A Series of Clinical Cases of Psychocutaneous Disorders in a Dermatology Unit in Albania
Migena V1, Petrit V2, Sabina D1* and Ermira V1
1Department of Dermatology, University Hospital Center “Mother Teresa”, Tirana, Albania
2Department of Emergency, University Hospital Center “Mother Teresa”, Tirana, Albania
Submission: April 03, 2023;Published: April 18, 2023
*Corresponding author: Sabina D, Department of Dermatology, University Hospital Center “Mother Teresa”, Tirana, Albania
How to cite this article: Migena V, Petrit V, Sabina D, Ermira V. A Series of Clinical Cases of Psychocutaneous Disorders in a Dermatology Unit in Albania. JOJ Dermatol & Cosmet. 2023; 5(3): 555664. DOI: 10.19080/JOJDC.2023.05.555664
Abstract
This study aims to represent our clinical experience with several psychocutaneous disorders, such as trichotillomania, neurotic excoriation, dermatitis artefacta, and parasitic delusion. Lightening the human mind’s way of function has always been a challenge and has attracted medical interest through the years. Psychodermatology has recently received attention because different mechanisms of psychoneuroimmunology are being explored. They can successfully explain different clinical presentations and drug therapy. Awareness, recognizing important risk factors (suicide, serious self-harm, other people harm, child abuse, and neglect), associated psychiatric diagnoses, adequate screening, seeking a specialized referral, and reasonable security measures should be on focus. The proper management needs a multidisciplinary team, including the dermatologist, the psychiatrist, the family physician, and the social support.
Keywords: Psychodermatology; Primary psychodermatological disorders; Psychocutaneous disorders; Self-induced lesions; Multidisciplinary team, Management
Introduction
Psychodermatology involves the interaction of the mind and skin. Skin and psyche are related to their common embryonic origin of being both ectodermal [1]. New evidence in psychoneuroimmunology suggests that skin and the psyche are affected by immunological regulation and endocrine changes [2]. As the prevalence of psychiatric disorder in dermatological outpatients is estimated at 30-40%, dermatologists often have to diagnose and treat comorbid psychiatric disorders [3]. In a study conducted two years ago in our country, dermatologists had significant knowledge gaps in adequately understanding and treating psychocutaneous disorders [4]. Since then, considerable effort has been made to better approach these peculiar patients in our clinic. Here we represent seven cases of psychocutaneous disorders.
Case Reports
The study includes seven patients who firstly sought a medical appointment with a dermatologist. A clinical description was made for each patient, followed by a psychiatric consultation.
Results
Case 1
Patient Xh. F, male, 73 years old, presents at the dermatology clinic accompanied by his daughter with complaints of the presence of numerous wounds on the body and head that were accompanied by the sensation of pain, burning, and uncontrolled itching. These problems had started 1.5 years ago, a period that coincided with the diagnosis of his wife with malignant diseases, according to the daughter. After her death, these elements had been increasing. The patient lived lonely. On dermatological examination, ulcers were observed on the head, extremities, and trunk. The ulcers were round to oval, with sharp edges, a clean base, surrounded by erythematous skin, irregularly distributed, and atypical (Figure 1). Also on the skin were excoriations, scars, and post-inflammatory hyperpigmentation (Figure 2). During hospitalization, he underwent laboratory and imaging examinations that were normal: a bacteriological examination of ulcerations showed the presence of E. coli. To rule out other causes of cutaneous ulcers, the histopathological response did not indicate any specific dermatosis. During the consultation with the psychiatrist, he complained of insomnia (3-4 hours of total sleep), stable mood present, mood-compatible affect, coherence in conversation, and time-oriented and self-oriented; a detailed anamnesis revealed that he had caused these elements by using matches. He partially accepted the truth after the psychiatrist’s perseverance. He started treatment with Escitalopram 20mg, Lorazepam 2.5mg ½ tab at dinner, and with an antibacterial and repairing agent, topically.
