Coping and Mental Health of Children with Special Needs in the Gaza Strip
Abdelaziz Mousa Thabet*
1Emeritus Professor of Child and Adolescent Psychiatry, Al Quds University, Palestine
Submission: September 06, 2017; Published: September 22, 2017
*Corresponding author: Thabet AA MD, PhD, Emeritus Professor of Child and Adolescent Psychiatry, School of Public Health, Al Quds University, Jerusalem, Palestine, Email: abdelazizt@hotmail.com
How to cite this article: Abdelaziz Mousa Thabet. Coping and Mental Health of Children with Special Needs in the Gaza Strip; JOJ Nurse Health Care. 2017; 4(3): 555637. DOI: 10.19080/JOJNHC.2017.04.555637
Abstract
Aim: The aim of the present study was to evaluate the prevalence of emotional and behavioral problems as estimated by the SDQ and coping strategies in Palestinian children with special needs in the Gaza Strip.
Method: The sample consisted of 79 children, parents and teachers. The age ranged from 5-17 years, mean age was 10.76.
Measures: Sociodemographic data was collected from parents, parents and teachers completed SDQ, while children completed Kidcope scale.
Results: Using SDQ for parents, 38% of children were rated as having psychological morbidity, 22.8% of them were hyperactive, 29.1% had emotional problems, 27.8% had conduct problems, 41.8% had abnormal peer problems, and 6.4% had abnormal prosocial behavior. Using SDQ for teachers, 26.6% of children were rated as having psychological morbidity, 11.4% of them were hyperactive, 2.5% had emotional, 24.1% had conduct problems, 21.5% had abnormal peer problems, and 14.1% had abnormal prosocial behavior. Children used a variety of coping strategies, the most common coping strategies were: wish the problem had never happened (91.2%), try to feel better by spending time with others like family, grown-ups or friends (86.8%), try to sort out the problem (82.4%), try to calm themselves down (82.1%), and try to sort out the problem by doing something or talking to someone about it (77.9%). The results showed that there was significant negative correlation between total coping strategies total SDQ- parents and emotional problems rated by parents.
Clinical implications: As a result of this study, service providers should concentrate on increasing services for the child with disability and assisting families to obtain information about available resources. Welfare officers have the responsibility to make sure that families receive appropriate financial assistance, especially caregivers of lower education and who themselves had medical problems. By understanding the circumstances of families caring for a child with disability, service providers can identify areas for improvement in the delivery of disability services. Future research is needed to assess caregivers of younger children and with more severe disability needed support services most.
Keywords: Children; Special needs; SDQ; Coping; Gaza strip
Introduction
Worldwide, an estimated 5% of children (about 93 million) aged 0-14 years have moderate or severe disability, with estimates ranging from 2.9% in high-income countries to 4.4-6.4% in low- income and middle-income countries [1].
Behavioral and emotional disorders include a wide range of behavioral patterns, ranging from externalizing to internalizing behavior disorders as well as combined behaviors that include features of both subtypes. Externalizing behaviors are actions that direct problematic energy outward and may include behaviors such as verbal and physical aggression, hyperactivity, noncompliance, and delinquent acts. In contrast, internalizing behaviors are directed toward the self that include social withdrawal, depression, substance abuse, feeding and eating disorders, anxiety, and schizophrenia [2]. Various studies have compared the total scores for problems between deaf and hard hearing students and hearing students using the Strengths and Difficulties Questionnaire [SDQ] [3]. Cerebral palsy (CP) is the most common cause of motor impairment in children, frequently resulting in a life-long disability in children. However, few studies have investigated the behavioral and emotional problems of children with CP. In an European multicenter study using a mental health screening instrument, Strengths and Difficulties Questionnaire (SDQ), found one in four children aged 8-12 years with CP had scores indicating mental health problems. They concluded with a need for in depth interviews to learn more about the extent of mental health problems in children with CP [4]. A similar population study from Iceland, where preschool children with CP were included, found a three to four fold increased risk for emotional and behavioral problems for these children compared to controls [5]. Other studies reported that children with CP suffered more often from emotional problems, peer problems, social withdrawal, attentional problems or dissocial behavior [6]. Matilla et al. [7] reported that 74% of children aged 9-16 years with Asperger's syndrome (AS)/ high-functioning autism (HFA) have co-existing psychiatric disorders.
