Early Radiographic and Clinical Outcomes of Five Patients Undergoing Open Instrumented Posterolateral Fusion Surgery with MagnetOsTM Flex Matrix
Ryan Goodmanson*, DO, Casey Butrico, PhD, Katherine Sage, DO
Submission: August 31, 2023; Published: October 02, 2023
*Corresponding author: Ryan Goodmanson, DO, 1231 Pine Grove Ave, Port Huron, MI 48060, USA
How to cite this article: Goodmanson R, Butrico C, Sage K. Early Radiographic and Clinical Outcomes of Five Patients Undergoing Open Instrumented Posterolateral Fusion Surgery with MagnetOsTM Flex Matrix. JOJ Case Stud. 2023; 14(3): 555886. DOI: 10.19080/JOJCS.2023.14.555886.
Abstract
One important factor in obtaining bony fusion in open posterolateral arthrodesis surgery is the bone graft chosen for the procedure. The gold standard is autograft bone in the form of Iliac Crest Bone Graft, but with limited supply and co-morbidities related to harvesting, surgeons have investigated alternative options. One alternative is synthetic calcium phosphate, which is increasingly used in place of autograft because of its efficacy, reasonable cost, low incidence of adverse reactions, and reduced need to harvest large amounts of autologous bone. MagnetOs Flex Matrix is a collagen containing synthetic biphasic calcium phosphate bone graft which harnesses the power of osteoimmunology through its NeedleGripTM surface topography. This surface topography polarizes macrophages to the M2 pro-healing phenotype, which in turn signals to mesenchymal stem cells to differentiate to osteoblasts and promote bone growth. Traditionally, collagen containing bone grafts are made with a tightly crosslinked type one collagen that takes 6-8 weeks to resorb once implanted. Kuros Biosciences invented MagnetOs Flex Matrix with an open fibrillar network of type one collagen made to reduce the collagen resorption time and increase the surface area of the bone graft. An open fibrillar collagen allows the surface features of the MagnetOs Granules to be exposed to the host tissue. This case series reviews five lumbar and cervical posterolateral spinal fusions in a challenging patient population. In each of the cases there was evidence of fusion at early timepoints, with radiographic signs including bony bridging, evidence of trabecular bone, and cortical ridges at the fusion site. Additionally, all of the patients reported improvement in patient reported outcome scores when utilizing MagnetOs Flex Matrix.
Keywords: Posterolateral arthrodesis surgery; Bone graft; MagnetOs Flex Matrix; Osteoimmunology
Introduction
One important factor in obtaining a solid fusion in open posterolateral arthrodesis surgery is the bone graft chosen for the procedure. The gold standard is autograft bone in the form of Iliac Crest Bone Graft, but with limited supply and co-morbidities related to harvesting, surgeons have investigated alternative options [1].
Furthermore, recent literature has demonstrated significant variability in autograft due to age, metabolic disease, and other factors [2]. As a result, multiple products have entered the market as an alternative or adjunct to autograft bone. One alternative is synthetic calcium phosphate, which is increasingly used in place of autograft because of its efficacy, reasonable cost, low incidence of adverse reactions, and reduced need to harvest large amounts of autologous bone [3-5]. MagnetOs Flex Matrix is a collagen containing synthetic biphasic calcium phosphate bone graft which harnesses the power of osteoimmunology through its NeedleGripTM surface topography. This surface topography polarizes macrophages to the M2 pro-healing phenotype, which in turn signal to mesenchymal stem cells to promote bone growth [6-11] *†.
In addition to the benefits of synthetic bone grafts, the variety of handling properties in this category are especially useful for surgeons. Specifically, formulations with collagen are popular because of improved handling capabilities, the ability to lay the graft in long strips in the posterolateral gutter, and the capacity to wick up bone marrow aspirate or blood. Traditionally, these bone grafts are made with a tightly crosslinked, highly woven type-one collagen that takes 6-8 weeks to resorb. Because of this, Kuros Biosciences investigated the use of collagen with an open, fibrillar network as opposed to a tightly crosslinked network (See Figure 1). By using an open fibrillar network, the surface features of the MagnetOs Granules obtain immediate contact with host tissue, thereby polarizing M2 macrophages and signaling to mesenchymal stem cells to promote bone growth. Additionally, in laboratory testing against other collagen products, MagnetOs Flex Matrix demonstrated greater wickability, a high granule to volume percentage which means less shedding of granules, and a flexible structure which is not brittle when dry and retains its structural properties when wet [6].

