A Histopathological Study of Endometrial Biopsies in Abnormal Uterine Bleeding
Manjari SKVSK1* and T Satya Prakash Venkatachalam2
1Post Graduate Department of Pathology, GSL Medical College and General Hospital, India
2Professor & HOD, Department of Pathology, GSL Medical College and General Hospital
Submission: August 19, 2023;Published: August 25, 2023
*Corresponding author: Manjari SKVSK, Post Graduate Department of Pathology, GSL Medical College and General Hospital, India
How to cite this article: Manjari S, T Satya Prakash V. A Histopathological Study of Endometrial Biopsies in Abnormal Uterine Bleeding. J Gynecol Women’s Health 2023: 25(5): 556172. DOI: 10.19080/JGWH.2023.25.556172
Abstract
Background: Abnormal uterine bleeding (AUB) is a very common gynecological problem for which histopathological examination of the endometrium is the gold standard to confirm the exact nature of the lesion and to rule out malignancy.
Methods: A prospective study was done in the Department of Pathology from October 2019 to October 2021 on two hundred endometrial biopsy specimens received from clinically diagnosed cases of AUB.
Result: AUB was most commonly seen in the age group of 41- 50 years. Most of the cases clinically presented with heavy menstrual bleeding. The most common histopathological finding was proliferative endometrium seen in 29% cases followed by secretory endometrium in 17% cases, endometrial carcinoma in 15% of cases and endometrial hyperplasia in 14.5% of cases.
Conclusion: Endometrial biopsy is a valuable tool for assessment of endometrial status in cases of AUB due to relative ease, accessibility of procedure and rapid availability of results.
Keywords: Abnormal uterine bleeding; Proliferative endometrium; Secretory endometrium; Carcinoma; Hyperplasia
Abbreviations: AUB: Abnormal Uterine Bleeding; AEH: Atypical Endometrial Hyperplasia; EIN: Endometrial Intraepithelial Neoplasia
Introduction
Menstrual disorders among women of all age groups continue to be a challenging proposition for clinicians to manage, the most important of them being abnormal uterine bleeding (AUB) [1]. The endometrium undergoes dynamic physiological and morphologic changes by the complex interplay of endogenous sex steroids and other systemic as well as iatrogenic factors and when this gets disturbed it. manifests as AUB. [2].
AUB is defined as a bleeding pattern that differs in frequency, duration, and amount from a pattern observed during a normal menstrual cycle or after menopause [3]. In India, the reported prevalence of AUB is around 17.9% [1]. The FIGO Working Group on Menstrual Disorders has classified the various causes for AUB into structural /organic causes and non-structural causes and represented as an acronym PALM- COEIN: polyp; adenomyosis; leiomyoma; malignancy and hyperplasia; coagulopathy; ovulatory dysfunction; endometrial; iatrogenic; and not yet classified [4,5].
Clinical bleeding patterns are determined by the heaviness, duration of flow, regularity, and frequency [6]. The terminologies menorrhagia, metrorrhagia, menometrorrhagia and dysfunctional uterine bleeding are poorly defined and confusing. FIGO Menstrual disorders Working Group in 2011 proposed to abandon the terminology dysfunctional uterine bleeding and use the terms AUB and heavy menstrual bleeding [5].
The causes of AUB vary with age. In the reproductive age group, it is most commonly due to hormonal imbalance while in the perimenopausal and menopausal women AUB is generally due to hyperplasia and malignancies [7]. Significant mortality or morbidity can occur if endometrial hyperplasia is untreated with progression to malignancy [2]. Endometrial biopsy is the gold standard method for distinguishing normal endometrium from pathological endometrium. Endometrial biopsy, dilation and curettage (D&C), and hysteroscopy are the most common endometrial sampling methods [8]. The D & C is the gold standard in diagnosing AUB, however over years it has been replaced by Pipelle’s endometrial biopsy as it is a safe and simple outpatient diagnostic procedure. Evaluation of endometrial biopsies helps not only to identify the cause of AUB but also to provide an appropriate treatment thereby reducing the need for complications associated with hysterectomies [9]. The aim of this study is to determine the spectrum of endometrial pathologies in patients of different age groups presenting with AUB..
Materials and Methods
This was a descriptive study conducted in the Department of Pathology, GSL Medical College and General Hospital, Rajahmundry from October 2019 to October 2021.Clinical history was collected from the patients .The study included a total of two hundred endometrial biopsies obtained from patients presenting with abnormal uterine bleeding of all age groups.
