Metastasis Detection and Clinical Significance According to Localization of Resecting Lymph Nodes in Female Reproductive System Cancers
Remzi Arslan1 and Burçin Ergul2
Department of Pathology, Faculty of Medicine, Atatürk University, Turkey
Submission: September 08, 2023; Published: September 11, 2023
*Corresponding author: Remzi Arslan, Department of Pathology, Faculty of Medicine, Atatürk University, Turkey
How to cite this article: Remzi A, Burçin E. Metastasis Detection and Clinical Significance According to Localization of Resecting Lymph Nodes in Female Reproductive System Cancers. J Gynecol Women’s Health 2023: 25(4): 556175. DOI: 10.19080/JGWH.2023.25.556175
Abstract
Introduction and Aim: Female reproductive system cancers (FRSC) are a major cause of morbidity and mortality all over the world, and especially cervical cancers are the 4th most common cancer after breast, lung and colorectal cancers. Ovarian and endometrial cancers have increased in recent years. Regional lymphadenectomy is frequently used during the initial surgery in the treatment of these tumors. Detection of metastases in resected lymph nodes constitutes an important histopathological and clinical prognostic parameter. In our study, it was aimed to investigate the detection of metastases according to localization in resected lymph nodes in FRSC cancers and to investigate its clinical significance.
Methods: In our study, pathological reports including female reproductive system cancers diagnosed at Atatürk University Faculty of Medicine, Pathology Department between January 1, 2010 and November 30, 2021 were retrospectively scanned. The age, organ, tumor type, localization of the resected lymph nodes and metastasis rates in these localizations were determined and compared with the literature.
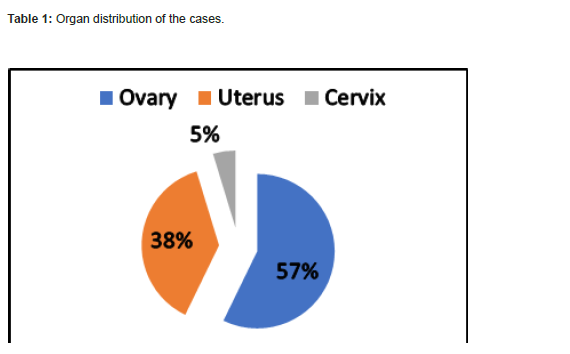
Results: In our study, 152 materials made due to FRSC were evaluated. The mean age of the cases was 56.86, and 87 (57%) of them were localized to the ovary, 58 (38%) of them to the uterus, and 7 (5%) of them to the cervix. Lymph node dissection was performed in 128 (84%) patients with tumor, and not to 24 (16%). In terms of tumor type, serous carcinoma was the first line and endometrioid carcinoma was second line. Metastasis rates were found to be 25% in the resected right pelvic lymph nodes and 23.7% in the left pelvic lymph nodes. Metastasis was detected in 35% of the paraaortic lymph nodes, and the rate was found to be higher.
Conclusion: In our study, regardless of type, it was observed that right and left pelvic node positivity was similar, and paraaortic lymph node metastasis was higher than the others. In assesments based on tumor subtypes, It is important to observe a higher rate of paraaortic and pelvic lymph node involvement in serous carcinomas in terms of guiding the treatment.
Keywords: Endometrial Carcinoma; Serous Carcinoma; Lymph Node; Metastasis
Introduction
Female reproductive system cancers (FRSC) are an important cause of morbidity and mortality all over the world, and according to GLOBOCAN 2020 data, cervical cancer is the fourth most common cancer after breast, lung and colorectal cancers [1]. In our country as well as all over the world, there has been a decrease in invasive cervical cancers in recent years, thanks to widespread cervical smear screening programs. On the other hand, uterine corpus cancers (endometrial cancers) are detected at a higher rate in our country [1]. Cervical cancers are more common at the age of 40-54 years. The mean age of incidence of endometrial cancers is 63 years, 5% of them are under 40 years of age, 20-25% are premenopausal, and 75-80% are postmenopausal. It is seen most frequently in ovarian cancers at the age of 63, and its mortality is higher than that of other female reproductive cancers [2]. In the etiology of tumors, genetically PTEN gene mutations, BRCA1 and BRCA2 mutations, especially Human Papilloma Virus (HPV), have an important role. In addition, smoking, obesity, sexually contagious diseases, various infertility treatments, etc. are among the important etiological causes [3,4]. In these cancers, the involved organ, tumor type, tumor size, depth of invasion, and lymph node involvement are among the most important prognostic parameters [3,4].