The purpose of this case series is to assess time to and efficacy of radiographic success, functional outcomes, and pain scores following on-label use of MagnetOs Flex Matrix in an open posterolateral fusion case series.
Case 1
A 51-year-old female with a history of low back pain and lower extremity radiculopathy presented with a VAS score of 10. Her past surgical history included a cholecystectomy and a previous L4-L5 lumbar fusion. Her past medical history included asthma, fibromyalgia, gastroesophageal reflux disease, hyperlipidemia, and seizures. The patient underwent an open posterolateral lumbar L3-S1 revision decompression and fusion using MagnetOs Flex Matrix and autograft and experienced no complications post-operatively. The patient had significant improvement post-operatively with resolution of symptoms and a post-operative VAS score of 4. Furthermore, at 12-weeks post-operatively, x-ray images show consolidation of MagnetOs Flex Matrix and fusion of the posterolateral fusion components with hardware in good position and anatomic alignment of the lumbar spine. See Radiographic Image Series 1 for radiographic details of this case.
Radiographic Image Series 1
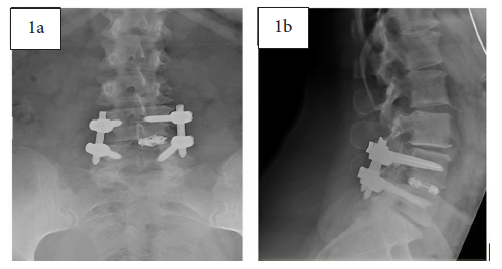
Pre-operative anterior-posterior (AP) (1a) and lateral (1b) x-rays demonstrating previous L4-L5 arthrodesis with instrumentation intact and evidence of pseudoarthrosis. There is adjacent segment disease at L3-L4 and L5-S1.

Pre-operative Computed Tomography (CT) Myelogram (1c and 1d).
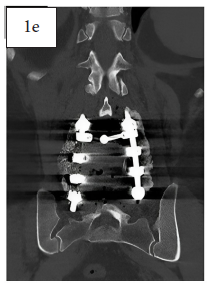
Immediate post-operative coronal CT (1e) showing revision surgery and early granular appearance of MagnetOs Flex Matrix in the posterolateral gutters bilaterally.

Two-week post-operative AP (1f) and lateral (1g) x-rays demonstrating reduced granularity and early signs of fusion.
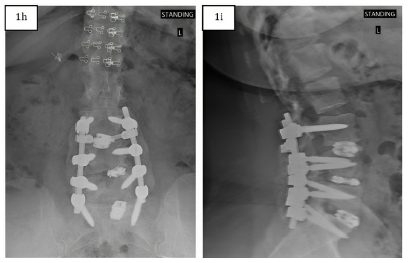
Twelve-week post-operative AP (1h) and lateral (1i) x-rays showing consolidation and resorption of MagnetOs Flex Matrix with remodeling of the bony fusion site.
Case 2
A 64-year-old male with a history of low back pain and lower extremity radiculopathy presented with a VAS score of 9. His past surgical history included a cervical fusion and prostatectomy. His past medical history included hypertension, hyperlipidemia, osteoarthritis, prostate cancer, gastroesophageal reflux disease, chronic obstructive pulmonary disease, and gastrointestinal bleed. The patient underwent an open posterolateral lumbar L4-S1 decompression and fusion using MagnetOs Flex Matrix and autograft, as well as an interbody fusion. There were no complications post-operatively. The patient had significant improvement with resolution of symptoms and a VAS score of 5 at two-weeks post-operatively. The patient had post-operative imaging which showed consolidation and fusion at the fusion site six-months post-operatively. See Radiographic Image Series 2 for radiographic details of this case.
