Cutaneous Manifestations of Lupus Erythematosus in Antananarivo (Madagascar)
Irina Mamisoa Ranaivo1*, Malalaniaina Andrianarison2, Fandresena Arilala Sendrasoa2, Onivola Raharolahy2, Lala Soavina Ramarozatovo2 and Fahafahantsoa Rapelanoro Rabenja2
1Department of Dermatology, University Hospital Morafeno, Madagascar
2 Department of Dermatology University Hospital Joseph Raseta Befelatanana Antananarivo, Madagascar
Submission: October 11, 2019; Published: November 14, 2019
*Corresponding author: Irina Mamisoa Ranaivo, Department of Dermatology, University Hospital Morafeno, Toamasina Madagascar.
How to cite this article: Irina Mamisoa Ranaivo, Malalaniaina Andrianarison, Fandresena Arilala Sendrasoa, Onivola Raharolahy, Lala Soavina Ramarozatovo. Cutaneous Manifestations of Lupus Erythematosus in Antananarivo (Madagascar). JOJ Dermatol & Cosmet. 2019; 2(1): 555576.
Abstract
Introduction: Lupus erythematosus is a serious autoimmune inflammatory disease. Mucocutaneous manifestations are the main clinical manifestations, so our aim is to determine the different cutaneous manifestations of lupus erythematosus in Antananarivo. Methods: A retrospective study was conducted over a period of 5 years from January 2007 to December 2011 in the medical derpartment of Joseph Raseta Befelatanana University Hospital. All patients who presented lupus erythematosus were included
Results: Among 57,509 patients seen in Joseph Raseta Befelatanana University Hospital, sixty-seven cases of lupus erythematosus were included. The mean age was 35.08 years [minimum: 9; maximum: 69 years]. The sex ratio was 0.06. Among these 67 patients, forty-six presented cutaneous manifestations (68, 65%). As specific lesions in lupus, chronic cutaneous lupus was observed in 47.82%, acute cutaneous lupus in 30.43% and subacute cutaneous lupus in 06.52% of patients. The other dermatological manifestations found were alopecia in 52.17%, photosensitivity in 43.47%, Raynaud’s phenomenon in 17.39% and bullous lesions in 06.52% of patients.
Conclusion: A little difference was found in epidemiological, clinical and paraclinical aspects in lupus Malagasy patients and Africans. Lupus erythematosus is still a under-diagnosed disease in Madagascar. A deeper understanding of the cutaneous manifestations of SLE is essential for diagnosis and prognosis.
Keywords: Lupus cutaneous manifestations Madagascar Photosensitivity Diagnosis
Abbrevations: Lupus; cutaneous manifestations; Madagascar; Photosensitivity; Diagnosis
Introduction
Systemic lupus erythematosus (SLE) is a multisystem disease characterized by immunological abnormalities. It is a multifaceted autoimmune inflammatory disease ranging patterns ranging from articular, benign cutaneous signs to severe visceral manifestations [1]. It is a chronic disease with a morbidity and mortality rate ranging from 5 to 20% [2,3]. The prevalence of SLE has been estimated at between 13 and 51 cases per 100,000 people worldwide [4,5]. Clinical onset is very polymorphic, and it is often underdiagnosed or diagnosed at a late stage, especially in Africa [6]. Early diagnosis of the disease could improve the survival of patients and knowledge of the different cutaneous manifestations would help early diagnosis of SLE especially in developing countries. Therefore, we aim is to determine the different dermatological manifestations of patients with lupus disease seen at the University Hospital Joseph Raseta Befelatanana (UH JRB) Antananarivo Madagascar
Materials and Methods
This is a descriptive retrospective study of the medical records of patients with lupus erythematosus seen and followed by the medical departments of UHJRB Antananarivo, for a period of five years from 1 January 2007 to 31 December 2011. All patients regardless of gender or age, with the diagnosis of lupus erythematosus seen in outpatient care and / or hospitalization with the medical departments of this hospital, with or without a cutaneous sign and having in addition fulfilled the criteria of ARA were included. Data were collected from medical records of patients. Patientshospitalized for lupus erythematosus but discharged with or without medical advice and those with incomplete medical records were excluded. The parameters studied were the demographic, clinical and paraclinical parameters of the patients.
