Prevalence and Determinants of Female Genital Mutilation at Beni-Suef
Momen Zakria Mohammed1, Hanan Elzeblawy Hassan2*, Fatima Hosny Abd-ELhakam1 and Rasha El-Syed Ebrahim1
1Lecturer of Obstetrics & Gynecology, Faculty of Medicine, Beni-Suef University
2Maternal and Newborn Health Nursing, Faculty of Nursing, Beni-Suef University, Egypt
Submission: December 02, 2022; Published: December 16, 2022
*Corresponding author: Hanan Elzeblawy Hassan, Maternal and Newborn Health Nursing, Faculty of Nursing, Beni-Suef University, Egypt
How to cite this article: Momen Z M, Hanan E H, Fatima H A-E, Rasha E-S E. Prevalence and Determinants of Female Genital Mutilation at Beni-Suef. J Gynecol Women’s Health 2022: 24(3): 556138. DOI: 10.19080/JGWH.2022.24.556138
Abstract
Background: Female genital mutilation is defined as a standard and cultural procedure that has all procedures that involve partial or complete removal of the external female genitalia, or other injuries to the female genital organs for non-medical reasons.
Aim: The aim of this study was assessed prevalence, determents, effect of female genital mutilation at Beni-Suef.
Subject & Methods: A descriptive cross-sectional study was used. The study population consisted of 2837 females in family health centers (FHCs) in different sitting at Beni-Suef. Α Structured Interviewing Questionnaire sheet was used to collect data.
Results: prevalence of Female Genital Mutilation (FGM/C) among total participants was 71.4%, 51% of them the mother was the person responsible for the mutilation decision. FGM is usually performed at home (62.3%), by doctors (55.6%), 51.3% of the females did not know the type of FGM/C they were exposed to. About 29.7% of participants are suffering from complication after FGM.
Conclusion & Recommendations: The prevalence of FGM/C is still high despite the health consequences of the procedure. Mothers were the main person that responsible for the FGM/C decision. The procedure of FGM is usually performed by doctors or nurse at home. A proportional percentage suffered from complication after FGM. An educational program for mothers about FGM is required to increase their awareness should be developed and disseminated.
Keywords: Prevalence; Determinants; Female genital mutilation; Family health centers; Infibulation
Abbreviations: FGM: Female Genital Mutilation; FHCs: Family Health Centers; EFHS: Egyptian Family Health Survey; WHO: World Health Organization; SYPE: Survey of Young People in Egypt
Introduction
Female genital mutilation has been defined by the World Health Organization as a standard and cultural procedure that has all procedures that involve partial or complete removal of the external female genitalia, or other injuries to the female genital organs for non-medical reasons [1-4]. Additionally, to have no health benefits, FGM interferes with normal body functions and may harm several aspects of a girl’s or woman’s life, including her physical, mental, and sexual health and her relationship together with her husband or partner and other close family members [5-7]. To determine the prevalence of FGM/C, many types of research were carried out in Egypt. According to research, FGM/C was found to be prevalent in majority of Egyptian females between the ages of 13-19 who had never been married [8-10]. The prevalence of FGM/C was reported to be half of females in a survey of schoolgirls across Egypt [11-12]. According to the Egyptian Family Health Survey (EFHS), in 2021, majority of Egyptian married women between the ages of 15 and 49 had undergone FGM. The World Health Organization (WHO) classifies the mutilation of the female genital into four distinct categories [13]. Three of the four categories are further attenuated into subcategories that classify the particular form of mutilation that was performed [1].
Type I
It includes the partial or total removal of the clitoris and/or prepuce. It has two main subtypes; type Ia which involves the removal of the prepuce and is called circumcision and sort Ib which involves the removal of the clitoris and therefore the prepuce and is termed clitoridectomy. Type I is known as “Sunna Circumcision”; a spiritual term linking the practice to the commands of the Prophet of Islam or “Khifad” the Arabic synonym of “reduction”; a term claiming that the Prophet of Islam endorsed partial instead of complete excision of the external genitalia [14,15]. In Egypt, types I and II also are called “Tahara”; the Arabic synonym of “purification” which points to the hygienic drive of the practice [16-17].
Type II
It includes the partial or total removal of the clitoris and therefore the labia minora with or without excision of labia majora. It also has three subtypes which are type IIa which involves removal of labia minora only, type IIb which involves partial or total removal of the clitoris with labia minora (sometimes the prepuce is affected as well) and type IIc which involves removal of the clitoris and both labia minora and Majora.
Type III
It’s also called infibulation. This kind includes the narrowing of the opening of the vagina and the creation of a seal covering by excision and repositioning of the labia minora or majora.
The clitoris and therefore the prepuce could be excised. Type III includes two subtypes: type IIIa which involves repositioning of labia minora and type IIIb which involves repositioning of labia majora after narrowing of the vaginal opening.
