Eruptive Guttate Hypomelanosis after SARS-Cov-2 Viral Vector Vaccine
Ferrari T1,2, Zengarini C1,2*, Venturoli S2,3, Mussi M1,2, Lazzaroto T3 and Dika E1,2
1Dermatology Unit, IRCCS of Azienda Ospedaliero-Universitaria di Bologna, Italy
2Dermatology Unit, Department of Experimental, Diagnostic and Specialty Medicine, University of Bologna, Italy
3Microbiology Unit, Department of Experimental, Diagnostic and Specialty Medicine, University of Bologna, Italy
Submission: October 15, 2022;Published: October 27, 2022
*Corresponding author: Zengarini C, Dermatology Unit, Department of Experimental, Diagnostic and Specialty Medicine, IRCCS of Azienda Ospedaliero-Universitaria di Bologna, Bologna, Italy
How to cite this article: Ferrari T, Zengarini C, Venturoli S, Mussi M, Lazzaroto T, et al. Eruptive Guttate Hypomelanosis after SARS-Cov-2 Viral Vector Vaccine. JOJ Dermatol & Cosmet. 2022; 4(5): 555650. DOI: 10.19080/JOJDC.2022.04.555650
Keywords:Guttate; Hypomelanosis; SARS-CoV-2; Autoimmune; Astrazeneca; COVID-19; Adverse drug reaction; ADRs; Vaccine
Case Report
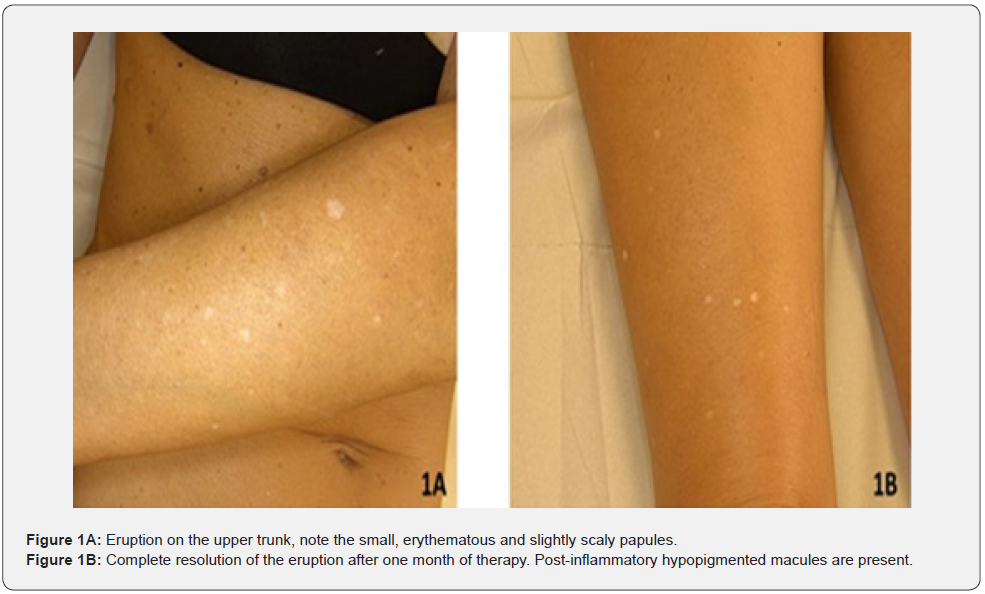
A 53-year-old female accessed our dermatological unit after the onset of whitish macules eruption on the abdomen, legs and arms. The patient was otherwise healthy and did not refer chronic drug intake. Clinical signs started one week after receiving the SARS-CoV-2 Adenoviral vector Vaxzevria (Astrazeneca) vaccine. She referred no significant symptoms after vaccination, except two days of fever and some sore throat. The patient did not assume any other medications in the past two months nor changed her habits in the last year. At the time of our consultation, we observed more than one hundred oval, porcelain white flat macules of 2 to 6 mm of diameter on the trunk, limbs, and back with well-demarcated borders (Figure 1A). A fine scale-covered most of the lesions. The face was spared, and the lesions were more evident on sun-exposed skin. Infective and inflammatory conditions causing skin depigmentation were considered in the differential diagnoses encompassing, macular hypomelanosis, vitiligo, pityriasis Versicolor, tuberous sclerosis, lichen sclerosus et atrophicus, guttate morphea, post-inflammatory hypopigmentation and guttate hypomelanosis.
