The Impact of Social Support Groups on Outcomes in Adult Patients with Type 2 Diabetes Attending Tenwek Hospital, in Bomet County
Moses Ndanyi1, John Ombogo2*, Godfrey Amalia1 and Jefferson Mutibo3
1Department, Clinical Medicine, Kakamega Medical Training College, Kenya
2Department, Nutritional Sciences, Masinde Muliro University of Science and Technology, Kenya
3Department, Diabetic Clinic, Kambiri Health Center, Kenya
Submission: November 11, 2022; Published: November 17, 2022
*Corresponding author: John Ombogo, Department, Nutritional Sciences, Masinde Muliro University of Science and Technology, Kenya
How to cite this article: Moses N, John O, Godfrey A, Jefferson M. The Impact of Social Support Groups on Outcomes in Adult Patients with Type 2 Diabetes Attending Tenwek Hospital, in Bomet County. J Gynecol Women’s Health 2022: 24(2): 556134. DOI: 10.19080/JGWH.2022.24.556134
Abstract
Diabetes is one of the fastest growing chronic diseases globally and in the United States. Although preventable, type 2 diabetes accounts for 90% of all cases of diabetes worldwide and continues to be a source of increased disability, lost productivity, mortality, and amplified healthcare costs. Proper disease management is crucial for achieving better diabetes-related outcomes. Evidence suggests that higher levels of social support are associated with improved clinical outcomes, reduced psychosocial symptomatology, and the adaptation of beneficial lifestyle activities; however, the role of social support in diabetes management is not yet well understood. The main purpose of this study is to explain and evaluate the influence of support groups and identity on goal setting and achievement in persons with type 2 diabetes. 100 hundred type 2 diabetic patients were interviewed. A structured interviewer-administered questionnaire was used to collect data. This is a descriptive study, and the data was keyed into excel. The researcher used percentages, tables and bar graphs to analyze the collected data and gave interpretations upon conclusion. Social support was associated with more optimal self-care and self-reported HbA1c outcomes. When diabetes-specific self-efficacy and distress were included as mediators, the direct path from social support became non-significant. Conversely, the indirect effects of social support through diabetes-specific self-efficacy and distress were significant across all diabetes groups and outcomes. Diabetes-specific self-efficacy and distress may be important mechanisms linking social support with diabetes self-care and clinical outcomes. Social support interventions could explore whether improving diabetes self-efficacy and decreasing diabetes distress could help improve self-care.
Keywords: Diabetes; Social support; Self-care; Diabetes distress; Self-efficacy; Health behaviour
Introduction
Burden of Diabetes
Diabetes is one of the most prevalent and fastest-growing chronic illnesses, globally affecting more than 346 million people worldwide (World Health Organization: 10 facts about diabetes 2011). It is emerging as a global epidemic due to the rapid increase in overweight, obesity, and physical inactivity. (World Health Organization: 10 facts about diabetes 2011) .The combined impact of poor awareness, insufficient access, limited services, and inadequate resources makes diabetes the leading cause of blindness, amputation, and kidney failure worldwide. (World Health Organization: 10 facts about diabetes 2011).
Cardiovascular disease (CVD) accounts for 50%-80% of deaths in people with diabetes, a number expected to rise by more than 50% in the next 10 years (World Health Organization: 10 facts about diabetes 2011. For these reasons, diabetes has become a major cause of premature illness and death in most countries and is predicted to become the seventh leading cause of death in the world by 2030. (World Health Organization: 10 facts about diabetes 2011). Additionally, diabetes accounted for 11.6% of total healthcare expenditure in 2010 (International Diabetes Federation2011). Estimated global healthcare expenditures to treat and prevent diabetes and its complications are expected to exceed US$490 billion by 2030; this equals approximately $561 billion (international dollars) by 2030(International Diabetes Federation2011).