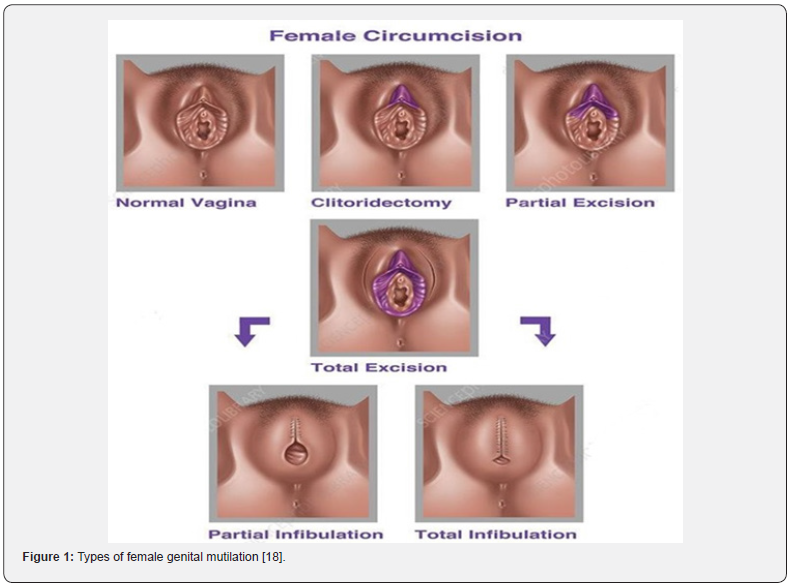
Type IV
It includes other harmful procedures done to the female genitalia for non-medical causes like piercing, incising, pricking, cauterization or scraping. De-infibulation is the reverse of infibulation which is completed surgically by cutting the closed vagina and removal of the genital scar tissues to enhance the wellbeing of females and permit sexual activity also as easiness of the childbirth process (Figure 1) [18] . Medicalization is defined by the World Health Organization (WHO) as “the circumstance in which FGM/C is performed by any health care practitioner, whether in a public or private health facility, at home, or anywhere else.” It encompasses all forms of FGM/C that include re-infibulation at any point in a woman’s life (United Nations Population Fund) [19,20]. Physicians, nurses, midwives, trained birth attendants, obstetricians, plastic surgeons, and others involved in delivering medical services to patients are among those participating in medicalized FGM/C [21].
Aim of the Study
The present study was carried find out about FGM in Beni-Suef Governorate through:
a) Assess Prevalence of Female Genital Mutilation at Beni- Suef
b) Assess determinants of Female Genital Mutilation at Beni-Suef
c) Assess effects of FGM at Beni-Suef
Research Questions
1. What is the prevalence of FGM at Beni-Suef?
2. What are the determinants of Female Genital Mutilation at Beni-Suef?
3. What are the effects of FGM on female life?
Subjects and Methods
Research Design
A Descriptive Cross-sectional study was used to achieve the aim of the current study
Subjects & Setting
Setting: The study was conducted in family health centers (FHCs) in different sitting at Beni-Suef Governorate.
Sample
Sample Type: A Convenient sample was used. The study sample was selected according to the following Inclusion criteria: 18-60 years old women; Can read and write.
Sample size: The study population consisted of all females (2837) who were accepted to participate in the study at the time of data collection (A period of six months from the start of data collection) and will be included in the study.
Tools of Data Collection: A pre-designed structured questionnaire was used to collect data. Data were collected through personal interviews.
The questionnaire is divided into three sections:
Section I: Prevalence of Female Genital Mutilation (FGM/C) among total participant women.
Section II: Determinants of Female Genital Mutilation at Beni-Suef as: Age at circumcision, who took the decision? Place at which performed, Medical examination before the procedure, Who perform it?, and types of circumcision.
Section III: Complications of Female Genital Mutilation (FGM/C) among the participant women.
Validity of the Tool: It was established by panel of experts from obstetrics and gynecological nursing and obstetrics and gynecological medicine and review of related literature for clarity, relevance, comprehensiveness, understanding, applicability and easiness.
Ethical Considerations: An oral consent accordingly to conduct the study was taken from each studied women to protect their rights before the start of the study. They were informed that they could withdraw at any time. A unique identifying number (subject ID) was assigned to the data collected from each woman to maintain confidentiality.
Administrative Considerations: Official permission was obtained by submission of an official letters from the Faculty of Nursing, Beni-Suef University to the responsible authorities of the study setting (family health centers (FHCs)) to obtain their permission for data collection for our study. These letters provided the study’s goal as well as photocopies of data collecting materials to obtain their consent and assistance with data collection.
Pilot Study: A pilot study was implemented on 10% of study participant included in the study to ascertain the relevance of the tools and estimate the length of the time needed to fill the sheet. Analysis of the pilot study revealed that minor modifications are required. These modifications were done, and women included in the pilot study were included in the total sample.
Field Work: Data were gathered over six months beginning in November 2021 and ending in April 2022. The researcher was present at the previously mentioned location until the entire sample size was gathered. Before data collection, the researcher introduced herself to the women and explained the purpose of the study.
Statistical Analysis: All data were collected, tabulated and statistically analyzed using IBM SPSS 25. Data was supplied, and appropriate analysis was performed for each parameter based on the type of data obtained.
Descriptive Statistics data were expressed as
a) Count and percentage: Used for describing and summarizing categorical data
b) Arithmetic mean (X-), Standard deviation (SD): Used for normally distributed quantitative data, these are used as measurements of central tendency and dispersion.
Analytical Statistics: Cronbach alpha and Spearman-Brown coefficients: The internal consistency of the generated tools was measured to assess their reliability.
Graphical presentation: Data visualization was done with Bie in 3D chart graphs.
