Impact of COVID on In-Hospital Outcomes in Patients with Anemia: Perspectives from National Inpatient Sample
Saad Javaid1*, Kelly Frasier2 and Nouman Aziz1
1Wyckoff Heights Medical Center, USA
2A T Still University School of Osteopathic Medicine, USA
Submission: December 02, 2023; Published: December 14, 2023
*Corresponding author: Saad Javaid MD, Wyckoff Heights Medical Center, 374 Stockholm St, Brooklyn, NY, 11237, USA, Email: sjavaid@wyckoffhospital.org
*Corresponding author: Ryan Goodmanson, DO, 1231 Pine Grove Ave, Port Huron, MI 48060, USA
How to cite this article: Saad J, Kelly F, Nouman A. Impact of COVID on In-Hospital Outcomes in Patients with Anemia: Perspectives from National Inpatient Sample. JOJ Case Stud. 2023; 14(3): 555889. DOI: 10.19080/JOJCS.2023.14.555889.
Abstract
Background: The implications of COVID on anemia patients have expressed concerns because many of these individuals already have weakened immune systems and are more susceptible to severe illness. Our research aimed to comprehensively explore the multifaceted impact of COVID-19 on patients admitted for anemia and the adverse outcomes associated with it.
Methods: We searched the National Inpatient Sample 2020 using ICD 10 codes to identify patients hospitalized with a primary discharge diagnosis of anemia, with or without a secondary diagnosis of COVID infection. A weighted sample was employed to determine baseline patient characteristics. A multivariate regression model was used to estimate primary and secondary outcomes.
Results: Among the 147165 patients admitted with anemia, 2290 had the concurrent diagnosis of COVID. Higher rates of mortality were noted among patients with COVID infection as compared to those without COVID. Length of stay was significantly increased in COVID patients, 5.10 days vs. 3.38 days, but hospitalization costs didn't significantly rise. COVID patients had higher odds of GI bleeding but lower EGD and colonoscopy rates, including the procedures to control active GI bleeding. COVID patients were more likely to develop acute respiratory failure, but there was no statistically significant difference between the two groups regarding mechanical ventilation or ICU admission.
Conclusion: In conclusion, our data indicated that concurrent COVID infection in patients hospitalized with anemia could lead to increased mortality risk, higher rates of GI bleeding, acute respiratory failure, and longer hospital stays.
Keywords: Anemia, COVID, National Inpatient sample; NIS; Anemia COVID
Introduction
The global pandemic caused by COVID-19 has affected a staggering number of individuals, with over 760 million people worldwide infected as of March 2023 and more than 6.8 million fatalities recorded [1]. The illness presents itself in varying degrees, ranging from asymptomatic cases to those that resemble the flu, while others develop severe acute respiratory distress syndrome (SARS-CoV-2). Hematologic manifestations observed in COVID-19 patients include but are not limited to anemia, thrombocytopenia, coagulopathy, lymphopenia, elevated ferritin levels, and elevated D-dimers; however, this article will concentrate on anemia specifically and the outcomes associated with concomitant COVID-19 infection.
Studies have suggested that COVID-19 could negatively affect the course of anemia in hospitalized patients [2-4]. The study focuses on evaluating the clinical outcomes of COVID infection in patients hospitalized with anemia. It takes into consideration how the spread of COVID-19 may have impacted access to healthcare for these vulnerable groups and offers insights into potential avenues for improving care delivery during pandemics in the future.
Materials and Methods
In our retrospective cohort study, we aimed to identify adult patients who were hospitalized with a primary diagnosis of anemia. To obtain relevant data, we expanded our research by utilizing the National Inpatient Sample for 2019. The National (Nationwide) Inpatient Sample (NIS) is a database that provides valuable insights into inpatient discharge data for the US population. The significance of this database is undeniable, given that it encompasses over 98% of the entire US population and almost 1,000 hospitals across the country. It includes discharges from community hospitals, excluding those concerning rehabilitation and long-term acute cases.
