Placenta Accreta Spectrum; Different Management Approach. A Report of Two Cases
Adegoriola Olubisi Ojurongbe1, Matthew Olusegun Fijabiyi2, Edwin Emeka Nwokolo1, Onazi Ochima1, William Oladiran Taiwo3 and Toyin oluwumi Fijabiyi1*
1Department of Obstetrics and Gynaecology, Federal Medical Centre Keffi, Nigeria
2Department of Obstetrics and Gynaecology, College of Clinical Sciences, Ladoke Akintola University of Technology, Ogbomoso, Nigeria
3The Limi Hospitals, Federal Capital Territotry, Nigeria
Submission: April 17, 2023; Published: April 25, 2023
*Corresponding author: Fijabiyi Matthew Olusegun, Department of Obstetrics and Gynecology, Ladoke Akintola University of Technology Ogbomoso, Nigeria
How to cite this article: Adegoriola O O, Matthew O F, Edwin E N, Onazi O, William Oladiran T. Placenta Accreta Spectrum; Different Management Approach. A Report of Two Cases. J Gynecol Women’s Health 2023: 25(1): 556154. DOI: 10.19080/JGWH.2023.25.556154
Abstract
Introduction: Placenta accreta spectrum (PAS) is one of the conditions that can be regarded as “obstetrician nightmare” because of its attendant severe maternal morbidity and significant mortality from haemorrhage, owing to its unique challenges in diagnosis and management. The incidence of PAS is on the rise in recent times due to increasing caesarean delivery rates. Early identification of patients with risk factors, multidisciplinary team management approach, availability of blood / blood ality.
Main symptoms: In this report of two cases the authors presented their experience in the management of two multiparous women with placenta accreta spectrum, the first patient had placenta percreta and the second patient had placenta increta.
The cases were referred from a peripheral facility with bleeding per vaginum and diagnosis was incidentally discovered at surgery.
Intervention: The first patient had a subtotal hysterectomy and the second patient had a conservative surgery (fertility sparing) with satisfactory post-operative outcomes.
Conclusion: Placenta accreta spectrum is an obstetrician nightmare due to the morbidity and mortality associated with it thus early identification of risk factors and effective management through multidisciplinary approach is paramount to a good outcome.
Keywords: Placenta accreta spectrum; placenta previa; Hysterectomy; Uterine tamponade; Morbidly adherent placenta
Introduction
Placenta accreta spectrum was previously known as morbidly adherent placenta or abnormally invasive placenta [1]. The spectrum describes a pathological adherence of the placenta to the myometrium making spontaneous detachment of the placenta difficult after delivery [1]. This range of abnormal placenta invasion includes placenta accreta, placenta increta and placenta percreta [1]. One of the accepted hypothesis on the etiology of PAS is theory that stated a defect of the endometrial - myometiral interface which leads to failure of normal decidualization in the area of uterine scar, which allows abnormally deep placental anchoring villi and trophoblast infiltration [1,2,]. Maternal morbidity and mortality resulting from PAS are usually severe and life –threatening haemorrhage, which in most cases requires massive blood transfusion and management is often multidisciplinary in approach involving surgical expertise, availability of blood transfusion facility, interventional radiology [1,2]. The incidence of PAS is on the rise in recent times due to increasing caesarean delivery rates as previous caesarean section is a major cause of abnormal placenta adherence [1-3].
We report two cases of multiparous women with PAS, the first was a case of placenta percreta and the second was placenta increta. They were both referred cases from a peripheral facility and diagnosis of placenta accreta spectrum were made incidentally intra-op. The first patient had a subtotal hysterectomy and the second had a conservative surgery (fertility sparing). Both patients did well post operatively were discharged home in good condition.
