Cavernous Cervical Hemangioma: Case Report
Rania G El-Skaan1* and Salma T Hafez2
1Department of Obstetrics and Gynecology, Ain Shams University, Egypt
2Department of Pathology, Ain Shams University, Egypt
Submission: November 13, 2023; Published: December 01, 2023
*Corresponding author: Rania Gamal El-Skaan, Department of Obstetrics and Gynecology, Faculty of Medicine, Ain Shams University, Cairo, Egypt, Email: dr.raniagamal2015@yahoo.com
How to cite this article: Rania G El-Sk, Salma T H. Cavernous Cervical Hemangioma: Case Report. JOJ Case Stud. 2023; 14(3): 555888. DOI: 10.19080/JOJCS.2023.14.555888.
Abstract
Uterine cervix cavernous hemangiomas are extremely rare benign tumors. They are more common in the third decade of life. They can occasionally cause obstetric and gynecological issues, although the majority are asymptomatic and are discovered by chance. Surgical treatment is usually the preferred method, which is usually undertaken in conjunction with other illnesses. We discuss a case of cervical hemangioma discovered accidentally in a 24-year-old woman. The reason for seeing a gynecologist was frequent episodes of post-coital bleeding shortly after her marriage. The Loop Electrosurgical Excision Procedure was carried out. Histological testing confirmed the diagnosis of cervical mixed benign capillary and cavernous hemangioma.
Keywords: Cavernous; Capillary hemangioma; Uterine cervix
Introduction
The uterine cervix cavernous hemangioma is a rare benign illness. There are just about 60 examples recorded in the literature. The majority of reported cases are around 35 years old. Cavernous hemangioma is most commonly found in the liver. Vaginal bleeding or discomfort are symptoms of a cavernous hemangioma. Intermenstrual spotting, atypical uterine bleeding, postmenopausal bleeding, post-coitus bleeding, infertility, and dyspareunia are gynecological problems [1,2].
Some incidences have been linked to pregnancy. Premature membrane rupture, postpartum bleeding, and disseminated intravascular coagulation are examples of obstetrical problems. The delivery method in a pregnant mother with a cervical cavernous hemangioma may pose a problem [3].
The treatment is generally surgical, which is the modality of choice in most situations, but conservative treatments such as cryotherapy, sclerosing agents, and laser may also be considered for preserving fertility in young females. In gynecological practice, embolization treatment for arteriovenous malformations has been crowned with success in patients with severe menorrhagia, with alleviation of symptoms and preservation of reproductive function [3]. However, if prior lines of treatment have failed, the cervical hemangioma can be treated with a hysterectomy [4].
Case Report
The patient in our case is a 24-year-old woman who recently got married and has been complaining of regular contact bleeding episodes. After consulting a doctor, the patient was prescribed numerous antibiotics to treat a pelvic infection. The patient was referred to a consultant gynecologic outpatient clinic after her severe attack of contact bleeding was managed with vaginal packing and patient stabilization. Regarding easy bruises, severe menstrual bleeding, or bleeding from other orifices, the patient’s history was unremarkable. The general inspection revealed nothing unusual. Upon local examination, the majority of the cervix was covered with a reddish-bluish region.
A colposcopic examination revealed several iodine-negative spots that were biopsied. The histopathological findings revealed HPV infection (flat condyloma) and chronic nonspecific cervicitis. The treatment for chronic cervicitis was detailed, and the patient was sent to specialized clinics so that he could receive HPV vaccination. The patient and her husband, were counseled on safe sex. A few days later, the patient experienced significant contact bleeding, which was controlled by vaginal packing. The patient was re-attach to the clinic, where a Multidisciplinary Team was convened and advice for LEEP excision under anesthesia of the reddish-blue area, as well as histopathological examination by senior staff in the histopathology unit at Ain Shams Maternity University Hospital.
Intraoperative full excision was performed, and hemostasis was achieved with cauterization of the bleeding spot, suturing of both cervical angels, and silver nitrate gauze packing. Followup of the patient’s symptoms on a regular basis by phone survey for her major symptoms, which have significantly improved. Histopathological studies revealed a benign capillary and cavernous hemangioma mixture (Figure 1 & 2).
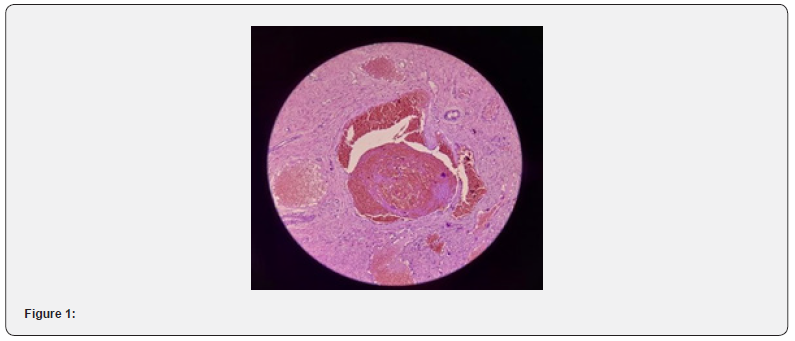
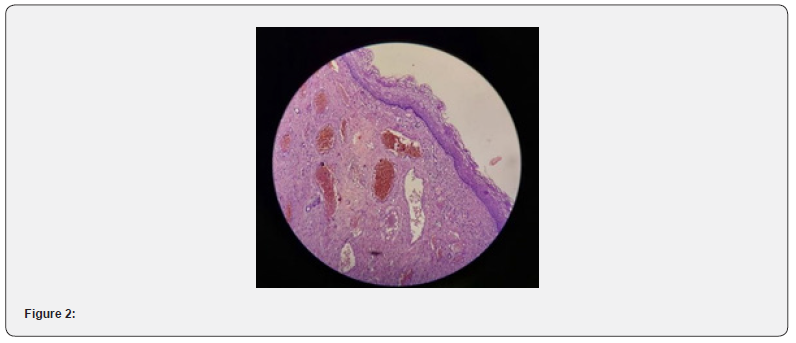
The patient was contacted at the Gynecologic Outpatient Clinic, reassured about the benign finding, and counseled about following up on cervical length during pregnancy between 18 and 24 weeks for early detection and management of future cervix shortening, as well as following up on HPV infection according to the local protocol of the early cancer detection unit.