Radiographic Image Series 2

Pre-operative MRI (2a) and CT (2b) demonstrating grade 3 spondylolisthesis at L4-L5 with degeneration and flattening of the L5 vertebra.
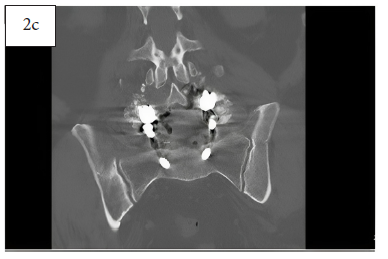
Immediate post-operative coronal CT image (2c) showing MagnetOs Flex Matrix in the posterolateral gutters.
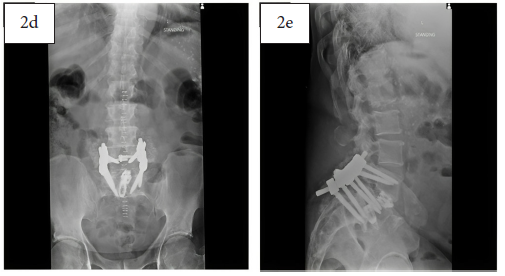
Two-week post-operative AP (2d) and lateral (2e) x-rays demonstrating reduced granularity and early signs of fusion with MagnetOs Flex Matrix in the posterolateral gutters.
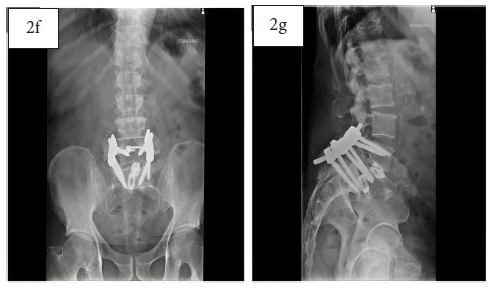
Twelve-week post-operative AP (2f) and lateral (2g) x-rays show consolidation and resorption of MagnetOs Flex Matrix with remodeling of the bony fusion site.
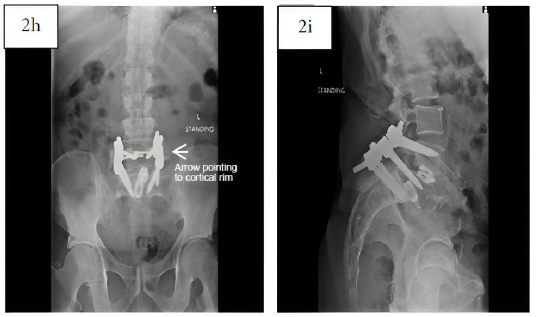
Six-month post-operative AP (2h) and lateral (2i) x-rays show posterolateral arthrodesis with trabecular bone at the posterolateral gutters and a cortical rim, indicative of solid bony fusion.
Case 3
A 73-year-old female with a history of low back pain, lower extremity radiculopathy, and weakness presented with a VAS score of 10. Her past surgical history included total knee arthroplasty. Her past medical history included hypertension, hyperlipidemia, mood disorder, scleroderma, and chronic anemia. The patient underwent an open posterolateral decompression and fusion at L4-S1 using MagnetOs Flex Matrix and autograft, and the patient experienced no complications post-operatively. The patient had significant improvement post-operatively with a resolution of symptoms and an improvement in VAS score to a 3. X-ray imaging at 12-weeks post-operatively demonstrated a fusion bridge with bone remodeling and graft resorption, coupled with trabecular structure and loss of granular appearance at the fusion site. See Image Series 3 for radiographic details of this case.