Patient and Observation
Case 1
Patient information: a 28 year old booked elsewhere G5P2 +2 (1 alive) woman with 1 previous caesarean section scar. She was unsure of LMP but early ultrasound scan done at 12weeks puts her gestational age at 34weeks 5 day at presentation. She was referred from a peripheral hospital on account of bleeding per vaginam of 3 hours duration. Bleeding was sudden in onset, unprovoked, bright red in colour, associated with clot, there was no history of warning bleed, fainting spells, dizziness, no proceeding trauma to the abdomen, no genital instrumentation or signs of labour. She had no co-morbidity. Index pregnancy was desired spontaneously conceived and confirmed by ultrasound at 12 weeks gestation. She booked for antenatal care at the referral centre at 24 weeks gestation. Pregnancy had been eventful until the occurrence of the above complaint. Her 1st and 2nd pregnancies were 6 and 5 years ago and both ended up as spontaneous miscarriages at 24 weeks and 8wks respectively with no post abortal complications. Her 3rd pregnancy was 3 years ago, spontaneously conceived, carried to term and had spontaneous vagina delivery of a live male neonate at term, birth weight was not known. Her 4th pregnancy was 1 year ago, spontaneously conceived, carried to term, delivered via emergency lower segment caesarean section on account of suspected prolonged labour, she was delivered of fresh still birth, birth weight was not known and there was no post partum complication.
Clinical Findings: Examination at presentation revealed a young woman, not in any obvious distress, anxious, not pale, anicteric, acyanosed, not dehydrated, nil pedal edema. Respiratory system examination was essentially within normal range. Cardiovascular examination showed a pulse rate of 110bpm, blood pressure of 120/70mmHg with heart sound 1 and 2 only. Abdominal examination findings were a gravidly enlarged abdomen which moves with respiration, a Pfanenstiel scar that healed by primary intention, there was no area of tenderness, no palpable organomegally, no palpable uterine contraction, symphiofundal height was 36cm, singleton fetus in longitudinal lie, cephalic presentation and a decent of 5/5. Fetal heart tone was not heard with Pinard stethoscope. Pelvic examination revealed perineum smeared with blood and blood clot seen at the introitus. Digital examination was deferred.
Diagnostic assessment: Preoperative packed cell volume was 28%, four units of blood were made available, serologies were all non-reactive.A bedside USS done revealed a viable fetus with major degree placenta previa type 4.
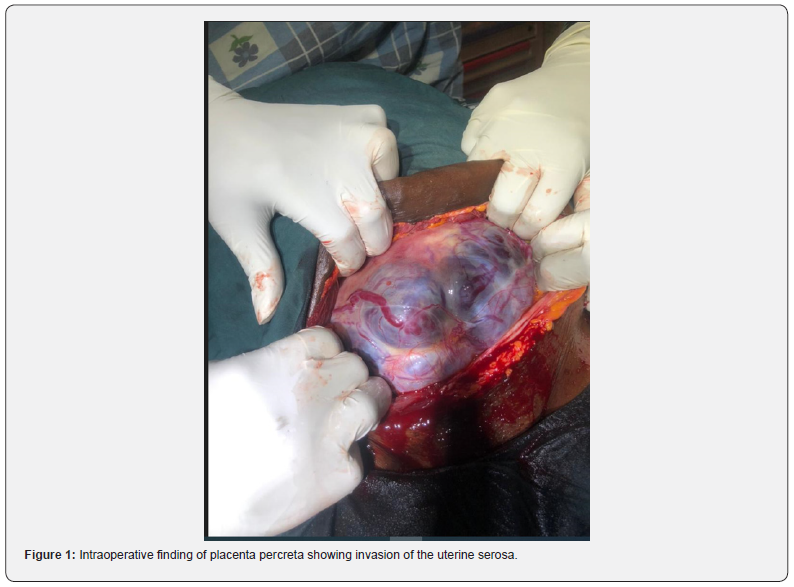
Diagnosis: An assessment of Antepartum haemorrhage due to placenta previa in a multigravida with 1 previous scar at 34 weeks was entertained. Therapeutic Interventions: She was admitted, counseled on findings and line of management. An informed consent for emergency caesarean section with possible subtotal abdominal hysterectomy was obtained. She had emergency lower segment caesarean section with concomitant sub-total hysterectomy under general anaesthesia. The intra-operative findings were: mild pelvic adhesion, anterior placenta percreta covering the lower 2/3 of anterior uterine wall with multiple visible prominent placenta vessel, normal tubes and ovaries (Figure1). A male neonate in delivered cephalic presentation, weighing 2.2kg with Apgar scores of 6 and 8 in 1st and 5th minutes, estimated blood loss was 3 Liters. She was transfused with five units of blood intra-opt, 10mls of 10% calcium gluconate was given after the third pint of blood. She also had 1gm of intravenous tranexamic acid. Post operatively she was placed on intravenous fluid, antibiotics and analgesics. She was managed in the high dependency unit and had two more units of blood transfused. Baby was admitted in the special care baby unit on account of prematurity. She did well and was discharged home with her baby on the 7th post operative day with a packed cell volume of 29%.