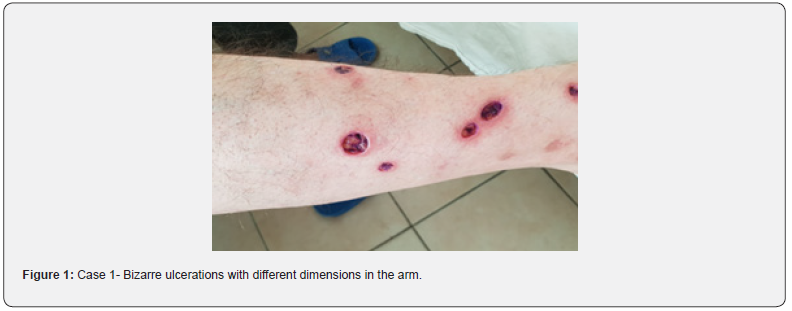
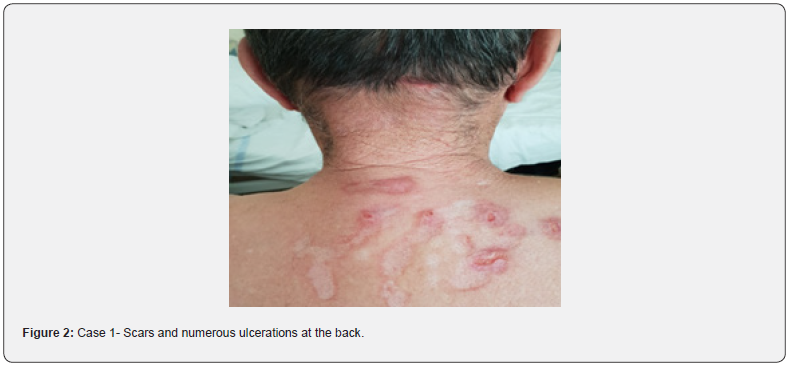
Case 2
Patient Z.E, female, 68 years old, is presented in the dermatology clinic with pruritus spread on the head, face, and body, insomnia for 5-6 months. She points out that these troubles started after an insect bite in the area of her right eyebrow, which now gives her the feeling of straw, and she sees living creatures like beetles dancing from face to head, neck, and body, watching them fall dead. The concomitant disease was hypertension, cardiac arrhythmia, and varicose veins, for which he received medication. On objective examination in the superior dexter region palpebralis, only 2-3 erythematous papules with slight squamous on the surface were observed (Figure 3). Examinations turned out to be normal, and in consultation with the psychiatrist, it was suggested that the complaints expressed about pruritus and the manner of their spread and their origin; body burns, and fluctuating temperatures which she failed to measure with a thermometer; disruption of quality of life and compromising the duration and schedule of sleep lead to a somatization disorder. Therapy was started with Fluvoxamine 100mg 1/2tab in the morning for ten days and then 1tab in continuation, Lorazepam 2.5mg 2x 1/2 tab/day.
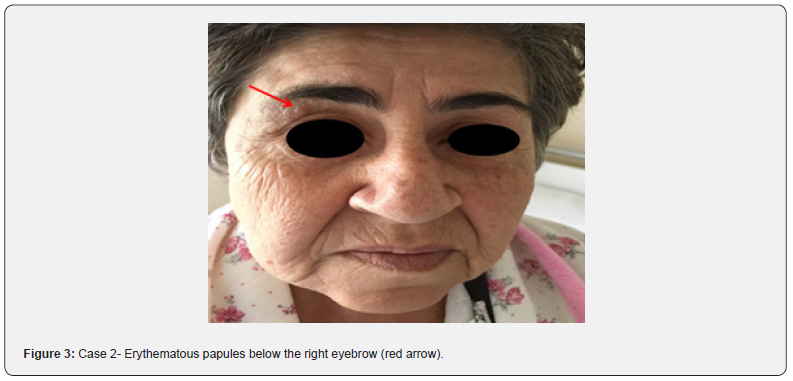
Case 3
Patient F.M, female, 10 years old, is presented in the dermatology clinic with severe pruritus on the body and extremities of 6 months that are more pronounced at night. Refers that there has been a short period in which they have entirely disappeared. During the conversation, there is an intervention of the mother in communication. In the objective examination, there were papulonodular, multiple, bilateral elements in the superior and inferior extremities, with discrete distribution, asymmetric dark color, and erosions in the center. Also, there were excoriations and post-inflammatory hyperpigmentation on the face and extremities (Figure 4). Laboratory and imaging examinations and skin biopsy to rule out pityriasis lichenoides chronica and papulosis lymphomatoide resulted not indicative. After consultation and examination of mental status, the psychiatrist identified symptoms of anxiety and symptomatic compulsions associated with increased concern for germs or diseases (approaching mosquitoes and animals caused her anxiety). To avoid this, she scratched the skin with frequent body washes). The history of the disease identifies an obsessive style tendency in doing everyday things. The psychiatrist recommends starting therapy for a short time: Phenibut 250mg 3x ½ tab/day for four weeks.