Horiuchi et al. [8] in the study of 173 patients with Autistic Spectrum Disorder (ASD) (age: 4-16 years) and 173 age- and sex-matched community children (control group). The Strengths and Difficulties Questionnaire scores were significantly higher in children with ASD than controls at all ages. The score of total difficulties was significantly higher in girls with ASD than in boys, while the score in male controls was significantly higher than in female controls.
Weber et al. [9] in a two-center cross-sectional study, caregivers of 121 adults and 88 children were ask to assess behavior of the patients through the parent/caregiver forms of the Child Behavior Checklist (CBCL), the Strengths and Difficulties Questionnaire (SDQ), and the Vineland Adaptive Behavior Scale II (VABS). Questionnaires were returned from 43 adults and 39 children. Results showed that in both groups they found the same frequency of abnormalities in attention problems (32.4 vs. 36.1%) and social interaction problems (32.3 vs. 33.3%) in the CBCL, and peer problems (38.9 vs. 75.7%) in the SDQ. Children show a lower percentage of abnormal prosocial behavior (41.7 vs. 16.2%) and lower abnormal rates of communication (88.2 vs. 61.5) and daily living skills (90.0 vs. 71.8), whereas the level of abnormalities in both groups in these dimensions of VABS notably high.
Coping Strategies
According to Lazarus and Folkmans' coping defined as: 'constantly changing cognitive and behavioral efforts to manage specific external and/or internal demands that are appraised as taxing or exceeding the resources of the person' [10]. Furthermore, Lazarus [11] said coping involves a reaction focused on changing psychological stress within the context of an unfavorable person- environment relationship. Coping with disability has been described from a developmental perspective [12-14], and aspects of coping among children and adolescents with and without congenital physical disabilities have been compared in a few studies [15,16]. However, empirical research on coping strategies among children and adolescents with mobility impairment is scarce, and the relation to demographic data, disability characteristics and well-being is largely unexplored. Hearing loss is one of the disabilities in children, studies exploring coping with the psychosocial experiences of hearing loss have distinguished between engaged copings and disengaged coping [17]. Engaged coping involves taking action to manage the effects of hearing loss, such as using hearing aids or communication strategies. Disengaged coping refers to avoiding addressing hearing loss, such as by denying or ignoring it, or by withdrawing from social situations. The aim of the present study was to evaluate the prevalence of emotional and behavioral problems as estimated by the SDQ and coping strategies in Palestinian children with special needs in the Gaza Strip.
Setting and Sample
The population of this study included a total of 100 parents and teachers attending Al Amal City Centre of Ability Development, Khan Younis. The complex of buildings of this center, include- hospital, clinics, EMS services and training, College of Ability Development, Psycho-social Centre, Rehabilitation Centre (parent and baby program; special kindergarten; special training program; special education school, vocational training, physiotherapy, speech therapy, physical education and range of arts-open studio, music, toy library, library, computer centre, etc..), children's club, museum, commercial shops, production workshops, Repair & adaptation of assistive devices workshop, main theatre, small theatre, fitness centre, sports hall, all-purpose hall, restaurant & cafeterias, garden/playground. Al Amal City is a community centre, and the main beneficiaries of the range of programs and services are children, youth and adults living in the Khan Younis governorate, but there are also others from Rafah, mid-area, Gaza and the north. In addition to the number of persons with disabilities and their families and other children and adults from the community receiving benefit from programs and services of Al Amal City, it is also an important training centre for students in different specialties (rehabilitation, occupational therapy, social work, administration, library science, computer, etc) from universities and colleges of the Gaza Strip.
Measures
Sociodemographic characteristic questionnaire
This questionnaire includes sex, age, place of residence, parental information, and family income.