Radiographic Image Series 3
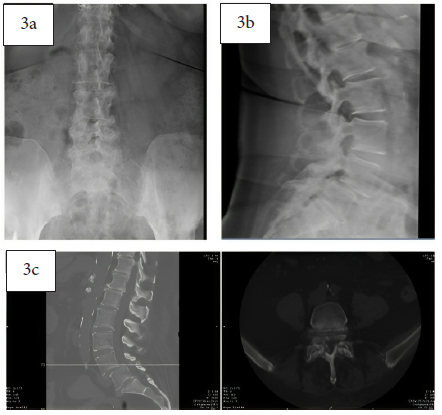
Pre-operative AP (3a) and lateral (3b) x-rays and pre-operative CT (3c) demonstrating grade 2 spondylolisthesis at L4-L5 with diffuse lumbar degenerative changes.
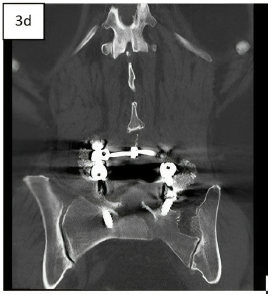
Immediate post-operative coronal CT images (3d) showing a granular appearance of MagnetOs Flex Matrix in the posterolateral gutters.
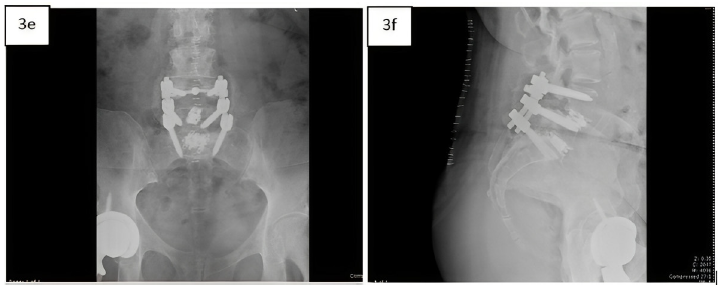
Two-week post-operative AP (3e) and lateral (3f) x-rays demonstrating reduced granularity and early signs of fusion with reduction of the spondylolisthesis.
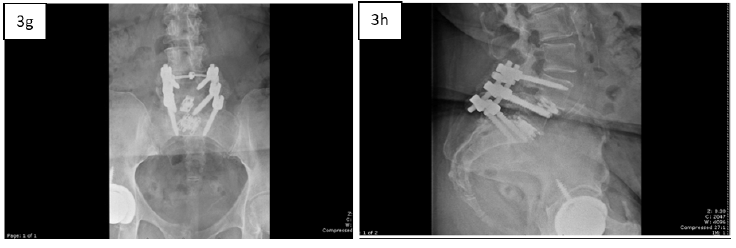
Twelve-week post-operative AP (3g) and lateral (3h) x-rays showing consolidation and resorption of MagnetOs Flex Matrix with remodeling of the bony fusion site.
Case 4
A 61 year-old male with a history of low back pain, lower extremity radiculopathy, and weakness presented with a VAS score of 10. His past surgical history included a cervical arthrodesis and bilateral knee arthroscopy. His past medical history included hypertension, hyperlipidemia, gastroesophageal reflux disease, diabetes mellitus type 2, chronic obstructive pulmonary disease, and pulmonary fibrosis. The patient underwent an open posterolateral fusion and decompression from T10-pelvis using MagnetOs Flex Matrix and autograft. He experienced no complications post-operatively. The patient had significant improvement after surgery with a resolution of symptoms and an improvement in VAS score to a 3. X-ray imaging at 5-months post-operatively demonstrated a fusion bridge with bone remodeling and graft resorption, coupled with trabecular structure and loss of granular appearance at the fusion site. See Image Series 4 for radiographic details of this case.
Radiographic Image Series 4

Pre-operative AP (4a) and lateral (4b) x-rays and pre-operative MRI (4c) demonstrating significant arthritic changes with degenerative disc disease, cord compression, and loss of lumbar lordosis.
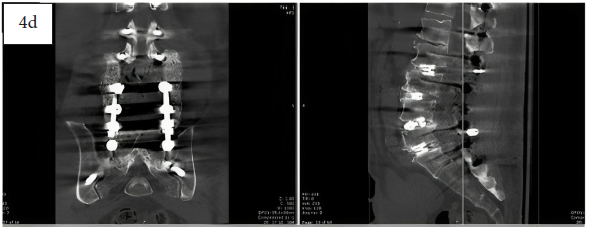
Immediate post-operative CT showing MagnetOs Flex Matrix in the posterolateral gutters (4d).