Follow up and Outcome: She was seen at the post natal clinic at 2 and 6 weeks after discharge with no complaint. She was further counseled on the effect of the surgery on her reproductive function and at the six weeks partum visit she was discharge from the clinic.
Case 2
Patient information: a 30 year old booked elsewhere G3P2 (non alive) woman with 2 previous caesarean section scars. She was referred from a peripheral facility where she was attending antenatal clinic on account of bleeding per vaginam of 12 hours duration and ultrasound diagnosis of major degree Placenta previa at gestational age of 36 weeks 4 days. She however presented with profuse bleeding which was bright red in colour, no abdominal pain, no blurring of vision, dizziness or fainting spell. She still perceived fetal movement at presentation. She booked the pregnancy at the referring facility at 20 weeks gestation and was not told of any abnormality aside from ultrasound finding of a low lying placenta and she was told that she will repeat the scan before delivery as the placenta might have migrated spontaneously before term. Her 1st pregnancy was delivered at term via emergency lower segment caesarean section on account of prolonged labour. She was delivered of a fresh still birth. The second pregnancy was delivered through emergency caesarean section on account of failed vaginal birth after caesarean section at term. She was delivered of a severely asphyxiated male child who later died 9 hours of life. There was no post operative complication sequel to the 2 surgical procedures.
Clinical findings: she appeared anxious, agitated, pale, well hydrated with ankle edema. Cardiovascular examination showed pulse rate of 112 beats per minutes, blood pressure of 100/60mmhg, heart sound 1 and 2 only. Respiratory rate was 22 cycles per minute, chest was clinically clear. Abdomen was gravidly enlarged, Pfanenstiel scar that healed with primary intension was noted, symphysiofundal height was 38 centimeter, a singleton fetus in longitudinal lie, cephalic presentation was palpated, fetal heart rate was 154 beats per minutes and regular. Pelvic examination showed bright red blood actively coming out of the vagina. Further pelvic examination was not done.
Diagnostic assessment: urgent bedside scan done in the labour room, showed a live fetus in longitudinal lie, cephalic presentation with placenta Previa type 3A. Preoperative full blood count showed packed cell volume of 26%, white blood cell count of 10,500 mm³, platelet count was 290 x 10⁹, Neutophil 70%, Lymphocytes 21%, Monocyte 8%, Eosinophils 1%. Serology was done and non reactive for human immunodeficiency virus 1 and 2, negative for Hepatitis B and C. Urinalysis was essentially normal. Four units of matched blood were made available for the procedure.
Diagnosis: An impression of Antepartum haemorrhage due to placenta Previa in a multigravida with 2 previous scar at 36weeks GA (to keep in view morbidly adherent palcenta) was made.