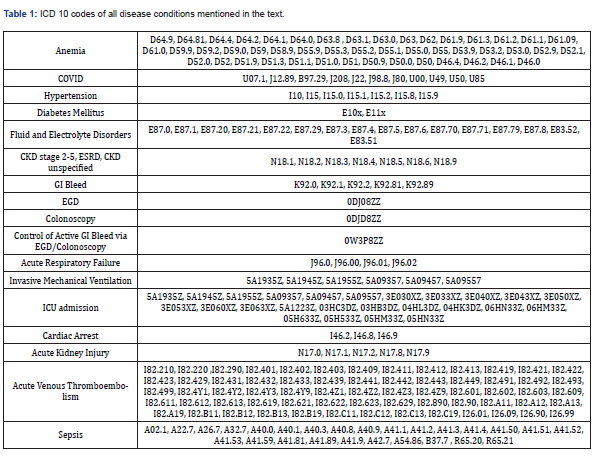
Inclusion criteria included patients aged 18 years and older who were hospitalized with the primary discharge diagnosis of anemia, and they were separated into two categories based on the presence or absence of COVID-19 virus infection. The diagnosis and procedures were identified using commonly employed coding programs such as ICD-10-CM and PCS classifications. The comprehensive list of ICD-10 codes used in this study can be viewed in detail by referring to Table 1. Patient and hospital characteristics, along with the comorbidities in both groups, were recorded.
The primary outcome was comparing mortality as a metric of clinical severity among patients hospitalized with anemia depending on the presence or absence of COVID-19 virus infection. Secondary outcomes included length of stay, upper GI endoscopy, colonoscopy, invasive mechanical ventilation, ICU admission, and hospital expenditure incurred as a gauge of healthcare resource utilization amongst both groups, as well as GI bleeding, acute respiratory failure, acute kidney injury, sepsis, venous thromboembolism, and cardiac arrest as measures of complications during the hospital stay.
Stata® (Statistics and Data) Version 17 BE software (StataCorp, Texas, USA) was used for data analysis. In the study, several rigorous statistical methods were employed to ensure accurate and reliable results. We utilized weighted samples for national estimates as per HCUP regulations when analyzing the NIS database. By using this approach, it was ensured that the findings would be representative of the entire population under study. Patients' demographics and comorbidities were calculated as proportions of the cohort, giving a more in-depth understanding of how prevalent they were among different subgroups. To compare the association between COVID-19 and non-COVID-19 subgroups, researchers used the Chi-squared test, a widely accepted method for testing associations between categorical variables. Similarly, the Student's t-test was used to compare continuous variables between the two groups. Furthermore, multivariate regression analysis was applied to adjust for possible confounders when calculating both primary and secondary outcomes. Significance thresholds were set at p0.05 during regression analysis, offering an additional layer of validation. Finally, the odds ratios derived from this comprehensive methodology provide valuable insights into how various factors contribute either positively or negatively toward overall health status and outcomes.
The studies using NIS are not subject to the Institutional Review Board as it does not contain patient identifiers or identifiable hospital or state information, in compliance with HIPAA regulations to protect patient anonymity.
Results
Baseline characteristics of the study population
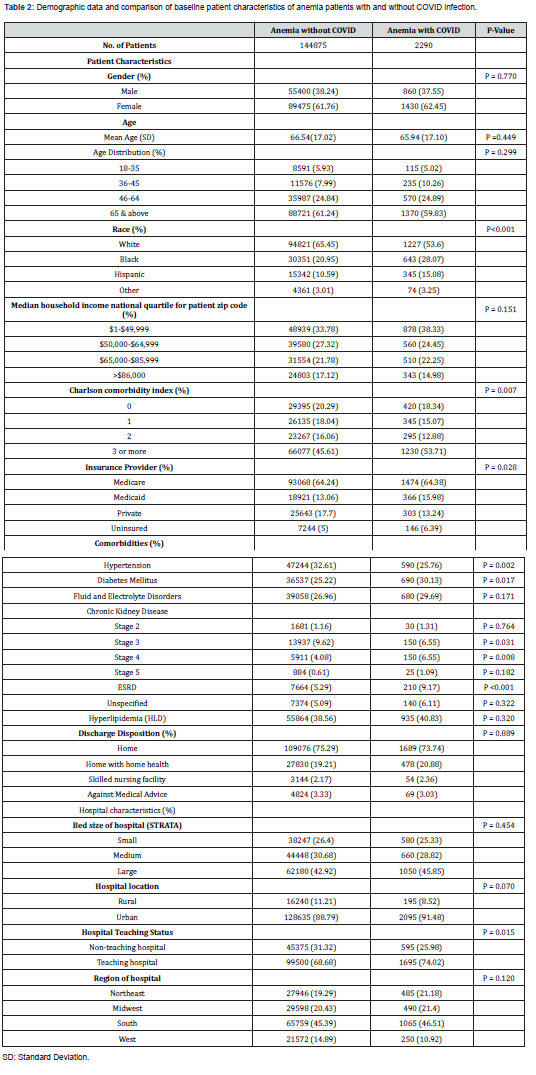
A total of 147,165 weighted hospitalizations with anemia were included in the study. 144,875 (98%) patients were without COVID-19 virus infection, and 2,290 (1.55%) had a secondary diagnosis of COVID-19 infection. Caucasians (65.5% vs. 53.6%) were more prevalent in the non-COVID-19 group, whereas African Americans (28.07% vs. 20.95%) and Hispanics (15.08% vs. 10.59%) were more prevalent in the COVID-19 group, P<0.001. A larger proportion of COVID-19 patients had a Charlson Index of >=3 (53.71% vs. 45.61%), P = 0.007. Similarly, a larger proportion of COVID-19 patients were uninsured (6.39% vs. 5%), and the non-COVID-19 patients tended to have more private insurance (17.7% vs. 13.24%), P = 0.028. A large proportion of COVID-19 patients were admitted to teaching hospitals as compared to non-COVID-19 patients (74.02 vs. 68.68%), P = 0.015. Table 2 summarizes the detailed baseline characteristics of both groups.