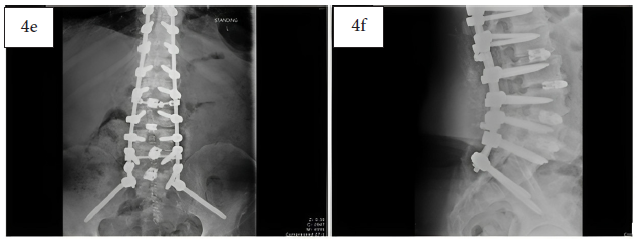
Two-week post-operative AP (4e) and lateral (4f) x-rays showing MagnetOs Flex Matrix in the posterolateral gutters. The granular appearance is fading as bone forms at the fusion site.
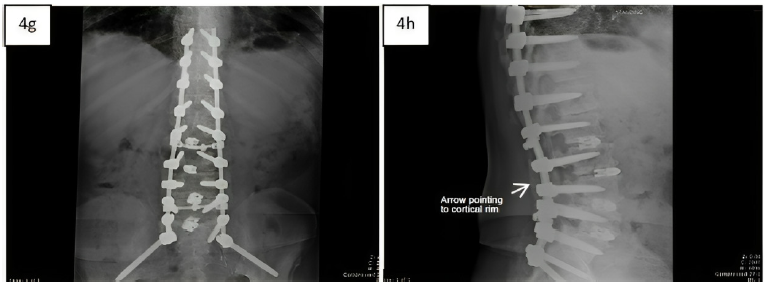
Five-month post-operative AP (4g) and lateral (4h) x-rays showing consolidation of the fusion sites with trabecular bone formation, bridging of the fusion gaps, and a cortical rim.
Case 5
A 62 year-old male with a history of upper extremity weakness, gait instability, myelopathy, and neck pain presented with a VAS score of 8. His past surgical history included a total knee arthroplasty and a knee arthroscopy. His past medical history included gastroesophageal reflux disease, hyperlipidemia, diabetes mellitus type 2, chronic obstructive pulmonary disease, and a hearing disorder. The patient underwent an open anterior C3-C6 discectomy and fusion with a posterior C2-T2 decompression and fusion. MagnetOs Flex Matrix and autograft were used for the posterior portion of the case. The patient experienced no complications post-operatively. The patient had significant improvement after surgery with a resolution of symptoms . X-ray imaging at 12 months post-operatively demonstrated a fusion bridge with bone remodeling and graft resorption, coupled with trabecular structure and loss of granular appearance at the fusion site. See Image Series 5 for radiographic details of this case.
Radiographic Image Series 5
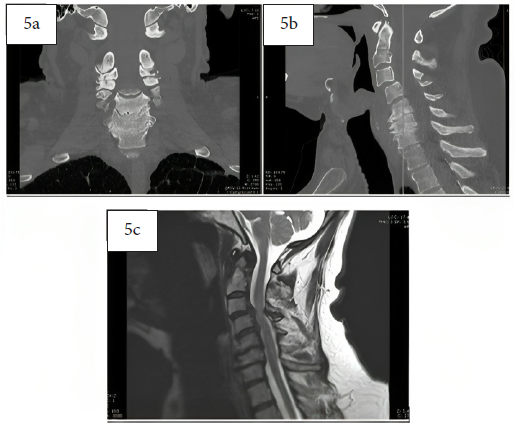
Pre-operative coronal (5a) and sagittal (5b) CT scans and pre-operative MRI (5c) demonstrating a cervical spine with disc degeneration, bony arthritic changes, cord compression at multiple levels, and loss of cervical lordosis.

Immediate post-operative CT scan (5d) showing the granular appearance of MagnetOs Flex Matrix in the posterolateral gutters bilaterally.

Six-week post-operative AP (5e) and lateral (5f) x-rays showing resorption of the graft and consolidation of the fusion site.
