Uterine Scar Ectopic Pregnancy – A Rare Case of Misdiagnosis Reflecting Changes in Contemporary Obstetric Practice
Shahnaz Aali*, Ayman Aboda, Eissara Punyapati, Carmen Brown, Ghazala Irshad and Brian McCully
Department of Obstetrics & Gynaecology, Mildura Base Public Hospital, Mildura VIC 3500, Australia.
Submission: July 05, 2022; Published: July 14, 2022
*Corresponding author: Dr Shahnaz Aali, Department of Obstetrics & Gynaecology, Mildura Base Public Hospital, Mildura VIC 3500, Australia
How to cite this article: Shahnaz A, Ayman A, Eissara P, Carmen B, Ghazala I, et al. Uterine Scar Ectopic Pregnancy – A Rare Case of Misdiagnosis Reflecting Changes in Contemporary Obstetric Practice. JOJ Case Stud. 2022; 13(5): 555871. DOI: 10.19080/JOJCS.2022.13.555871.
Abstract
Caesarean scar and cervical ectopic pregnancies are rare but life-threatening complications of early pregnancy. Diagnosis may be difficult, particularly in discerning one from the other, as both may share early clinical and ultrasonographic features. Although treatment strategies are similar at the early stage of management, pathways of care soon diverge, which means the correct diagnosis is crucial to ensure the most appropriate decisions for ongoing decision-making. We present a caesarean scar ectopic case, initially diagnosed as early cervical pregnancy. The case highlights the difficulty that may confound the critical distinction between these two early presentations of pregnancy complication. It goes on to describe successful management using single dose systemic methotrexate despite variance with standard treatment protocols. Finally, we present a hypothesis to explain why diagnostic ambiguity may relate to current trends of best obstetric practice.
Keywords: Ectopic pregnancy; Scar ectopic; Cervical ectopic; Caesarean section; Obstructed labour; Maternal morbidity
Introduction
Ectopic pregnancy (EP) accounts for nearly 4 per cent of all pregnancy-related deaths in the first trimester. It is a leading cause of maternal mortality despite improved clinical and diagnostic strategies to promote detection and early access to treatment [1]. Cervical and caesarean scar ectopics are the rarest of such pregnancies. In the former, implantation occurs within the endocervical canal. In scar ectopics, the pregnancy develops at the site of a previous uterine incision, most commonly from a prior Caesarean section but also from other transmural procedures such as hysterotomy.
Cervical pregnancy (CP) accounts for less than 1% of EPs, with an incidence of approximately 1/8628 to 1/10000 of all pregnancies [2]. It may be associated with catastrophic haemorrhage, mainly if there is delay or uncertainty in either diagnosis or treatment. The maternal outcome may be grievous, including high mortality rates or significant residual morbidity, such as emergency hysterectomy [3]. Caesarean scar pregnancies (CSP) are somewhat more common, accounting for nearly 4% of all EPs. They often arise following operative delivery, complicating approximately 1 in 500 caesarean births [4]. With little surprise, the rising incidence of caesarean deliveries worldwide has been associated with an increased predictive risk of future CSPs. As with CP, maternal outcomes depend on diagnosis; the earlier, the better. If unrecognized or delayed, sequelae may include uterine rupture, major haemorrhage, and emergency hysterectomy [5].
The distinction between a CP and a CSP may remain challenging, particularly when implantation occurs low at the isthmic-cervical junction [6]. This may confuse definitive diagnosis leading to either delay or misdirection of effective management. Fortunately, there has been significant progress in diagnosing EP with the routine use of early surveillance transvaginal ultrasound (TVUSS) in pregnancy. We report the case of a woman who presented with transvaginal bleeding and abdominal pain in early pregnancy. Clinical examination, blood workup and diagnostic imaging, including TVUSS, suggested the diagnosis of cervical ectopic with evidence of foetal heart activity. Five days after standard treatment with a single dose of systemic methotrexate, it became apparent that the ectopic was in a previous caesarean scar. We hypothesize that the misidentification was because of an unusually low incision from the previous surgery, which was conducted at full dilatation in the setting of obstructed labour. Nonetheless, the patient responded well to the treatment regime, suggesting that a single dose of systemic methotrexate may be successful even in the presence of fetal cardiac activity and may be recommended as first-line management for CSP and CP.