Primary outcomes
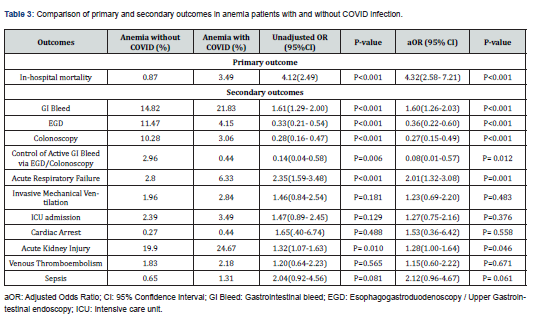
After carefully accounting for potential confounding variables, such as baseline characteristics, comorbidities, and hospital characteristics in our analysis, the mortality rate (the primary outcome) was significantly higher (3.49% vs. 0.87%) among patients who were found to have concomitant COVID-19 infection as compared to the non-COVID-19 group with the adjusted odds ratio of 4.32, 95% CI (2.58- 7.21), P< 0.001 (Table 3).
Secondary outcomes
In terms of secondary outcomes, COVID-19 was significantly associated with increased odds of GI bleeding aOR 1.60 (95% CI 1.26-2.03), P <0.001, and acute respiratory failure aOR 2.01 (95% CI 1.32-3.08), P = 0.001. However, no statistically significant difference was noted with regard to invasive mechanical ventilation aOR 1.23 (95% CI 0.69-2.22), P = 0.48; admission to an intensive care unit aOR 1.27 (95% CI 0.75-2.16), P = 0.38; sepsis aOR 2.12 (95% CI 0.96-4.67), P = 0.06; venous thromboembolism aOR 1.15 (95% CI 0.60-2.22), P = 0.671; and cardiac arrest aOR 1.53 (95% CI 0.36-6.42), P = 0.56 (Figure 1). However, surprisingly, the rates of upper GI endoscopy aOR 0.36 (95% CI 0.22-0.60), P< 0.001, colonoscopy aOR 0.27 (95% CI 0.15-0.49), P< 0.001, and EGD/colonoscopy to control active GI bleed aOR 0.08 (95% CI 0.01-0.57), P = 0.001, were significantly decreased in the COVID-19 patients despite the increased odds of GI bleeding (Table 3).
The length of stay was increased 5.10 days (95% CI: 3.83–6.38) vs. 3.38 days (3.30–3.46), P< 0.001 in the COVID-19 patients (Figure 2), and there was no statistically significant difference in the hospitalization charges between the two groups: 45,116 USD (95% CI: 43,229–47,003) vs. 55,698 USD (95% CI: 39,737–71,660), P = 0.178 (Table 4)

Discussion
Anemia refers to a medical condition characterized by reduced levels of red blood cells or hemoglobin concentration within the erythrocytes, which hinders efficient oxygen transport via hemoglobin. Consequently, an insufficient supply of oxygenated blood reaches various tissues across the body. COVID-19 is a disease with multi-systemic implications, capable of impacting not only the respiratory system but also various other organs within the body. The presentation of symptoms can differ among individuals [5]. Pre-existing anemia or anemia upon admission for a hospitalization related to COVID-19 is associated with poor outcomes, increased length of hospital stay, and increased mortality [4,6,7]. Recent studies demonstrated pre-existing anemia represents a risk factor for severe COVID-19 infection [8,9]. Additionally, the decreased oxygen delivery to peripheral tissues seen in patients with anemia leads to a decreased supply and increased demand on the lungs in COVID-19 pneumonia, which leads to increases in acute respiratory distress syndrome (ARDS). COVID-19 infection of the lungs leads to increased oxygen demand due to respiratory compromise. The exaggerated immune response and pathogenesis of hematologic disease are caused by significant elevation in pro-inflammatory markers such as IL-beta, IL-2, IL-4, IL-10, TNF-alpha, and IFN lambda [10]. Hematologic manifestations seen in patients with active COVID-19 infections may improve after the infection subsides, but hematologic symptoms may run a longer course and become exacerbated in patients with underlying hematologic disorders, such as anemia [11]. The implications of COVID-19 on anemic patients raise concerns because many of these individuals already have weakened immune systems and are more prone to severe illness.

