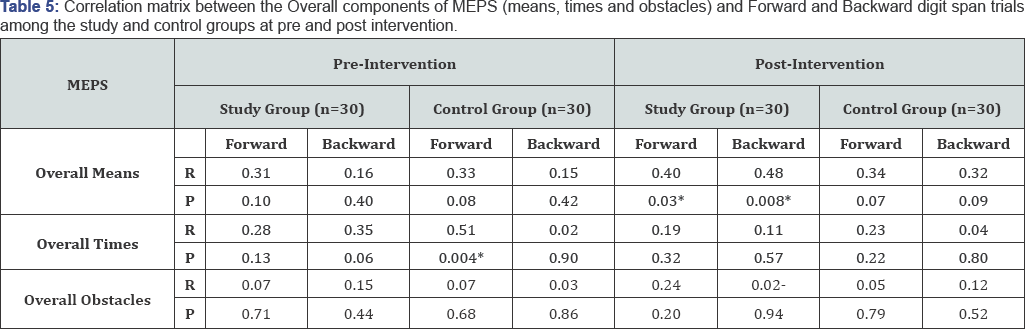
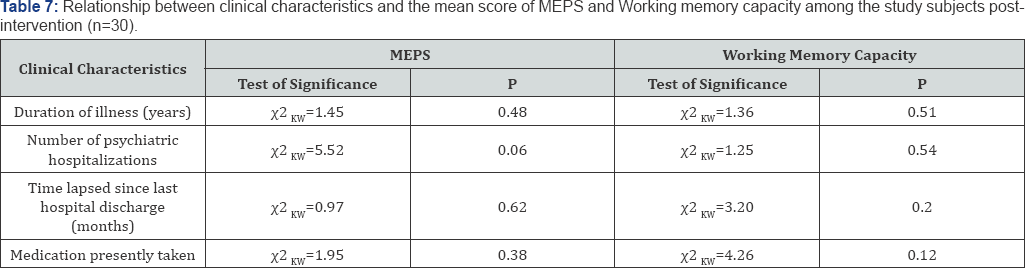
Table 1 summarizes the socio- demographic characteristics of the study and control groups. No statistically significant difference was found in relation to all socio- demographic characteristics. The absence of any statistically significant difference between the studied groups can reflect that both groups were almost matched. FET: Fisher's Exact test; X2: Chi-square test; MCP: Monte Carlo test; Z : Mann Whitney test; *Significant value at P ≤0.05. MCP: Monte Carlo test X2: Chi-square test ZMW: Mann Whitney test *Significant at P≤0.05 Table 2 presents the distribution of the studied patients with study and control group in relation to duration of illness, number schizophrenia according to their clinical characteristics, there of psychiatric hospitalization, time lapsed since the last hospital was no statistically significant differences noticed between the discharge, and medications currently prescribed for patients. ZWil= Wilcoxon Signed Ranks Test; ZMW: Mann Whitney test *Significant at P≤0.05 **P<0.001 ***P<0.001. Table 3 displays the mean difference scores of MEPS in relation to the three vignettes among the study and control groups at pre, and post-intervention. It can be noticed that the mean score of the overall means in the study group increased from 3.20±1.52 pre- intervention to 5.90±2.26 post- intervention, with a highly statistically significant difference (ZWil=-4.24, P=0.000). Comparing the mean difference score between the study and control groups post- intervention, a highly statistically significant difference between both groups was observed (ZMW=-4.94, P=0.000).The mean difference score of the overall obstacles at post- intervention in the study group was 0.57±3.04 compared to 0.0±1.58 in the control group. A statistically significant difference between the two groups was noticed (ZMW=-2.46, P=0.01). Moreover, the displayed table showed that at post- intervention phase, the mean difference score of the overall MEPS among the study group was 3.46±12.19 compared to -0.2±6.12 in the control group. A highly statistically significant difference between both groups was observed (ZMW=-5.05, P=0.000). Figure 1 shows the effect of problem solving training intervention on the working memory capacity scores among the study and control groups at pre, and post intervention. It was noticed from this figure that at post- intervention phase the percentage of the studied patients who had low working memory capacity dropped to 16.67% for the study group compared to 50.00% for the control one. Likewise, more than three quarters of the study group had moderate working memory capacity (76.67%) compared to half of the control group (50.00%). Furthermore, the same figure showed that none of both study and control groups (0.0%) demonstrates high working memory capacity at pre-intervention phase. Whereas, post-intervention 6.67% of the study group had high working memory capacity compared to none of the control group (0.0%), with a statistically significant difference between them (FET = 8.27, P=0.01) Figure 2 presents the total mean difference scores of the working memory capacity among the study and control groups at pre, and post-intervention. The figure shows that the total mean scores of the working memory capacity increased from 8.93±2.30 before intervention to 12.27±3.49 post- intervention, with a mean difference score of 3.34±2.06. Yet, a highly statistically significant relation was found (ZWil= -3.64, P=0.000). r: Spearman's rho coefficient. *: Statistically significant at P≤0.05. **: Statistically significant at P≤0.001. Table 4 displays the correlation matrix between the overall components of MEPS (means, times, obstacles) among the study and control groups at pre and post intervention phase. From this table it can be concluded that at pre- intervention phase, a significant positive correlation was found between the overall means and the overall obstacles among the study group (r=0.39, p=0.03). Whereas, the overall means was positively and significantly correlated with both the overall times and the overall obstacles among the control group (r=0.53, p=0.003 and r=0.36, p=0.05, respectively).Also, the overall means was positively correlated with the overall obstacles among the control group post- intervention (r=0.42, p=0.02). r: Spearman's rho coefficient. *: Statistically significant at P≤0.05. **: Statistically significant at P≤0.001. Table 5 presents the correlation matrix between the overall components of MEPS (means, times, obstacles) and forward and backward digit span trials among the study and control groups at pre and post intervention. The table shows a statistically significant