A Study of Intralesional Tranexamic Acid versus Platelet Rich Plasma in Melasma- A Split Face Comparative Study
Madan lal*, Manisha Nijhawan, Divya Yadav, Manish Rijhwani and Sankalp Awasthi
Mahatma Gandhi Medical College And Hospital , Ricco Industrial Area, Sitapura, India
Submission: January 21, 2021;Published: February 11, 2020
*Corresponding author: Madan Lal, Mahatma Gandhi Medical College And Hospital, Ricco Industrial Area, Sitapura, India
How to cite this article: Madan l, Manisha N, Divya Y, Manish R, Sankalp A. A Study of Intralesional Tranexamic Acid versus Platelet Rich Plasma in Melasma- A Split Face Comparative Study. JOJ Dermatol & Cosmet. 2021; 3(4): 555625. DOI: 10.19080/JOJDC.2021.03.555625
Abstract
Melasma is a chronic acquired hypermelanosis of sun- exposed area . Mostly seen in women of reproductive age group, commonly occurring after the pregnancy. Various causative factors play a vital role in etiology like sex hormone, phototoxic drug, sun exposure. This study sought to evaluate the comparative effect of intralesional tranexamic acid and platelet rich plasma for Melasma. This is a prospective , open-label study with a sample size of 37. The procedure was done at interval of 21 days(4 visits) and followed for three month at monthly basis.
Keywords: Melasma; Tranexamic Acid; Platelet Rich Plasma
Abbreviations: TA: Tranexamic acid; PRP: platelet rich plasma; mMASI: modified melasma area severity score
Introduction
Melasma is derived from a greek word “melas” meaning “black”. Melasma is a acquired more or less symmetrical hypermelanosis of sun-exposed skin [1,2]. Melasma is a chronic disorder characterized by grey-brown patches and macules with well defined geographic borders affecting sun exposed area of the face such as the bridge of the nose, cheek, upper lip, forehead and mandibular area . Melasma is classified into epidermal, dermal and mixed type on the basis of wood’s lamp examination. It is mostly seen in women of reproductive age group and onset is usually after the pregnancy. Males are affected in around 10% of the total cases. Various causative factors play a role in aggravation and precipitation of melasma which includes sex hormones, oral contraceptive pills, phototoxic drugs, genetic predisposition, sun exposure [3]. Melasma is more common in Asians and Middle East Countries [4]. Various treatment options such as topical depigmenting agents [5], chemical peels [6], dermabrasion, laser therapies [7], platelet rich plasma have been utilised in different studies. Intralesional Tranexamic acid (TA) is a plasmin inhibitor which decreases abnormal fibrinolysis to reduce blood loss [8]. TA also inhibits UV induced plasmin activity in keratinocytes by inhibiting the binding of plasminogen to keratinocytes leading to less quantity of free arachidonic acid and reduced ability to produce prostaglandins , thereby reducing melanogenesis [9]. TA also has a role in inhibiting keratinocyte-activating-melanocytes pathway. TA also reduces hyperpigmentation by blocking generation of single chain urokinase PA by keratinocytes which increases melanocytic activity [10]. The platelet rich plasma (PRP) is a plasma suspension obtained after centrifugation of whole blood, containing higher platelet, complement factors and a range of growth factor, chemokines-cytokine and various plasma protein concentration [11,12]. These platelet derived growth factors leads to increased synthesis of hyaluronic acid, which is responsible for maintaining skin tone and volume, hence reducing the skin pigmentation. The aim of this study was to compare and evaluate the efficacy and safety of intradermal injection of TA and PRP in the treatment of different types of melasma.
Material and Method
37 patients with melasma were included in this study. All patients were recruited from the OPD of Dermatology and Venereology Department, Mahatma Gandhi Medical College, Jaipur from the period of March 2019 to February 2020. Adult patients between 20 and 50 years of age with moderate-to-severe melasma were included in the study after taking written informed consent. Patients with history of oral contraceptive pills (during the last 12 months), bleeding disorders, use of anticoagulants, topical treatment e.g. hydroquinone (one month before the study), active dermatoses, pregnant or lactating females and patients with unrealistic expectations were excluded. After obtaining detailed personal and medical history, Wood’s lamp examination was performed to classify the type of melasma. A modified MASI scoring system was used to assess the severity of melasma. In the intralesional group, patients were administered intradermal injections of tranexamic acid. About 2U of tranexamic acid was drawn in a 40U/ml 30gauge insulin syringe and diluted with normal saline up to 1 ml (remaining 38 U out of total 40 U) to get a concentration of approximately 4 mg/ml of tranexamic acid. Intradermal injections were given at the site of melasma, after application of topical anesthetic, keeping a distance of around 1cm from each injection.
Four sessions at intervals of a 21days were carried out. Various measures for strict photoprotection were explained to each patient. All patients were given the same sunscreen (of sun protection factor 50) for the entire 6 months. The left side of the face was treated with intralesional injection of PRP using 40U/ml insulin syringe. Approximately 1 ml of PRP was injected intradermally for the lesions. To assess the clinical response, clinical photographs were taken at the beginning of the therapy and then serially after 21 days. mMASI scoring, was performed at 21 days intervals and any adverse events and complications were recorded. The response to treatment in each patient was graded at the end of the study as: No response(no improvement), mild response(<25% improvement), moderate response (25% to < 50% improvement), good response (50% to <75%improvement), very good response(>75% improvement). Each case was followed up for 6 months to look for further improvement/relapse.