Inclusion Criteria
Endometrial biopsies in patients presenting with AUB
Exclusion Criteria
a) Patients presenting with bleeding due to primary or
secondary bleeding disorders,
b) AUB secondary to cervical and vaginal lesions.
c) Unsatisfactory samples (Only blood clots and fibrin; no
endometrial gland /stroma)
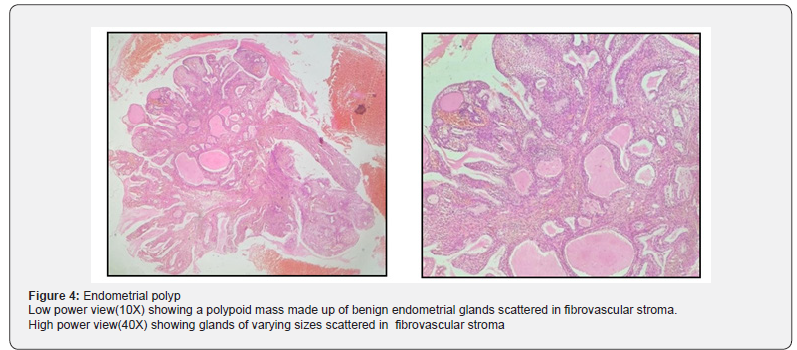
Endometrial biopsy specimens were obtained by either Pipelle’s endometrial biopsy or by dilatation and curettage. The samples received were fixed in10% formal saline. All the gross findings were recorded. Paraffin blocks were made from these biopsies after subjecting to standard histopathology processing. Tissue sections were made as per standard protocol and stained by Hematoxylin and Eosin (H&E) stain. The slides were examined by a pathologist. Microscopic findings and histopathological diagnosis were noted (Figure 1-3).
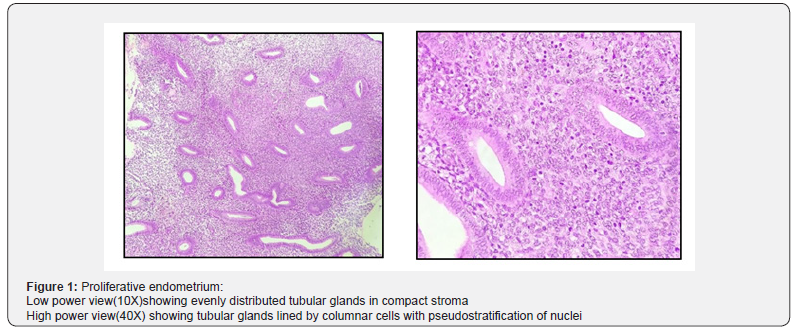
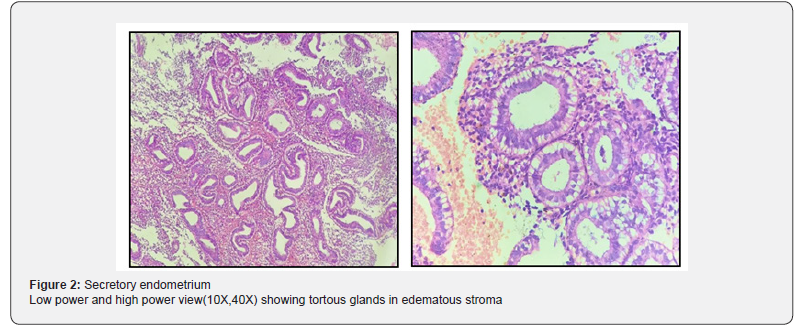
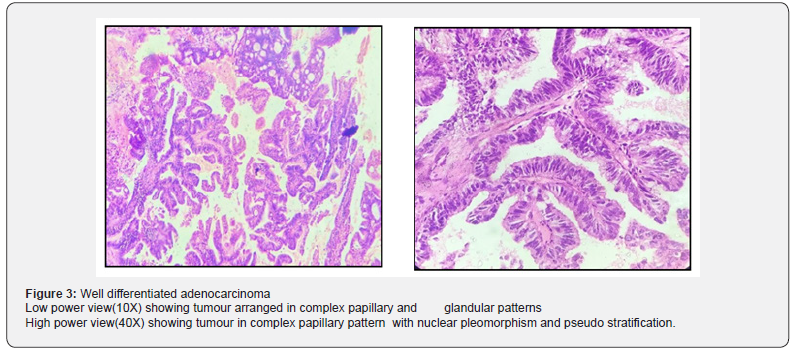
Statistical Analysis
Statistical analysis was performed using MS excel 2010.