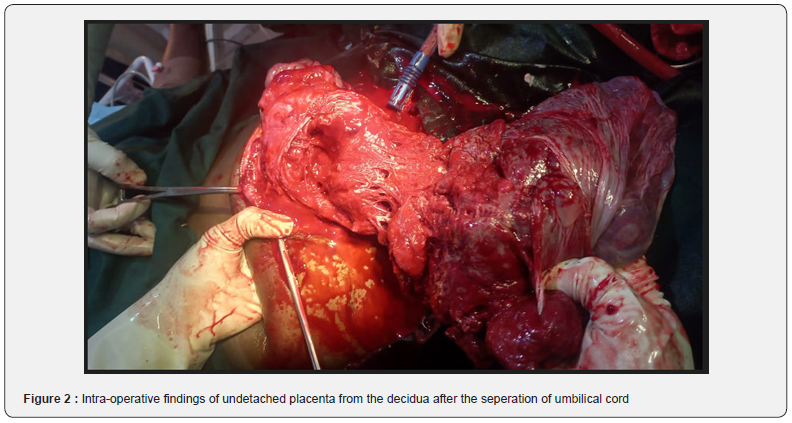
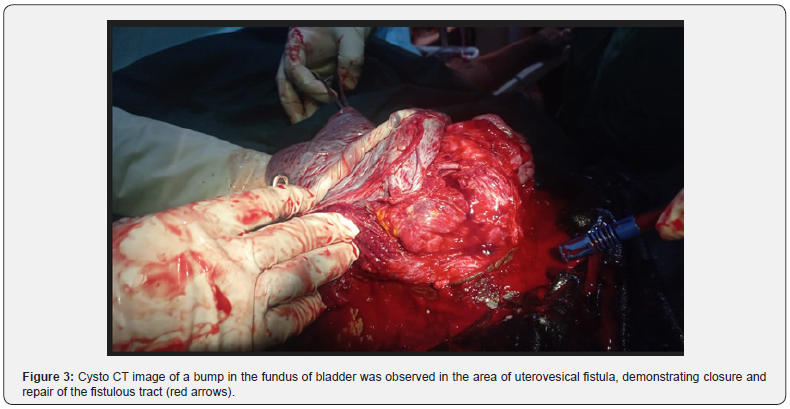
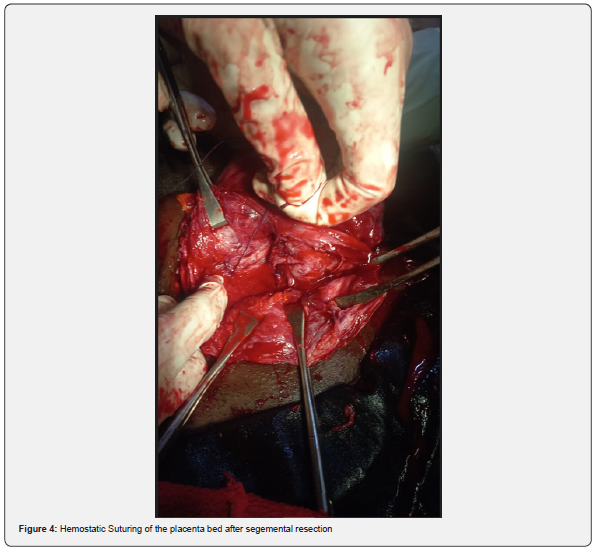
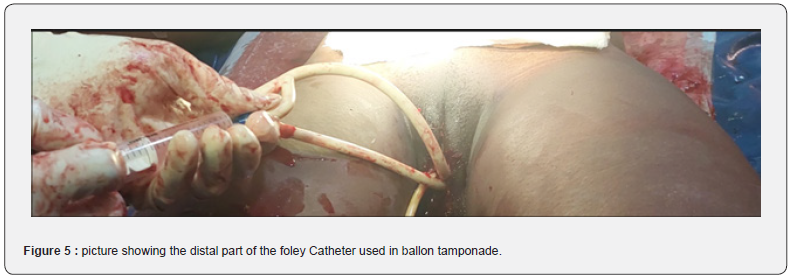
Therapeutic interventions: She was admitted in labour room, counseled on findings and possibly of having morbidly adherent placenta which could be complicated by massive hemorrhage and thus warrant surgical removal of her uterus just in case conservative management fails. An informed consent for emergency caesarean section with possible subtotal abdominal hysterectomy was obtained. She eventually had emergency lower segment caesarean section with the following intra-operative findings, adhesion between anterior abdominal wall and anterior, fundal part of the uterus. Multiple, dilated and tortuous blood vessels were noted on the serosa of the lower uterine segment, a male neonate in delivered cephalic presentation, weighing 3.2kg with Apgar scores of 7 and 8 in 1st and 5th minutes was extracted through an incision made above the dilated blood vessels on the serosa of the lower part of the uterus. The placenta had deeply invaded into the lower one third of the uterus, making the placenta to be adherent to the lower uterine segment (Figure 2&3). Some part of the placental was separated but other parts were deeply invaded the decidua (Figure 3). Segemental resection of the lower uterine segment where there was deep placenta invasion beyond the decidua was done and Hemostatic sutures ŵere applied (Figure 4). Two foleys catheters size 24 was placed into the uterine cavity and the distal end of the catheter exit through the Os into the vagina (Figure 5). The uterus was closed in 2 layers with vicryl 2 sutures and the catheters were inflated with 250ml warm saline each to tamponade the uterine cavity. IV oxytocin infusion 40 units in 1 litre of saline to run every 8 hours was instituted. One thousand microgram of misoprostol was passed into rectum, intramuscular ergometrine 0.5mg stat was also administered. Intravenous ceftriaxone 1gm 12 hourly for 72 hours. She had 3 units of blood transfused intra-operatively. The estimated blood loss was 2 litres. Her vital signs in the immediate post op were normal. Packed cell volume on POD 1 was 24%, she was later transfused with 3 units of blood. The uterine tamponade was removed after 48 hours and she remained stable with minimal lochia per vaginum. She was continued on oral antibiotics for another 7 days and oral analgesic for 5 days. Her vital signs remained stable. She was discharged home on day 8 post Op in good health condition. She was very satisfied with the quality of care she had and was full of praise to all the hospital staffs that managed her.