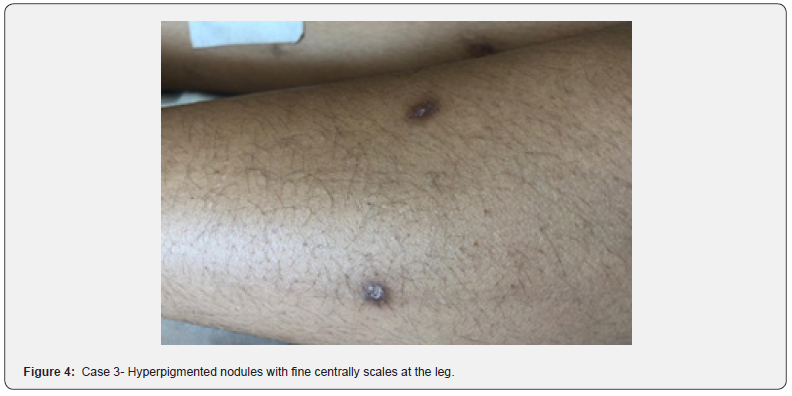
Case 4
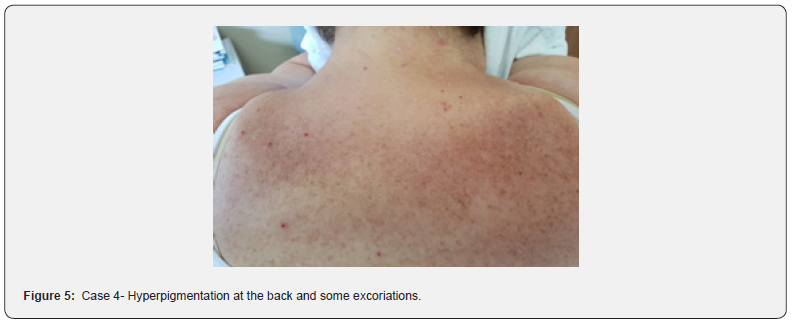
Patient L.C, female, 63 years old, presents at the dermatology clinic with pimples on the chest and arms and severe itching of the head and scalp for a month. Refers to suffering from chronic insomnia. The patient lived alone for six years after her husband’s death. The practice of excessive hygiene characterized her lifestyle. On dermatological examination, reddish-brown papules were observed, eroded on the surface, some with sero-hemorrhagic crusts on the surface, and hyperpigmented skin (Figure 5) The histopathological response was compatible with chronic eczema with pronounced ulceration. He was given local medication and was followed by an outpatient psychiatrist to treat neurotic excoriation.
Case 5
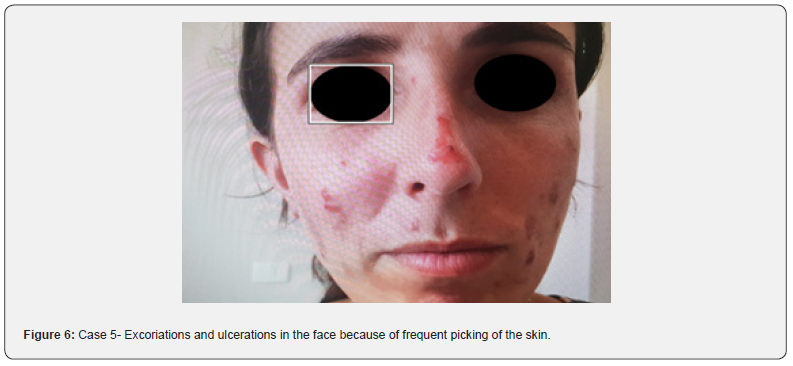
The patient presents to the dermatology clinic with ulcerations localized in exposed areas on the face and accessible parts of the extremities with bizarre shapes and irregular locations (Figure 6). She referred to the presence of parasites in the body, which she tried to get rid of. In consultation with the psychiatrist, it was concluded of parasitic delusion and followed up by the psychiatrist.