Regional lymphadenectomy is frequently used during the initial surgery in the treatment of these tumors. Detection of metastases in resected lymph nodes constitutes an important histopathological and clinical prognostic parameter. This is especially important for clinical staging and chemo-radiotherapy management [5]. In our study, it was aimed to investigate the detection of metastases according to localization in resected lymph nodes in FRSC cancers and to investigate its clinical significance.
Methods
In our study, pathological reports including female reproductive system cancers diagnosed at Atatürk University Faculty of Medicine, Pathology Department between January 1, 2010 and November 30, 2021 were retrospectively scanned. The age, organ, tumor type, localization of the resected lymph nodes and metastasis rates in these localizations were determined and compared with the literature.
Result
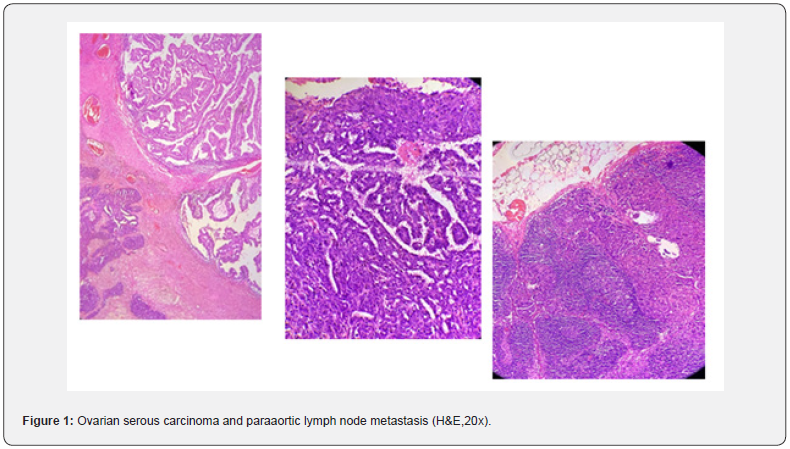
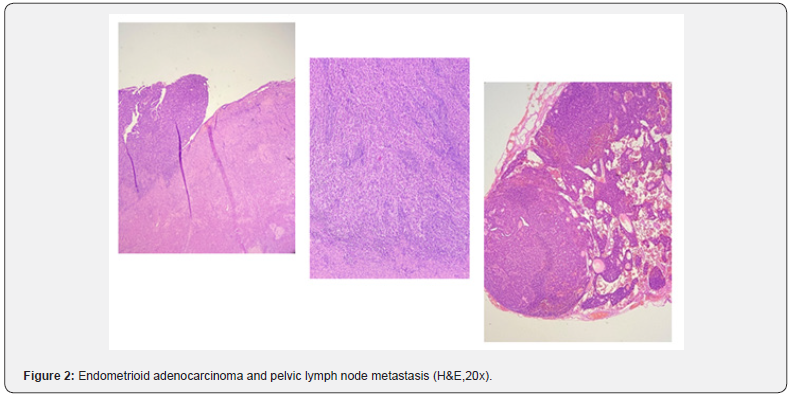
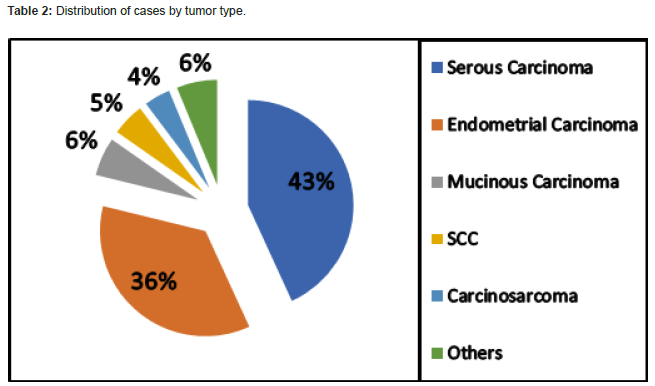
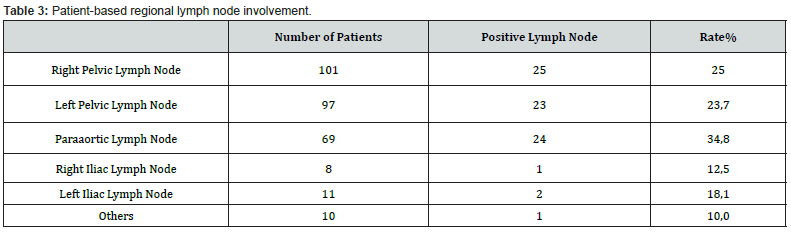
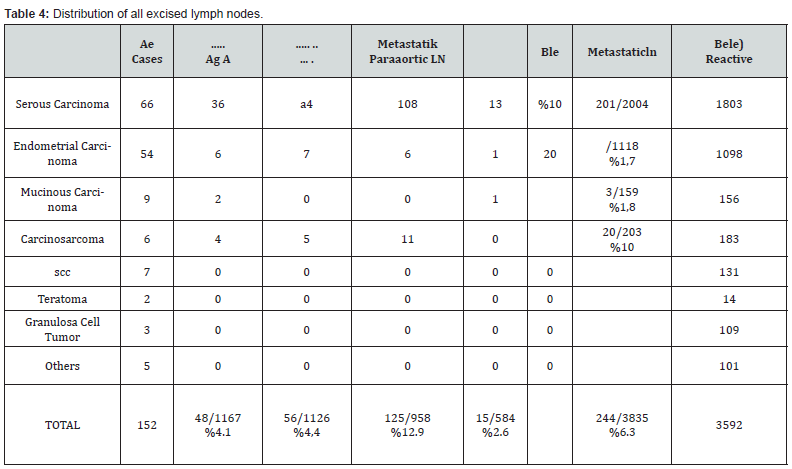
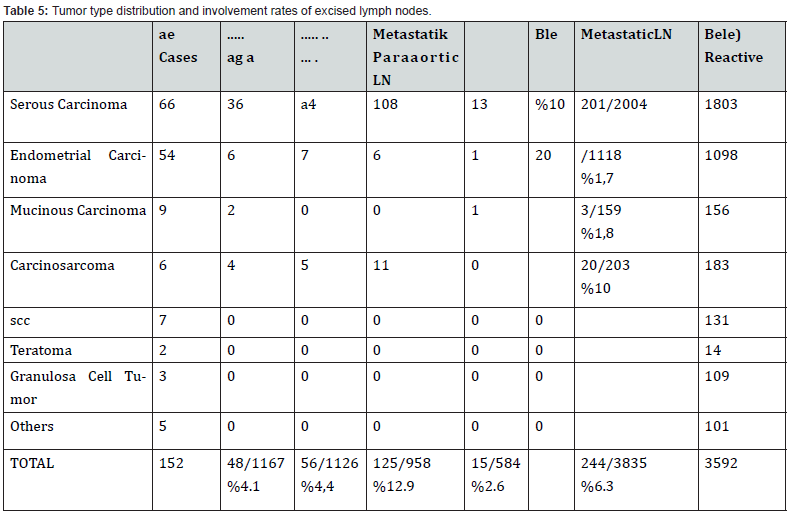
In our study, 152 materials made due to FRSC were evaluated. Of the cases, 87 of them were ovary, 58 of them were uterus, and 7 of them were cervix, and the mean age was 56.86 (Table 1). Lymph node dissection was performed in 128 (84%) patients with tumors, and not to 24 (16%). As the tumor type, serous carcinoma was the first with 66 cases, endometrioid carcinoma was the second with 54 cases, and mucinous carcinoma was the third with 9 cases, and other diagnoses were given (Table 2) (Figures 1& 2). The resected lymph nodes were regionally classified as right pelvic lymph nodes, left pelvic lymph nodes, paraaortic lymph nodes, right iliac lymph nodes, left iliac lymph nodes and other groups. Metastasis was detected in 34.8% of the paraaortic lymph nodes, and the rate was found to be higher (Table 3). The distribution of lymph nodes within tumor type and resected lymph nodes is summarized in Tables 4&5. Metastases were detected in 4.1% of the total excised right pelvic lymph nodes and 4.4% of the left pelvic lymph nodes. Metastasis was detected in 12.9% of the paraaortic lymph nodes, regardless of the tumor type.