Strengths and difficulties questionnaire (parents and teachers) [3]
The SDQ is a brief screening scale for emotional and behavioral problems among young people aged 4-17 years of age [18]. The questionnaire is one of the most commonly used scales in the assessment of children's strengths and difficulties in child psychiatry [19-21]. It consists of 25 items, 14 describe perceived difficulties, 10 perceived strengths and one is neutral ('gets on better with adults than with other children'). Each perceived difficulties item is scored on a 0-2 scale (not true, somewhat true, certainly true). Each perceived strengths item is scored in the reverse manner, i.e. 2: not true, 1: somewhat true, 0: certainly true. There are three versions of this questionnaire, one for parents, teachers, and one for children above 11 years. The 25 SDQ items are divided into scales of Hyperactivity, Emotional Problems, Conduct Problems, Peer Problems and Prosocial Scale (five items per scale). A score is calculated for each scale (range 0-10) and a total difficulties score for the four scales (excluding prosocial behavior, which was considered different from psychological difficulties), i.e. a range of 0-40. The SDQ has been previously used in the Palestinian culture [22,23]. In this study, internal consistency for parents from using Cronbach's Alpha was high (α=0.84); the split half reliability of the scale was (α= 0.79).
The kidcope[24]
This self-report checklist [24] requires the child to think about a specific situation and to assess which of 15 coping strategies they have used. The strategies and items are distraction (e.g. try to forget it; do something else to forget it); social withdrawal (stay on your own; keep quiet about the problem); cognitive restructuring (try to see the good side of things); self-criticism (blame yourself for causing the problem); blaming others (blame someone else for causing the problem); problem solving (try to sort the problem out by thinking of answers or talking to someone about it; try to sort it out by doing something); emotional regulation (shout, scream, get angry; try to calm yourself down); wishful thinking (wish the problem had never happened; wish you could make things different); social support (try to feel better by spending time with others like family- parents, brothers or sister; try to feel better by spending time with friends); resignation (do nothing because the problem could not be solved). The child rates both use and perceived effectiveness of each strategy. The authors conceptually selected the strategies after reviewing the coping literature. The scale has been used with healthy adolescents, pediatric patients and children attending a diabetic camp. The psychometric properties have been reported and indicate moderate to high correlations between Kidcope and the Coping Strategies Inventory and Adolescent Coping Orientation for Problem Experiences (ACOPE) [24]. Reliability, determined by assessing coping strategies across two similar situations found moderate correlations (.56-.72) with test-retest correlation assessed over 3-7 days demonstrating acceptable levels of reliability (correlations .41-.83). In this study, internal consistency for using Cronbach's Alpha was high (α=0.78); the split half reliability of the scale was (0.73).
Study Procedure
A permission was granted from Amal center Administration. Another letter was send to parents explaining the aim of the study and about their right not to participate with their children in study and ask them to sign the letter and send it back to the center with children if they agree to participate with their children in the study. Data was conducted by 3 trained social workers and community mental health workers with previous experiences in data collection in similar research. Data was collected in September 2009.
Analysis
The survey questionnaire was quantitatively analyzed by statistical package for the social sciences (SPSS win, Ver. 20). Frequency distribution was used in statistical analysis. Independent t-test for the sample and One-way.
Analysis of Variance (ANOVA) was used as the main statistical techniques in the study. The t-test was used to determine any statistically significant differences caused by children's gender and mental health problems, whereas ANOVA was employed to determine any statistically significant differences among parents with regard to their education, place of residence, type of work, number of siblings, and child's age. Pearson correlation test was used to test the correlation between children mental health rated by parents and teachers and coping strategies.