Result
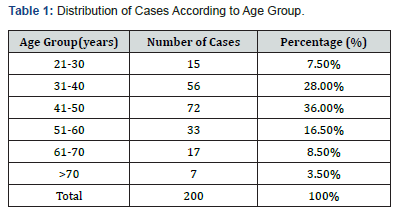
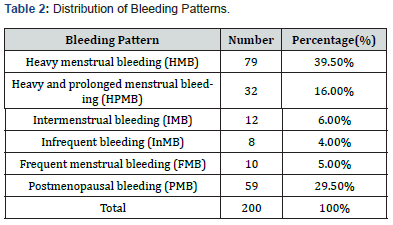
The present study included patients aged 21 to 84 years. Majority of cases (36%) were seen in the age group of 41-50 years (Table 1). The incidence of AUB was found to be 89% in multiparous women, 5.5%in nulliparous women and 5.5% in grand multiparous women. The presenting symptoms in this study were heavy menstrual bleeding found in 39.5 % cases, postmenopausal bleeding in 29.5 % cases, heavy and prolonged menstrual bleeding in 16 % cases, intermenstrual bleeding in 6 % cases, frequent menstrual bleeding in 5% cases and infrequent menstrual bleeding in 4% cases (Table 2).
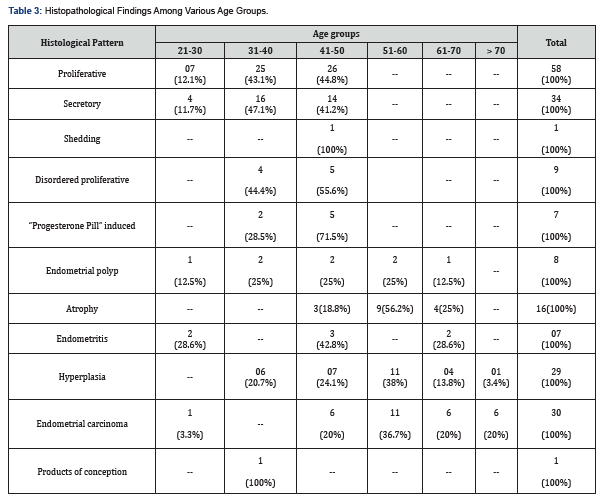
Proliferative phase endometrium was the most common etiology in 29% cases followed by secretory phase endometrium in 17% cases, endometrial carcinoma in 15% cases, endometrial hyperplasia in 14.5% cases, atrophic endometrium in 8% cases, disordered proliferative endometrium in 4.5% cases, endometrial polyp in 4% cases, non-specific/chronic endometritis in 3.5% cases, “Progesterone Pill” induced endometrium in 3.5% cases, shedding endometrium in 0.5% cases and products of conception in remaining 0.5% cases.
Normal endometrial pattern comprising of proliferative phase endometrium, secretory phase endometrium and shedding endometrium was predominantly found in 31-40and 41-50 year age group while endometrial carcinoma and endometrial hyperplasia were predominantly found in 51-60 year age group. Out of two hundred samples, one hundred and fortyone samples belonged to the pre-menopausal age group with proliferative endometrium and secretory endometrium being the most common etiology. Whereas in the post-menopausal age, endometrial carcinoma was the most common etiology followed by endometrial hyperplasia and atrophic endometrium (Table 3)..
Endometrial hyperplasia constitutes 14.5% of cases, out of which 58.6% cases were hyperplasia without atypia and 41.4% cases were AEH/EIN. Among 30 endometrial carcinomas, 29 (96.7%) were of endometrioid type and 1 (3.3%) case of serous sub type.
Discussion
AUB exhibits different presentations and varied causes leading to considerable social and physical morbidity in all societies, thus demanding appropriate evaluation and management [10]. Endometrial evaluation is performed to assess the hormonal influence of the endometrium and also to diagnose premalignant and malignant conditions [11].