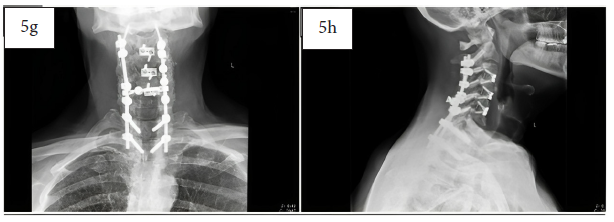
Six-month post-operative AP (5g) and lateral (5h) x-ray images showing solid bony fusion and trabecular bone in the posterolateral gutters.
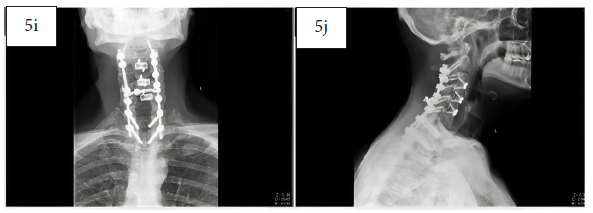
Twelve-month post-operative AP (5i) and lateral (5j) x-ray images showing bony fusion of the arthrodesis sites.
Discussion
Time to fusion is an important consideration in open posterolateral spinal fusion surgery, particularly in patients with multiple co-morbidities and challenges to successful fusion [12]. In the lumbar spine, fusion rates vary based on several factors including approach, instrumentation, patient co-morbidities, levels of arthrodesis, and the bone graft chosen for the case. Several papers have sought to determine how these factors affect the pseudarthrosis rate and revision rates in arthrodesis [13,14].
This case series utilizing MagnetOs Flex Matrix demonstrates rapid predictable evidence of bony fusion in five challenging posterolateral arthrodesis patients with multiple imaging modalities. Throughout these cases, the post-operative imaging shows a consistent remodeling of bone and resorption of the bone graft resulting in trabecular bone formation at the fusion site and loss of granular appearance as early as six weeks. In each case there is early bone formation at the fusion site on imaging, with bony bridging evident in the posterolateral space. Furthermore, this cohort of patients was challenging, with one revision and multiple co-morbidities known to affect fusion outcomes.
Determination of time to fusion is a challenge, with no gold standard for fusion criteria classification, imaging modality, or number of weeks post-operatively to assess fusion status. However, one recent meta-review of bone grafts in posterolateral lumbar fusion reviewed 81 articles with at least one-year radiographic follow up via either x-ray or CT and reported a relatively high range of 80-100% fusion rate at one-year post-operatively. The downside of this meta-review is that the fusion assessments were mainly subjective, biased, and based on x-ray [15]. Conversely, a level one prospective, randomized intra-patient controlled study comparing a synthetic bone graft to autograft in a posterolateral fusion model with independent radiology reviews reported a 55% fusion rate of the synthetic bone graft on CT at one-year postoperatively [16].
MagnetOs Flex Matrix, through its submicron needle-shaped surface topography, provides traction for the body’s vitally important pro-healing immune cells, M2 macrophages [7-9,11]*†. This in turn unlocks previously untapped potential to stimulate stem cells and form new bone throughout the graft [7-9,11]*†. Furthermore, MagnetOs Granules have been shown to form bone in a soft tissue muscle pouch of a large mammal without added cells or growth factors, which is relevant in large bone defects as are found in posterolateral fusion sites [7]. Globally, the MagnetOs bone graft family of products has been implanted in over 15,000 patients.
Conclusion
This case series demonstrates evidence of fusion at early time points, radiographic efficacy, and positive patient reported outcomes of MagnetOs Flex Matrix in a retrospective cohort of challenging patients undergoing posterolateral fusion.
Conflict of Interest
The study was supported by a grant from Kuros Biosciences BV. RG is a consultant for Kuros Biosciences BV. KS and CB have has financial disclosures with Kuros Biosciences BV.
*Results from in vivo laboratory testing may not be predictive of clinical experience in humans. For important safety and intended use information please visit kurosbio.com.
†MagnetOs is not cleared by the FDA as an osteoinductive bone graft.