COVID-19 implicates multi-organ involvement with different pathways of injury. Specific to anemia, scientific literature has pointed out two potential pathophysiological mechanisms:
i. Severe acute respiratory syndrome-coronavirus-2 (SARS-CoV-2) interaction with hemoglobin molecule, through CD147, CD26, and other receptors located on erythrocyte and/or blood cell precursors;
ii. Hepcidin-mimetic action of a viral spike protein, inducing ferroprotein blockage [12].
Due to pathologic metabolic pathways derived from hemoglobin denaturation and iron metabolism dysregulation, hematologic clinical syndromes may follow. These hematologic clinical syndromes include pulmonary edema based on arterial vasoconstriction and altered alveoli-capillary barrier, sideroblastic-like anemia, endothelitis, vasospastic acro syndrome, and arterio-venous thromboembolism [12]. With the aforementioned hemoglobin dysfunction and generalized hypoxic state occurring in patients without the prior hematologic disorder, the impact of infection of COVID-19 on patients with an established anemia diagnosis or anemia upon admission warrants prompt consideration and investigation.
Emerging research suggests that COVID-19 infection can increase the likelihood of adverse events in patients with pre-existing conditions such as anemia. The susceptibility of these individuals to severe respiratory distress syndrome, coupled with their compromised immune system function, makes them particularly vulnerable to complications arising from viral infections like COVID-19 [13]. In our retrospective analysis, we found that anemic patients with COVID-19 infections had a significantly higher mortality rate than those without COVID-19 infections, as this can also be supported by emerging studies that indicate the mortality rate among this subset of patients has been significantly higher than that among those without underlying comorbidities [14]. Patients with both anemia and concomitant COVID-19 experience a lengthier period of hospitalization, as evident from our study, suggesting that the impact of COVID-19 is more severe in such cases. This observation highlights the potential complications associated with simultaneous diagnoses of these two medical conditions, underscoring the need for prompt diagnosis and treatment to ensure optimal patient outcomes [8].
Our study additionally demonstrates that the presence of COVID-19 is linked with a heightened likelihood of experiencing gastrointestinal bleeding. The association between the virus and gastrointestinal bleeding highlights the importance of further academic exploration into COVID-19's impact on the digestive system. Research studies have shown that the virus causes inflammation throughout the body, including within the digestive system, which may contribute to this risk factor for gastrointestinal bleeding [15]. But interestingly, the rates of upper gastrointestinal endoscopy, colonoscopy, and upper and lower gastrointestinal endoscopic procedures to control active gastrointestinal bleeding were significantly decreased, as evident from our study. This could be explained by the significant disruption of healthcare services due to the unprecedented outbreak of COVID-19. One such area that has been affected is surgical and endoscopic procedures, which were being avoided or postponed due to reasons such as resource scarcity and infection risk [16]. The COVID-19 virus infection is of significant concern due to its propensity for inducing severe respiratory failure, which can be particularly problematic for patients who are already suffering from underlying health conditions like anemia. Our recent study adds further weight to this concerning trend by demonstrating that hospitalized individuals with COVID-19 faced a significantly higher risk of experiencing acute respiratory failure than those without the virus. These results demonstrate the crucial need for healthcare professionals and caregivers to provide comprehensive care and management tailored to address these vulnerabilities in affected patients.
One of the most noteworthy attributes of this study was its ability to delve deeply into demographic data and outcomes on a vast national level. Furthermore, it employed an advanced multivariate logistic regression analysis that had the ability to account for various potentially confounding variables, making it all the more robust and reliable in terms of findings. However, our investigation possesses certain inherent constraints that should be acknowledged. The ICD-10 codes primarily function as billing tools, hence constraining the clinical information's sensitivity. Because the criteria for COVID-19 virus infection were established using a secondary diagnosis, it is difficult to accurately gauge the degree of infection within this range.