The latter represents a type of hypomelanosis typically observed in elder, fair-skinned women [1]. The distribution of the macules and an examination for fungal ifae readily ruled out pityriasis Versicolor. On a clinical base, macular hypomelanosis does not present with a well-demarcated border. Post- inflammatory hypopigmentation was also excluded because of the lack of a previous history of dermatitis. The sudden eruption described after the COVID-19 vaccination and the patient’s query addressing the cause of the immunisation made further tests necessary. On histopathologic examination, a skin biopsy showed epithelial atrophy, a patchy absence of melanocytes and melanin, flattening of the net pegs, and basket woven hyperkeratosis. Since the eruption of hypopigmented macules has been associated with several viral infections [2], we delivered a skin sample to our microbiology department to test for HPV and herpes virus strains. All skin tests resulted negative to PCR tests. We then concluded with the diagnosis of guttate hypomelanosis triggered by the SARS-CoV-2 Adenoviral vector Vaxevria (AstraZeneca). Hypopigmented macules in adult patients without clear pathogenesis have been called “idiopathic guttate hypomelanosis” or “lenticular leukoderma”. Amoeboid, feathery, petaloid and nebuloid patterns of dermoscopic presentation have been described in these skin manifestations. Macules usually become uniform upon time, less visible in fair-skinned women with no tan and more definite during the summer season. The pathogenesis of guttate hypomelanosis is still to be determined. Chronic sun exposure and senile degeneration are thought to represent essential causative factors, together with repetitive traumatisms of the skin caused by epilation and somatic genetic alterations in predisposed patients. An association with autoimmunity impairment has been proposed.
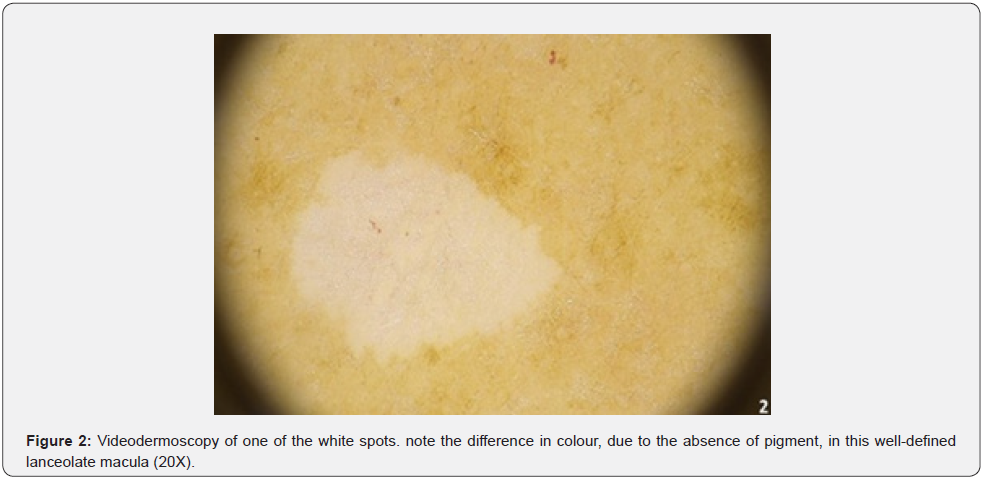
However, no correlation of increased prevalence of autoimmune diseases in idiopathic guttate melanosis patients or their relatives has been demonstrated in previous studies. Our patient presented fair skin (phototype II, Fitzpatrick scale) and signs of actinic damage on clinical examination, such as the presence of numerous solar lentigo on the face and the dorsum. Dermoscopy showed a petaloid pattern of the macules with well-defined petallike borders (Figure 1B). We believe that the inflammatory status elicited by the vaccine [3] could have quickened the damage progression of already impaired melanocytes, accelerating the development of hypomelanotic macules (Figure 2).
The description of skin reactions in the course of Covid-19 infections is being widely reported, as well as vaccine related or skin transient manifestations due to protective devices or hygiene measures [4-5]. Most of the manifestations are transient and not life threatening. A better understanding of the skin manifestations, even if not linked to severe symptoms but in any case, sometimes widespread and visible, is useful for reducing anxiety in patients facing the difficult pandemic period.
References
- Ankad BS, Beergouder SL (2015) Dermoscopic evaluation of idiopathic guttate hypomelanosis: A preliminary observation. Indian Dermatol Online J 6(3): 164-167.
- Zawar V, Bharatia P, Chuh A (2014) Eruptive hypomelanosis: a novel exanthem associated with viral symptoms in children. JAMA Dermatol 150(11): 1197-1201.
- Bataille V, Puig S (2022) COVID-19 vaccines and skin manifestations. Br J Dermatol 186(1): 15.
- Bardazzi F, Savoia F, Dika E, Tabanelli M, Giacomini F (2007) Acquired aquagenic keratoderma. Pediatr Dermatol 24(2): 197-198.
- Jeyanathan M, Afkhami S, Smaill F, Miller MS, Lichty BD, et al. (2020) Immunological considerations for COVID-19 vaccine strategies. Nat Rev Immunol 20(10): 615-632.






