Result
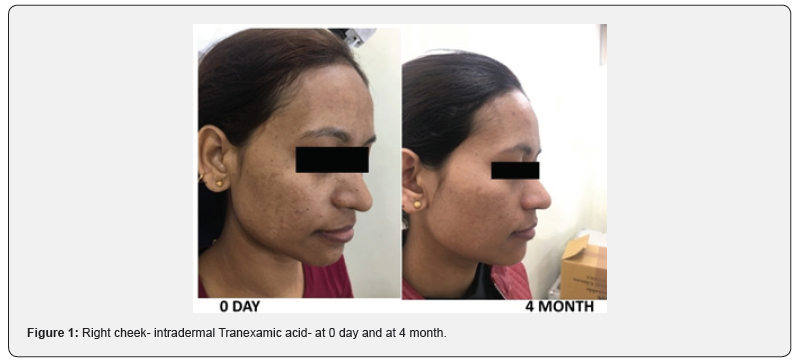
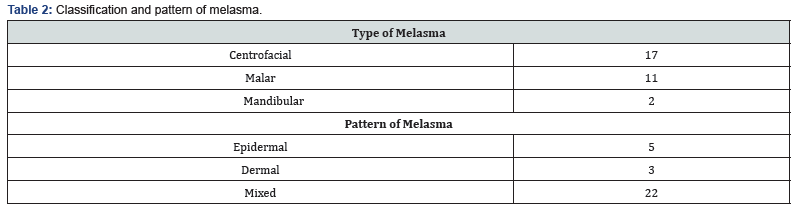
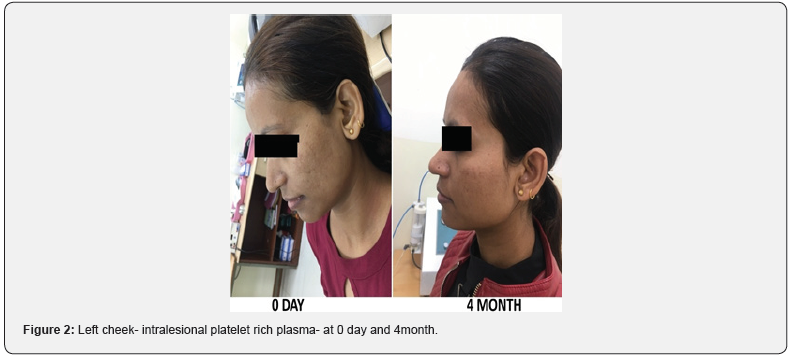
Out of 37 patients, 7 were lost in follow up. Total 30 patients completed the study, maximum no. of patients (16 pts.) belonged to age group 20-30 year (Table 1). All patients included were having Fitzpatrick skin type 4 or 5. 28 patients showed centrofacial or malar pattern of distribution of melasma. 22 (73.3%) patients had mixed type of melasma (Table 2). In the intralesional TA group , the mean mMASI score before starting of treatment was 7.83±3.18 (mMASI 1) and at the end of seventh visit (mMASI 7) was 4.5±1.9 (Figure 1). In the PRP group, the mean mMASI score at the baseline was 7.81±3.17 (mMASI 1) and at the end of seventh visit (mMASI 7) was 5.1±1.8 (Figure 2). Out of 30 patients who completed the study only five patients had the family history of melasma . Regarding predisposing factors, melasma in 3 patients was related to pregnancy and 6 patients has reported to be moderate to severe sun exposure.
Discussion
This is a randomized, open-label, comparative study done during period of March 2019 to February 2020. The patients diagnosed as melasma in Dermatology OPD at Mahatma Gandhi Hospital, Jaipur during study period and those who volunteered for intralesional TA and PRP treatment modalities were included in the study. This study showed that intradermal TA was more effective than PRP. Melasma is a distressful condition for patient as it affects the face and have a negative impact on quality of the life of patients, affecting their psychological and emotional well- being. Mechanism of action of TA in treatment of melasma is not fully understood but is assumed to suppress UV induced plasmin activity in keratinocyte. Firstly, TA inhibits the interaction of plasminogen and keratinocyte, subsequently reducing the synthesis of free arachadonic acid and prostaglandins which stimulates tyrosinase activity. Plasmin is also responsible for angiogenesis as it increases diffusible forms of vascular endothelial growth factor. Thus, TA leads to reduction of angiogenesis by inhibiting plasmin. Human keratinocytes secrete the urokinase-type plasminogen activator which is responsible for the increased activity of melanocytes in vitro. Inhibition of this mechanism by TA leads to decrease in hyperpigmentation in melasma patients [13].