Conclusion
COVID-19 is a serious, potentially fatal illness that carries a high risk of morbidity and mortality among hospitalized anemic patients. Our study indicates that the occurrence of COVID-19 in individuals with anemia leads to elevated mortality rates or more unfavorable outcomes during their hospital stay relative to those without COVID-19 infection. Additionally, COVID-19 can prolong hospitalization duration while also increasing susceptibility to other comorbidities like gastrointestinal bleeding or acute respiratory failure. This study represents a crucial initial step toward improving our comprehension regarding the influence of COVID-19 on hospitalized patients suffering from anemia.
Declaration
Conflict of interest disclosure statement: The authors declare that they have no conflict of interest.
Ethics approval: HCUP Databases Are Limited Data Sets that do not include patients' identification, consent or review by an institutional review board (IRB) is not required for use of limited data sets.
Data availability: The datasets generated and/or analyzed during the current study are available at https://hcup-us.ahrq.gov/databases.jsp.
Competing interests: No competing interests of authors listed.
Funding information: No funding was received by any of the authors or by any of the agencies/parties.
Permission to reproduce material from other sources: No material was reproduced from other sources.
References
- COVID-19 Weekly Epidemiological Update. Edition 134 published 15 March 2023. World Health Organization.
- Asadzadeh R, Mozafari A, Shafiei E, Kaffashian M, Ahmadi I, et al. (2022) On-Admission Anemia and Survival Rate in COVID-19 Patients. IBJ 26(5) :389-397.
- Chen C, Zhou W, Fan W, Ning X, Yang S, et al. (2021) Association of anemia and COVID-19 in hospitalized patients. Future Virology 16(7): 459-466.
- Faghih Dinevari M, Somi MH, Sadeghi Majd E, et al. (2021) Anemia predicts poor outcomes of COVID-19 in hospitalized patients: a prospective study in Iran. BMC Infect Dis 21(170).
- Gupta A, Madhavan MV, Sehgal K, Nair N, Mahajan S, et al. (2020) Extrapulmonary manifestations of COVID-19. Nat Med 26(7): 1017-1032.
- Bergamaschi G, de Andreis FB, Aronico N, Lenti MV, Barteselli C, et al. (2021) Anemia in patients with COVID-19: pathogenesis and clinical significance. Clinical and Experimental Medicine 21(2): 239-246.
- Hariyanto TI, Japar KV, Kwenandar F, Damay V, Siregar JI, et al. (2021) Inflammatory and hematologic markers as predictors of severe outcomes in COVID-19 infection: a systematic review and meta-analysis. The American Journal of Emergency Medicine 41: 110-119.
- Tao Z, Xu J, Chen W, Yang Z, Xu X, et al. (2020) Anemia is associated with severe illness in COVID-19: A retrospective cohort study. J Med Virol 93(3): 1478-1488.
- Young BE, Ong SWX, Kalimuddin S, Low JG, Tan SY, et al. (2020) Epidemiologic Features and Clinical Course of Patients Infected with SARS-CoV-2 in Singapore. JAMA 323(15): 1488-1494.
- Agbuduwe C, Basu S (2020) Haematological manifestations of COVID-19: From cytopenia to coagulopathy. Eur J Haematol 105(5): 540-546.
- Korompoki E, Gavriatopoulou M, Fotiou D, Ntanasis-Stathopoulos I, Dimopoulos MA, et al. (2022) Late-onset hematological complications post COVID-19: An emerging medical problem for the hematologist. American Journal of Hematology 97(1): 119-128.
- Cavezzi A, Troiani E, Corrao S (2020) COVID-19: hemoglobin, iron, and hypoxia beyond inflammation. A narrative review. Clin Pract 10(2): 1271.
- Ackerman JM, Hill SE, Murray DR (2018) The behavioral immune system: Current concerns and future directions. Soc Personal Psychol Compass 12(2): e12371.
- Jha M, Tak ML, Gupta R, Sharma P, Rajpurohit V, et al. (2022) Relationship of anemia with COVID-19 deaths: A retrospective cross-sectional study. Journal of Anaesthesiology, Clinical Pharmacology 38(Suppl 1): S115-S119.
- Negro A, Villa G, Rolandi S, Lucchini A, Bambi S (2022) Gastrointestinal Bleeding in COVID-19 Patients: A Rapid Review. Gastroenterology nursing: the Official Journal of the Society of Gastroenterology Nurses and Associates 45(4): 267-275.
- Hayee B, The SCOTS project group, East J, et al. (2021) Multicentre prospective study of COVID-19 transmission following outpatient GI endoscopy in the UK. Gut 70(5): 825-828.






























