Abstract
The use of intensity-modulated radiotherapy treatment (IMRT) to treat various tumour sites has gained wider publicity in recent years due to its ability to decrease the radiation dose to adjacent organs [1]. The small bowel can be irradiated when treating the pelvis. Acute and late radiation-induced toxicity to the small bowel has been reported when radiotherapy dose to small bowel threshold is exceeded [2]. It has been suggested that absolute volume of small bowel receiving ≥ 15 Gy should be held to, 120 cc to minimise acute toxicity, when delineating the contours of bowel loops. If the entire volume of bowel bag is contoured then the volume receiving > 45 Gy should be < 195 cc [3]. Various manoeuvres have been implemented to reduce the doses to organs at risk (OAR), such as the small intestine. IMRT has been shown to reduce to radiotherapy dose to small bowel compared to 3- dimensional conformal radiotherapy (3D-CRT) [4,5]. Prone positioning on belly board has been shown to decrease radiotherapy dose to the small bowel in gynaecologic pelvic IMRT [6]. Prone position on belly board has also been shown to reduce radiotherapy dose to small bowel during in prostate pelvic IMRT as well [7]. Another way to reduce radiotherapy dose to small bowel is to insert intra-pelvic tissue expander [8]. Mesh slings insertion also has been used to reduce radiotherapy dose to small bowel [9].
Keywords: Radiotherapy; Prostate cancer; pelvic IMRT; Bladder
Introduction
Distended bladder was found to be more effective than belly board device to reduce the volume of irradiated small bowel in patients receiving conformal pelvic radiotherapy [10]. A retrospective study reported that empty bladder increases radiotherapy dose to small bowel in patients receiving gynaecologic pelvic IMRT [11]. Prostate cancer patients are instructed to have a full bladder prior radiotherapy to reduce small bowel radiotherapy dose. Compliance can be difficult to achieve in older population who already have pre-existing prostate conditions. It is remaining an open question whether adapting IMRT to treat prostate cancer does not require to have a full bladder. In this study, we aim to evaluate the effect of bladder filling on dose distributions for the small intestine as measured by V20, V30, V40 and V50.
Materials and Methods
A waiver of authorization was obtained from the Institutional Review Board, and clinical data of 60 prostate cancer patients treated with radiotherapy in 2016 at our institution were retrospectively reviewed. All patients had tissue diagnoses of prostate adenocarcinoma, confirmed by cytologic or pathologic review at our institution. All cases were identified with medical record number (MRN). Data was collected using a combination of an electronic database, case notes. Radiation records were obtained for all patients from Eclipse treatment planning system (Eclipse TPS). We collected information on bladder and small bowel volumes, small bowel volume which received 20 Gy (V20), 30 Gy (V30), 40 Gy (V40) and 50 Gy (V50). The minimum dose to the PTV was 95% of the prescribed dose (7400 cGy in 32 fractions). Patients are asked to empty their bladder then drink 3 cups of water within 5 minutes. They hold this in the bladder for at least 30 minutes until the planning scan is complete. Patients who have a catheter were excluded from the study. Patients who had prostatectomy were also excluded. All patients were scanned with a full bladder on supine position. PTV and OAR including small bowel which were countered by 6 different consultant clinical oncologists to reflect day to day practice. Small bowel was contoured as bowel bag. Radiotherapy plans were generated using Intensity-Modulated Radiation Therapy (IMRT). Bladder volumes, dose volume histograms (DVHs) V20, V30, V40 and V50 for small intestine were obtained for each patient. We ran the Spearman’s rho correlation coefficient to measure the strength of the linear relationship between the bladder volume and the dose to the small bowel. we used partial correlation coefficients controlling for small bowel volume.