Discussion
FRSC is an important cause of morbidity and mortality all over the world. Although cervical cancer rates have decreased in recent years, especially due to cervical smear screening, other endometrial and ovarian cancers have been increasing relatively. Significant survival rates are achieved with early detection of lesions and appropriate surgery [6].
Prognostic parameters are especially important in terms of directing the patient to chemo and radiotherapy after surgery. Among these, regional lymph node involvement is very important, and any lymph node involvement carries the pathological stage directly to III. From this point of view, any lymph node involvement constitutes Stage IIIB in cervical cancers, IIIA in ovarian cancers and stage IIIC in endometrial cancers [5].
In our study, patient-based lymph node involvement and detection rates of metastasis in removed lymph nodes were determined in regional lymph nodes resected in FRSC. In this sense, in terms of involvement of right and left pelvic lymph nodes, right pelvic lymph nodes were detected in 25% of patients and left pelvic lymph nodes were detected at similar rates in 23.7% of patients. Fotopoulou et al. detected a positive lymph node rate in 21% of the cases diagnosed with endometrioid carcinoma, and while there was pelvic and paraaortic involvement in 61% of them, only pelvic involvement was detected in 23% of the cases. Fotolopou et al. and in some other studies, the higher rate of metastatic total pelvic lymph nodes (right+left) in endometrioid carcinomas in our study was found to be compatible with the literature [7-10].
In the study of Bacalbasa et al., 48 patients diagnosed with early stage serous carcinoma, paraaortic lymph node metastasis was found in 22.9%, while pelvic lymph node metastasis was found in 18.75%. In a study by Harter et al., 125 cases with a diagnosis of ovarian carcinoma were examined, positive lymph nodes were detected in a total of 104 patients (83.2%), and para-aortic lymph node metastasis was found in 48% of the patients. In our study, similar to the later study, lymph node metastasis was detected in 81.8% of 66 patients with serous carcinoma, para-aortic lymph node metastasis was observed in 35.9% and pelvic lymph node metastasis was observed in 24.2%. The high rate of paraaortic lymph node involvement was evaluated in line with the literature [11-14]. In our study, the presence of involvement in 4.2% of the resected pelvic lymph nodes is not in agreement with the study of Kumar et al., while the involvement in paraaotic lymph nodes is similar (8). In the study of Guo et al., the rate of patients with isolated para-aortic lymphatic metastases (13.7%) was similar to our study (12.9%) [15].
On the other hand, both pelvic and paraaortic lymph node involvement was detected at a higher rate in carcinosarcomas than in other tumors.
Conclusion
In our study, regardless of type, it was observed that right and left pelvic node involvement was similar, and paraaortic lymph node metastasis was higher than the others. Paraaortic lymph node involvement was found to be higher in serous carcinomas than in other tumor types. No significant difference was observed in rightleft, pelvic and paraaortic lymph node metastases in endometrioid carcinoma cases. The findings are consistent with the literature. Detection of metastases in paraaortic lymph nodes higher than other regional lymph nodes was found to be important for the management of surgery. During resection, paraaortic lymph nodes require special attention and studying frozen from these lymph nodes may be necessary.