correlation between the overall means and the forward and backward digit span test among the study group at post-intervention phase (r=0.40, P-0.03 and r=0.48, P-0.008, respectively). Moreover, the displayed table showed a statistically significant correlation between the overall times and the forward digit span test among the control group at pre- intervention phase (r=0.51, P=0.004). ZMW: Mann Whitney test, x2 KW: Kruskal Wallis Test. Table 6 shows the relationship between socio-demographic characteristics and the mean scores of MEPS and working memory capacity among the study subjects post-intervention (n=30). No statistically significant association was found between the studied patients' socio-demographic characteristics and their mean scores on MEPS and working memory capacity. X2 KW: Kruskal Wallis Test. Table 7 shows the relationship between clinical characteristics and the mean scores of MEPS and working memory capacity among the study subjects post-intervention (n=30). No statistically significant associations were detected between the mean scores of MEPS and working memory capacity of the studied subjects and their clinical characteristics.
The interpersonal problem solving ability in the present study was assessed by the patients’ abilities to address three main dimensions namely; means, times and obstacles. Results of the present study showed that patients who received interpersonal problem-solving training intervention exhibited greater improvement in the mean score of the overall means compared to the control group. These results may be attributed to the acquired competencies and skills developed during the implementation of the interpersonal problem-solving program itself, as the training program encompasses a wide array of exercises that all aimed at providing patients in the study group with the opportunities to apply several mental skills including; attention, memorizing, executive functioning, abstraction, reasoning, cognitive flexibility, self-monitoring, problem-solving abilities, planning and decision making. Presumably, by using such skills, the cognitive functions of the patients improved and hence it is reflected in their abilities to solve the displayed interpersonal problems. For example, exercise! & 2 (Paying attention and Memory for Faces, respectively) are intended to give patients of the study group some practice in paying attention to the changes that happened in the context of interpersonal interactions. This in turn helped them in recognizing problems, when they arise and how they could be solved. Paying attention to the ever-changing environment might ultimately sharpen the patients' awareness to identify the different emotions concerning others' feelings. This is clearly evident in the present study in exercise 3 (Magazine Faces), in which patients of the study group learned to identify emotions concerning others' feelings via decoding the different emotional states from the displayed pictures and making up a story about why the person in the displayed pictures has experienced such emotions. Accordingly, this exercise allows patients of the study group to learn that when they are involved in a relationships, they should understand others' implied intentions/thoughts and emotions through their visual signals or facial expressions. Irani et al. [15] found that teaching patients with schizophrenia to recognize other's emotions, generate solutions to everyday social problems and develop social interactional skills (e.g. eye contact) that could help in maximizing their social problem solving skills. The time factor as one dimension of the interpersonal problem solving ability; is concerned with the awareness of patients in the study group that solving the encountered problems might take some time or they must wait for a propitious moment to carry out the mean of the plan. Result of the present study showed that at post-intervention phase, the mean score of the overall time improved insignificantly among patients of the study group compared to the control one. This insignificant improvement could be partly explained by the nature of the disease and its pernicious effect on the impulse control, that makes the probability to weigh the consequences of their actions either for themselves or for others difficult. Needless to say that impulsiveness is a salient feature in patients with schizophrenia [16]. It is worth noting that at post-intervention phase, the abilities of patients in the study group to address the obstacles that might interfere with solving the displayed problems were improved after conducting the training intervention. This improvement may be attributed to the effect of the training program on improving the meta cognitive