Results
Socio-demographic characteristics of study population
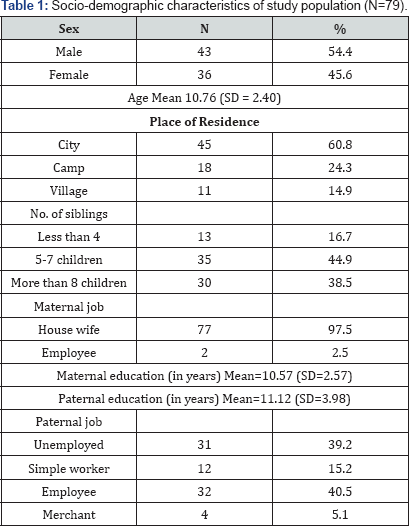
Overall, of 100 participants recruited, 79 parents and teachers (79%) completed the SDQ. The final sample consisted of 79 children with special needs (36 girls, 43 boys), aged 5 years to 17 years and their parents and teachers, 54.4% were boys and 45.6% were girls. The age ranged from 5-17 years, mean age was 10.76 (SD=2.40).
Children families consisted of large number of children, as 13 (16.7%) had 4 or less children, 35 families (44.9%) had 5-7 children, and 30 families (38.5%) had 8 or more children. Forty- five (60.8%) live in the city, 18 of children (24.3%) live in camps, and 14/9% live in village (Table 1).
Psychological symptoms of children rated by parents using SDQ -parents form
The most common psychological symptoms rated by parents were: shares readily with other children (treats, toys, pencils etc.) (78.5%), kind to younger children (75.9%), often volunteers to help others (parents, teachers, other children) (70.9%), considerate of other people's feelings (62.8%), helpful if someone is hurt, upset or feeling ill (60.8%), gets on better with adults than with other children (41.8%), restless, overactive, cannot stay still for long (39.2%), has at least one good friend (39.2%), can stop and thinks things over before acting (38%), many fears, easily scared (38%), easily distracted, concentration wander (30.4%), and often has temper tantrums or hot tempers (25.3%).
General mental health problems using SDQ by parents
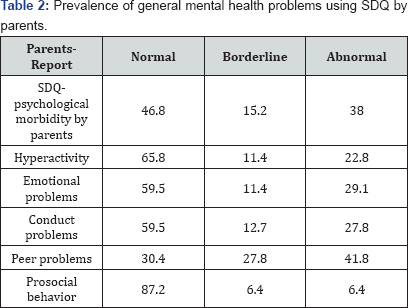
Prevalence of general mental health problems using SDQ by parents: Using SDQ for parents, 38% of children were rated as having psychological morbidity (were considered as having a problem) (cut-off point =17-40), 22.8% of them were hyperactive (7-10), 29.1% had emotional problems (5-10), 27.8% had conduct problems (4-10), 41.8% had abnormal peer problems (4-10), and 6.4% had abnormal prosocial behavior (0-4). Independent t test showed no gender differences in total SDQ-parents. Oneway Analysis of Variance (ANOVA) tests showed no significant differences in number of siblings and total SDQ parents (Table 2).
Psychological symptoms of children rated by teachers: The most common psychological symptoms rated by parents were: Shares readily with other children (treats, toys, pencils etc.) (68.9%), kind to younger children (54.7%), restless, overactive, cannot stay still for long (44%), often volunteers to help others (parents, teachers, other children) (44%), helpful if someone is hurt, upset or feeling ill (40%), considerate of other people’s feelings (30.7%), has at least one good friend (29.3%), often fights with other children or bullies them (21.3%), and can stop and thinks things over before acting (21.3%).
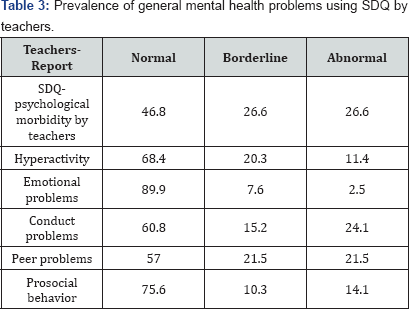
Prevalence of general mental health problems using SDQ by teachers: Using SDQ for teachers, 26.6% of children were rated as having psychological morbidity (cut-off point =17-40), 11.4% of them were hyperactive (7-10), 2.5% had emotional problems (5-10), 24.1% had conduct problems (4-10), 21.5% had abnormal peer problems (4-10), and 14.1% had abnormal prosocial behavior (0-4). One-way Analysis of Variance (ANOVA) tests showed no significant differences in number of siblings and total SDQ teachers (Table 3).
