Spontaneous Perforation of Pyometra Presenting as Acute Abdomen in Postmenopausal Women: A Case Report
Bimita Mahat1*, Jyotsna Sharma Tiwari1, Rumina Malla1, Rachana Saha1 and Sital Karki2
1Kathmandu Medical College Teaching Hospital, Nepal
2Kanti Children’s Hospital, Nepal
Submission: December 21, 2022; Published: January 05, 2022
*Corresponding author: Bimita Mahat, Kathmandu Medical College Teaching Hospital, Nepal
How to cite this article: Bimita M, Jyotsna Sharma T, Rumina M, Rachana S, Sital K. Spontaneous Perforation of Pyometra Presenting as Acute Abdomen in Postmenopausal Women: A Case Report. J Gynecol Women’s Health 2023: 24(3): 556140. DOI: 10.19080/JGWH.2023.24.556140
Abstract
Background: Pyometra is a buildup of pus in the uterine cavity. It is a rare gynecologic condition occurring in 0.5% of patients and is more common in the postmenopausal age group. Spontaneous perforation of a pyometra is an uncommon complication. In most cases, a diagnosis of a ruptured pyometra is made intraoperatively. This paper reports a case of spontaneous perforation of pyometra presenting with generalized peritonitis and pneumoperitoneum.
Case Description: A 74 -year-old P2L2 with postmenopausal status was brought to the emergency department with a history of abdominal pain and intermittent fever. Emergency computed tomography of the abdomen and pelvis with contrast was done, which revealed a focal defect (uterine rupture) within the anterior wall of the uterus. Mild to moderate peritoneal collection with pneumoperitoneum and reactive wall thickening of jejunum bowel loops. Emergency exploratory laparotomy was planned. At laparotomy, about 1500 mL of pus from the source of uterine was found in the abdominal cavity, while the gastrointestinal tract was intact and a perforation of 5 x 4 cm on the fundus of the uterus was seen intraoperatively. A total abdominal hysterectomy and a bilateral salphingo-oophorectomy were performed. Histopathological reports were suggestive of pyometra and chronic cervicitis with acute salpingitis. Postoperatively (within 12hrs), her conditions were unstable and she went to the Refractory septic shock. Unfortunately, the patient suffered from cardiac events and died on the 8th post-op day.
Conclusion: Perforation of pyometra is a rare case, age of women, prompt diagnosis, management, and treatment is crucial. Ultrasonography has a limited role in the diagnosis of perforated pyometra, hence additional diagnostic radiographic imaging could be used, prompt exploration is an important part in diagnosis. Mortality from spontaneously performed pyometra exceeds 40%. It highlights the importance of multidisciplinary involvement in treating sepsis.
Keywords: Acute abdomen; Postmenopause; Pyometra; Spontaneous perforation of pyometra
Introduction
Pyometra is a collection of pus in the uterine cavity with several aetiologies like malignancy of the genital tract more commonly and sometimes benign lesions and other benign conditions. The clinical presentation of pyometra is a whitish discharge per vaginum and sometimes lower abdominal pain and bleeding per vaginum also. Spontaneous rupture of pyometra is a rare complication. Usually, a definite diagnosis of spontaneous rupture pyometra was made only by laparotomy. A 2014 literature review found only 81 reported cases from 1949-2015 and noted a mortality rate of 31%. This case report illustrates an otherwise healthy post-menopausal female who developed an intrauterine infection that progressed to a rare surgical emergency called pyometra.
Case Report
A 74 -year-old P2L2 with postmenopausal status was brought to the emergency department with a history of abdominal pain for three days and intermittent fever for five days. A thorough physical examination revealed her vitals were BP- 110/80mm of Hg, Pulse - 68bpm, RR- 16/min, Spo2–98% in RA. On her abdominal examination, the abdomen was diffuse and marked tenderness and muscle rigidity with rebound tenderness over the whole abdomen. Per speculum examination showed a healthy-looking cervix with normal discharge and on her prevaginal examination, uterus size could not be assessed due to guarding and rigidity, and fornices could not be commented.