Currently in the U.S., 25.8 million people (or 8.3% of the population) have diabetes, and 7.0 million are still undiagnosed (Centers for Disease Control and Prevention; Atlanta, GA: 2011). Nearly 1.9 million people 20 years of age or older were newly diagnosed with diabetes in 2010 in the U.S.; an estimated 79 million adults 20 years of age or older have pre-diabetes (Centers for Disease Control and Prevention; Atlanta, GA: 2011). Men and minorities-non-Hispanic Blacks, Hispanics (Mexican Americans, Puerto Ricans, and Cubans), and American Indians/Native Americans/Pacific Islanders-are more affected, as compared with women and non-Hispanic Whites, respectively (American Diabetes Association 2011). As has been observed globally, diabetes is the leading cause of complications, including heart disease and stroke, kidney failure, and no - traumatic lower-limb amputations (American Diabetes Association 2011). It is the cause of new cases of blindness among adults in the U.S. and, according to 2007 estimates, is the seventh leading cause of death in the U.S (American Diabetes Association). Regrettably, people diagnosed with diabetes have twice the risk of death of people of similar age without diabetes (Centers for Disease Control and Prevention; Atlanta, GA: 2011). Given the vast number of people affected by this chronic disease, the total estimated costs for diabetes in the U.S. are $174 billion annually. (Centers for Disease Control and Prevention; Atlanta, GA: 2011).
Although preventable, type 2 diabetes (T2DM) accounts for 90% of all cases of diabetes worldwide (Centers for Disease Control and Prevention; Atlanta, GA: 2011). Evidence shows that at least 30 min of moderate exercise, along with healthy eating habits, aids in preventing and managing diabetes and diabetes-related outcomes (Centers for Disease Control and Prevention; Atlanta, GA: 2011). These behaviours, in addition to other self-care activities such as home blood glucose monitoring, taking medications as prescribed, obtaining preventive services, and limiting alcohol intake and tobacco use, make living and adjusting to a life with diabetes more manageable. Self-management of T2DM, however, requires the assistance of multiple sources of support groups. (World Health Organization: 10 facts about diabetes 2011).
Although new treatments and technology have aided in controlling the disease in many individuals, the challenges of diabetes self-management are overwhelming for most. Diabetes is a chronic disease for which control demands patient selfmanagement (Diabetes Educator 2007; 33: 139S-144S).Selfmanagement behaviours include monitoring blood glucose levels, taking medication, maintaining a healthy diet and regularly exercising. For most patients, it is important to conduct daily foot exams. However, despite the technological and scientific advances made toward the treatment of diabetes, the American Association of Clinical Endocrinologists (2005) reports that only 1 in 3 patients with type 2 diabetes is well controlled. The American Association of Diabetes Educators suggests that only one-half of patients adhere to medication. There are relatively high levels of non-adherence in all areas of self-management behaviours. This non-adherence is perhaps due to the fact that self-management behaviours usually require changes in the patient’s daily life. (American Association of Diabetes Educators.2004).
Antimicrobial synthetic polymers have gained much popularity owing to the permanent antimicrobial activity, especially the cationic compounds which are promising candidate materials for biomedical applications. PEI (polyethylenimine) is a polycationic and antimicrobial polymer [31-35]. PEI has been utilized as drug carrier in biomedical applications because of their ability to enter cells or permeabilize cell membranes [24]. On the other hand, it has been used in gene therapy applications [36,37], filtration technologies [38] and tissue engineering [39]. Electrospinning is an effective technique which can be utilized to produce useful ultrafine bio nano textiles. Due to their large surface area, bionanotextiles have received much interest in various applications such as medical textiles, filtration and drug delivery systems [40]. In comparison to conventional wound dressing materials bionanotextiles produced by electrospinning technology have advanced properties. These properties are controlled liquid evaporation, excellent oxygen permeability and prevention of bacterial infections with ultrafine pores. Porous structure of bionanotextiles absorb wound exudates efficiently and prevent wound drying up [3].
In the literature there are many studies about electrospinning of silk fibroin, but reports on electrospinning of PEI are relatively scarce. In this study, for the first time in literature, it was aimed to fabricate PEI/fibroin antibacterial bionanotextiles serving as wound dressings with stable, non-leaching antibacterial activity. For this purpose polyethylenimine (PEI) was added to silk fibroin and hydrophilic polycationic, and antibacterial composite bio nanotextiles were fabricated by electrospinning technique. On the other hand, previous studies have demonstrated that the sulfated silk fibroin has anticoagulant activity [41,42]. Highly sulfated biomolecules such as heparin are widely used as an antimicrobial agent [43]. Also in the light of this information silk fibroin nanofibers were functionalized with sulphate group in order to test their antibacterial activity.