Case Presentation
A 43-year-old woman, G4P2M1, presented to the emergency department (ED) with vaginal bleeding and lower abdominal pain. She was eight weeks pregnant based on the dates of her last menstrual period. A serum β-hCG was positive at 18,203mIU/mL. Her past obstetric history included two previous caesarean delivery and one miscarriage requiring curettage. On examination, the patient was alert with a GCS of 15 and though uncomfortable, was not acutely distressed. Vital sign assessment showed a stable blood pressure of 114/75mmHg without a postural drop and a heart rate of 75bpm. Her abdomen was soft and non-tender to palpation. Speculum examination demonstrated a small amount of fresh and clotted blood at the vaginal vault. The cervix appeared bulbous and bulky, and the external os was closed. There was no significant pelvic or cervical tenderness on digital examination. Ultrasound imaging (TVUSS) demonstrated a 6weeks pregnancy with foetal cardiac activity in the extreme lower segment of the uterus and upper cervical region (Figure 1).
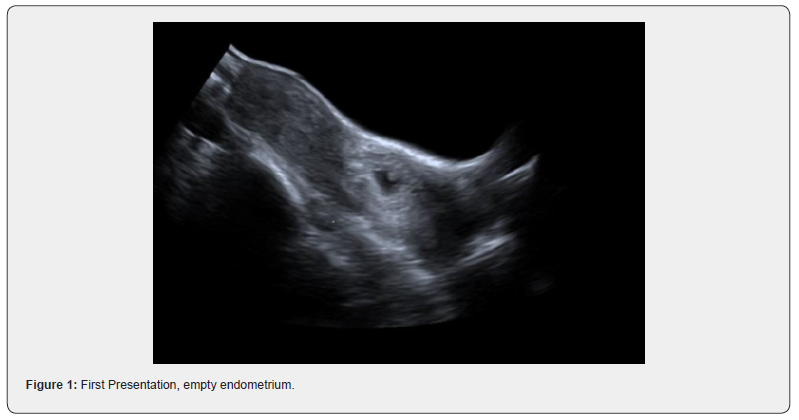
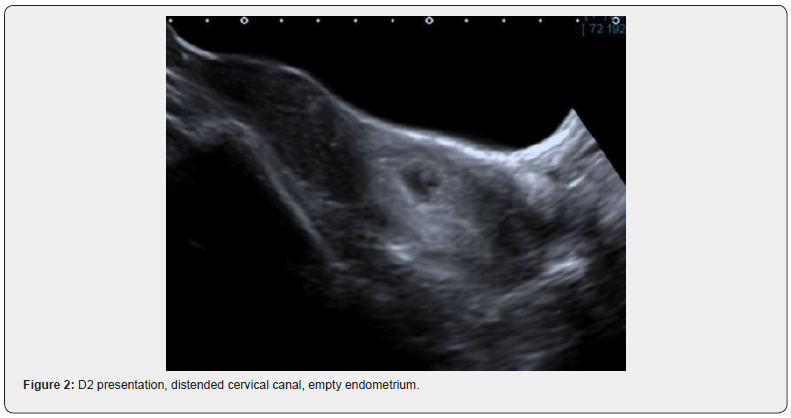
Expectant care was recommended pending a repeat ultrasound examination. Two days later, the ultrasound reported persistence of gestation sac with yolk sac and foetal pole with cardiac activity confirming ongoing viability. The pregnancy sac appeared to be in the upper cervical canal. The cervix appeared diffusely expanded and heterogeneous, indicating a haematoma surrounding the sac. These appearances were consistent with a diagnosis of cervical ectopic pregnancy with some evidence of early rupture or chorionic bleed (Figure 2).
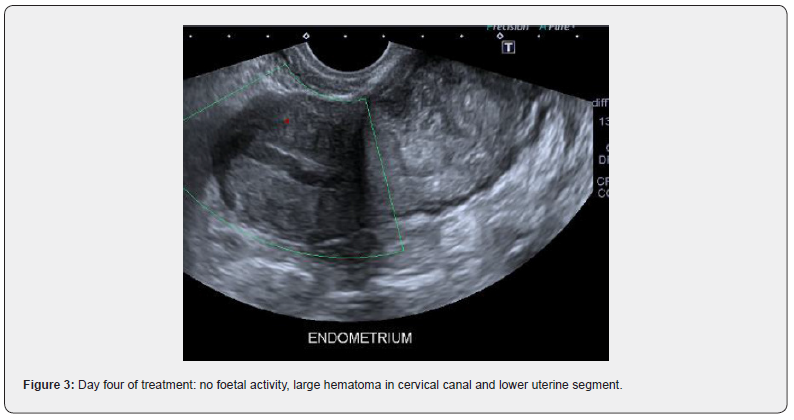
The patient was admitted for observation. A single dose of intramuscular methotrexate was administered the next day. The bleeding subsided, and she was discharged with a plan to repeat serial β-hCG levels on days four and seven, with a repeat ultrasound in one week. Unfortunately, the patient presented with further vaginal bleeding and increased lower abdomen pain four days later. The β-hCG was 16,622mIU. Repeat ultrasound revealed a large, heterogeneous avascular area consistent with haematoma, which spanned the cervix and measured 74 x 50 x 39mm. The gestational sac was still evident; however, cardiac activity had ceased (Figure 3).