Laboratory studies demonstrated a white blood cell count of 10,500/mm3, Hemoglobin of 12.6mg/dl, and assessed normal kidney and liver functions. A plain abdominal X-ray film showed free air below the diaphragm. Given the absence of any peritonism and features suggestive of bowel obstruction, perforation of the viscus, most likely uterus, was suspected. Emergency computed tomography of the abdomen and pelvis with contrast was done, which revealed a hypodense collection admixed with multiple air foci in the endometrial cavity with thinned-out myometrium and a focal defect (uterine rupture) within the anterior wall of the uterus. Mild to moderate peritoneal collection with pneumoperitoneum and reactive wall thickening of jejunum bowel loops. All evidence from the case history, lab reports, radiography suggested a case of spontaneous perforation of pyometra with generalized peritonitis.
Thus, an emergency exploratory laparotomy was planned.
She underwent an emergency laparotomy under general anesthesia. Before surgery, informed consent was taken from the patient and patient party. Intraoperatively, a perforation of the anterior wall of the uterus, approximately 3x 2cm in diameter, located in the fundus, with purulent fluid exuding from the lesion with compression was noted (Figures 1&2). 1.5L of seropurulent fluid in the peritoneal cavity was also collected. To ascertain gastrointestinal and gallbladder involvement, a surgeon was consulted for expert opinion which revealed no any abnormal findings. A total blood loss of 450ml was present. A diagnosis of generalized peritonitis due to the spontaneous perforation of pyometra was confirmed intraoperatively. A total hysterectomy with bilateral salpingo-oophorectomy was carried out. Macroscopically, a dent of 4cm x 5cm on the anterior fundus of the uterus was noted. The endometrium was damaged with multiple areas of hemorrhage and necrotic spots with brownblack discoloration.
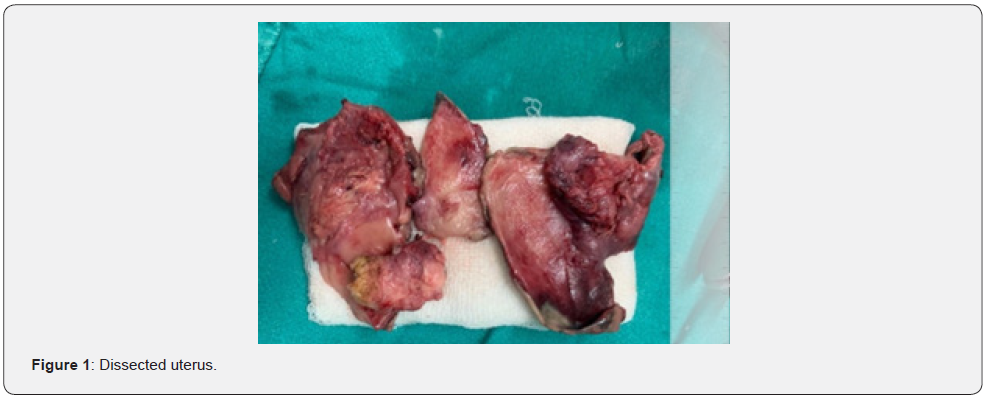
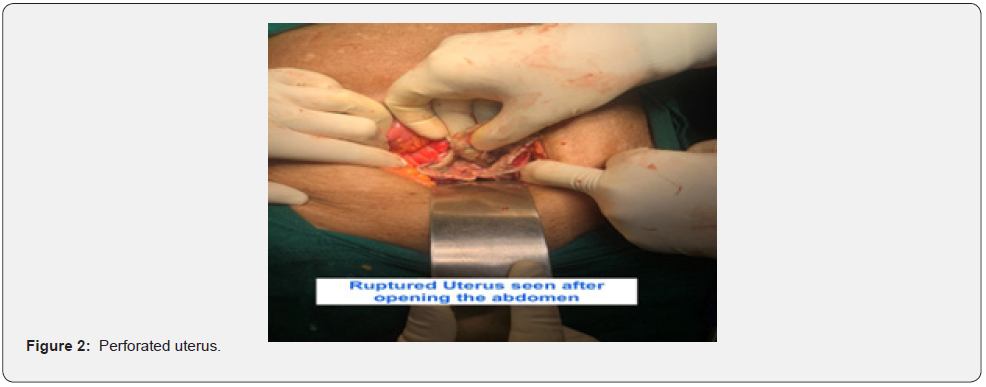
On pathological reporting, pyometra with an enlarged uterus, destruction of the endometrium, and cervical occlusion was found. There was no evidence of malignancy. The culture of the purulent fluid in the peritoneal cavity showed no growth of the organism. Histopathological reports were suggestive of pyometra and chronic cervicitis with acute salpingitis.