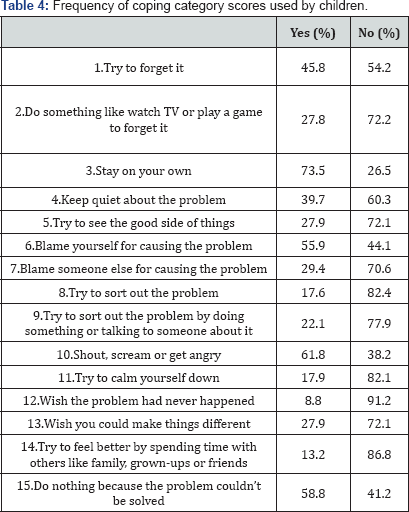
Coping with trauma and stress in children (Kidcope): Children used a variety of coping strategies, the most common coping strategies used by children to overcoming the problems and stress were: wish the problem had never happened (91.2%), try to feel better by spending time with others like family, grownups or friends (86.8%), try to sort out the problem (82.4%), try to calm themselves down (82.1%), and try to sort out the problem by doing something or talking to someone about it (77.9%). Independent t test showed no gender differences in total coping strategies of children (Table 4).

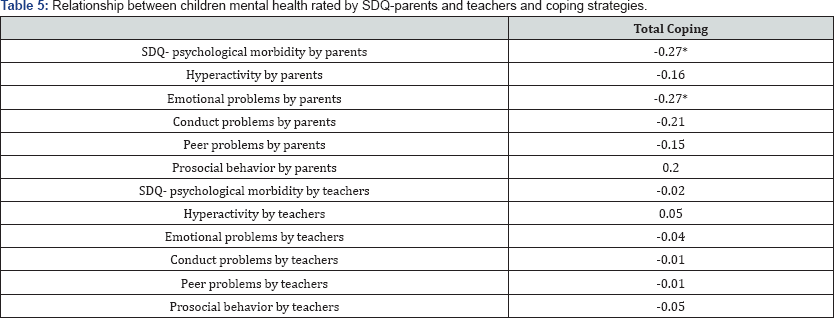
Relationship between children mental health rated by SDQ-parents and teachers and coping strategies: Pearson correlation test was used to test the correlation between children mental health rated by parents and teachers and coping strategies. The results showed that there was significant negative correlation between total coping strategies total SDQ- parents (r = - 0.27, p = 0.001) and emotional problems rated by parents (r = - 0.27, p = 0.001) (Table 5).
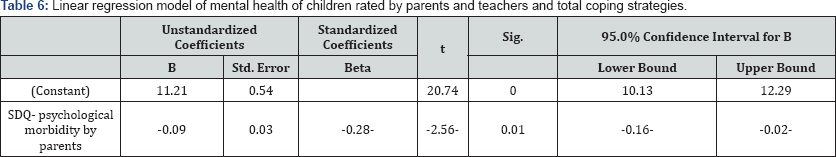
Prediction of coping strategies by mental health problems rated by teachers and parents: In a linear regression model, mental health problems rated by parents and teachers were entered as an independent variables and total coping strategies as dependent variable. Psychological morbidity by parents was negatively predicting coping strategies: (β=-0.28, t (79), p<0.001), R2 = .07, F(1, 79) = 5.47, p< .01 (Table 6).