Result
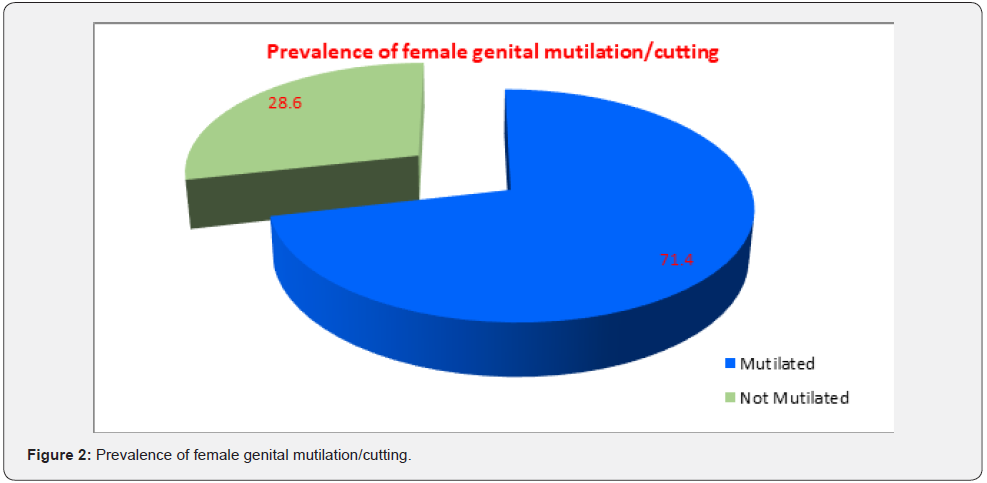
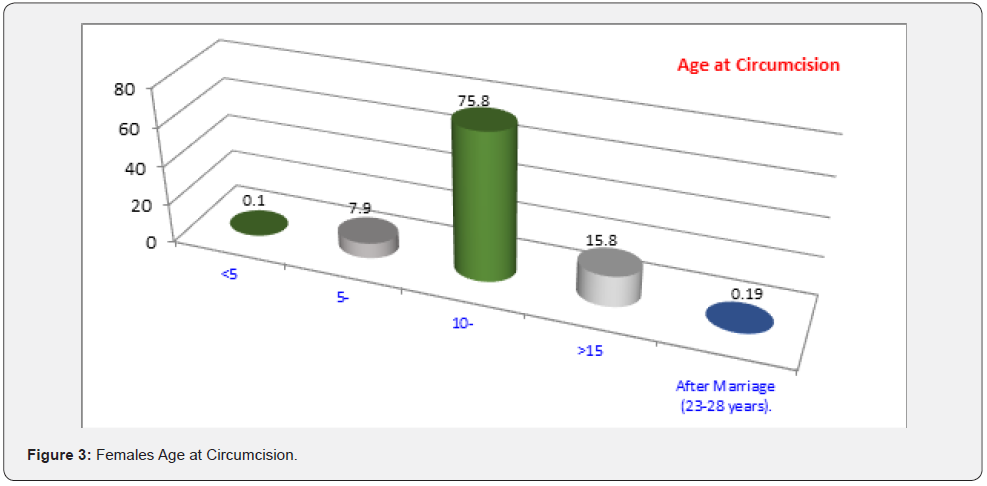
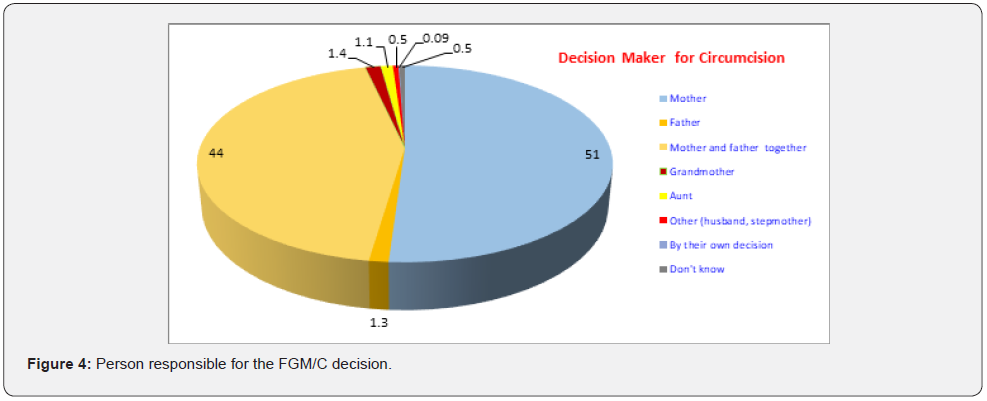
(Figure 2) Shows that the prevalence of Female Genital Mutilation (FGM/C) among total participants (2837) at Beni- Suef is 71.4%. (Figure 3) Presented the distribution of females aged 18-60 years according to their age at their mutilation. The percentage of those who had been mutilated was 15.8% at over 15 years old, compared to 75.8% of those who had been mutilated between the ages of 10 to 15, and 7.9% of those who had been mutilated between the ages of 5-10. Only 0.1% of the females under the age of five (2-3 years) have female genital mutilation. It is worth mentioning that 4 of the participants were mutilated after her marriage their ages ranged between 23-28 years. (Figure 4) Portrayed the distribution of mutilated females’ aged18-60 years according to the person responsible for the FGM/C decision. It shows that more than half of mutilation cases (51%), the mother was the person responsible for the mutilation decision, and in 44% both parents were responsible for the mutilation decision. Only 2 of the participants were mutilated by her decision.