The morphological, chemical, thermal characterizations of bionanotextiles were done by scanning electron microscopy (SEM), Fourier transform infrared (ATR-FTIR) spectroscopy, differential scanning calorimetry (DSC), thermogravimetric analysis (TGA), respectively. Moreover, cytotoxicity studies of the bionanotextiles were performed and their antibacterial activities against Pseudomonas aeruginosa and Staphylococcus aureus were evaluated.
Results
Introduction
The results of the research project exploring the impact of social support groups on the outcome among type two diabetic patients are reported in this chapter. The analysis results are presented per study objectives and described in tables, bar charts and pie charts. The sample size for the analysis was 50 clients who are support group users and 50 who do not support group users. Qualitative data was collected and keyed in MS-excel database
Social-Demographic Characteristics
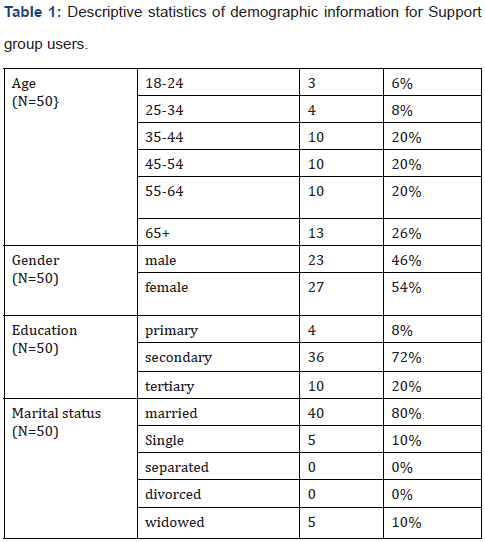
Table 1 below shows descriptive statistics of demographic information for support group users. The table 2 below shows age in years, gender, level of education and marital status. The respondents among support group users (n=50) were 46% male (n=23) and 54% (n=27) female. All age ranges were represented, however, the majority of the population was over the age of 35. Six per cent (n=3) of the population were aged 18-34, 18% of the population (n=10) were aged 35-44, 20% of the population (n=10) were aged 45-54, 20% of the population (n=10) were aged 55-64 and 20% of the population (n=13) was over the age of 65. The majority of the population was married (n=43), six per cent were single (n=5), none were separated nor divorced and five respondents were widowed. The educational background of the respondents varied; the majority of the respondents had completed high school (n=20).
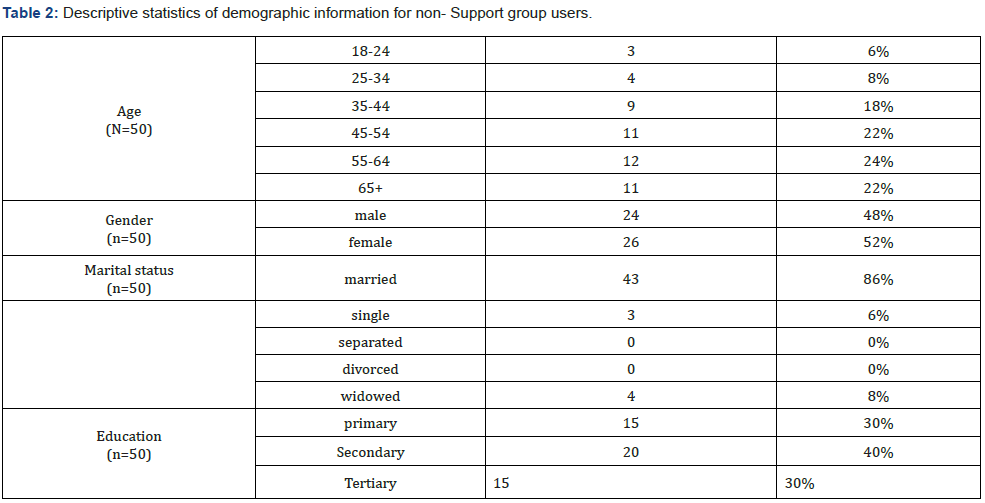
(n=50) was 48% male (n=23) and 52% (n=27) female. All age ranges were represented, however, the majority of the population was over the age of 35. Six per cent (n=3) of the population were aged 18-34, 18% of the population (n=9) were aged 35- 44, 22% of the population (n=11) were aged 45-54, 24% of the population (n=12) were aged 55-64 and 22% of the population (n=11) was over the age of 65. The majority of the population was married (n=43), six per cent were single (n=5), none were separated nor divorced and five respondents were widowed. The educational background of the respondents varied; a majority of the respondents had completed high school (n=20) (Figure 1&2).