Results
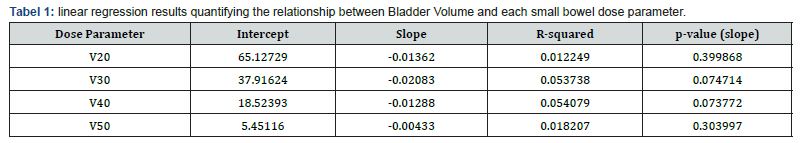
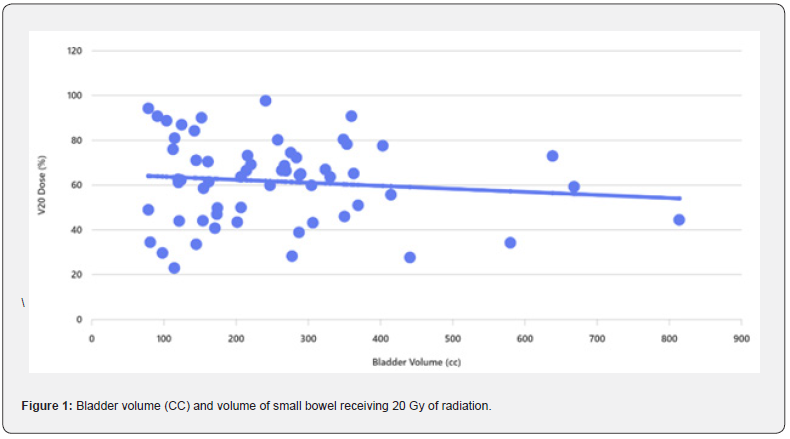
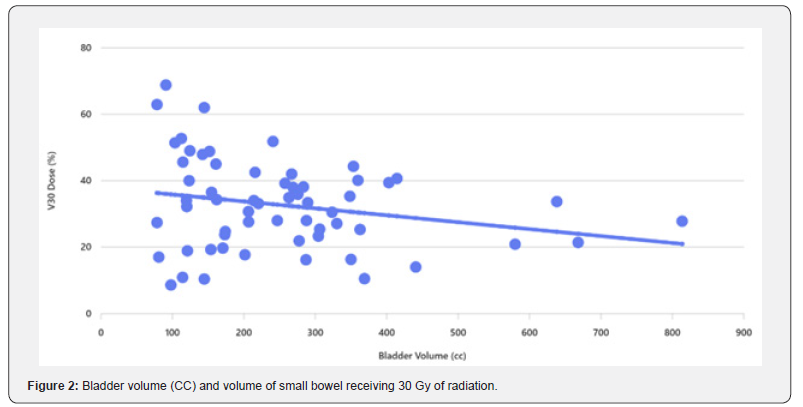
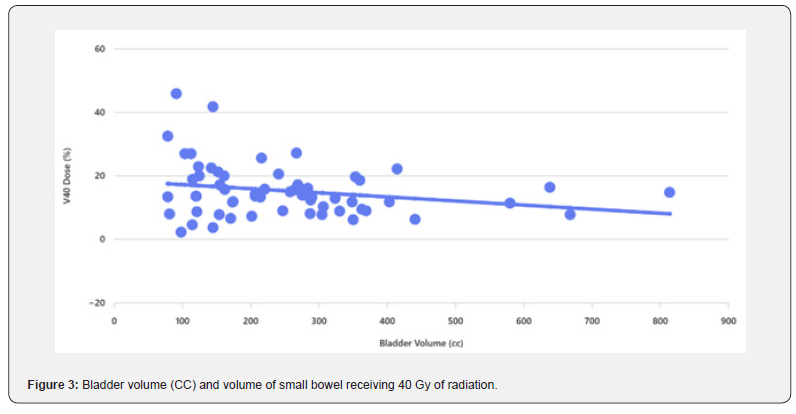
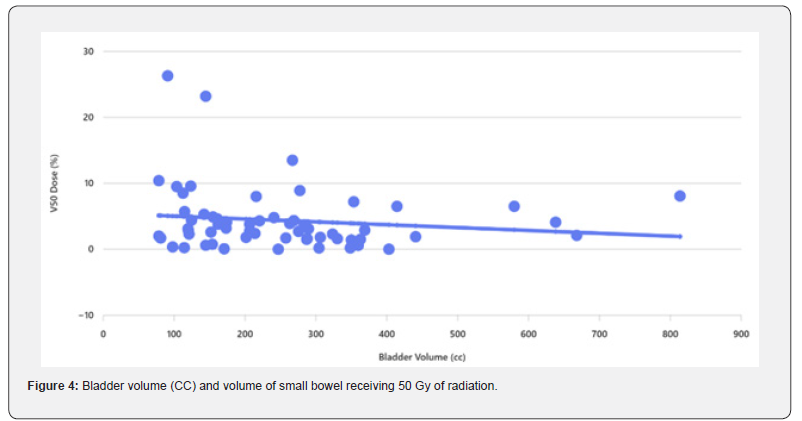
We used partial correlation coefficients controlling for small bowel volume, the results showed that there is inverse correlation between bladder volume and radiotherapy dose to small bowel. The bladder volume increased, V20, V30 and V40 were decreased. The percent variation is just putting the magnitude of effect of the bladder in context. It seems to have a bigger effect on V30 and V40 compared to V20 and V50. There is about 11% of the variation in V30 & V40 which can be explained by bladder volume. The percentage of variation is approximately 5% for V20 & V50. The correlation analysis between Bladder Volume and small bowel dose parameters: V20: -0.1, V30: -0.23, V40: -0.23 and V50: -0.13. This indicates a negative correlation: as bladder volume increases, the dose to the small bowel tends to decrease slightly, especially for higher dose levels (V30 and V40 show the strongest negative correlation).
