Fat Tissue Grafting in Scleroderma Complications Treatment: Experience of a Single Centre
Faggioli Paola1, Falaschi Monica2, Mazzone Antonino1, Selmi C3, De Santis M3,Beretta L4, Vigone B4, Epis OM5 and Ughi N5
1Department of Internal Medicine and Rheumatology, ASST Ovest Mi Legnano, Italy
2Deparment of Plastic and Reconstructive Surgery, ASST Ovest Mi Legnano, Italy
3Rheumatology and Immunology Unit IRCCS Humanitas Univeristy Rozzano, Italy
4Immunology Unit University of medicine 1th Milan, Italy
5Rehumatology Unit Niguarda Hospital Milan, Italy
Submission: October 05, 2022;Published: October 17, 2022
*Corresponding author: Paola Faggioli, Department of Internal Medicine and Rheumatology, ASST Ovest Mi Legnano, Italy
How to cite this article: Paola F, Monica F, Antonino M. Fat Tissue Grafting in Scleroderma Complications Treatment: Experience of a Single Centre. JOJ Dermatol & Cosmet. 2022; 4(5): 555649. DOI: 10.19080/JOJDC.2022.04.555649
Abstract
Objective: Fat Tissue Grafting (FTG) is usually employed in the treatment of fibrotic diseases or sclerotic outcomes. In systemic sclerosis (SSc), patients (pts) gradually develop face and perioral skin thickness which limits mouth function. None of the common therapies is effective.
Methods: we treated 22 pts affected by SSc (20 female, 2 man), median age 47±15y, with a mean 9.4 years (8±4y) of disease. FTG was carried out in accord with modified Colemans’ procedure. Fat was taken mainly from periumbilical areas (only in 2 pts from trochanteric areas) and was injected at 8 points around the lips. No adverse complications were reported. At baseline, 6 and 12 months, we tested mouth opening by measuring interincisal distance, oral functionality by MHISS scale and a patient satisfaction questionnaire was administered. Two pts repeated FTG after 12 months.
Results: an 11 mm (8-18mm range) median increase of interincisal distance was reported at 6 months and in 80% of pts at 12 months (p<0.03). A significant improvement in MHIS scale was also observed (p<003). The patient satisfaction questionnaire showed 95% positive results and 80% of the patient replied affirmatively to the question about the repetition of FTG.
Conclusion: In SSc pts perioral FTG can be a valid therapeutic option to improve mouth function, perioral thickness and esthetic appearance.
Abbreviations: FTG: Fat Tissue Grafting; SSc: Systemic Sclerosis; MRSS: Modified Rod Mnan Skin Score
Keywords:Fat graft Systemic Sclerosis
Introduction
Systemic sclerosis (SSc) is a chronic disease, whose etiology has not yet been clarified. Its pathogenetic aspects are the activation of the immune system by autoantibodies production and the involvement of microcirculation, characterized by ischemia and vasoconstriction, followed by endothelial cellular activation which leads to a proliferative fibrotic vascular lumen evolution and subsequent deposition in the skin and internal organs of the extracellular matrix [1]. Many advances have been recently made in the knowledge of this disease and new therapies had been proposed, which have certainly brought to an increase of the survival and quality of life.
Nevertheless, none therapy has been shown to be able to effectively arrest the fibrotic evolution [2]. Recently, adipose tissue has been identified as a tissue rich in mesenchymal-like stem cells, totipotent cells that can differentiate into endothelial cells and hematopoietic precursors with properties of angiogenic, immunomodulatory and repairing tissues activities in according to tissue graft injected [3].
Studies related to their use in scleroderma are relatively few, only on small groups of patients, but the results are encouraging, mainly for the treatment of lesions of the face and digital ulcers unresponsive to conventional treatment [4-6].
Materials and Methods
We treated with perioral FTG 22 pts (20 F, 2 M) affected by SSc (according to American Rheumatism Association diagnostic criteria) and with diffuse cutaneous SSc. The median age was 47±15y with a mean 9.4 years (8±4y) of disease. Autoantibodies research was positive for Scl70 in 14 pts (13F/1M) and for the centromeric pattern in 6 pts (5F+1M). All the patients had a high Modified Rod Mnan Skin Score (MRSS) with thickening of the perioral skin (score 3 in the perioral skin, score 2 in zygomatic and chin areas) and micrognathia. FTG was indicated when there were difficulties with chewing, swallowing and opening the oral fissure (interincisal distance <40 mm) or the patient had malnutrition with recent weight loss, disabling Sicca Syndrome, need for dental treatment. All the pts were treated with monthly Iloprost infusions, and immunosuppressive therapies (including Mycophenolate Mofetil, Azathioprine, Methylprednisolone). All the pts gave a written informed consent and the procedure was conducted in according to National Health Service (NHS).