skills of the patients in the study group. For example, in exercise 5 (Thirty Questions); patients practiced the skills of asking questions in an organized and unambiguous way about the displayed problems. In this respect, this exercise entailed them to stand outside of their own experience in order to reflect upon self from the perspective of others. In addition, to make ongoing monitoring or introspecting on their own thoughts, feelings and behaviors. Ultimately, they can plausibly think about the possible causes and obstacles of the displayed problem. In other words, such exercise might enhance the studied patients with schizophrenia to attend to the displayed social problems, and become emotionally involved in order to infer what another person might feel by adopting the other person's point of view. The present study findings demonstrated that the mean score of the overall MEPS among patients of the study group significantly improved after the program implementation compared to the control group. Again, this might be true as the problem-solving training exercises could provide patients in the study group with the opportunity to identify problems accurately, form a detailed picture about what other people are thinking and feeling in a given situation (i.e. improve awareness of others' feelings as well as themselves), to take others’ points of view, and to negotiate between one's wishes and the demands of the relevant others to manage relationships successfully. Additionally, they practiced the skills of thinking about alternatives ways to solve problems, deciding to select the most effective solution, and evaluate the pros and cons associated with implementation of the best alternative. It can be said that the use of the interpersonal problem-solving program as an intervention enhanced the higher-order cognitive functioning including; their metacognitive skills. Metacognition, as a high level mental process, is associated with the enhancement of the problem-solving skills [17,18]. Lysaker et al. [17] reported that patients with schizophrenia who have lesser metacognitive capacities tend to have fewer enduring social relationships and fewer of the necessary foundations needed for relatedness [19]. However, metacognitive skills were not assessed in the present study. Therefore, the efficacy of the problem-solving training program on the metacognitive skills of patients with schizophrenia needs to be further explored. Introspection or self-reflection has also been found to be one of the key aspects of metacognitive skills [20]. In this respect; the training program in the current study could contribute to the development of introspection among patients in the study group, that might in turn, improve their problem solving ability. For example, exercise 8 (Creating Alternatives); patients of the study group are presented with different interpersonal problems (e.g. getting along with individual's boss, amusing oneself when alone) and they were asked to generate their own solutions to such given problems. Therefore, patients in the study group would have the chance to introspect deeply into their inner experience, and to analyze their own thoughts and feelings in order to construct a complete description of their own mental state in which they are involved. Hence, such practice increases their self-awareness to recognize the effective strategies to solve the problem at hand. Lysaker et al. [17] demonstrated that the awareness of one’s own thoughts and feelings was linked to understanding mutuality and psychological mindedness about interpersonal relationships [21]. Furthermore, the effectiveness of the problem solving training program in the current study could be attributed to using training exercises which enhanced the assertiveness skills among patients in the study group. This could be justified in the light of the findings of Yurtsa & Ozdemir [22] who found that problem-solving skills can be affected by the individuals' competencies in their social interactions, including taking an active role and assertiveness skills [22]. Assertiveness skills encompasses nonverbal communication skills such as; the importance of maintaining eye to eye contact, the appropriate use of facial expression, proxemics, developing skills in asking questions and so on [23]. All of these were already practiced and role played by the experimental group all over the program sessions. For instance, exercise 6 (Finding out about people); this exercise aimed at teaching the patients various ways that people can use to find out about other people thinking and feelings. The study group learned and practiced how to get required information by asking the other partners direct questions about what they