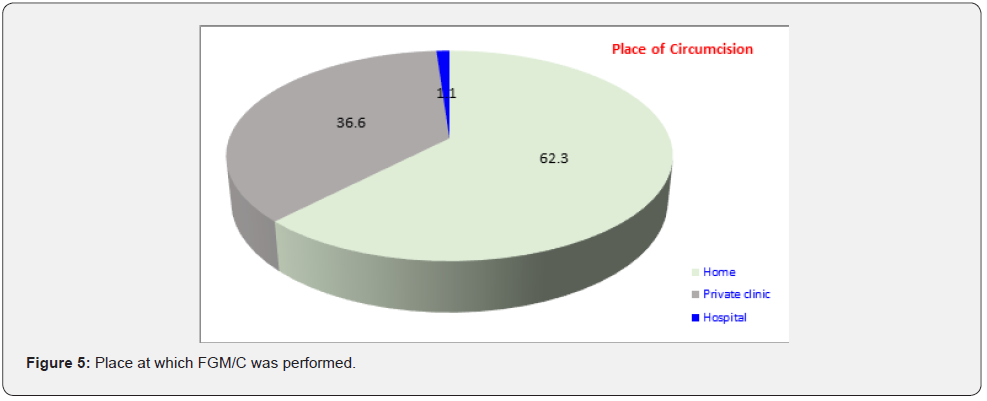
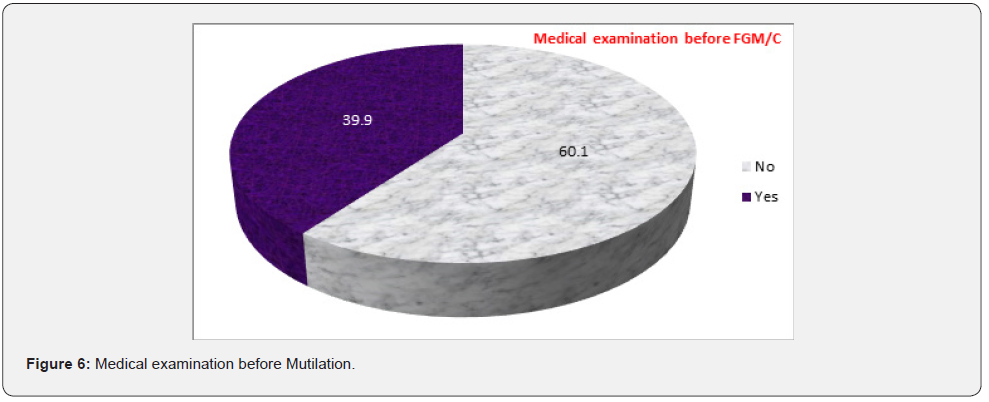
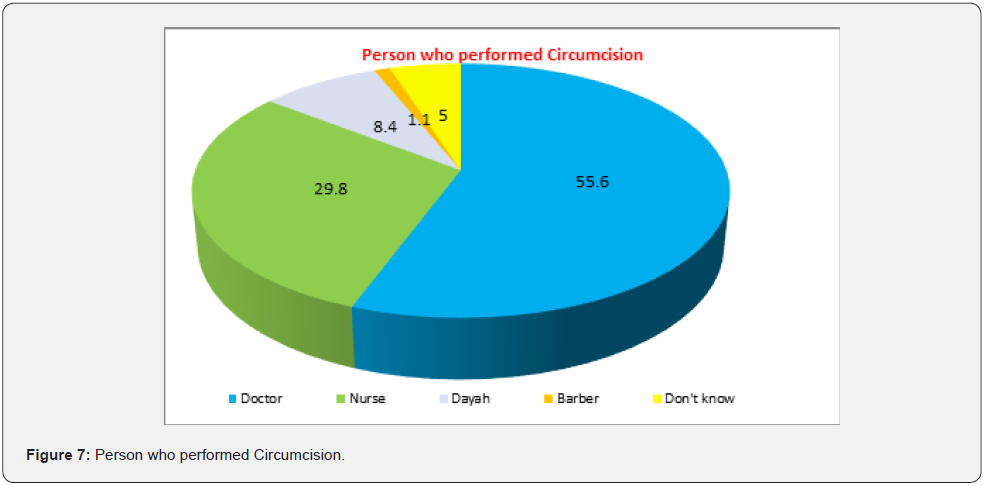
(Figure 5) Presented the distribution of mutilated females aged 18-60 years according to the place at which FGM/C was performed. The procedure of FGM is usually performed at home 62.3% followed by private clinics 36.6%. (Figure 6) Portrayed the distribution of mutilated females aged 18-60 years according to if medical examination was done before the procedure. Among participants, 39.9% were medically examined by physicians or other mutilators to know whether they needed to be mutilated or not. (Figure 7) Presented the distribution of mutilated females aged 18-60 years according to the person performing the FGM/C. It shows that doctors were the most common person performing the mutilation (55.6%), followed by nurse (29.8%), dayah (8.4%), barbers (1.1%), and 5% of the participants don’t know the person performing mutilation.