Conclusion
More studies of good quality are needed to draw adequate conclusions regarding the relationship between vitamin D levels and COVID-19 infection in the pregnant population.
References
- Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, et al. (2021) Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 71(3): 209-249.
- Yetimalar Mh, Uzmanı Joc. Kadin Genital Kanserleri.
- Höhn AK, Brambs CE, Hiller GGR, May D, Schmoeckel E, et al. (2021) Horn L-C. 2020 WHO classification of female genital tumors. Geburtshilfe Frauenheilkd 81(10): 1145-1153.
- Weiderpass E, Hashim D, Labrèche F (2020) Malignant tumors of the female reproductive system. Occupational Cancers, pp. 439-453.
- Mariani A, Dowdy SC, Cliby WA, Haddock MG, Keeney GL, et al. (2006) Efficacy of systematic lymphadenectomy and adjuvant radiotherapy in node-positive endometrial cancer patients. Gynecol oncol 101(2): 200-208.
- Eggemann H, Ignatov T, Kaiser K, Burger E, Costa SD, et al. (2016) Survival advantage of lymphadenectomy in endometrial cancer. J Cancer Res Clin Oncol 142(5): 1051-1060.
- Hirahatake K, Hareyama H, Sakuragi N, Nishiya M, Makinoda S, et al. (1997) A clinical and pathologic study on para‐aortic lymph node metastasis in endometrial carcinoma. J Surg Oncol 65(2): 82-87.
- Kumar S, Podratz KC, Bakkum-Gamez JN, Dowdy SC, Weaver AL, et al. (2014) Prospective assessment of the prevalence of pelvic, paraaortic and high paraaortic lymph node metastasis in endometrial cancer. Gynecol oncol 132(1): 38-43.
- Mariani A, Dowdy SC, Cliby WA, Gostout BS, Jones MB, et al. (2008) Prospective assessment of lymphatic dissemination in endometrial cancer: a paradigm shift in surgical staging. Gynecol oncol 109(1): 11-18.
- Fotopoulou C, Savvatis K, Kraetschell R, Schefold JC, Lichtenegger W, et al. (2010) Systematic pelvic and aortic lymphadenectomy in intermediate and high-risk endometrial cancer: lymph-node mapping and identification of predictive factors for lymph-node status. European Journal of Obstetrics & Gynecology and Reproductive Biology 149(2): 199-203.
- Harter P, Gnauert K, Hils R, Lehmann T, Fisseler-Eckhoff A, et al. (2007) Pattern and clinical predictors of lymph node metastases in epithelial ovarian cancer. Int J Gynecol Cancer 17(6): 1238-1244.
- Takeshima N, Hirai Y, Umayahara K, Fujiwara K, Takizawa K, et al. (2005) Lymph node metastasis in ovarian cancer: difference between serous and non-serous primary tumors. Gynecol oncol 99(2): 427-431.
- Bacalbasa N, Balescu I, Vilcu M, Dima S, Diaconu C, et al. (2020) The risk of para-aortic lymph node metastases in apparent early stage ovarian cancer. Medicina (Kaunas) 56(3): 108.
- Prader S, Vollmar N, du Bois A, Heitz F, Schneider S, et al. (2019) Pattern and impact of metastatic cardiophrenic lymph nodes in advanced epithelial ovarian cancer. Gynecol Oncol 152(1): 76-81.
- Guo J, Qian H, Ma F, Zhang Y, Cui X, et al. (2020) The characteristics of isolated para-aortic lymph node metastases in endometrial cancer and their prognostic significance. Ther Adv Med Oncol 12: 1758835920933036.






























