Health System Strengthening-Focussing on Referrals: An Analysis from India
Anil Kumar Gupta1, Shweta Talati2, Sudip Bhattacharya3*Amarjeet Singh4
1Professor and Head, Department of Hospital Administraion, Postgraduate Institute of Medical Education and Research, India
2Assistant professor, Department of Hospital Administration, Postgraduate Institute of Medical Education and Research, India
3Senior Resident, Department of Hospital Administration, Postgraduate Institute of Medical Education and Research, India
4Professor, School of Public Health, Postgraduate Institute of Medical Education and Research, India
Submission: June 26, 2017; Published: June 30, 2017
*Corresponding author: Sudip Bhattacharya, Postgraduate Institute of Medical Education and Research, India, Email: drsudip81@gmail.com
How to cite this article: Anil Kumar G, Shweta T, Sudip B, Amarjeet S. Health System Strengthening-Focussing on Referrals: An Analysis from India. JOJ Nurse Health Care. 2017; 2(4): 555592. DOI: 10.19080/JOJNHC.2017.02.555592
Introduction
A referral is a process in which a health worker at a one level of the health system, having insufficient resources (drugs, equipment, skills) to manage a clinical condition, seeks the help of a better or differently resourced facility at the same or higher level to assist in (WHO).
Referral system plays a vital role in management of diseases in any healthcare system. Typically, this system is pyramidal. Primary healthcare centers (PHC) constitute the base, which is large in numbers. Less number of secondary centers are in the middle, and a fewer number of tertiary care centers constitute the top. The PHC offer the minimum levels of essential tests and all basic treatments on an outpatient care basis, the secondary level centers are able to offer most of the diagnostic tests and management facilities, including hospitalization, interventional procedures, surgery, and rehabilitation programs. Tertiary level centers usually restricted for complex interventions and surgical procedures, prescription of high end costly tests. Secondary and tertiary level centers are also important for appropriate for training programs to strengthen our health care workforce [1].
Common reasons for referral (either an emergency or routine cases) are:
- For taking expert opinion for the patient.
- For seeking additional services for the patient.
- For seeking better treatment of the patient.
- For using of high end diagnostic and therapeutic tools, which is not available at current level.
An active referral system ensures a handy relationship between every levels of health care delivery system i.e. primary, secondary and tertiary health care. It also ensures public to receive the optimal utilization of health care which is adjacent to their residence [2].
One of the major aim of referral system is to make cost- effective utilization of health care. Hence it ensures better quality care in all levels if, it is functioning properly [1].
A good referral system should have following characteristics
- Patients should be given optimal care at the right level, right time and right cost.
- Optimal and cost-efficient utilization of health care systems.
- Optimal and appropriate utilization of specialist services for needy persons.
- Optimal utilization of primary health care services.
Referral System in Developed Countries
In developed countries (e.g. United Kingdom) a certain number of people used to register under a General Practitioner (GP). Say, service of 1000 populations are catered by one GP. So in case any urgency or emergency they have to go to the GP first, if he/she thinks that the patient needs referral, only then he can go to the higher level facility. So there is a systemic pathway of referral which have to follow by all [3].
An innovative referral system is developed by Canterbury Health Services in New Zealand in 2008. They called it “health pathways.” This change was very much appreciated to their health care system. These were basically consensus statements on a written standard protocols whereby doctors and health workers have collectively planned “patient pathways” and “treatment protocols.” It is managed by the community. It integrates guidelines on referrals and existing resources for doctors, to avoid unnecessary referrals. Simultaneously they also perform proper investigations to be performed before making a referral(4). Resources are always limited as compared to the increasing needs and demands of the mankind, so innovation is the only way to provide the optimal services to the target population. Some countries have already tried innovations to reduce the burden of referred patients.
Innovations in Referral System
Example 1
We can take an example of Chronic Obstructive Pulmonary Disease (COPD). From referral data analysis in Canterbury, New Zealand it was found that most common cause of hospitalization among aged was COPD. Later specific programme for COPD was introduced. Patients are given treatment protocols in this programme. Simple incorporated devices are used such as a fridge magnet by which they can assess their normal oxygen saturation and exercise tolerance on it. It permitted the paramedics working in ambulance service to know the 'normal' oxygen saturation ranges for the patient. Additionally, it was supported by tele calling to a pulmonologist. It was evident from the case study that a paramedic can play a role of decision maker for that patient's referral needs, by passing the overburdened doctors. Thus innovative empowerment programme worked well in Canterbury. A winter data of 2012, Canterbury estimated that nearly 40 per cent of COPD patients were side-tracked to the other centres, who would previously have been taken to the emergency department [4].
Example 2
Wear National Health Scheme Foundation Trust (WNHSFT) instigated an evaluation response team for mental health patients. It provided a helpline via 24X7 to the patients. This service provided Nurses triage through telephone consultation. The nurse advised to the patients with their current medical problems and it allowed transfer into other services. Thus optimal utilization of health care resources were obtained. GPs also felt more comfortable in managing mental health patients [5].
The evaluation response team for mental health patients resulted in
- Rapid response for referral, as they applied the policy of "face to face triage."
- Undertaking home visits quickly (usually within one hour)
- Referral to General Practitioner services
- Referral to existing Crisis Resolution
- Simply providing telephone advice
Staff used to meet regularly to discuss patient referrals. It enabled aversion to the large proportion of urgent referrals to be taken into the most suitable OPDs. Hence reduction load on existing referral system, or they proceed with an agreed management plan [5]. These are the examples of referral systems in advance countries.