Case 6
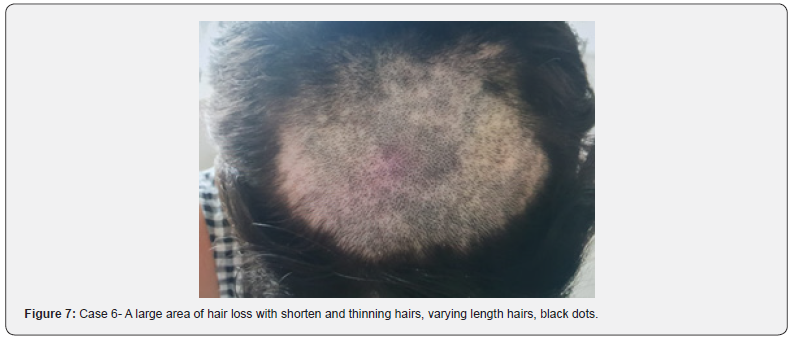
The patient presents to the dermatology clinic with complaints of hair loss and the tuft of fallen hair. She and her mother do not accept it for self-induced reasons. There was no associated itching or burning sensation before hair loss. Locally, normal scalp is noticed, with a large area of hair loss, broken hair, black dots, and hair of varying length in the vertex crani region. (Figure 7) A psychiatrist followed-up the patient for trichotillomania treatment.
Case 7
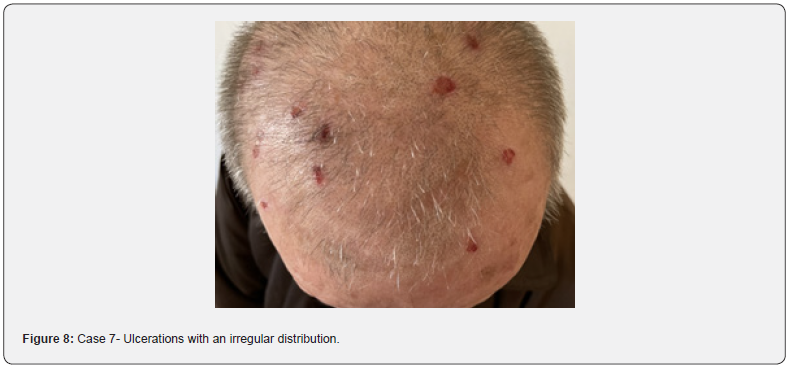
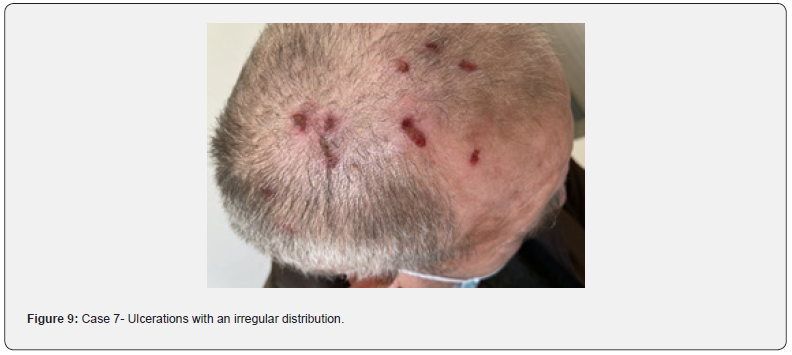
The patient presents to the dermatology clinic with complaints of small wounds on the scalp. It was initially treated with local medications for folliculitis but without improvement (Figure 8,9). During the more detailed anamnesis, the patient showed that he was quite anxious, especially recently, after his wife’s diagnosis of malignant disease. Based on the history and objective examination showing multiple erosions in the scalp and frontal region, some scattered follicular pustules were thought to be self-induced; therefore, in addition to dermatological treatment, consultation with a psychiatrist was suggested to cure the symptoms of stress and expressed anxiety.
Discussion
Psychodermatology is a branch of dermatology that has begun to develop in scientific terms in recent years. Information about these diseases is not constant because psychocutaneous diseases are considered rare. Still, in medical practice, every dermatologist is highly likely to deal with patients with atypical lesions, bizarre forms and distribution, and resistance to collaboration. This guides the dermatologist’s initiative to report his experience and raise awareness. It is firstly necessary to be familiar with the classification of psychocutaneous diseases.
Although there is no universally accepted classification system, the most commonly employed system classifies psychodermatological disorders into five main groups according to the category of skin disorder. They are classified as psychophysiological disorders (refers to a skin disorder that is worsened by emotional stress), primary psychiatric disorders (refers to a skin disorder in which the primary problem is psychologic; the skin manifestations are self-induced), secondary psychiatric disorders (affect patients with significant psychologic problems that have a profoundly negative impact on their selfesteem and body image), cutaneous sensory syndromes (the patient presents with either disagreeable skin sensations (i.e., itching, burning, stinging) or pain (i.e., allodynia) and/or negative sensory symptoms (i.e., numbness, hypoaesthesia)), and use of psychotropic medications in dermatology [2-4]. Here, we present essential information about the psychocutaneous disorders we faced in the above clinical cases.