Discussion
Using SDQ for parents, our study showed that 38% of children were rated as having psychological morbidity, 22.8% of them were hyperactive, 29.1% had emotional problems, 27.8% had conduct problems, 41.8% had abnormal peer problems, and 6.4% had abnormal prosocial behavior. No gender differences in total SDQ-parents. Using SDQ for teachers, 26.6% of children were rated as having psychological morbidity, 11.4% of them were hyperactive, 2.5% had emotional problems, 24.1% had conduct problems, 21.5% had abnormal peer problems, and 14.1% had abnormal prosocial behavior. No significant differences in total SDQ teachers and number of siblings. Similarly in study of mental health problems of children diagnosed with CP in Gaza, showed that prevalence of child behavior problems rated by parents was (37%). While, the prevalence of child behavior problems rated by therapist was (44.7%). There was discrepancy on detection of caseness between parents and therapists. Therapists were detecting child behavior problems in CP children more than the parents. There were no statistical significance differences between boys and girls in total child emotional and behavioral problems and internalizing problems, however boys scored more than girls in externalizing problems [25]. Our results support previous findings regarding a high prevalence of emotional and behavioral problems in children with CP (46%) [26]. The proportion of children with possible psychopathology in our study is similar to the proportion a study (40%), using similar instruments (a direct interview with Strength and Difficulties Questionnaire (SDQ) [4]. In another study of 374 traumatized children in Gaza Strip. The study showed that 59.9% of children rated themselves as having psychiatric morbidity compared to 61.5% by parents' report, 17.4% reported hyperactivity compared to 23.5% by parents' report, 57.2% reported emotional problems compared to 51.9% by parents' report, 72.7% reported conduct problems compared to 82.1% by parents report, 32.9% reported peer relationships compared to 40.6% by parents' report, and 8% reported social problems compared to 13% by parents’ report [27]. Furthermore, Thabet et al. [23] in study of a sample consisted of 391 disable Palestinian children in the Gaza Strip which was selected randomly from the data base of two NGOs working with such group of children. The results showed that children reported mean conduct disorder was 1.33; oppositional disorder was 5; mean overanxious was 6.75; separation anxiety mean was 6.36; and depression was 7.57. There were statistically significant differences toward boys in depression. According to parents, mean conduct disorder mean was 1.94; mean oppositional disorder was 6.09; mean overanxious was 7.47; separation anxiety mean was 6.48; and mean depression was 9.6. The study showed that mean depression in boys was 10.4 compared to 8.9 in girls. There were statistically significant differences toward boys in depression. Recently in a study a sample of 816 middle school students from both genders, who were randomly selected from different schools in two big cities in Oman, participants' self-ratings were the highest on the emotional symptoms (29.2%) and peer problems (20.2%) subscales, followed by hyperactivity (17.4%) and conduct problems (13.8%). With regards to the borderline range, participants were rated the highest on emotional symptoms (15.1%), peer problems (15.3%) followed by conduct problems (13.1%) and hyperactivity (12.9%), respectively. Almost half of the participants showed some type of emotional and behavioral difficulties as reflected by the difficulty score (32.1%) in the clinical range and 20% in the borderline range) [28].
Children used a variety of coping strategies, the most common coping strategies used by children to overcoming the problems and stress were: wish the problem had never happened (91.2%), try to feel better by spending time with others like family, grownups or friends (86.8%), try to sort out the problem (82.4%), try to calm themselves down (82.1%), and try to sort out the problem by doing something or talking to someone about it (77.9%). Independent t test showed no gender differences in total coping strategies of children. The results showed that there was significant negative correlation between total coping strategies total SDQ- parents and emotional problems rated by parents. Previous studies of traumatized children in the Gaza Strip showed that Palestinian adolescents mainly cope commonly by developing social support, investing in close friends, and/ or engaging in demanding activities. The study showed that adolescents experienced traumatic experiences developed less social support and positively asked more professional support as coping strategies [29,30].
Studies exploring coping with the psychosocial experiences of hearing loss as one of the disabilities in children have distinguished between engaged copings and disengaged coping [17]. Engaged coping involves taking action to manage the effects of hearing loss, such as using hearing aids or communication strategies. Disengaged coping refers to avoiding addressing hearing loss, such as by denying or ignoring it, or by withdrawing from social situations. In another study of children in south of Gaza Strip, Thabet [23] showed that children used a variety of coping strategies. The most common coping strategies used by children were: 71.6% of children said they go along with their parents and rules, 64.1% try to improve themselves (get body in shape, get better grades, etc.), 64.1% of them pray, 59.9% work hard on schoolwork or other school projects, 52.8% do things with their family. While the least common coping strategies used were: drinking beer, using sedatives (4.6%) and smoking (3.1%).