FTG procedure
The FTG was performed in according to modified Colemans’ technique [7] in the operating room with thermal protection and under mild sedation (midazolam 2.5-3.5 mg iv). Local anesthesia was carried out at donor site (14 pts at periumbilical region and 2 pts at trochanteric areas). The anesthetic solution (modified Klein’s solution) consisted of 100 ml of saline solution, 20 mL of mepivacaine 2% (AIC, Monico SPA, Venice, Italy), and 5 ml of sodium bicarbonate in solution with 1mEq / ml epinephrine (SALF pharmacological Laboratory SpA, Bergamo, Italy).Three or five subcutaneous injections were performed, then after small incisions, the adipose tissue was taken with cannulae for suction connected with a Luer-lock syringe of 10 ml under vacuum, using radial movements in the subcutaneous tissue (Top face Asp aesthetic set The Talaudiere- France). The incisions were sutured with absorbable stitches (Vicryl Rapid Ethicon Surgery™, Johnson & Johnson Company) and to avoid bruising or hematomas, a compression bandaging (Tensoplast BSN Medical, Germany More polyurethan Mepilex Molnlycke Health Care foam) was put on the donor area and left for 5 days. The adipose tissue was sterilely centrifuged at 1000 rpm x 3 minutes (Hettic EBA 21 Italia Srl Italy), and then the filtrate was centrifuged, placed in syringes of 1 ml under vacuum connected to a blunt cannula for inoculation by 20 G (Top Face Asp Aesthetic - The Talaudiere- France). After the same local anesthesia previously described, the injection of adipose tissue was performed at 6 points around the perioral area and 2 points near to the commissure. For the injection sites, we used the same absorbable sutures and a simple medication. Amoxicillin or Levofloxacin was prescribed for 4-5 days. The hospitalization lasted few hours for observation and, if there were no complications, the discharge occurred the same day. Two pts received fat injection also in zygomatic zone was observed a muscular atrophy.
Clinimetric parameters concerning the oral functions were performed by MHISS scale [8], without evaluating xerostomia by sugar or saliva tests. The opening of the oral fissure was assessed by means of a caliper before and after the intervention, using as a landmark the distance between the incisors upper and lower arch and subsequently we performed a photographic control with digital reassessing of the parameters.
The global health degree was evaluated by the scale Global Health (GH) graduated from 0 to 100. The parameters were measured at baseline and during the follow-up every 3 months for 1 year. The patients were administered a questionnaire, using an adapted Likert scale, about their oral functions at baseline and at follow-up and about their grade of satisfaction for the procedure. There was also a question about their will to repeat the operation if necessary.
Due to the small sample, a true statistical analysis was not carried out, even if a correlation trend was found using a test for paired data (Student T-test and Wilcoxon test for paired data) (SPSS for windows).
Results
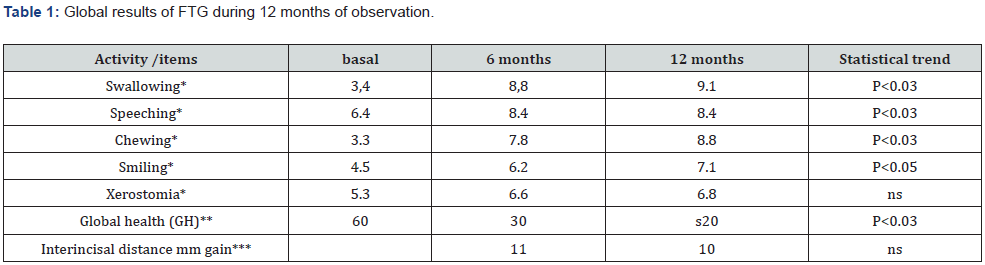
* median of numeric scale 0 worse 10 better
** GH visuoanalogic scale 0 better 100 worse
* measured by caliper and photographic control
Results were assessed on self-reporting from baseline, together with measurements of the opening of the oral fissure at 6 and 12 months from FTG. On average, there was a substantial improvement in speech, chewing, swallowing, smile that was conserved steadily over time with a significant trend statistical correlation (p<003). No improvement was found on xerostomia.