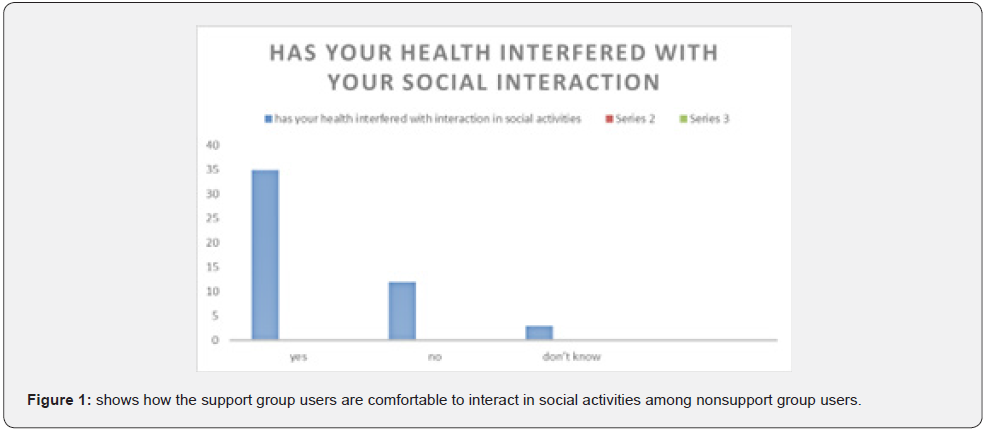
Non-Support Group User and Ability to Interact in Social Activities
Most non-support group users 70% were not able to interact in social events comfortably and to interact with others comfortably. Nevertheless, some of the respondents were able to interact well with others in social activities very few of the respondents had no idea whether their health interfered with their social activities. 4.5 interaction between health and hobbies for support group user (Figure 3).