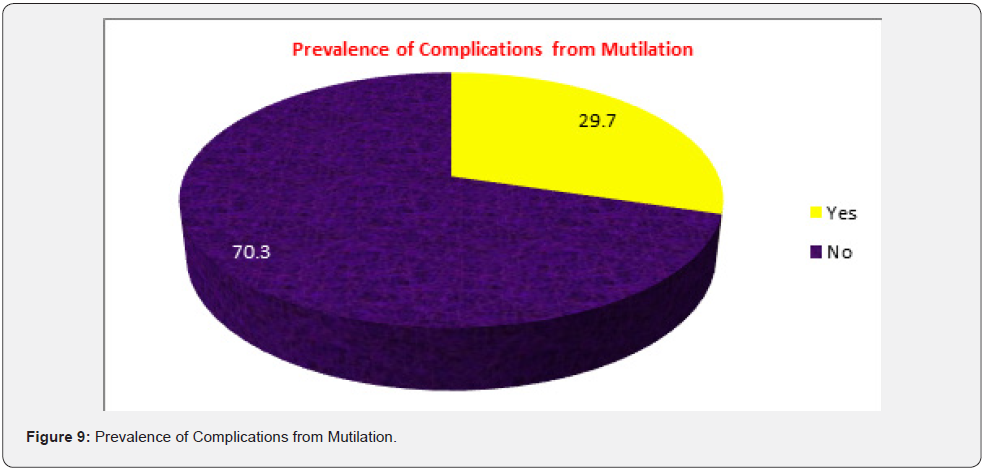
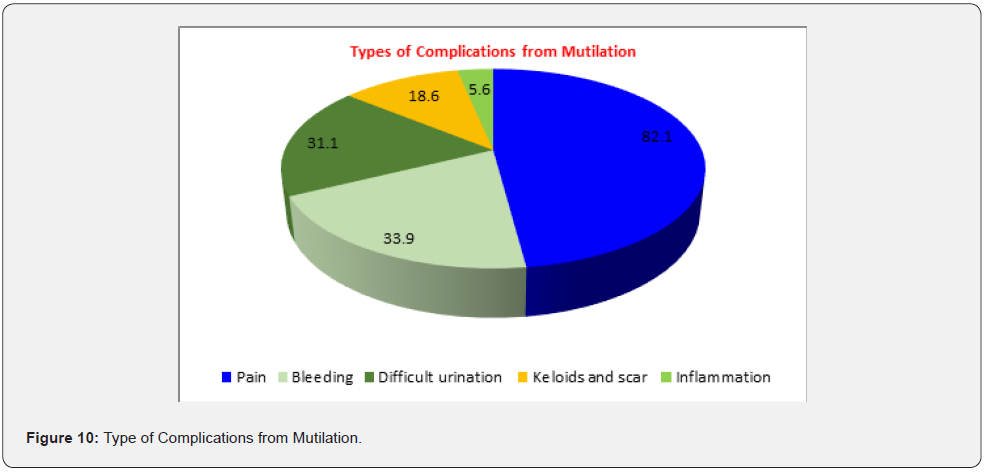
(Figure 8) Presented the distribution of mutilated females aged 18-60 years according to type of FGM/C that the participants were exposed. Regarding the type of FGM/C, 51.3% of the females did not know the type of FGM/C they were exposed to, 16.2% faced Sunni FGM/C (clitoridectomy), and 3.5% faced excision FGM/C and 0.3% underwent pharaonic FGM/C (infibulation). (Figure 9) Portrayed the distribution the prevalence of complications from the mutilation among participant sample. About 29.7% of participants are suffering from complication after FGM. (Figure 10) Showed the distribution types of complications from the mutilation among participant sample. About 82.1% of them suffering from pain after the surgery, also 33.9% mentioned severe bleeding, 31.1% suffers from difficult micturition and about 18.6 have a keloid and scar from the mutilation.
Discussion
Female genital mutilation/cutting is still one of the largest public health issues in Egypt and its governorates, despite the efforts made by the Egyptian government to eradicate it. The prevalence of FGM in the present study was lower than the prevalence of FGM/C stated in the latest study reported by Abd- ELhakam [15]. The results of the current study showed that the prevalence of Female Genital Mutilation (FGM/C) among total participants at Beni-Suef is 71.4%. The prevalence of FGM/C discovered in the current study was in line with that of FGM/C reported in studies carried out nationally and internationally.
Firstly, at the international level; results were in in line with results in southern Iran by [22], Kurdistan Iraq by [23] and Sudan by [24]. Sudan is one of the foremost practicing FGM/C countries . Nearly 12 million females were found to possess undergone FGM/C constituting; 9% of the mutilated females worldwide with a prevalence of FGM/C of 87% (50%-90%) and approximately two-thirds of them had undergone type III FGM/C. In Mauritania, the prevalence of FGM/C is 67% [20]. However, results of current study are higher than other Arabian countries. In Oman, the prevalence of FGM/C isn’t known. Some suggested that the prevalence of FGM/C among Omani females is around 20- 30% [25]. In the United Arab Emirates (UAE), the prevalence of FGM/C was 41.4% among Emirate females with a decrease in the prevalence among the younger generations [26].
In Yemen, and Iraq, the prevalence of FGM/C is 19%, and 8%, correspondingly [20]. In Saudi Arabia, no reliable data exist about FGM, and therefore the prevalence reports are lacking. The prevalence and regional localization of FGM are anecdotally reported, mostly among migrant populations and within the southern region of Saudi Arabia. As an example, a teaching hospital study in Jeddah found that 41.5 percent of participants suffering from FGM were Saudi women [27]. The variation in prevalence between the current study and that study could be explained by the difference in the criteria of included participants, various sample sizes, and variable places of the studies. Additionally, schoolgirls might not yet be of mutilation age. On the other hand, it was lower than the prevalence reported in Minia [28], El-Beheria Governorate [29], Luxor [30], Slum [31], Suhag [32], Oman [33], and different regions in Ethiopia [34], Sudan [35], and Somalia [36].