Postoperatively (within 12hrs), her condition was unstable and she went to the Refractory septic shock with an increasing need for ionotropic and vasopressors, her vitals were BP- 80/50mm of Hg, Pulse- 102 beats per minute. She was immediately intubated and kept in the ventilator support with broad-spectrum antibiotics and inotropic support of noradrenaline @ 0.3mcg/ kg/min, vasopressor @ 4.8U/hr and adrenaline @ 0.2mcg/kg/ min. She was managed with increasing doses of inotropes despite proper fluid resuscitation. An echocardiographic screening by the intensivist revealed global hypokinesia with moderately reduced ejection fraction. Septic cardiomyopathy with the doubtful presence of ischemic heart disease was also reported. Dobutamine was added to the ionotropic support at the rate of 10mcg/kg/ min. Urine output was maintained up to 1ml/kg/min. Despite the patient being in septic shock, pulmonary involvement in terms of increased oxygen requirement and ventilator support was not needed in the successive ICU days. The patient was improved gradually with a tapered dose of inotropes and improved cardiac contraction (bedside Echo screening test).
On the 3rd postoperative day, the patient’s condition was deteriorated. She had risen body temperature to a maximum of 106 F. Paracetamol was added 1gm 6 hourly and Antibiotics were upgraded to meropenem and clindamycin, ornidazole. Blood investigations revealed a total count of 13,700/mm3 and deranged liver function with total bilirubin of 3.4, direct bilirubin of 2, alanine transaminase of 150, aspartate aminotransferase of 175, and serum albumin of 2.3. The ionotropic requirement was further increased and the patient’s condition was not favorable in terms of hemodynamic stability, hence was kept on ventilator support with delayed weaning.
On the 7th postoperative day, an electrocardiogram (ECG) showed ST-segment elevation with troponin I, and CK-MB, elevated aspirin and clopidogrel were added and the patient was advised to undergo urgent cardiac intervention, but the patient’s next of kin opted for conservative management because of age factor. Unfortunately, the patient died on the 8th postoperative day.
Conclusion and Discussion
Pyometra is theorized to develop as a result of interference with the natural drainage of the uterus and is commonly caused by malignant or benign tumors, radiation cervicitis, atrophic cervicitis, puerperal infections, and congenital anomalies [1]. Streptococcus species, Bacteroides fragilis, and Escherichia coli are the most common organisms isolated in pyometra [2]. The typical symptoms of pyometra include uterine enlargement, cramping, vaginal discharge, acute abdominal pain, and postmenopausal bleeding [3]. Spontaneous perforation of a pyometra is an uncommon complication, establishing a preoperative diagnosis of pyometra is difficult because the classic symptoms of vaginal discharge, lower abdominal pain, and uterine enlargement are all nonspecific. It is especially challenging to diagnose in the case of an emergency presentation [4].
A postmenopausal lady of age 74 yrs was admitted in the emergency department with the symptoms of generalized pain abdomen for 3 days and intermittent fever since 5 days, with normal pervaginal discharge and no postmenopausal bleeding. Because of the nonspecific symptoms, it was difficult to make a probable diagnosis at the initial phase.
After exploratory laparotomy, there was perforation on the anterior fundus of the uterus. Hence, the diagnosis of spontaneous perforation of pyometra was made intraoperatively. The endometrium was damaged with multiple areas of hemorrhage and necrotic spots with brown-black discoloration. There was no evidence of malignancy on histopathological tests. The culture of the purulent fluid in the peritoneal cavity showed no growth of the organism. Histopathological reports were suggestive of pyometra and chronic cervicitis with acute salpingitis.
Most of the finding of our case is similar to the previous reports and researches. Henriksen noted 7 cases of spontaneous perforation among 208 patients with pyometra and uterine cancer in 1956. Only 15 other cases have been documented, four of which were associated with malignant tumors of the uterus or other organs, and ten were without malignancy. In six patients (40%), plain abdominal X-ray films showed free air in the subphrenic space, and anaerobic bacteria were grown by culture of the peritoneal fluid in seven cases [2-5]. Spontaneous perforation of the uterus usually occurs at a site of degenerative or necrotic change after pyometra develops due to the impairment of natural drainage via the cervix. Generalized peritonitis due to the spontaneous perforation of pyometra is very rare, and only a few cases are reported. However, in our case we did not find any evidence of malignancy and growth of any organism in the peritoneal fluid.