On day 7, β-hCG dropped to 14,494 and continued to decline steadily to less than five mIU/mL at six weeks. The patient was re-admitted and transferred for tertiary hospital review the following day. A subsequent scan by a sub-specialty practitioner (Certificate in Obstetrics & Gynaecology Ultrasound COGU) demonstrated a collapsed gestational sac within a previous caesarean scar, extending through the myometrium to within 3mm of the anterior serosal surface. The findings were consistent with a satisfactory response to current medical management. Adjunctive surgical intervention was not required. The patient's symptoms improved with continued expectant support, and she was discharged to await the results of further β-hCG tracking.
Discussion
An ectopic scar pregnancy is onerous to diagnose. It occurs in approximately 1 in 2000 pregnancies 8. However, in up to 13.6 per cent of cases, the diagnosis will be either missed or confused with other conditions of early pregnancy failure such as cervical ectopic pregnancy, spontaneous miscarriage or low intrauterine implantation. There are two types of CSP, Endogenic, which means “of the scar” and includes those where growth occurs towards the uterine cavity, and exogenic or “of the niche", where growth is towards the bladder and abdominal cavity and is associated with a much greater risk of scar rupture with intra-abdominal bleeding. In these cases, early detection is vital to decrease the burden of catastrophic complications [9]. As expected, CSP usually presents in patients with a known previous caesarean delivery or other uterine surgery such as a hysterotomy. While vaginal bleeding and abdominal pain are frequent harbingers of disease, it is essential to note that nearly one-third will be asymptomatic at the time of ultrasound diagnosis [10].
Curiously, cervical ectopic pregnancy may share similar origins. Previous caesarean sections have been implicated, but more commonly, procedures such as dilatation and curettage, particularly if associated with Asherman's syndrome, prior cervical surgery and embryo transfer procedures of in vitro fertilization [11]. Patients with cervical pregnancy may present with painless first trimester vaginal bleeding. Occasionally, when associated with early cramping pain, the diagnosis may be confused with spontaneous miscarriage. On examination, findings include a soft distended cervix which is disproportionally enlarged compared to the uterus, a partially opened external cervical os and a likelihood of haemorrhage following manipulation of the cervix [12].
Identification of a pregnancy sac at the site of a caesarean scar is diagnostic of CSP [7]. In contrast, a gestational sac in the cervix with an intact portion of the cervical canal between it and the lower uterine endometrium is diagnostic of CP [13]. Our case report presents a patient for whom the early diagnosis was mistaken. She had a history of two previous caesarean section deliveries and one miscarriage, all of which may predispose risk for either condition. Vaginal bleeding and abdominal pain were present. Ultrasound examination revealed an empty uterine cavity and a distended cervical canal containing a gestational sac consistent with a CP. Subsequently, a more detailed examination changed the diagnosis and correctly identified a CSP. To this conundrum, we offer the following possible explanation. An ectopic scar pregnancy will develop in the scar of previous surgery. The location of this scar may vary. In the case of a caesarean section, the scar is usually approximated high in the lower uterine segment to keep it distanced from the bladder. We suggest that in obstructed labour, particularly when the cervix is fully dilated, the tissues of the upper cervix and lower uterine segment may be so distended that they merge. When this occurs, the transverse incision of delivery may be much lower than expected, traversing upper cervical tissue.
Our case reports an unexpected complication of such surgery. The ectopic was developing in the cervix; we did not realize that the previous caesarean scar was also in this region.
In general, management decisions for CSP and CP are affected by the gestational age of the pregnancy, the stability of the patient, evidence of rupture and viability, the patient’s desires for future fertility, and perhaps, most importantly, the resources and expertise of the care providers treating the patient. There is no single guideline of best care [7,14-16]. Choices may include systemic or intra-lesion methotrexate or surgical intervention. Based on Green-top Guidelines, medical management with methotrexate is considered most appropriate for cervical pregnancy. There is, however, less available evidence to recommend its efficacy when caesarean scar pregnancy is suspected. In this setting, current recommendations suggest a surgical rather than medical approach. Whilst we are grateful, we acknowledge reports from authors such as Drever and Bodie et al. [16,17] who caution that patients with CSP are most likely to encounter treatment failure using systemic methotrexate when foetal heart activity is present and β-hCG levels greater than 12,000 [16,17]. This is significant because it means that, in our case, surgical management would have been the most appropriate choice of care. Fortunately, however, treatment was successful, and our patient went on to enjoy a complete recovery.