Secondly, at a national level; According to a survey conducted among students at Beni-Suef University (2018), FGM/C is prevalent among female students. FGM was performed on slightly less than half of our students (47.3%). FGM/C was more common in students who lived in rural regions or had illiterate parents [15]. Moreover, Benha city reported by [37], Assiut and Fayoum by [30], Kafr El Sheikh by [31]. However, the result of the current study was substantially higher than the prevalence that reported in the UAE, and Iran [38]. Results of the current study revealed that the minority of those who had been mutilated was over 15 years, compared to majority of those who had been mutilated between the ages of 10 and 15, and near to tenth of those who had been mutilated between the ages of 5-10.
Only zero point one of the females under the age of five (2-3 years) have female genital mutilation. The mean age at the time of mutilation was greater in the current study compared to studies in conducted Ethiopia [39], southern Iran [22], and El-Mansoura Center, El-Dakahlia among school girls [23], respectively. About three fourths of those had been mutilated between the ages of 10 and 15 years. These findings were comparable to the WHO report, which demonstrates that FGM/C is performed on women of any age, from infancy through marriage, but most commonly between the ages of 4 and 10 before puberty [40]. According to the Survey of young people in Egypt (SYPE), mutilation was performed at a younger age in Upper Egypt compared to the urban governorates and Lower Egypt for females [41]. However, data demonstrates that most Egyptian females are mutilated before puberty [21]. Regarding the mutilation decision, in more than half of mutilated cases, the mother was the person responsible for the mutilation decision. This was lower than the results of [42] who reported that mothers were responsible for FGM/C decisions.
The disparities in the demographics of the individuals and study sites may account for this [42]. On the other hand, in the current study, a higher percentage of females said that both parents had decided to have FGM or C. Research in the Somali and Harari societies of eastern Ethiopia found that mothers decide to circumcise their daughters and play a significant part in the procedure. Female circumcision never involves men [43]. The study also reported that two of the participants themselves decided to undergo FGM/C. This was lower than the results of Alradie, et al. [43] who reported that five percent of the samples were mutilated by her decision. In the current study, medical professionals carried out majority of the FGM/C procedures (physicians and nurses). However, the rate was comparable to the study conducted in Upper Egypt, which showed that girls were mutilated by medical professionals of nurses, young physicians, and senior physicians, respectively [44].
This was in line with UNICEF, 2018. These are the nations with the highest frequency of medicalized FGM/C. Egypt (78 percent), Sudan (77 percent), Guinea (31 percent), Djibouti (21 percent), Kenya (20 percent), Iraq (14 percent), Yemen (13 percent), and Nigeria (12 percent) [20]. Moreover, UNICEF reported that FGM is most commonly performed by health care providers in Egypt and Sudan, with doctors doing the procedure in Egypt and midwives performing the procedure in Sudan. In Egypt alone, 1.5 million girls and women have had their hair cut by health care providers, 1.2 million of whom have had their hair trimmed by doctors [20]. Regarding the type of FGM: more than half of the participants of the females did not know the type of FGM/C they were exposed to. Among those who knew, type I was the most commonly reported type, followed by type II. Only zero point three underwent pharaonic FGM/C (infibulation). The same outcomes were confirmed by other studies in Egypt [45-47]. The most frequent type of FGM/C in the United Arab Emirates study was type I, followed by Type II and Type III. According to a study conducted in Southern Iran, type I FGM/C and clitoral nicking were the two most common [48-49].
The majority of participants in the [50] study in Ethiopia had type I FGM/C, followed by type III, while more than half of participants in the Hussein et al. [51] study had type III FGM/C [50,51]. Type I FGM/C is more frequently used than type II in cultures where it is practiced. About nearly one-third of participants in the current study are suffering from complications after FGM. This was less than a study conducted in Sierra Leone where the majority of respondents reported complications of FGM [52]. About majority of them suffer from pain after the surgery, also one third have severe bleeding, near to one third suffer from difficult micturition and about one-fifth have a keloid and scar from the mutilation. These complications, including pain, heavy bleeding during the surgery, and trouble urinating, were also mentioned in the Nigerian study [53-57]. Contrarily, research carried out in Ethiopia revealed that During the operation, there were several immediate problems, including severe bleeding, infection, urinary incontinence, and genital organ enlargement [39].
Conclusion and Recommendations
The prevalence of FGM/C is still higher despite the health consequences of the procedure. Type I and Type II FGM/C procedures are the most typical ones carried out in Egypt. Mothers were the main person that responsible for the FGM/C decision. The procedure of FGM is usually performed by doctors or nurse at home. A proportional percentage suffered from complication after FGM. An educational program for mothers about FGM is required to increase their awareness should be developed and disseminated.
References
- (2018) Care of girls and women living with female genital mutilation: A clinical handbook. World Health Organization (WHO).
- Hassan H, Abd-ELhakam F, Ebrahim R, Mohammed M (2022) Call for Change Enhancement Upper Egyptian Females' Knowledge Regarding Effect of Female Genital Mutilation. American Journal of Public Health Research 10(5).
- Abd-ELhakam F, Ebrahim R, Mohammed M, Hassan H (2022) Relationship between Socio Demographic Data and Female Genital Mutilation. Archives of Medical Case Reports and Case Study 6(4).
- Ebrahim R, Mohammed M, Hassan H, Abd-ELhakam F (2022) Relationship between Personal Characteristics and the Person Performing Female Genital Mutilation. Journal of Community Medicine and Public Health Reports.