These results indicate that larger bladder volumes are associated with lower small bowel dose exposure, which aligns with clinical practice where bladder filling can help displace the small bowel out of the high-dose region. The effect is modest but more pronounced for intermediate dose levels (V30 and V40). Tabel 1 showed linear regression which confirmed a negative slope confirm that increasing bladder volume tends to reduce small bowel dose. There was a size effect, for every 1 cc increase in bladder volume. For example, V30 decreases by ~0.021% and V40 by ~0.013% which showed borderline significance (p ≈ 0.075), suggesting a trend but not strong evidence. Furthermore, R² values are low (<0.06), meaning bladder volume explains only a small fraction of dose variability.
Discussion
This study investigated the relationship between bladder volume and radiation dose to the small bowel in patients undergoing pelvic IMRT for prostate cancer. The results demonstrated a general trend: as bladder volume increased, the radiation dose to the small bowel decreased across all measured dose-volume histogram (DVH) parameters (V20, V30, V40, V50). The strongest negative correlations were observed for V30 and V40 (r = -0.23 for both), with V40 approaching statistical significance (p ≈ 0.074), but overall, the correlations did not reach conventional thresholds for significance. The effect was modest, with bladder volume explaining about 11% of the variation in V30 and V40, and approximately 5% for V20 and V50. The observed inverse relationship aligns with the theoretical rationale and prior evidence that bladder distension can displace the small bowel superiorly and out of the high-dose region during pelvic radiotherapy. This effect has been previously described by Kim et al. (2005), who found that a distended bladder was more effective than a belly board device in reducing irradiated small bowel volume during pelvic IMRT. Similarly, another study reported that an empty bladder increased the dose to the small bowel in prostate cancer radiotherapy, underscoring the importance of bladder filling protocols.
Despite these trends, our study’s lack of statistical significance for most DVH parameters suggests that the effect of bladder volume may be more nuanced in clinical practice. Variability in contouring practices, as highlighted by Kavanagh et al. (2010), and differences in patient anatomy or compliance with bladder filling protocols could contribute to the modest correlations observed. Additionally, the retrospective nature of our study and the relatively small sample size (n = 60) may have limited the statistical power to detect significant associations. Previous research has established dose constraints for the small bowel to minimise acute toxicity. Liu et al. (2007) recommended limiting the absolute volume of small bowel receiving ≥15 Gy to 120 cc, while Kavanagh et al. (2010) suggested keeping the volume receiving >45 Gy below 195 cc. Our findings support the continued relevance of these constraints, as increased bladder volume tended to reduce small bowel exposure, particularly at higher dose levels (V30 and V40). The challenge of achieving consistent bladder filling, especially in older patients with prostate conditions, has been noted in the literature and was evident in our cohort. This practical limitation may partially explain the variability in our results and highlights the need for patient-specific approaches to bladder management during radiotherapy.
Several limitations of the study must be acknowledged. First,
the study is a retrospective
a. Design: The retrospective nature of this study
introduces potential biases, such as selection bias and limited
control over protocol adherence. With only 60 patients, the study
may be underpowered to detect subtle but clinically meaningful
associations. The lack of statistical significance may reflect limited
sample size rather than a true absence of effect. There are variability
in Contouring of the small bowel and other OARs were contoured
by six different consultant clinical oncologists, introducing interobserver
variability that could affect dose-volume measurements.
Furthermore, although a standard protocol was used, actual
bladder volumes likely varied due to differences in patient
compliance and physiological factors, potentially diluting the
observed effect. There is also a lack of clinical outcome data. The
study focused on dosimetry parameters without correlating these
with clinical outcomes such as gastrointestinal toxicity, limiting
the ability to assess the clinical significance of the findings.
b. The study is single-center experience: Data were
collected from a single institution, which may limit generalizability.
There is a potential confounding factors like influencing small
bowel dose, such as body mass index, pelvic anatomy, or prior
abdominal surgery, were not controlled for in this analysis. Finally,
all scans were performed in the supine position; alternative
positioning strategies were not evaluated.