Follow up and outcomes: She was seen twice in postnatal clinic, first at 2 weeks after discharge and second 6 weeks later with no complaint. Her wound had healed perfectly well and was counseled for contraceptives which she opted for implanon insertion.
Patients perspective: the patients were satisfactory with the quality of care they got and happy about the successful outcomes of the treatments.
Informed consent: Informed consents were obtained from the patients for the information and pictures provided in this manuscript.
Discussion
In placenta accreta, the placenta villi are attached to the myometrium, in placenta increta, the placenta villi invades the myometrium while in placenta percreta, the villi extend beyond the uterine serosa [1]. The first case presented had placenta percreta and the second had placenta increta. One of the accepted hypotheses on the etiology of PAS is theory that stated a defect of the endometrial – myometiral interface while other studies suggested disruptions within the uterine cavity causing damage to the endometrial-myometrial interface which affects scar development and increases the likelihood of PAS [2]. In recent commentary some authors are beginning to see PAS as a disease arising from a combination of factors such as a defective deciduas, abnormal trophoblastic attachment, abnormal angiogenesis with vascular remodeling and progressive uterine scar dehiscence [4]. There are multiple risk factors associated with PAS, the most common is a previous caesarean section delivery, with an increased probability with increased number of cesarean section [3]. Placenta previa is reported in around half of all cases of PAS [5]. The incidence of PAS is also noted to increase with placenta previa and previous caesarean section scar [1]. Other additional risk factors noted include advanced maternal age, multiparity, prior uterine surgeries or curettage, submucous fibroid, chronic endometritis, Asherman’s syndrome [1-3]. The two cases presented had placenta previa, previous caesarean section scar. In addition the first case had uterine curettage on two occasions for spontaneous miscarriage.