Trichotillomania is an obsessive-compulsive disorder– related condition characterized by repetitive hair pulling, causing hair loss. Currently, it is classified under obsessive-compulsive spectrum disorder by DSM-5. Various hypothetical models have been used, including the psychoanalytical, biological, and behavioral models. This disorder is seen in early childhood or adolescence, predominantly in females. The most common sites of hair pulling include the scalp, eyelashes, eyebrows, pubic hair, body hair, and facial hair. The dominant hand is used in most cases, so hair loss usually occurs on the contralateral side of the body. The pattern of hair loss is often bizarre, with angular or irregular borders containing hairs of varying lengths. It may be confused with alopecia areata, tinea capitis, traction alopecia, androgenetic alopecia, monilethrix, pili torti, loose anagen syndrome, and various secondary causes of alopecia such as syphilis, lupus erythematosus, lymphoma, and various endocrinopathies [2]. Diagnosis is primarily clinical, but scalp biopsy can be done in ambiguous cases [5]. Habit reversal therapy reduces receptive unwanted behaviors by bringing them to conscious awareness and replacing them with alternative behaviors that are not bothersome or interfere with the overall quality of life-combined with pharmacological treatment, has been used successfully. Selective serotonin reuptake inhibitors, selective norepinephrine reuptake inhibitors, and N-acetylcysteine are used in treating trichotillomania [6].
Dermatitis artefacta is currently classified in somatic symptoms and related disorders in the DSM-5. Patients with factitious disorder present with various symptoms of disease processes that are intentionally produced to assume the role of a sick person. The symptoms are caused voluntarily and consciously with no intention of secondary gain. Recent studies suggest the prevalence in dermatology clinics is between 0.04% and 1.5%. Warning signs for factitious disorders are female sex, healthcare training, multiple emergency room visits, hospitalizations, doctor shopping, vague symptoms and history, lack of objective findings to support history, suspicious shape and color of the lesions on examination of blood, urine, or sputum cultures that grow unexpected organisms. Several hypotheses are discussed: social learning hypothesis, self-punishment, social signaling, implicit identification hypothesis, pain analgesia or opiate hypothesis, pragmatic hypothesis, and tension-regulation hypothesis. Bizarre crude presentations are easy to diagnose. At times, lesions mimic specific dermatosis, where a skin biopsy must be considered. Dermatitis Artefacta’s histopathology is usually nonspecific but can sometimes provide supportive information [7,8].
Treatment of factitious disorder requires a multidisciplinary team. Psychotherapy is the first-line treatment. Selective serotonin reuptake inhibitors, antipsychotics, mood stabilizers, and antianxiety agents have been used with variable success in comorbid psychiatric symptoms.
Patients with Delusional Parasitosis typically present to the dermatologist and report experiencing sensations of parasites crawling inside or on their skin Hebbar et al. [2] found it the most common subtype of delusional disorders [9]. Patients commonly bring samples of the bugs, typically pieces of their hair or skin, referred to as “matchbox” or “specimen sign.” In the primary form, the delusion is self-manifested; in the secondary form, the delusion is secondary to substance abuse, nutritional deficiencies, and another medical condition or psychiatric illness. Diagnosing and treating patients with delusion of parasitosis is always challenging for dermatologists and psychiatrists alike. Careful history-taking is vital in elucidating the underlying causes of patients with the secondary form of the disorder [10].
Skin-Picking Disorder is also known as excoriation disorder, psychogenic excoriation, and dermatillomania. Most commonly seen in adolescence and middle adulthood. The condition is characterized by physical damage to the skin from excessive and repetitive touching, pulling, squeezing, pinching, and/or rubbing. The lesions are mostly seen in areas that the dominant hand can reach. The lesions are visible in different stages of healing and may have delayed healing due to the chronic nature of the condition. The lesions are commonly hypo- or hyperpigmented and appear as linear scabs or scars. Psychiatric comorbidity is common and includes depression, anxiety, substance abuse, and in severe cases, suicidal ideations. Both psychotherapy and pharmacologic (SSRIs, antipsychotics, opioid antagonists, and glutamate modulators) treatment are effective in the successful management of patients.