Conclusion
The diagnosis of CP and CSP can be challenging to differentiate. We highlight a case where previous decision-making for a caesarean section may have contributed to this ambiguity. This is important because it highlights a potential consequence of current trends to avoid or delay operative deliveries. We speculate that greater tolerance of obstructed labour may lead to an excessive stretch of lower uterine and pelvic tissues such that a lower segment incision may inadvertently impinge the cervix. If later complicated by ectopic pregnancy, diagnosis may be misdirected because of the unexpectedly low position of the previous scar. This error may then lead to an incorrect choice of the best treatment. Fortunately for us, clinical outcome was not adversely affected. We propose that with greater awareness of complications that may follow operative delivery for obstructed labour, an improved differential diagnosis between scar and cervical ectopic pregnancy may be possible.
References
- Creanga A, Shapiro Mendoza CK, Bish CL, Zane S, Berg CJ, et al. (2011) Trends in ectopic pregnancy mortality in the United States: 1980-2007. Obstet Gynecol 117(4): 837-843.
- Elmokadem AH, Abdel Wahab RM, El Zayadi AA, Elrakhawy MM (2019) Uterine Artery Embolization and Methotrexate Infusion as Sole Management for Cesarean Scar and Cervical Ectopic Pregnancies: A Single-Center Experience and Literature Review. Can Assoc Radiol J 70(3):307-316.
- Dziedzic JM, Patel PV (2019) Cervical ectopic pregnancy: a rare site of implantation. J Emerg Med 56(6): e123-e125.
- Diakosavvas M, Kathopoulis N, Angelou K, Chatzipapas I, Zacharakis D, et al. (2022) Hysteroscopic treatment of Cesarean Scar Pregnancy: A systematic review. Eur J Obstet Gynecol Reprod Biol 270: 42-49.
- Rivera-Rodríguez AJ, Zarazúa OJ, Bermúdez LAC, Ramírez LNV, Ciocca OCC (2019) A case report of a misdiagnosed cesarean scar pregnancy in a hemodynamically compromised patient. Human Pathology: Case Reports 18: 200344.
- Rizk B (2010) Ultrasonography in reproductive medicine and infertility.
- Timor Tritsch I, Monteagudo A (2012) Unforeseen consequences of the increasing rate of cesarean deliveries: early placenta accreta and cesarean scar pregnancy. A review. Am J Obstet Gynecol 207(1): 14-29.
- Rotas M, Haberman S, Levgur M (2006) Cesarean scar ectopic pregnancies: etiology, diagnosis, and management. Obstet Gynecol 107(6): 1373-1381.
- Jameel K, Mannan GA, Niaz R, Hayat D (2021) Cesarean Scar Ectopic Pregnancy: A Diagnostic and Management Challenge. Cureus 13(4): e14463.
- Berhie SH, Molina RL, Davis MR, Anchan RM, Wang KC (2015) Beware the scar: Laparoscopic hysterectomy for 7-week cesarean delivery scar implantation pregnancy. Am J Obstet Gynecol 212(2): 247.e1-247.e2.
- Eblen A, Pridham D, Tatum CM (1999) Conservative management of an 11-week cervical pregnancy. A case report. J Reprod Med 44(1): 61-64.
- Leeman LM, Wendland CL (2000) Cervical ectopic pregnancy: diagnosis with endovaginal ultrasound examination and successful treatment with methotrexate. Arch Fam Med 9(1): 72-77.
- Rizk B, Holliday CP, Owens S, Abuzeid M (2013) Cervical and cesarean scar ectopic pregnancies: Diagnosis and management. Middle East Fertility Society Journal 18(2): 67-73.
- Heidar Z, Modarres SZ, Abediasl Z, Khaghani A, Salehi E, et al. (2021) Cesarean scar pregnancy treatment: a case series. J Med Case Rep 15(1): 506.
- Agarwal N, Gainder S, Chopra S, Rohilla M, Prasad G, et al. (2021) The Management of Scar Ectopic: A Single-Center Experience. Cureus 13(6): e15881.
- Bodur S, Özdamar O, Kiliç S, Gün I (2015) The efficacy of the systemic methotrexate treatment in caesarean scar ectopic pregnancy: A quantitative review of English literature. J Obstet Gynaecol 35(3): 290-296.
- Drever N, Bertolone J, Shawki M, Janssens S (2020) Caesarean scar ectopic pregnancy: Experience from an Australian tertiary centre. Aust New Zeal J Obstet Gynaecol 60(3): 330-335.






