Referral Systems in India
Indian health care system is plagued by overpopulation, lack of expert clinicians, lack of motivation among existing health work force like Nurses, Laboratory technicians and a following an effective referral mechanism. Though there is a provision for referral of patients from lower to higher level health facilities according to the seriousness, need of the patients and also availability of the resources and vice versa. (Figure 1).
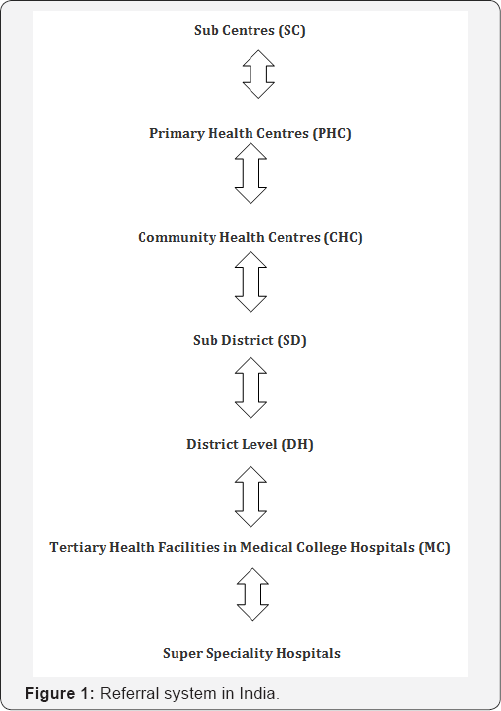
Unfortunately, a different scenario is observed at ground level. It is opposite to the principle mentioned above. In India any one (patients) can go to anywhere, irrespective of level of existing architectural hierarchy in health care system without any referral. It exerts a huge burden burden on the higher level facilities. Usually it is seen that large number of patients with minor illnesses flock around the Out Patient Departments (OPDs). Ideally these patients can be easily tacked at the lower level health facility.
A study shows that more than 50% morbidity could have been seen at the PHC level. Unfortunately, they consume resources of a higher level health facility, which can be effectively utilized for the serious ones [6].
Why Implementing a Successful Referral System in India is Difficult?
Multiple studies have documented the root causes of failure in referral systems in India.
These are:
- Lack of skilled and motivated manpower, especially in secondary level.
- Inadequate infrastructure in the PHCs.
- Non adherence on the referral system guidelines.
- Lack of accountability in each level for controlling of unnecessary referrals.
- Lack of back referral of minor cases coming directly to higher level.
- Non-availability of universal health card like in developed countries where the health facility for primary treatment or screening is indicated for a particular population.
Way Forward
It is not a very task. There is a huge disparity in health care spending in India unlike developed countries. India spends very little on health budget compared to the western countries. In India there is also a set protocol for referral, but nobody follows. There also reasons behind it. After 50 years of independence, government has failed to provide basic health care services round the clock to the door steps of a common people [7]. The common problems have already discussed above. Those problems should be addressed on priority basis. Innovations, like demarcations of using a particular health facility by a particular people on the basis on Aadhar card address can be an option [8]. Making a strict instruction, e.g., only those seen in the labelled health facilities would be considered for health services once referred.
It will lessen the load in the higher facilities. Hence the health care providers can allot their precious time and energy by serving needy patients with maintaining the quality.
Conclusion
In conclusion we can say that strengthening primary care with adhering to strict regulations and innovations are necessary for improvement in existing referral systems in India.
References
- Jindal SK. Promotion of Standard Treatment Guidelines and Building Referral System for Management of Common Noncommunicable Diseases in India. Indian J Community Med. 2011 Dec 1;36(5):38.
- Types of Healthcare [Internet]. TrioTree Technologies Pvt Ltd. [cited 2017 Jun 30]. Available from: http://triotree.com/blog/healthcare- primary-secondary-and-tertiary-brief-description/types-of- healthcare/
- Choices NHS. GP referrals - The NHS in England - NHS Choices [Internet]. 2017 [cited 2017 Jun 30]. Available from: http://www.nhs. uk/NHSEngland/AboutNHSservices/doctors/Pages/gp-referrals.aspx
- Timmins N, Ham C. The quest for integrated health and social care: a case study in Canterbury, New Zealand [Internet]. Kings Fund; 2013 [cited 2017 Jun 30]. Available from: https://www.hqsc.govt.nz/assets/ General-NEMR-files-images-/kings-fund-CDHB-Sept-2013.pdf
- Campbell JL, Fletcher E, Britten N, Green C, Holt T, Lattimer V, et al. The clinical effectiveness and cost-effectiveness of telephone triage for managing same-day consultation requests in general practice: a cluster randomised controlled trial comparing general practitioner- led and nurse-led management systems with usual care (the ESTEEM trial). NIHR Journals Library; 2015.
- Potharaju HR, Kabra SG. Prescription audit of outpatient attendees of secondary level government hospitals in Maharashtra. Indian J Pharmacol. 2011 Mar 1;43(2):150.
- Bhattacharya S, Singh A. Why tuberculosis control programmes fail? Role of microlevel and macrolevel factors: an analysis from India. BMJ Case Rep. 2017 Apr 21;2017:bcr-2017-219606.
- UIDAI - Official Website [Internet]. [cited 2017 Jun 30]. Available from: https://uidai.gov.in/






