Results
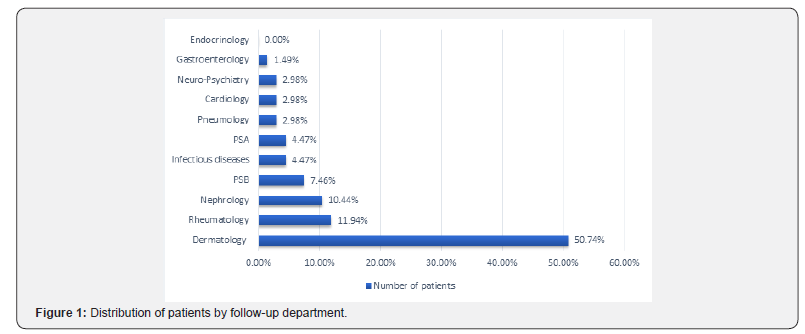
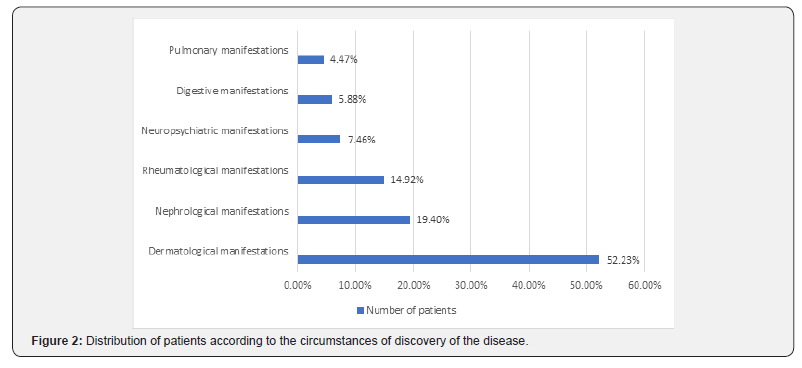
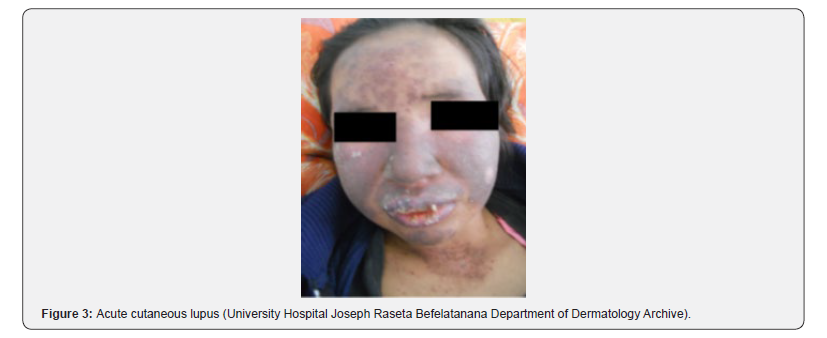
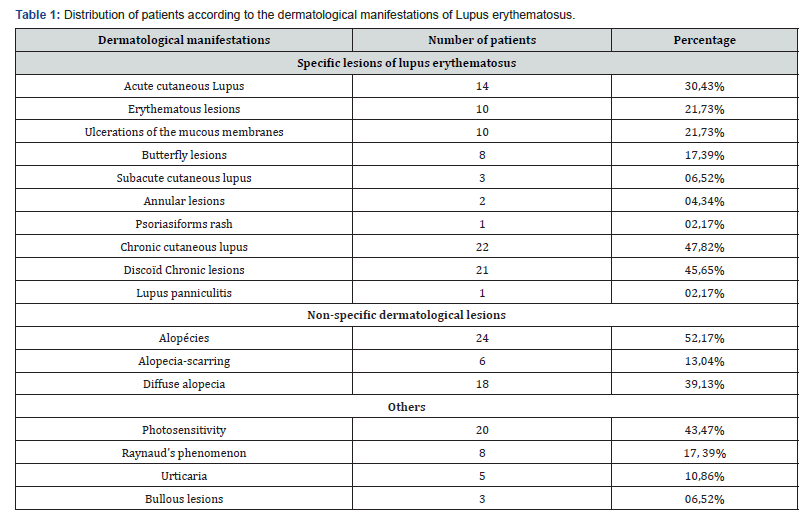
During the study period, 57,509 patients were seen at the UH JRB. Ninety-two patients had lupus erythematosus, sixty-seven of which were included in the study, a prevalence of 0.11%. The mean age was 35.08 years [minimum: 9; maximum: 69 years]. A clear female predominance was found with a sex ratio H / F of 0.06 (4 men and 63 women). Most patients were seen and followed in Dermatology Department 50.74% (36 patients) as reported in (Figure 1). A first-order family history of lupus erythematosus was noted in6 of our patients (8.95%). The diagnostic delay of lupus erythematosus was 1 to 120 months with a mean delay of 28.62 months. The dermatological manifestations were the first circumstances of discovery of lupus erythematosus, in 35 patients (52.23%) (Figure 2). Dermatological manifestations were found in 46 patients (68.65%). As specific lesions in lupus, chronic cutaneous lupus was observed in 47.82%, acute cutaneous lupus in 30.43% (Figure 3) and subacute cutaneous lupus in 06.52% of patients. For non-specific skin lesions, alopecia was found in 52.17%, photosensitivity in 43.47%, Raynaud’s phenomenon in 17.39%, urticaria in 10.39% and bullous lesions in 6, 52% of patients. The different skin manifestations of lupus are shown in (Table 1). For clinical forms, fifty-eight patients had systemic lupus (86.56%) and only nine patients had cutaneous lupus erythematosus (13.43%). Biologically, forty-two out of 58 patients (72.41%) had an accelerated erythrocyte sedimentation rate (ESR). Immunologically, antinuclear antibodies was made by 51 patients, of whom forty-one were positive (80.39%). anti-native DNA antibodies was done by 30
Discussion
Although our study was done in only one hospital, our series allowed us to characterize the epidemiological aspect of lupus erythematosus disease in Antananarivo and to appreciate the dermatological manifestations. Our study found a prevalence of 0.11%, which is comparable to previous data in Africa [7]. Most of our patients were enrolled in the