Implications
For the time being, service providers should concentrate on increasing services for the child with disability and assisting families to obtain information about available resources. Welfare officers have the responsibility to make sure that families receive appropriate financial assistance, especially caregivers of lower education and who themselves had medical problems. By understanding the circumstances of families caring for a child with disability, service providers can identify areas for improvement in the delivery of disability services. Future research is needed to assess caregivers of younger children and with more severe disability needed support services most. More attention should also be directed at children with learning disability so that their caregivers get the information and coping strategies that they need [31-34].
Limitations of the Study
The study is restricted by some limitations that hinder the generalization of its findings:
A. The number of children with disability was relatively low. Therefore, I am still hesitant to generalize the interpretation of this analysis since the number of children with disability in each behavior is small.
B. The study sample includes parents and teachers of children with different types of disability attending one center for such group and from only one city in Gaza Strip (Khan Younis).
C. The study uses mainly the questionnaire as a research instrument, whereas other instruments such as interviews and observation reports were not used.
D. Data were collected using a survey model.
Acknowledgement
We are grateful for families and teachers of children who helped us in finishing this study.
References
- http://www.who.int/healthinfo/global_burden
- Kauffman JM, Landrum TJ (2013) Characteristics of emotional and behavioral disorders of children and youth, (10th edn), Boston: Pearson/Merrill.
- Goodman R (1997) The strengths and difficulties questionnaire: A research note. J Child Psychol Psychiatry 38(5): 581-586.
- Parkes J, White-Koning M, Dickinson HO, Thyen U, Arnaud C, et al. (2008) Psychological problems in children with cerebral palsy: A cross-sectional European study. J Child Psychol Psychiatry 49(4): 405413.
- Sigurdardottir S, Indredavik MS, Eiriksdottir A, Einarsdottir K, Gudmundsson HS, et al. (2010) Behavioral and emotional symptoms of preschool children with cerebral palsy. A population-based study.Dev Med Child Neurol 52(11): 1056-1661.
- Brossard-Racine M, Hall N, Majnemer A, Majnemer A, Michael I, et al. (2012) Behavioral problems in school age children with cerebral palsy. Eur J Paediatr Neurol 16(1): 35-41.
- Mattila ML, Hurtig T, Haapsamo H, Jussila K, Kuusikko-Gauffin S, et al. (2010) Comorbid psychiatric disorders associated with Asperger syndrome/high-functioning autism: a community- and clinic-based study. J Autism Dev Disord 40(9): 1080-1093.
- Horiuchi F, Oka Y, Uno H, Kawabe K, Okada F, et al. (2014) Age- and sex- related emotional and behavioral problems in children with autism spectrum disorders: comparison with control children. Psychiatry Clin Neurosci 68(7): 542-550.
- Weber P, Bolli P, Heimgartner N, Pierina Merlo P, Zehnder T, et al. (2016) Behavioral and emotional problems in children and adults with cerebral palsy. Eur J Paediatr Neurol 20(2): 270-274.
- Lazarus RS, Folkman S (1984) 'Coping and adaptations.' In: Gentry WD (Ed.), Handbook of Behavioral Medicine, Guilford, New York, pp. 282325.
- Lazarus RS (1993) From psychological stress to the emotions: a history of changing outlooks. Annu Rev Psychol 44: 1-22.
- Williamson GG, Zeitlin S (1988) Enhancing the coping of young children with disabilities. Pediatr Ann17: 778-83.
- Anderson EM, Clarke L, Spain B (1982) Disability in adolescence. Methuen & Co, England, pp. 319-341.
- Carlson CE, Ricci J, Shade-Zeldow Y (1990) Psychosocial aspects of disability in children. Pediatrician 17(4): 213-221.