A pneumoperitoneum associated with a ruptured pyometra is recognized only in less than 30% of cases [6]. The presence of free intraperitoneal and intrauterine air may be due to gas-forming organisms such as Escherichia coli and Bacteroides fragilis. The passage of air through the hemodynamic parameters of the genital canal into the peritoneal cavity is also well documented [7]. GI perforation is the cause of pneumoperitoneum in 85–95% of cases and requires surgical intervention as its definitive management [8,9]. In our report, there was no specific bacterial culture growth from the sample received at laparotomy.
As illustrated by Shapey et al. [8], while CT is often indicated in such circumstances, it may be difficult to accurately make a radiological diagnosis of spontaneously perforated pyometra, especially when imaging is reviewed in the acute setting and often not by a specialist abdominopelvic radiologist. Gynecological sonography may be the most adequate to illustrate fluid accumulation in utero, despite the absence of gynecological symptoms in most cases. Ultrasonography is the first and most sensitive examination for the evaluation of pyometra but has a limited role in the diagnosis of perforated pyometra [10]. Likewise, in our case we did the ultrasonography and CT scan before the exploratory laparotomy, but the radiological diagnosis was not that clear and confirm, thus the treating team decided to go for surgery.
Perforated pyometra cases should be treated with total abdominal hysterectomy with bilateral salpingo-oophorectomy, thorough drainage and irrigation of the pelvic abdominal cavity, postoperative intensive care support, and administration of broad-spectrum antibiotics. It highlights the importance of multidisciplinary involvement in treating sepsis [11]. Similarly, to the above recommendation, we treated the case with total abdominal hysterectomy with B/L salphingo-oopherctomy. Postoperatively she was managed with broad spectrum antibiotics and resuscitation and a multidisciplinary approach. As previous evidence showed, mortality from spontaneously performed pyometra exceeds 40% [11], in our case despite all treatment and management provided according to the protocol, unfortunately we could not save the patient and she died on the 8th postoperative day.
Informed Consent
Was taken from a relative of the patient and can be provided on request.
References
- Henriksen PT (1956) Pyometra is associated with malignant lesions of the cervix and uterus. Am J Obstet Gynecol 72(4): 884-895.
- Ikeda M, Takahashi T, Kurachi H (2013) Spontaneous perforation of pyometra: a report of seven cases and review of the literature. Gynecol Obstet Invest 75(4): 243-249.
- Hansen PT, Lindholt J (1985) Spontaneously perforated pyometra: a differential diagnosis in acute abdomen. Ann Chir Gynaecol 74(6): 294-295.
- Sussman AM, Boyd CR, Christy RS, Rudolph R (1989) Pneumoperitoneum and an acute abdominal condition caused by spontaneous perforation of a pyometra in an elderly woman: a case report. Surgery 105(2 Pt 1): 230-231.
- Yildizhan B, Uyar E, Sismanoglu A, fulluoglu GG, Kavak Z, et al. (2006) Spontaneous perforation of pyometra. Infect Dis Obstet Gynecol 2006: 2676.
- Omori H, Asahi H, Inoue Y, Irinoda T, Saito K, et al. (2003) Pneumoperitoneum without perforation of the gastrointestinal tract. Dig Surg 20(4): 334-338.
- Ou YC, Lan KC, Lin H, Tsai CC, Changchien CC, et al. (2010) Clinical characteristics of perforated pyometra and impending perforation: specific issues in a gynecological emergency. J Obstet Gynaecol Res 36(3): 661-666.
- Shapey M, Nasser T, Dickens P, Haldar M, Solkar MH, et al. (2012) Spontaneously perforated pyometra: an unusual cause of acute abdomen and pneumoperitoneum. Ann R Coll Surg Engl 94(8): e246-e248.
- Roh JJ, Thompson JS, Harned RK, Hodgson PE (1983) Value of pneumoperitoneum in the diagnosis of visceral perforation. Am J Surg 146(6): 830-833.
- Huang Y, Tian Q (2018) Postmenopausal spontaneous rupture of pyometra: A case report. Medicine (Baltimore) 97(52): e13659.
- Yamada T, Ando N, Shibata N, Suitou M, Takagi H, et al. (2015) Spontaneous perforation of pyometra presenting as acute abdomen and pneumoperitoneum mimicking those of gastrointestinal origin. Case Rep Surg 2015: 548481.






