- Hassan H, Abd-ELhakam F, Ebrahim R, Mohammed M (2022) Prevalence of Female Genital Mutilation in Northern Upper Egypt. American Journal of Nursing Research 10(3).
- Abd-ELhakam F, Ebrahim R, Mohammed M, Hassan H (2022) Female Genital Mutilation: Females' Related Knowledge. Biomedical Research and Clinical Reviews 7(2).
- Abd-ELhakam F, Ebrahim R, Mohammed M, Hassan H (2022) Female Genital Mutilation: Relationship Association between Upper Egyptian Females' Knowledge and Attitude. American Journal of Medical Case Reports 10(12).
- Ibrahim B, Sallam S, El Tawila S, El Gibaly O, El Sahn F, et al. (1999) Transitions to adulthood: a national survey of Egyptian adolescents. Cairo: Population Council 7(2): 25-30.
- Mohammed M, Abd-ELhakam F, Hassan H, Ebrahim R (2022) Study Females' Intention to practice Female Genital Mutilation for their daughters at Beni-Suef. Public Health Open Access 6(2).
- Hassan H, Abd-ELhakam F, Ebrahim R, Mohammed M (2022) Female Genital Mutilation: Females' Intention in Northern Upper Egypt. Journal of Obstetrics Gynecology and Reproductive Sciences 6(4).
- Tag-Eldin MA, Gadallah MA, Al-Tayeb MN, Abdel-Aty M, Mansour E, et al. (2008) Prevalence of female genital cutting among Egyptian girls. Bull World Health Organ 86 (4): 269-274.
- Abd-ELhakam F, Hassan H, Ebrahim R, Mohammed M (2022) Relationship between Females' Intention of Mutilating Their Daughters and Demographic Characteristics, Journal of Psychology and Neuroscience 4(3).
- (2016) Sexual and reproductive health: health risks of female genital mutilation (FGM). World Health Organization (WHO).
- Hassan H, Ebrahim R, Mohammed M, Abd-ELhakam F (2022) Female Genital Mutilation: Impact on Knowledge, Attitude, Sexual Score Domains and Intention of Females in Northern Upper Egypt. Archives of Medical Case Reports and Case Study 6(4).
- Abd-ELhakam F (2022) Prevalence of Female Genital Mutilation at Beni-Suef Governorate, Egypt. [Master's Disseration, Beni-Suef University]. Beni-Suef.
- Cetorelli, V, Wilson B, Batyra E, Coast E (2020) Female genital mutilation/cutting in Mali and Mauritania: understanding trends and evaluating policies. Studies in family planning 51(1): 51-69.
- Ebrahim R, Abd-ELhakam F, Hassan H, Mohammed M (2022) Relationship between Females' Knowledge and Attitude and Intention of Female Genital Mutilation. Research in Psychology and Behavioral Sciences 10(1): 2333-438X.
- Abdulcadir J, Catania L, Hindin MJ, Say L, Petignat P, et al. (2016) Female genital mutilation: A Visual Reference and Learning Tool for Health Care Professionals. Obstet Gynecol 128(5): 958-963.
- United Nations Population Fund [UNFPA] (2018) UNFPA-UNICEF joint program to eliminate female genital mutilation. UNFPA
- (2018) At least 200 million girls and women alive today living in 30 countries have undergone FGM. UNICEF.
- El-Gibaly O, Aziz, M, Abou Hussein S (2019) Health care providers’ and mothers’ perceptions about the medicalization of female genital mutilation or cutting in Egypt: a cross-sectional qualitative study. BMC Int Health Hum Rights 19(1): 26.
- Dehghankhalili M, Fallahi S, Mahmudi F, Ghaffarpasand F, Shahrzad ME, et al. (2015) Epidemiology, regional characteristics, knowledge, and attitude toward female genital mutilation/cutting in southern Iran. The Journal of Sexual Medicine 12(7): 1577-1583.
- Yasin BA, Al-Tawil NG, Shabila NP, Al-Hadithi TS (2013) Female genital mutilation among Iraqi Kurdish women: a cross-sectional study from Erbil city. BMC Public Health 13: 809.
- Sharfi A, Elmegboul M, Abdella A (2013) The continuing challenge of female genital mutilation in Sudan. African Journal of Urology 19(3): 136-140.
- Thabet H, Al-Kharousi A (2018) Female Genital Mutilation in the Middle East: Placing Oman on the Map. National and University Library of Iceland 13: 11-76.
- Al Awar S, Al-Jefout M, Osman N, Balayah Z, Al Kindi N, et al. (2020) Prevalence, knowledge, attitude, and practices of female genital mutilation and cutting (FGM/C) among the United Arab Emirates population. BMC Women's Health 20(1): 79.
- Aldosari H (2017) The effect of gender norms on women's health in Saudi Arabia. Washington, DC: Arab Gulf States Institute in Washington, USA.
- Yount KM (2003) Diverging Prevalence of Female Genital Cutting. Isim Leiden 12(1): 36-37.
- Abd Elwahed AY, Ali WK, Ghattas VN (2019) Experience of Female Genital Cutting and Sexual Satisfaction Among Rural Married Women in El Beheria Governorate. International Journal of Studies in Nursing 4(1): 46.
- EL-Gharib MN (2019) Female genital cutting: A persistent African health challenge. Gyne and Obste Open A Open J 1(1): 1-6.