dermatology department, representing 50.74% of our study population, rheumatology (11.94%) and nephrology (10.44%). This result can be explained by the fact that lupus is mainly manifested by mucocutaneous, articular and nephrological lesions [8,9]. The mean age of our patients is35.08 years which is consistent with data reported by some studies done in Maghreb [9,10] and in Africa in particular in Togo [6]. The female predominance is classic in lupus and it confirmed in our study 94.02% with a sex ratio of 0.06 [1,9]. Eighty-five percent of our patients had a family history of first-degree lupus erythematosus. This result is consistent with those reported in the literature [11]. However, it differs from that reported by Al-Maini and al in Oman, in 73 patients. During this period, a high prevalence of familial cases was noted in 48% of their patients [12]. Note that in Madagascar, the genetic study is not yet available. The time to diagnosis lupus in our study ranged from 1 to 120 months. Several factors may be involved. First of all, the factor related to the disease itself, lupus can manifest as a mono-visceral involvement and remain as such for several years [1]. And that the clinical manifestations of lupus disease are very polymorphic hence the delay diagnosis. Secondly, the low economic and geographic accessibility of care services by patients, the use of traditional treatments, or self-medication, especially for chronic diseases, delay consultations and diagnosis [13,14]. In our study lupus was revealed by dermatological manifestations in 52, 23% this result agreed with that of Togo [6]. Dermatological manifestations were present in 68.65% of our patients, this result was lower than the studies done in Tunisia and Morocco with dermatological manifestations respectively at 82% and 85.2% [9,10]. This difference was probably due to the small size of our sample and erythematous lesions are sometimes difficult to assess on dark skin. Many dermatological manifestations can be observed during lupus disease. These different cutaneous manifestations can coexist in the same patient. Similarly, all cutaneous lupus erythematosus may be associated with SLE [15].