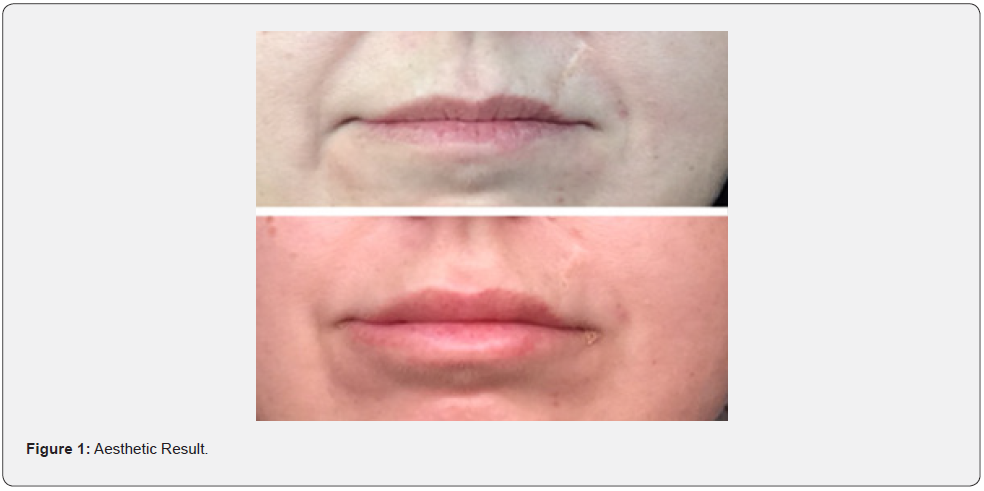
The opening of the oral fissure was measured at baseline, 6 and 12 months. The median increase of the interincisal distance was 11 mm (8- 18 mm range) at 6 months, without a significant difference at 12 months. After the procedure, there was a modest decrease in the MRSS in the perioral area from a score of 3 to a score of 1-2. The patient satisfaction questionnaire showed 95% positive results (excellent or good) without no sufficient or insufficient answers. 80% of the patients replied affirmatively to the question about the repetition of FTG. 70% gained 4-5 kg at 6 months, without variation at 12 months. 60% had the possibility to begin dental care (Figures 1 & 2) (Table 1).
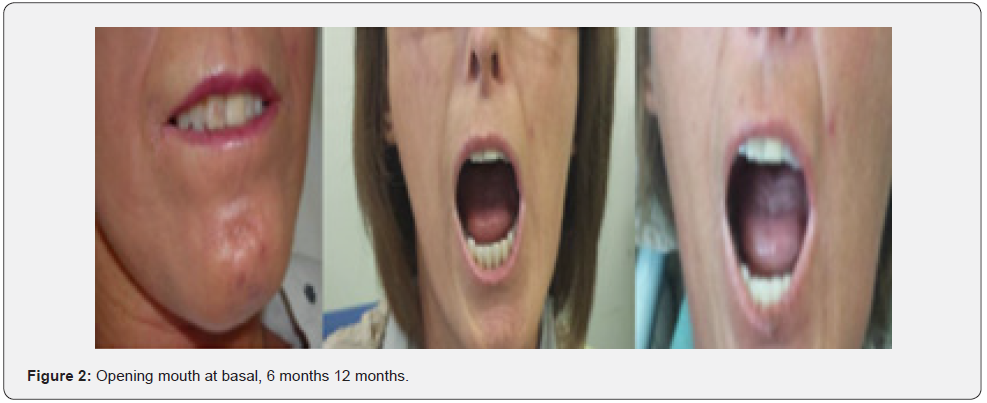
Conclusion
In our paper, we reported preliminary results about FTG for the treatment of fibrosing disease such as scleroderma, in according to initial results of the use of FTG in other diseases: post-irradiation therapy [9], irradiated breast [10] and systemic sclerosis [11].
So far, the treatment of scleroderma microstomia was based on a bilateral surgical commissurotomy of the lip, with questionable and often aesthetically invalid results. The association of physiotherapy or stretching programs could lead to some benefit [12].
Some Authors [5] have suggested that adipose tissue rich in totipotent mesenchymal cells may have conceptually similar results to the treatment with autologous stem cells, albeit at localized and not systemic level, although it is not currently possible to assume these are interchangeable techniques. From our results, it could be concluded that the efficacy of FTG can not only be attributed to the effect of filling, which is known to have a short duration, but rather to the activation of various biological mechanisms that could cause the observed morphological changes [13]. The fact that the elasticity parameters worsen in some series in the first month (probably for the filling effect related to volume expansion) but improve after three months could be explained according to the activation of cellular cytokine pathway by adipocytes and mesenchymal cells contained in the fat that would express their regenerative potential. Therefore, hypoxia present at tissue level in scleroderma patients might be one of these stimuli and may explain the activation of adipocytes and the production of anti-inflammatory cytokines and cell growth factors that may be responsible for the clinical response to FTG in this pathology [14].