Some clinical considerations and characteristics of the patients involved in the study, as well as the relationship with the dermatologist and psychiatrist, are presented below:
• These patients had their first medical approach with the dermatologist, and specialized treatment from the tertiary center was requested on average after 2-3 follow-up sessions by the district dermatologists.
• Such an evolution of the course of the disease is observed: Consultation with different doctors for many years, difficulty making a diagnosis by doctors, the belief that doctors are incompetent, ineffective treatment, and treatment is interrupted (vicious circle).
• The coexistence of psychic and cutaneous touch should serve as an alarm signal not only because of the risks posed by this category of vulnerable patients but also the costs of long-term misdiagnosis: biopsies, microbiological examinations, blood tests, consultations, opinions, hospitalizations and medications which are administered before the final diagnosis are very expensive.
The most common differential diagnoses for primary psychiatric disorders include Prurigo nodularis, Eczema chronicum, Contact dermatitis, bacterial infections, alopecia areata, etc.
• The morphology of cutaneous elements is diverse, and the type, level of gravity, distribution, and tolerance to treatment depend on the psychosocial level of the patient.
• It is also necessary to build a reliable relationship with the patient’s family to obtain the necessary medical information about the origin of the concerns and the causes and to guarantee the continuation of therapy.
• Dermatological treatment does not require being aggressive, prioritizing correcting primary psychiatric disorders.
A supportive approach avoiding condemnation is always preferable. The dermatologist should be prepared for a prolonged treatment with repeated relapses and never express disappointment or hostility over these failures. The treatment of factitious disease is often unsatisfactory, whether a dermatologist, a psychiatrist, or both manage it.10 Most patients with psychocutaneous disorders can be broadly categorized under four diagnoses: anxiety, depression, psychosis, and obsessivecompulsive disorder. The choice of psychotropic medication is based primarily on the nature of the underlying psychopathology. The initial and most important step in successfully managing these patients is establishing rapport. It is necessary to start both dermatologic and psychotropic treatment simultaneously. Management includes standard psychotropic drugs, placebo effect, suggestion, cognitive-behavioral methods, biofeedback, and hypnosis. Whenever simple measures fail to produce the desired results, a combination of drugs or the addition of nonpharmacological therapy may be required. In all our cases the patient management has started with medicamentous treatment prescribed by the psychiatrist to have faster clinical improvement.
Conclusion
Enriching our knowledge related to the psychodermatology medical branch is very important. Our aim was not only to present some clinical cases of some psychocutaneous disorders but to learn more by exchanging our practical experience in dealing with such complex patients and not underestimating their complaints. Sometimes, cutaneous manifestations are the first call for help from a patient who may seem very calm. This prompts the dermatologist to be the first who raise the alarm and properly manage complex cases. Patients with psychocutaneous problems are similar and different in the stories they bring. Therefore, the relationship with them should not recognize boundaries. Proper management requires information from the dermatologist in the diagnostical and therapeutical approach, including the psychiatrist, to improve the patient’s quality of life in these scenarios.
References
- Jafferany M, Jorgaqi E (2020) Psychodermatology in Balkans: Knowledge, awareness, and practice patterns of dermatologists in Albania. Dermatologic Therapy e13286.
- Jafferany M (2002) Handbook of Psychodermatology.
- Bewley A (ed.), Psychodermatology in Clinical Practice.
- Koo J, Lebwohl A (2001) Psycho Dermatology: the mind and skin connection. Am Fam Physician 64(11): 1873-1878.
- Gupta MA, Gupta AK (2013) Cutaneous sensory disorder. Semin Cutan Med Surg 32(2): 110-118.
- Muller SA (1990) Trichotillomania: A histopathologic study in sixty six patients. J Am Acad Dermatol 23: 56-62.
- Yadav S, Narang T, Kumaran MS (2013) Psychodermatology: A comprehensive review. Indian J Dermatol Venereol Leprol 79: 176-192.
- McSween R, Stevens A, Millard L (1996) Sex, lies and dermatopathology. Br J Dermatol 135: 27.
- Hebbar S, Ahuja N, Chandrasekaran R (1999) High prevalence of delusional parasitosis in an Indian setting. Indian J Psychiatry 41: 136-139.
- Rodríguez Pichardo A, García Bravo B (2013) Dermatitis artefacta: a review. Actas Dermosifiliogr 104: 854-866.






