Microscopic pictures shows stratified squamous epithelium with underlying stroma showing large cavernous and capillary type channels lined by flat endothelial cells and filled with blood, some show organizing thrombus (H&E 40X and 10X respectively).
Discussion
Hemangiomas are a common type of benign vascular disease. It most often affects the skin, subcutaneous tissue, oral cavity, liver, and kidneys. Hemangioma of the cervix, on the other hand, is extremely rare, with just about 60 occurrences reported in the literature to date. The first mention of it occurred in 1948. The great majority of reported cervical hemangiomas are in women of reproductive age [1]. The tumor is thought to be more common in the second and third decades of life and appears as postcoital or intermittent vaginal bleeding in 35% of cases. Cervical cancer should be ruled out cytologically and/or via biopsy in these circumstances [1,5].
The association between oral contraceptives and pregnancy suggests that the hormone has a function in the development of cervical hemangiomas. The symptoms of hemangiomas may be exacerbated by changes in hormone levels during pregnancy. Because of the presence of estrogen receptors in hemangioma endothelial cells, estrogen plays a crucial role in its development [1]. To date, all cases of cervix hemangiomas described in the literature have shown increasing uterine bleeding symptoms that do not respond to conservative therapy [3].
The majority of these lesions are asymptomatic, but they can occasionally cause aberrant vaginal bleeding and should thus be included in the differential diagnosis of individuals with vaginal bleeding. The microscopic view of the cervical hemangioma in this case showed huge cavernous and capillary-type channels lined by endothelial cells and filled with blood, with some organizing thrombus.
In most cases, surgical therapy is the preferred method. Tanaka et al. [6], on the other hand, showed spontaneous regression of the lesion. In this case, LEEP excision was performed, and the diagnosis was confirmed through histological testing.
In histology, they are made up of dilated blood vessels lined by ordinary endothelial cells with no unusual mitoses. Adventitial fibrosis can cause thickening of the vascular walls. Calcifications are also possible. If there is a benign lesion with a vascular component of reactional character, such as a pyogenic or botryomycosis granuloma, a differential histological diagnosis can be performed. However, the polyploidy of the lesion, its welldefined lobules, and the presence of a substantial inflammatory infiltrate all argue in favor of the lesion’s reactionary nature [6].
Reggiani L et al. [7] present three cases of cervical hemangioma in asymptomatic women, two of which were identified as cavernous hemangiomas and one as capillary hemangiomas. CD31, CD34, and factor-VIII-related antigens were all immunoreactive in all malignancies. There was evidence of estrogen receptor foci expression. With progesterone receptor antibodies, there were no positives. The presence of estrogen receptors in cervical hemangioma endothelial cells shows that this hormone has a direct role in hemangioma development. A potential target therapy is mentioned [7].
Case 2
Hemangioma occurs rarely on the cervix. The clinical manifestation varies. In this situation, it could be prolonged contact bleeding. Others may be asymptomatic or have obstetrical issues. The Histopathological
References
- Busca A, Parra-Herran C (2016) Hemangiomas of the uterine cervix: Association with abnormal bleeding and pain in young women and hormone receptor expression. Report of four cases and review of the literature. Pathol Res Pract 212(6): 532-538.
- Gupta R, Singh S, Nigam S, Khurana N (2006) Benign vascular tumors of female genital tract. Int J Gynecol Cancer 16: 1195-1200.
- Elkhateb S, Idrissi MA, Laabadi K, Chbani L, Chaara H, et al. (2011) Cavernous hemangioma of the cervix and pregnancy: A case report. Open J Obstet Gynecol 1(4): 221-225.
- Powell JL, Zwirek SJ, Sankey HZ (1991) Hemangioma of the cervix managed with the Nd: YAG laser. Obstet Gynaecol 78(5 Pt 2): 962-964.
- Mahapatra S, Das BP, Kar A, Das R, Hazra K, Sethy S (2012) A cavernous haemangioma of the uterine cervix during pregnancy. South Afr J Gynaecol Oncol 4(2): 63-65.
- Tanaka N, Tsuda M, Samura O, Miyoshi H, Hara T, et al. (2007) Blue rubber bleb nevus syndrome: Report of a patient with haemangiomas of the vaginal portion of the cervix appearing during pregnancy. Journal of Obstetrics and Gynaecology Research 33(4): 546-548.
- Reggiani Bonetti L, Boselli F, Lupi M, Bettelli S, Schirosi L, et al. (2009) Expression of estrogen receptor in haemangioma of the uterine cervix: Reports of three cases and review of the literature. Archives of Gynecology and Obstetrics 280(3): 469-472.






