The long-term effects of this type of treatment are currently unknown. However, some preliminary data at 12 months followup seems to confirm the benefits in the long term, despite the filling effect is over [15-16].
There are some limits to FGT treatment: the lack of Plastic Surgery Departments able to perform surgery, often the lack of nursing support and the refund from NHS, because this procedure is often considered as mere aesthetic surgery. Moreover, in patients with lower body mass index, the removal of moderate amounts of fat can be very demanding and difficult to carry out. As for future prospects, a proposal suggested by Magalon and his group [14,17] is the use of platelet-rich plasma combined with fat to ensure a better survival of graft.
Further randomized controlled studies are needed to confirm these observational data, conducted on a limited series of patients.
References
- Barsotti S, Stagnaro C, Della Rossa A (2015) Systemic sclerosis: a critical digest of the recent literature. Clin Exp Rheumatol 33: S3-S14.
- Tyndall A, Tyrrel Kennedy A, Allanore Y, Khanna D (2014) Clinical and experimental scleroderma. Clin Exp Rheumatol 32: S-3.
- Gimble JM, Katz AJ, Bunnell BA (2007) Adipose-derived stem cells for regenerative medicine. Circ Res 100: 1249-1260.
- Del Bene, Pozzi MR, Rovati L, Mazzola I, Erba, Bonomi S (2014) Autologous fat grafting for scleroderma-induced digital ulcers. An effective technique in patients with systemic sclerosis. Hand Chir Mikrochir Plast Chir 46: 242-247.
- Del Papa N, Caviggioli F, Sambataro D, Zaccara E, Vinci V, et al. (2015) Autologous Fat Grafting in the Treatment of Fibrotic Perioral Changes in Patients with Systemic Sclerosis. Cell Transplantation 24: 63-72.
- Roh MR, Jung JY, Chung KY (2008) Autologous fat transplantation for depressed linear scleroderma-induced facial atrophic scars. Dermatol. Surg 34: 1659-1665.
- Coleman SR (2006) Structural fat grafting: more than a permanent filler Plast Reconstr Surg 118: 108-120.
- Mouthon L, Rannou F, Bérezné A, C Pagnoux C, J-P Arène JP, et al (2007) Development and validation of a scale for mouth handicap in systemic sclerosis: the mouth handicap in systemic sclerosis scale. Ann Rheum Dis 66: 1651-1655.
- Rigotti G, Marchi A, Galié M, Baroni G, Benati D, et al. (2007) Clinical treatment of radiotherapy tissue damages by lipoaspirates transplant: A healing process mediated by adipose derived stem cells. Plast Reconstr Surg 119: 1409-1422.
- Salgarello M, Visconti G, Barone-Adesi L (2012) Fat grafting and breast reconstruction with implant: Another option for irradiated breast cancer patients. Plast Reconstr Surg 129: 317-329.
- Scuderi N, Ceccarelli S, Onesti MG, Fioramonti P, Guidi P, et al. (2013) Human adipose-derived stem cells for cell-based therapies in the treatment of systemic sclerosis. Cell Transplant 22: 779-795.
- Maddali Bongi S, Landi G, Del Rosso A, Miniati I, Conforti ML, et al. (2011) The rehabilitation of facial involvement in systemic sclerosis: efficacy of the combination of connective tissue massage, Kabat’s technique and kinesitherapy -a randomized controlled trial. Rheumatol Int 31: 895-901.
- Hsu VM, Stransky CA, Bucky LP, Percec I (2012) Fat grafting's past, present, and future: why adipose tissue is emerging as a critical link to the advancement of regenerative medicine. Aesthetic Surgery Journal 32: 892-899.
- Magalon G, Daumas A, Sautereau N, Magalon J, Sabatie F, et al. (2015) Regenerative Approach to Scleroderma with Fat Grafting. Clin Plastic Surg 42: 353-364.
- Guillaume-Jugnot P, Daumas A, Magalon J Jouve E, Nguyen PS, et al. (2016) Autologous adipose derived stromal vascular fraction in patients with systemic sclerosis: 12-month follow-up. Rheumatology 55: 301-306.
- Arena A, Committeri U , Maglitto F, Salzano G, Dell’Aversana Orabona G, et al. (2022) Three different types of fat grafting for facial systemic sclerosis: a case series. J Clin Med 11(18): 5489.
- Abellan Lopez M, Philandrianos C, Daumas A, Velier M, Arcani R, et al. (2022) Assessing the effect of PRP addition to facial micro-lipofilling for patients suffering from Scleroderma: A prospective routine care analysis. Ann Chir Plast Esthet 17: S0294-1260(22)00118-2.






