- Abdou MS, Wahdan IM, El-Nimr NA (2020) Prevalence of Female Genital Mutilation, and Women’s Knowledge, Attitude, and Intention to Practice in Egypt: A Nationwide Survey. Journal of High Institute of Public Health 50(3): 139-145.
- Yousef F, Hamed A, Mostafa N (2017) Female genital cutting: prevalence, knowledge, and attitudes of Sohag University level students, Upper Egypt. Egyptian Journal of Community Medicine 35(1): 17-25.
- Al-Hinai H (2014) Female genital mutilation in the Sultanate of Oman. Stop FGM Middle East 1(1): 26.
- Abdisa B, Desalegn M, Tesew A (2017) Assessment of the prevalence of FGM and associated factors among women’s of reproductive age group in Kebirbeyah Town, Somali Region Eastern Ethiopia. Health Science Journal 11(4): 1-9.
- Elduma A H (2018) Female genital mutilation in Sudan. Open access Maced J Med Sci 6(2): 430-434.
- Adiguzel C, Baş Y, Erhan MD, Gelle MA (2019) The female genital mutilation/cutting experience in Somali women: their wishes, knowledge, and attitude. Gynecol Obstet Invest 84(2): 118-127.
- Elnashar A, Abdelhady R (2007) The impact of female genital cutting on health of newly married women. Int J Gynecol Obstet 97(3): 238-244.
- Bahrami M, Ghaderi E, Farazi E, Bahramy A (2018) The prevalence of female genital mutilation and related factors among women in Kamyaran, Iran. Chronic Diseases Journal 6(3): 113-119.
- Bogale D, Markos D, Kaso M (2014) Prevalence of female genital mutilation and its effect on women’s health in Bale zone, Ethiopia: a cross-sectional study. BMC Public Health 14: 1076.
- (2020) Female genital mutilation. World Health Organization (WHO).
- Roushdy R, Sieverding M (2015) Panel Survey of Young People in Egypt (SYPE) 2014: Generating evidence for policy, programs, and research.
- Yasin YA (2014) Prevalence of female genital mutilation among schoolgirls in El Mansoura Center, El-Dakahlia Governorate, Egypt. IOSR Journal of Dental and Medical Sciences 13: 11-76.
- lradie-Mohamed A, Kabir R, Arafat SM (2020) Decision-making process in female genital mutilation: a systematic review. Int J Environ Res Public Health 17(10): 3362.
- Rasheed SM, Abd-Ellah AH, Yousef FM (2011) Female genital mutilation in Upper Egypt in the new millennium. Int J Gynecol Obstet 114(1): 47-50.
- El-Defrawi MH, Lotfy G, Dandash KF, Refaat AH, Eyada M (2001) Female genital mutilation and its psychosexual impact. J Sex Marital Ther 27(5): 465-473.
- Hassan H, Abd-ELhakam F, Zakria M, El-sayed R (2022) Female Genital Mutilation in Northern Upper Egypt: Prospects of Reasons for Performing and Refusing. International Journal of Nursing Science 12(1).
- Mitwaly A, Abd El Aal D, Aziz P, Hassanin A, Abbas A (2017) A recent look for the implication and attitude of practicing female genital mutilation in Upper Egypt: a cross sectional study. International Journal of Reproduction, Contraception Obstetrics and Gynecology 6(10).
- Ismail K, Fadol E, Sheikh E, Mohammed H, Elkheir H (2017) The opinion and role of men in female circumcision in Khartoum State in 2015-2016. Reproductive System and Sexual Disorders 6(3): 1-15.
- Abd-ELhakam F, Ebrahim R, Mohammed M, Hassan H (2022) Relationship between Women's Intention for Female Genital Mutilation and their Exposure to Complication and Pressure. Journal of Medical Case Reports and Case series.
- Yirga WS, Kassa NA, Gebremichael MW, Aro AR (2012) Female genital mutilation: Prevalence, perceptions and effect on women's health in Kersa district of Ethiopia. Int J Womens Health 4: 45-54.
- Hussein MA, Adem A, Mohammed MA (2013) Knowledge, attitude and practice of female genital mutilation among women in Jigjiga Town, Eastern Ethiopia. Gaziantep Medical Journal 19(3): 164-168.
- Bjalkander O, Bangura L, Leigh B, Berggren V, Bergstrom S, et al. (2012) Health complications of female genital mutilation in Sierra Leone. Int J Womens Health 4: 321-331.
- Hassan H (2020) Evidence-Based Practice in Midwifery and Maternity Nursing for Excellent Quality of Care Outcomes. American Journal of Nursing Research 8(6): 606-607.
- Mandara MU (2004) Female genital mutilation in Nigeria. Int J Gynecol Obstet 84(3): 291-298.
- Hassan H, Saber N, Sheha E (2019) Comprehension of Dyspareunia and Related Anxiety among Northern Upper Egyptian women: Impact of Nursing Consultation Context Using PLISSIT Model. Nursing & Care Open Access Journal 6(1): 1-19.
- Hassan H., Mohammed M., Abd-ELhakam F., Ebrahim R. Female Genital Mutilation: Study Sexual Issues. American Journal of Nursing Research, 2023; 11(1).
- Hassan H., Abd-ELhakam F., Ebrahim R., Mohammed M. Study Females’ Attitude toward Female Genital Mutilation. Journal of Gynecology and Women’s Health, 2022, 24(3): 1-9 DOI: 10.19080/ JGWH.2022.24.556137






