Antenatal diagnosis of PAS is greatly encouraged because feto-maternal outcome is better when delivery is carried out in tertiary facility before the onset of labour or bleeding with the disruption of the placenta. Antenatal diagnosis accuracy reaches about 95%, however several population studies revealed that many women with PAS remains undetected before delivery [6]. Therefore it is paramount that all women with risk factors for PAS such as placenta previa, previous caesarean section, should be evaluated antenatally by an experienced Obstetrician and Gynaecologist with expertise in diagnosis of PAS with ultrasound scan. Our index cases were not diagnosed in antenatal period. The main diagnostic modality for antenatal cases is by obstetrics ultrasound, which could be trans- abdominal or transvaginal [7]. Features of placenta accreta may be visible as early as the first trimester but most women are diagnosed in the second and third trimester. Significant songraphic finding on ultrasound associated with PAS in second and third trimester is placenta previa as seen in about 80% of cases; Placenta previa was seen in both patients. There could be the presence of multiple vascular lacunae (lakes) within the placenta, loss of normal hypoechoic zone between the placenta and myomatrium, decreased retroplacenta myometrial thickness (less than 1mm), abnormalities of the uterine serosabladder interface and extension of placenta into the myometrium, serosa or bladder [7].
The use of colour flow Doppler shows turbulent lacunar blood flow, which is the finding in PAS [8]. Magnetic resonance imaging (MRI) is the other major tool used for the antenatal diagnosis of PAS but it is unclear whether MRI improves diagnosis of PAS beyond what is achieved on ultrasound. However MRI may be useful in diagnosis of difficult cases such as posterior placenta previa, to assess the depth of invasion and lateral extension of myometrial invasion where placenta percreta is suspected [9]. Unfortunately, MRI is expensive and not readily available in our environment. Antenatal diagnosis of PAS provides an opportunity to optimize management and ultimately improve outcome [1-3]. This optimal management should be planned and carried out in highly experienced maternity centres that have coordinated care team with ability to mobilize additional expertise and resources when the need arise [1,2]. There are four options of management of placenta accreta spectrum that are have been evaluated with varying degree of success over the years: the conservative treatment, the one step conservative surgery (alternative conservative technique), the extractive method and lastly, the Cesearean hysterectomy which is the radical approach [10].
The preffered choice of management depending on the degree of invasion, clinical parameters, surgical expertise, the available facilities and wishes of the woman. One of the important steps in the management of PAS is to avoid the temptation of removing the placenta either during conservative or radical approach. Making no attempt to remove the placenta is associated with decreased level of haemorrhage and a reduced need for blood transfusion. However, this might be practicable in accidentally diagnosed placenta accreta that was noted intraop as attempt would have been made to deliver the placenta through cord traction and fails as it was seen in the second case presented. When diagnosis is made antenatally, it is important at delivery to balance maternal risk and benefits with those of the fetus. Some authors have reported that performing a caesarean delivery with concomitant caesarean hysterectomy which is considered gold standard before the onset of labour improves maternal outcome, although mortality as high as 7% had been recorded in some cases due to untreatable haemorrhage. It is advisable that all facility performing deliveries should consider the possibility of a case of PAS and have plan to manage such or stabilize patient rapidly and transfer to a higher level of care. Prior to delivery Patients are counseled on the high likelihood for caesarean delivery with or without hysterectomy and informed consent is obtained to that effect. In both case four units of blood were made available and the haematologist and the blood bank were on standby. Some cases might require placing a ureteric stent or cystocoscopy, where there is likelihood of injuring the bladder or interventional radiology with elective arterial balloon occlusion or embolization can be done in order to combact hemorrhage [10]. Incidentally diagnosed cases could be findings at caesarean delivery either prior to placement of uterine incision or after the uterus had been opened, fetus delivered and attempt at delivery of the placenta failed. It is also possible to make a diagnosis of PAS after vaginal delivery. The diagnosis for these cases was incidentally made at surgery. In the first case it was before incision was made on the uterus, while the second was after delivery of the fetus. The management modality can be conservative or radical in approach and these will depend on degree of invasion- accrete, increta or percreta. For accreta a gentle attempt to manually remove the placenta may be successful and surgical haemostasis secured [10]. Our patient with placenta increta had segemental uterine resection and reconstrucion of the uterus together with tamponade of the placenta bed with foleys catheter. If attempts to gently deliver the placenta fails, the placenta can be left in situ, arterial embolization or pelvic devascularization can be done. Patient could be given methotrexate injection, antibiotics and intravenous oxytocics with the believe that spontaneous placenta expulsion or placenta resorption will occour spontaneously, however months of close follow up is required due to the morbidity associated with this approach [10]. In case of placenta increta and percreta a conservative approach can be done by closing the uterine incision with the placenta in situ and patient is managed as in placenta accreta. In situation where future fertility is a concern, fertility sparing surgery can also be done with segmental resection of the invaded myometrium together with the placenta and repair of the myometrium with or without uterine balloon tamponade as it was done in the second patient presented. Finally a sub-total or total abdominal hysterectomy can be done with the placenta in situ after delivery of the fetus. The first patient had sub-total hysterectomy and the second segmental resection with repair and placement of a uterine balloon catheter for tamponade on account of consideration for future fertility.