PRP was reported to successfully treat melasma in a Turkish study. The study showed improvement of more than 80% in melasma at the end of the third session. They did not provide any other treatment or post treatment care. No recurrence has been reported for 6 month follow up [14]. Mesotherapy was introduced by Pistor in France [15]. Now it is widely used. This technique includes subcutaneous or intradermal microinjections of 0.05 to 0.1 mL at the lesional sites. The aim is to deliver an adequate amount of drug at the lesional site and avoiding major side effects of oral medication. There was mild discomfort and erythema seen which subsided without the need for other interventions. In this study, we have used localized microinjections (mesotherapy) to deliver TA and PRP. At tranexamic side in our study the mean MASI before treatment was 7.83±3.18 and at the end of the 7th visit MASI was 4.5±1.9 and out of 30 patients 20% showed no improvement, 26.6% showed mild improvement, 23.3% showed moderate improvement while 10% showed excellent improvement, while a study done by Ahmed Said Abdelshafy showed statistically significant difference as regard mMASI between baseline with a mean ± SD (6.92 ± 5) and at end of treatment with a mean ±SD (2.83 ±2.97). According to the degree of improvement, 4 patients (17.4%) showed moderate improvement, 8 patients (34.8%) showed good improvement and 11 patients (47.8%) showed excellent improvement. At PRP side , in our study the initial mean MASI before injection was 7.81±3.17 and at the end of 7th visit was 5.1± 1.8. According to our study 20% showed no improvement while 30% showed mild improvement, and 16.67% with good improvement and 16.66% with very good improvement. which was quite similar to study done by Ahmed Said Abdelshafy which showed statistically significant difference as regard mMASI between baseline with a mean ±SD (7.54±4.67) and at the end of treatment with a mean ±SD (4.6±3.41). According to the degree of improvement, 2 patients (8.7%) showed no improvement, 3 patients (13%) showed poor improvement, 8 patients (34.8%) showed moderate improvement, 7 patients (30.4%) showed good improvement and 3 patients (13%) showed excellent improvement [16]. Thus, intralesional tranexamic acid showed much better improvement than platelet rich plasma in Melasma.
References
- Sanchez NP, Pathak MA, Sato S, Fitzpatrick TB, Sanchez JL et al. (1981) Melasma: a clinical, light microscopic, ultrastructural, and immunofluorescence study. J Am Acad Dermatol 4(6): 698-710.
- Hexsel D, Rodrigues TC, Dal’Forno T, Lima MM, Zechmeister (2009) Melasma and pregnancy in southern Brazil. J Eur Acad Dermatol Venereol 23(3): 367-368.
- Grimes PE (1995) Melasma. Etiologic and therapeutic considerations. Arch Dermatol 131(12): 1453-1457.
- Morelli JG, Norris DA (1993) Influence of inflammatory mediator and cytokines in human melanocyte function. J Invest Dermatol 100: 191S-1915.
- Bentley PB, Bayles MA (1975) Cutaneous reactions to topical application of hydroquinone. Results of a 6-year investigation. S Afr Med J 49(34): 1391-1395.
- Hurley ME, Guervara IL, Gonzales RM, Pandya AG (2002) Efficacy of glycolic acid peels in the treatment of melasma. Arch Dermatol 138(12): 1578-1582.
- Li YH, Chen JZ, Wei HC, Wu Y, Liu M, et al. (2008) Efficacy and safety of intense pulsed light in treatment of melasma in Chinese patients. Dermatol Surg 34(5): 693-700.
- Shimizu M, Naito T, Okano A, Aoyagi T (1965) Trans-4 aminomethylcyclohex anecarboxylic acid as a potent antiplasmin agent. Chem Pharm Bull (Tokyo) 13(8): 1012-1014.
- Ebrahimi B, Naeini FF (2014) Topical tranexamic acid as promosing treatment for melasma. J Res Med Sci 19(8): 753-757.
- Maeda K, Tomita Y (2007) Mechanism of the inhibitory effect of tranexamic acid on melanogenesis in cultured human melanocytes in the presence of keratinocyteconditioned medium. J Health Sci 53(4): 389-396.
- Alshami S (2014) Treatment of periorbital hyperpigmentation using platelet rich plasma injections. AJDV 3(5): 87-94.
- Alves R, Grimalt R (2018) A Review of Platelet-Rich Plasma: History, Biology, Mechanism of Action, and Classification. Skin Appendage Disord 4(1): 18-24.
- Zhang XY, Yang XH, Yang H, Yang YP (2003) Study of inhibitory effect of acidum tranexamicum on melanin synthesis. Chin J Dermatovenerol Int Tradit West Med 2: 227-229.
- Çayırlı M, Çalışkan E, Açıkgöz G, Ahmet HE, Gunes E (2014) Regression of melasma with platetlet rich plasma treatment. Ann Dermatol 26(3): 401-412.
- Pistor M (1979) Un defi therapeutiche: la mesotherapie. In: 3rd (edn.), Maloine, France, pp. 1-50.
- Abdelshafy A (2019) Intralesional Tranexamic Acid Versus Platelet Rich Plasma in Melasma Treatment . A Split Face Comparative Study.






