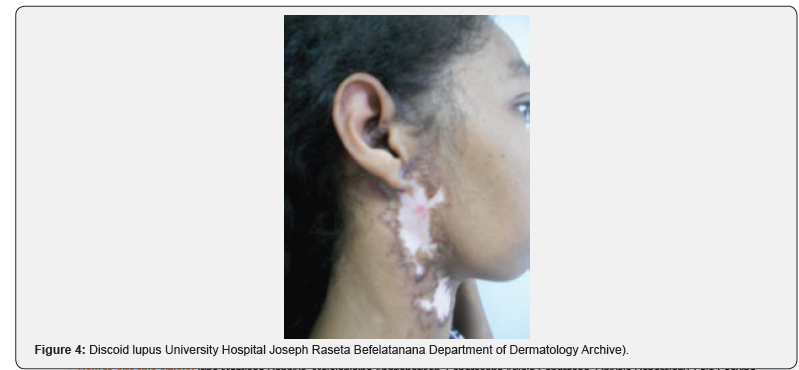
Thus, for the specific manifestations of lupus, chronic cutaneous lupus was present in 47.82% of lupus patients represented mainly by discoid lupus (Figure 4), acute cutaneous lupus was present in 30.43% of patients including erythematous lesions in photo-exposed zones and ulcerations of the mucous membranes. Finally, subacute cutaneous lupus was observed in 6.52% lupus. These results were similar to previous African studies, especially those made in Lomé and Dakar [7-8]. But in some papers acute cutaneous lupus is most often observed (60-88%) at the onset of systemic lupus erythematosus [16,17]. It is more visible on fair skin and could be underestimated on black or dark skin. Subacute cutaneous lupus most often affects Caucasians (85%) [17]. Regarding other manifestations, alopecia was frequent in our series (52.17%) alopecia- scarring in 13,04% of cases and diffuse alopecia type telogen effluvium contemporaneous with a flare of lupus erythematosus systemic or occurring 3 months after [17]. Photosensitivity, a common symptom and part of the diagnostic criteria for ARA, was found in 43.47% of our patients. According to the literature it is present in 40%- 90% of patients with lupus erythematosus [18,19] Photosensitivity may not only be manifested by cutaneous symptoms, such as rash or tingling, but also by asthenia and arthralgia. But its appreciation is difficult as the duration between sun exposure and the appearance of signs varies from a few days to 6 weeks [18]. The presence of Raynaud’s phenomenon in our patients (17.39%) was consistent with previous data described in the literature [9,17] as well as the presence of urticaria 10.86%. Bullous lesions were found in 6.52% of our patients, while bullous lupus is a rare manifestation of SLE. It may be the first sign of SLE with severe visceral involvement, especially renal [20]. All these forms of cutaneous lupus can be associated with SLE with a variable frequency. Thus 86.56% of patients had systemic lupus erythematosus and only 13.43% isolated cutaneous lupus. More than 90% of patients with acute cutaneous lupus erythematosus will have SLE. Ten to twenty percent of patients with discoid lupus will have SLE. And panniculitis is observed in only 2 to 3% of SLE cases in our study (2.17%) [17]. The presence of inflammatory syndrome including the acceleration of the ESR, the presence of antibodies against and native anti-DNA antibodies were comparable to those found in the literature. Skin lesions do not influence the immunological and biological profile of lupus patients [9,16].
Conclusion
According to our study, 68.65% of the lupus patients seen in the Antananarivo UHJRB had cutaneous manifestations. Chronic lupus was observed in 47.82% of patients and acute lupus erythematosus at 30.43%. We found that there was little difference between patients in Madagascar and those in sub-Saharan Africa, both in epidemiological, clinical and paraclinical aspects. But it should be noted that lack of knowledge and ignorance of the disease make lupus under-diagnosed in Madagascar.
References
- Dörner T, Furie R (2019) Novel paradigms in systemic lupus erythematosus. Lancet 393(10188): 2344-2358.