Conclusion
PAS is one of the conditions that can be regarded as “obstetrician nightmare” because of its attendant severe maternal morbidity and significant mortality. Early identification of patients with risk factors is critical for effective management plan. Management options can be conservative to radical approach depending on several factors. The role multidisciplinary team approach is sine qua non to a favourable feto-maternal outcome with reduction in morbidity and mortality.
Authors Contributions
Patient management : Fijabiyi Matthew Olusegun, Ojurongbe Olubisi Adegoriola, Nwokolo Edwin, Onazi Ochima, Fijabiyi Toyin Oluwumi, Taiwo William.
Manuscript drafting and revision: Fijabiyi Matthew Olusegun, Ojurongbe Olubisi Adegoriola.
References
- Jauniaux E, Collins S, Burton GJ (2018) Placenta accrete spectrum: pathophysiology and evidence-based anatomy for prenatal ultrasound imaging. Am J Obstet Gynecol 218(1): 75-87.
- Jauniaux E, Jurkovic D (2012) Placenta accrete: pathogenesis of a 20th century iatrogenic uterine disease. Plaecenta 33(4): 244-251.
- Morland M, Sarno L, Napolitana R, Angela C, Giovanni T, et al. (2013) Placenta accrete: incidence and risk factors in an area with a particularly high rate of caesarean section. Acta Obstet Gynecol Scand 92(4): 457-460.
- Einerson BD, Comstock J, silver RM, Branch DW, Woorward PJ, et al. (2020) Placenta Accreta Spectrum Disorder: Uterine Dehiscence, Not Placenta Invasion. Obstet Gynecol135(5): 1104-1111.
- Thurn L, Lindqvist PG, Jakobsson M, Colmorn LB, Klungsoyr K, et al. (2016) Abnormally invasive placenta- prevalence, risk factors and antenatal suspicion: results from a large population –based pregnancy cohort study in the Nordic countries. BJOG 123(8): 1348-1355.
- Bailit JL, Grobman WA, Rice MM, Reddy UM, Wapner RJ, et al. (2015) Morbidly adherent placenta treatment and outcomes. Obstet Gynecol 125(3): 683-689.
- Collins SL, Ascroft A, Braun T, Calda P, Langhoff-Roos J, et al. (2016) Proposal for standardized ultrasound description of abnormally invasive placenta (AIP). Ultrasound Obstet Gynecol 47(3): 271-275.
- Collins SL, Stevenson GN, Al-Khan A, Illsley NP, Lawrence I, et al. (2015) Three-Dimensional Power Doppler Ultrasonography for Diagnosing Abnormally Invasive Placenta and Quantifying the Risk. Obstet Gynecol 126(3): 645-653.
- Einerson BD, Rodriguez CE, Kennedy AM, Woodward PJ, Donnelly MA, et al. (2018) Magnetic resonance imaging is often misleading when used as an adjunct to ultrasound in the management of placenta accreta spectrum disorders. Am J Obstet Gynecol 218: 618.el- 618.e7.
- Sentilhes L, Goffinet F, Kayem G (2013) Management of placenta accrete. Acts Obstet Gynecol Scand 92(10): 1125-1134.






