References
- Radcliff K, Hwang R, Hilibrand A, Smith HE, Gruskay J, et al. (2012) The effect of iliac crest autograft on the outcome of fusion in the setting of degenerative spondylolisthesis: a subgroup analysis of the Spine Patient Outcomes Research Trial (SPORT). J Bone Joint Surg Am 94(18): 1685-1692.
- Park DK, Roberts R, Arnold P, Kim DH, Sasso R, et al. (2019) Lumbar Spine Fusion Rates With Local Bone in Posterolateral and Combined Posterolateral and Interbody Approaches. J Am Acad Orthop Surg 3(11): e018.
- Burger EL, et al. (2007) Orthopedics 30: 939-942.
- Nickoli MS, Hsu WK (2014) Ceramic-based bone grafts as a bone grafts extender for lumbar spine arthrodesis: a systematic review Global Spine J 4(3): 211-216.
- Holmes RE, Mooney V, Bucholz R, Tencer A (1984) A coralline hydroxyapatite bone graft substitute. Preliminary report Clinical Orthopedics and Related Research 188: 252-262.
- Kucko N, et al. (2022) Evaluation of a calcium phosphate-collagen matrix bone graft with needle-shaped submicron surface topography in a clinically relevant sheet posterolateral lumbar spine fusion model. Presented at the North American Spine Society Annual Meeting. October 12-25, 2022. Chicago, IL.
- Duan R, van Dijk LA, Barbieri D, de Groot F, Yuan H, et al. (2019) Accelerated bone formation by biphasic calcium phosphate with a novel sub-micron surface topography. Eur Cell Mater 37: 60-73.
- Van Dijk LA, de Groot FB, Rosenberg AJW, Pelletier M, Christou C, et al. (2020) MagnetOs, Vitoss, and Novabone in a Multi-endpoint Study of Posterolateral Fusion: A True Fusion or Not? Clin Spine Surg 33(6): E276-E287.
- Van Dijk LA, Duan R, Luo X, Barbieri D, Pelletier M, et al. (2018) Biphasic calcium phosphate with submicron surface topography in an Ovine model of instrumented posterolateral spinal fusion. JOR Spine 1(4): e1039.
- Van Dijk LA, Barbieri D, de Groot FB, Yuan H, Oliver R, et al. (2019) Efficacy of a synthetic calcium phosphate with submicron surface topography as autograft extender in lapine posterolateral spinal fusion. J Biomed Mater Res Part B: Appl Biomater 107(6): 2080-2090.
- Van Dijk LA, de Groot F, Yuan H, Campion C, Patel A, et al. (2021) From benchtop to clinic: a translational analysis of the immune response to submicron topography and its relevance to bone healing. eCM 41: 756-773.
- Whitmore RG, Stephen J, Stein SC, Campbell PG, Yadla S, et al. (2012) Patient comorbidities and complications after spinal surgery: a societal-based cost analysis. Spine 37(12): 1065-1071.
- Manzur M, Virk SS, Jivanelli B, Vaishnav AS, McAnany SJ, et al. (2019) The rate of fusion for stand-alone anterior lumbar interbody fusion: a systematic review. Spine J 19(7): 1294-1301.
- Levin JM, Tanenbaum JE, Steinmetz MP, Mroz TE, Overley SC (2018) Posterolateral fusion (PLF) versus transforaminal lumbar interbody fusion (TLIF) for spondylolisthesis: a systematic review and meta-analysis. Spine J 18(6): 1088-1098.
- Morris MT, Tarpada SP, Cho W (2018) Bone graft materials for posterolateral fusion made simple: a systematic review. ESJ 27(8): 1856-1867.
- Lehr AM, Oner FC, Delawi D, Stellato RK, Hoebink EA, et al. (2020) Efficacy of a Standalone Microporous Ceramic Versus Autograft in Instrumented Posterolateral Spinal Fusion: A Multicenter, Randomized, Intrapatient Controlled, Noninferiority Trial. Spine 45(14): 944-951.






