The findings suggest that bladder filling protocols can contribute to reducing small bowel dose during pelvic IMRT, but the effect may be modest and subject to individual patient factors. Achieving consistent bladder filling can be challenging, especially in older patients or those with prostate conditions, as noted in both our cohort and previous studies. Therefore, while bladder filling should remain a component of best practice, it should be complemented by other strategies for organ-at-risk (OAR) sparing, such as prone positioning or the use of intra-pelvic tissue expanders. Individualised treatment planning is essential, taking into account patient-specific anatomy and compliance. Advanced imaging and adaptive radiotherapy techniques may further optimise OAR sparing in the future. Future research should address these limitations by employing prospective, multicentre designs with larger sample sizes, standardised contouring protocols, and inclusion of clinical outcome data. Further studies should also explore the interplay between bladder volume, small bowel position, and patient-reported toxicity, as well as the potential benefits of advanced imaging and adaptive radiotherapy.
Conclusion
In Conclusion, this study adds to the evidence that bladder filling can reduce small bowel irradiation during pelvic IMRT, though the effect may be modest and influenced by patientspecific factors. Continued research and individualised patient management are essential to optimise the therapeutic ratio in pelvic radiotherapy.
References
- Meyer J, Richter A, Pfreundner L, Guckenberger M, Krieger T, et al., (2009) An interlaced IMRT technique for elongated tumor volumes. Med Dosim 34: 170-178.
- Liu YM, Shiau CY, Lee ML, Huang PI, Hsieh CM, et al., (2007) The role and strategy of IMRT in radiotherapy of pelvic tumors: Dose escalation and critical organ sparing in prostate cancer. Int J Radiat Oncol Biol Phys 67(4): 1113-1123.
- Kavanagh BD, Pan CC, Dawson LA, Das SK, Li XA, et al., (2010) Radiation dose-volume effects in the stomach and small bowel. Int J Radiat Oncol Biol Phys 76(3 Suppl): S101-7.
- Nutting CM, Convery DJ, Cosgrove VP, Rowbottom C, Padhani AR, et al., (2000) Reduction of small and large bowel irradiation using an optimized intensity-modulated pelvic radiotherapy technique in patients with prostate cancer. Int J Radiat Oncol Biol Phys 48: 649-656.
- Portelance L, Chao KS, Grigsby PW, Bennet H, Low D (2001) Intensity-modulated radiation therapy (IMRT) reduces small bowel, rectum, and bladder doses in patients with cervical cancer receiving pelvic and para-aortic irradiation. Int J Radiat Oncol Biol Phys 51(1): 261-6.
- Adli M, Mayr NA, Kaiser HS, Skwarchuk MW, Meeks SL, et al., (2003) Does prone positioning reduce small bowel dose in pelvic radiation with intensity-modulated radiotherapy for gynecologic cancer? Int J Radiat Oncol Biol Phys 57(1): 230-238.
- Koszo R, Varga L, Fodor E, Kahan Z, Cserhati A, et al., (2019) Prone Positioning on a Belly Board Decreases Rectal and Bowel Doses in Pelvic Intensity-Modulated Radiation Therapy (IMRT) for Prostate Cancer. Pathol Oncol Res 25(3): 995-1002.
- Herbert SH, Solin LJ, Hoffman JP, Schultz DJ, Curran WJ, et al., (1993) Volumetric analysis of small bowel displacement from radiation portals with the use of a pelvic tissue expander. Int J Radiat Oncol Biol Phys 25(5): 885-893.
- Bachmann R, Heinzelmann F, Muller AC, Ladurner R, Schneider CC, et al., (2015) Laparoscopic pelvic mesh placement with closure of pelvic floor entrance to prevent small intestine radiation trauma - A retrospective cohort analysis. Int J Surg 23: 62-67.
- Kim TH, Chie EK, Kim DY, Park SY, Cho KH, et al., (2005) Comparison of the belly board device method and the distended bladder method for reducing irradiated small bowel volumes in preoperative radiotherapy of rectal cancer patients. Int J Radiat Oncol Biol Phys: 62: 769-775.
- Lei C, Ma S, Huang M, An J, Liang B, et al., (2019) Long-Term Survival and Late Toxicity Associated With Pelvic Intensity Modulated Radiation Therapy (IMRT) for Cervical Cancer Involving CT-Based Positive Lymph Nodes. Front Oncol 9: 520.






