might think and feel in relation to certain subjects. In addition, how to be assertive in getting the information and not taking the word of the third party about the person in whom they are interested but interacting with this person directly. Concerning the working memory capacity, results of the present study revealed that the total mean scores of the working memory capacity among the study group has significantly improved post-intervention compared to the control one. This result could be attributed to the training exercises which allowed patients to sustain focusing, constantly maintaining and updating the context of information concerning social interactions, through counteracting the patients' disrupting mental representation or being distracted by internal or external events (e.g. hallucination or noise). Additionally, to maintain conscious storage of information needed to execute cognitive tasks such as processing of information, sequencing of mental operations, reasoning, strategic planning, problem solving and decision making. Veltro et al. [24] found that the problem solving program improved the schizophrenic subjects' problem solving strategies and working memory capacity. They became more skilled in defining their problem/goal, identifying the possible solutions, choosing an appropriate solution and evaluating the chosen plan of action. Moreover, a variety of behavioral techniques were used in the current problem-solving training program, the demonstration of the modeled behavior helped patients of the study group to selectively attend to social stimuli, ignore extraneous sensory output in order to maintain adequate task-relevant information, manipulate information, access relevant stored memories, and select appropriate actions, hence, improving their working memory capacity and problem solving abilities. In this respect, Eskin [25] postulated that modeling can provide more efficient and effective means for teaching new behavior as well as motivating patients with schizophrenia to change unacceptable behaviors during the practice of the problem-solving training program. Positive reinforcement for the desired behavior was another related technique used throughout the training program in the present study. The researcher provided continuous reinforcement for the engagement and compliance on attending the sessions. Behavioral theories argued the importance of direct reinforcement as a way to modify or change undesirable behavior as well as increase the probability of a behavior being repeated. According to Rodewald et al. [26], positive reinforcement was particularly relevant to the basic cognitive training, in which learning from positive reinforcement and feedback was essential for improving the problem-solving ability among patients with schizophrenia. Collectively, it can be possible to draw a conclusion that the interpersonal problem solving training program contributed positively in widening the schizophrenic patients’ horizons of thinking about more means, times and obstacles to solve their encountered interpersonal problems. However, this improvement might be specifically to the cognitive tasks that are mostly related to problem-solving ability and working memory capacity, it could be also generalized to other cognitive functioning (e.g: attention, visual processing, cognitive flexibility & social cognition). Perhaps this because that the training program enables the schizophrenic patients to master such cognitive operations required for dealing with the interpersonal problem situations, which in turn, enhance their working memory capacity. Therefore, it is necessary for the mental health nurses to offer patients with the therapeutic experiences that allow them to bridge between the skills acquired in training program and those needed for real-life functioning.
According to the findings of the present study, it can be concluded that the problem solving training intervention; that is concerned with the problems arising within the interpersonal context during the everyday social interactions, contributed positively in the enhancement of the interpersonal problemsolving ability and working memory capacity among patients with schizophrenia. The problem solving training intervention should be incorporated in the psychiatric hospitals' protocol of care including written guidelines about the appropriate way of the program application.
Abstract
Introduction
The Aim of the Work
Materials and Methods Design of the Study and Setting
Inclusion criteria
Tools of the study
The training intervention
Planning phase
Implementation phase
Evaluation stage
Ethical Considerations
Statistical Analysis
Results

Discussion
Conclusion
References






