- Hajji M, Harzallah A, Kaaroud H, Ben Hamida F, Barbouch S, et al. (2014) Les facteurs prédictifs de mortalité au cours du lupus. Néphrologie & Thérapeutique 10(5): 275.
- Bouras M, Hali F, Khadir K, Benchikhi H (2014) Lupus érythémateux systémique: mortalité et facteurs de mauvais pronostic dans une série marocaine de 129 cas. Ann Dermatol Vénéréol 141: 141-143.
- Esmaeilzadeh E, Khodamoradi Z, Nazarinia MA (2019) One-decade study of distinct features, morbidity and mortality of systemic lupus erythematosus (an update on systemic lupus erythematosus in the Fars Province of Iran). Lupus 28(11): 1360-1367.
- Gergianaki I, Fanouriakis A, Repa A, Spirou G, Chatzi L, et al (2017). Epidemiology and burden of systemic lupus erythematosus in a Southern European population: Data from the community-based lupus registry of Crete, Greece. Ann Rheum Dis 76(12): 1992-2000.
- Kombate K, Saka B, Oniankitan OI (2008) Le Lupus Systé-mique à Lomé, Togo Med Trop 2008; 68: 283-286.
- Teclessou NJ, Kombaté K, Akakpo AS, Saka B, Matakloé H, et al. (2017) Maladie lupique en milieu hospitalier à Lomé : Etude rétrospective de 116 cas. RAFMI 4 (1-1): 19-23.
- Diop MM, Gueye YA, Lèye A, Touré PS, Berthe A, et al. (2014) Les modes de révélation du lupus érythémateux systémique à Dakar (Sénégal) : à propos d’une série de 161 cas. RAFMI 1(2): 1-15.
- Louzir B, Othmani S, Ben Abdelhafidh N (2003) Le lupus érythémateux systémique en Tunisie. Étude multicentrique nationale. À propos de 295 observations. Rev Méd Int 24 :768-777.
- Bouatba L, Bachir H, Ammouri W (2014) Lupus érythémateux systémique au Maroc: étude analytique monocentrique de 440 patients. Rev Méd Int 35S : A142.
- Deligny C, Thomas L, Dubreuil F (2002) Lupus systémique en Martinique: enquête épidé Rev Med Int 23(1): 21-29.
- Al-Maini MH, El-Ageb EM, Al-Wahaibi SS, Al-Farsi Y, Richens ER (2003) Demographic, autoimmune, and clinical profiles of patients with systemic lupus erythematosus in Oman. Rheumatol Int 23(4): 186-191.
- Fandresena FA, Ranaivo IM, Razanakoto NH, Onivola R, Lala SR et al. (2017) Limited Management of Systemic Erythematosus Lupus in Madagascar. International Journal of Clinical Dermatology 1(1): 1-4.
- Ranaivo IM, Sendrasoa FA, Harioly Nirina MOJ (2019) Self-Medication during Dermatological Disorders Seen in the Dermatology Department of the University Hospital Joseph Raseta Befelatanana, Antananarivo Madagascar. EC Microbiology 15(5) : 339-343.
- Doffoel-Hantz V, Savi V (2017) Principales manifestations dermatologiques du lupus érythémateux disséminé. Actualités pharmaceutiques 56(567): 22-25.
- Larbi T, Abdelkefi C, Elouni A, Bouslema K, Hamzaoui S, et al. (2015) Manifestations dermatologiques du lupus érythémateux systé Rev Méd Int 36S : A96.
- Francès C, Barète S, Piette JC (2008) Manifestations dermatologiques du lupus. Rev Méd Int 29(9): 701-709.
- Bens G(2009) Photosensibilité du lupus érythé Rev Méd Int 30(10): 857-865.
- Ahluwalia J, Marsch A (2019) Photosensitivity and photoprotection in patients with lupus erythematosus Lupus 28(6): 1-6.
- Jira M, Elqatni M, Sekkach Y, Elomri N, Mekouar F, et al. (2013) Étude de trois cas de lupus érythémateux bulleux. Ann Dermatol Vénéréol 140(12): 778-783.






