The most common age group presenting with AUB in the present study is 41-50 years (36 %) followed by 31-40 years which is in concordance with the studies done by Jairajpuri ZS et al. [12] (35.89%) and Khurram N et al. [13] (37%). An increased number of cases in this age group, which is mostly the perimenopausal age, could be due to the fact that as women reach menopause, there is a decrease in the number of ovarian follicles along with increased resistance to gonadotrophic stimulation resulting in a low level of oestrogen which is an essential requirement for growth and maintenance of normal endometrium. [14]. The highest incidence of AUB is seen in multiparous women in the present study (89%) which is in concordance with the study done by Golecha N et al. [15] (82%)
Heavy menstrual bleeding (39.5%) is the most common type of bleeding pattern noted which correlates with the study done by Singh P et al. [16] (40%). The next common bleeding pattern observed is postmenopausal bleeding which correlates with the study done by Bindroo S et al. [17]. Histopathological examination of the endometrium showed patterns ranging from physiological to pathological lesions of the endometrium. The most predominant histopathological finding is the normal cyclical pattern (46.5%) which correlates with the studies done by Singh P et al. [13] Khurram N et al. [16] and Rachamallu L et al. [18]. The bleeding in the proliferative phase may be due to anovulatory cycles and bleeding in the secretory phase may be due to ovulatory dysfunctional uterine bleeding.
The high proportion of endometrial carcinoma (15%) in our study compared to other studies [19-22] is presumably because our hospital is a teaching hospital and a referral centre for oncology cases. Most of the endometrial hyperplasia cases presented in the postmenopausal age group. Endometrial hyperplasia is a precursor for endometrial cancer with an overall risk of progression to cancer being 5-10%. Hence, its identification is important in cases presenting with AUB. Atrophic endometrium constituted 8% of the total number of cases with most cases presenting in the postmenopausal age group similar to the study done by Bhatta S et al. [20]. Benign endometrial polyps constituted 4 % of the total number of cases in the present study which correlates with the study done by Khan et al. [11] Prolonged oestrogen stimulation leads to hyperplasia of basal endometrial layer resulting in polyp formation.
Chronic/non-specific endometritis was diagnosed in 3.5% of cases which correlates with the study done by Vaidya et al. [23] Endometritis is a contributing factor for AUB. Subepithelial capillary plexus and surface epithelium are rendered fragile by inflammatory mediators leading to breaks and micro erosions resulting in uterine bleeding.
Conclusion
AUB is one of the most common conditions affecting women of all ages. It is caused by various endometrial pathologies that can directly and indirectly lead to clinical problems causing impairment of physical and mental health of women. Endometrial sampling through both office endometrial biopsy and endometrial curettage after dilatation are equally useful in obtaining endometrial samples.
Histopathological evaluation of endometrial biopsies plays a crucial role in the evaluation of and diagnosis of various gynaecological conditions. AUB cases on assessment by histopathological examination in this study revealed varying patterns: endometrial hyperplasia, atrophic endometrium and endometrial carcinoma which can overtly be considered as the aetiology in many cases. However, in the remaining cases, the endometrial histology was within normal limits and was either in proliferative phase or in secretory phase indicating the possible existence of an eluding aetiology.
In postmenopausal women, endometrial carcinoma is the commonest cause for AUB. However, in this study, this ominous disease was detected in equal proportions to endometrial hyperplasia in women of reproductive age also and hence requires to be kept in mind while assessing AUB cases in this age group.
Hence, accurate identification of the causative factor of AUB by histopathological evaluation of endometrial biopsy samples still remains the gold standard for the diagnosis of endometrial pathology.
References
- Malati BG, Ashok M (2017) Endometrial histopathology in abnormal uterine bleeding. J Archives of Cytology and Histopathology Research 2(4): 70-74.
- Tiwari A, Kaur N, Jain S, Rai R, Jain SK, et al. (2016) Histopathological study of Endometrial Biopsy Specimens for Abnormal Uterine Bleeding. J Lumbini Med Coll 4(2): 72-76.
- Iqbal MB, Tushar K, Anushree K, Ashily K, Banerjee B, et al. (2018) Spectrum of Endometrial lesions in patients presenting with abnormal uterine bleeding. Ind J Path Oncol 5(4): 587-591.
- Vani BS, Vani R, Jijiya Bai P (2019) Histopathological evaluation of endometrial biopsies and curetting’s in abnormal uterine bleeding. Trop J Path Microbiol 5(4): 190-197.