- Monsen RB (1992) Autonomy, coping, and self-care agency in healthy adolescents and in adolescents with spina bifida. J Pediatr Nurs 7(1): 9-13.
- Janelle S (1992) Locus of control in nondisabled versus congenitally physically disabled adolescents. Am J Occup Ther 46(4): 334-342.
- Heffernan E, Coulson N, Henshaw H, Barry JG, Ferguson MA, et al. (2016) Understanding the psychosocial experiences of adults with mild moderate hearing loss: An application of Leventhal's self regulatory model. Int J Audiol 55(Supl 3): S3-S12.
- Goodman R (1994) A modified version of the Rutter parent questionnaire including extra items on children's strengths: A research note. J Child Psychol Psychiatry 35(8): 1483-1494.
- Goodman R, Scott S (1999) Comparing the Strengths and Difficulties Questionnaire and the child behavior checklist: Is small beautiful? J Abnorm Child Psychol 27(1): 17-24.
- Goodman R, Ford T, Simmons H, Gatward R, Meltzer H, et al. (2000) Using the strengths and difficulties questionnaire (SDQ) to screen for child psychiatric disorders in a community sample. The Br J Psychiatry 177: 534-539.
- Goodman R (2001) Psychometric properties of the strengths and difficulties questionnaire. J Am Acad Child Adolesc Psychiatry 40(11): 1337-1345.
- Thabet AA, Stretch D, Vostanis P (2000) Child mental health problems in Arab children: application of the strengths and difficulties questionnaire. Int J Soc Psychiatry 46(4): 266-280.
- Thabet AA, Thabet SS (2017) Coping with trauma among children in South of Gaza Strip. Psychol Cogn Sci Open J 3(2): 36-47.
- Spirito A, Stark L, Gil K, Tyc V (1995) Coping with every day and disease-related stressors by chronically ill children and adolescents. J Am Acad Child Adolesc Psychiatry 34(3): 283-290.
- Saleh S, Thabet AA, Vostanis P (2007) Prevalence of emotional and behavioral problems in cerebral palsy children in gaza strip. Arabpsynet E. Journal: N° 15 & 16-Summer & Autumn, pp. 174-179.
- Rackauskaite G, Bilenberg N, Bech BH, Uldall P, 0stergaard JR (2016) Screening for psychopathology in a national cohort of 8- to 15-year-old children with cerebral palsy. Res Dev Disabil 171-180.
- Thabet AA, Abu Tawahina A, El Sarraj E, Vostanis P (2009) Effect of war on Palestinian children behavioural and emotional problems. Arabpsynet E Journal 24: 26-30.
- Emam MM, Kazem AM, Al-Zubaidy AA (2016) Emotional and behavioral difficulties among middle school students in Oman: an examination of prevalence rate and gender differences. Emotional and behavioral difficulties 21(3): 314-328.
- Thabet AA, Omar ELB, Panos, Vostanis (2014) Trauma, PTSD, Anxiety, and coping strategies among Palestinians adolescents exposed to War on Gaza. Arab Journal of Psychiatry 25(1): 71-82.
- Folkman S (1984) 'Personal control and stress and coping process: a theoretical analysis.' Journal of Personality and Social Psychology 46(4): 839-852.
- Goodman A, Goodman R (2012) Strengths and Difficulties Questionnaire scores and mental health in looked after children. Br J Psychiatry 200(5): 426-427.
- Scarinci N, Worrall L, Hickson L (2008) The effect of hearing impairment in older people on the spouse. Int J Audiol 47(3): 141-151.
- Shuichi U, Horiuchi F, Oka Y, Uno H, Kawabe K, et al. (2014) Age- and sex-related emotional and behavioral problems in children with autism spectrum disorders: Comparison with control children. Psychiatry Clin Neurosci 68: 542-550.
- Thabet AA, Abu Tawahina A, Henley D, Pelling H, Vostanis P, et al. (2015) Mental health and quality of life of disable palestinian children in the gaza strip. Health 7(8): 994-1006.






