- Munro MG, Critchley HOD, Broder MS, Fraser IS (2011) FIGO Working Group on Menstrual Disorders. FIGO classification system (PALM-COEIN) for causes of abnormal uterine bleeding in nongravid women of reproductive age. Int J Gynaecol Obstet 113(1): 3-13.
- Mutakha GS, Mwaliko E, Kirwa P (2020) Clinical bleeding patterns and management techniques of abnormal uterine bleeding at a teaching and referral hospital in Western Kenya. PLoS One 15(12): e0243166.
- Puneet K, Anureet K, Anil Kumar S, Harpreet S (2016) A two year histopathological study of endometrial biopsies in a teaching hospital in Northern India. Ind J Path Oncol 3(3): 508-519.
- Günakan E, Atak Z, Albayrak M, Kurban Y, Şimşek GG, et al. (2018) Endometrial histopathology results and evaluation of endometrial cancer risk in geriatric women. Prz Menopauzalny 17(1): 18-21.
- Prathipaa R, Divya J (2016) Histopathological study of endometrial samples in abnormal uterine bleeding. Indian J Pathol Oncol 7(4): 567-570.
- Swati BM, Abdul GK (2016) Histopathological patterns of endometrial lesions in patients with abnormal uterine bleeding in rural area of Western Maharashtra. Ind J Path Oncol 3(4): 665-672.
- Damle RP, Dravid NV, Suryawanshi KH, Gadre AS, Bagale PS, et al. (2013) Clinicopathological spectrum of endometrial changes in Peri-menopausal and post-menopausal abnormal uterine bleeding: A 2 years study. J Clin Diagn Res 7(12): 2774-2776.
- Khan R, Haiyat S, Maheshwari V, Hakim S (2019) Clinico-Pathological spectrum of endometrial lesions in patients with abnormal uterine bleeding in accordance with PALM-COEIN classification: A prospective study of 3 years in a tertiary care hospital of Western Uttar Pradesh. Ann Pathol Lab Med 6(2): A76-83.
- Jairajpuri ZS, Rana S, Jetley S (2013) Atypical uterine bleeding-Histopathological audit of endometrium A study of 638 cases. Al Ameen J Med Sci 6(1): 21-28.
- Khurram N, Ghumman NA, Yusuf NW (2020) Morphological pattern of endometrial biopsy in women with clinical diagnosis of abnormal uterine bleeding. Esculapio 16(4): pk1-5.
- Mahapatra M, Mishra P (2015) Clinicopathological evaluation of abnormal uterine bleeding. J Health Res Rev 2(2): 45-49.
- Golecha N, Porwal V (2018) Abnormal uterine bleeding: A study of its clinical spectrum and incidence of histopathological patterns of endometrium as a function of age with parity. Ind J Obstet Gynecol Res 5(3): 339-343.
- Singh P (2018) Abnormal uterine bleeding-evaluation by endometrial aspiration. J Midlife Health 9(1): 32-35.
- Bindroo S, Garg M, Kaur T (2018) Histopathological spectrum of endometrium in abnormal uterine bleeding. Int J Reprod Contracept ObstetGynecol 7: 3633-3637.
- Rachamallu L, Bhavani V, Byna P (2015) Histological correlation of pipelle endometrial sampling with dilatation and curettage in abnormal uterine bleeding. Int J Reprod Contracept Obstet Gynecol 4: 1324-1329.
- Mahmoud MM, Rifat aseel ghazi (2013) Endometrial Histopathological Changes in Women with Abnormal Uterine Bleeding in Kirkuk City, a Clinicopathological Study. Med J Babylon 10(3): 567-582.
- Bhatta S, Sinha AK (2012) Histopathological study of endometrium in abnormal uterine bleeding. J Pathol Nepal 2(4): 297-300.
- Sajitha K, Padma SK, Shetty KJ, Kishan Prasad HL, Permi HS, et al. (2014) Study of histopathological patterns of endometrium in abnormal uterine bleeding. CHRISMED J Health Res 1(2): 76-81.
- Jyotsana, Manhas K, Sharma S (2004) Role of hysteroscopy and laparoscopy in evaluation of abnormal uterine bleeding. JK Sci 6(1): 23-27.
- Vaidya S, Lakhey M, Vaidya SA, Sharma PK, Hirachand S, et al. (2013) Histopathological pattern of abnormal uterine bleeding in endometrial biopsies. Nepal Med Coll J 15(1): 74-77.






