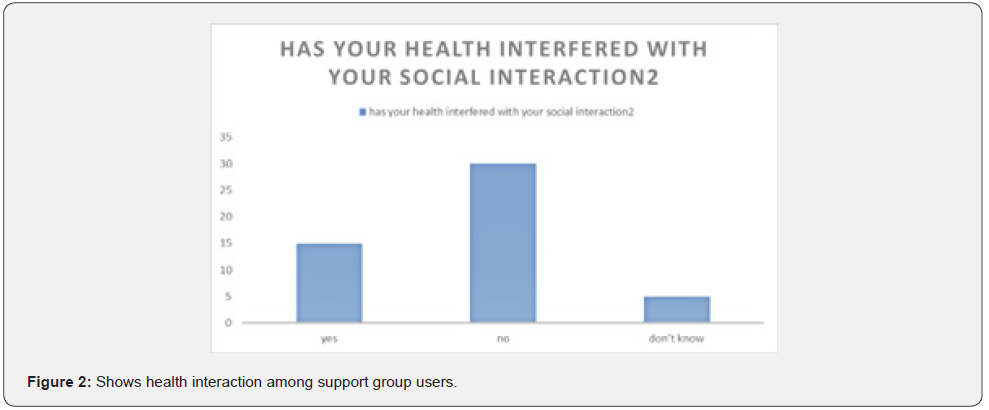
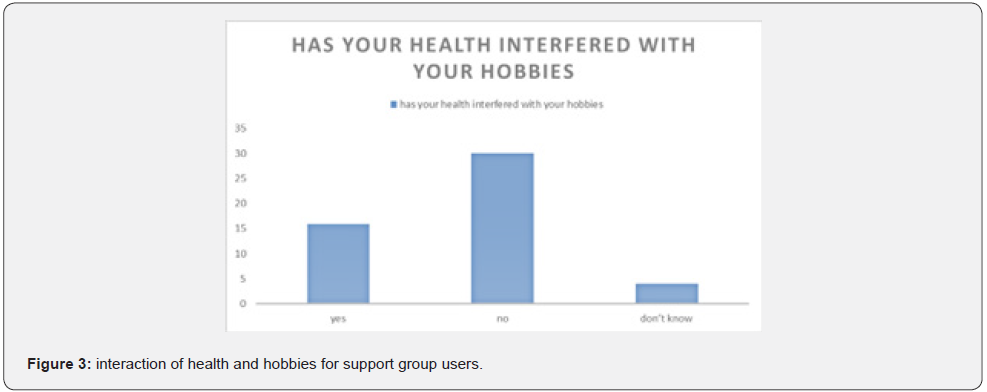
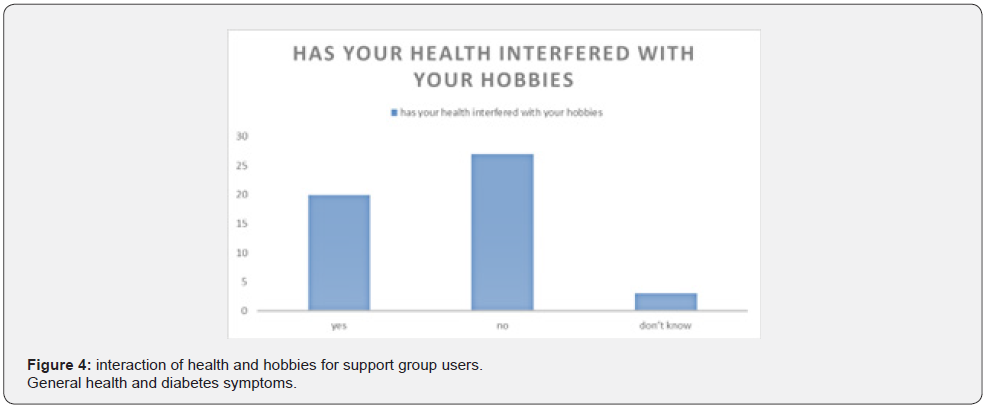
Figure 3 above shows that most of the support group users 60% were able and happy to continue with their hobbies despite their health problems 34 % could not participate in their hobbies and 6 % were not sure if they could still participate in their hobbies (Figure 4)
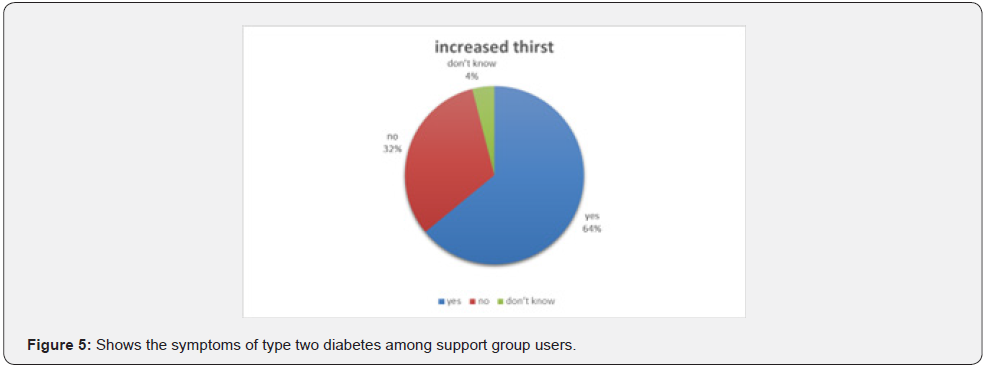
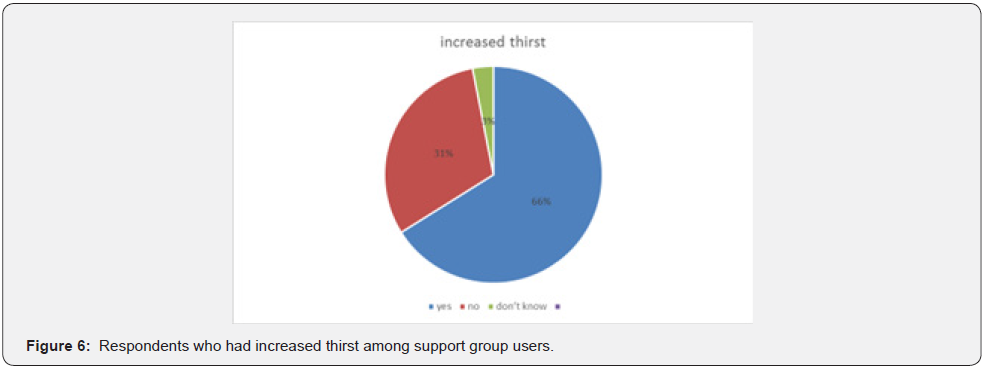
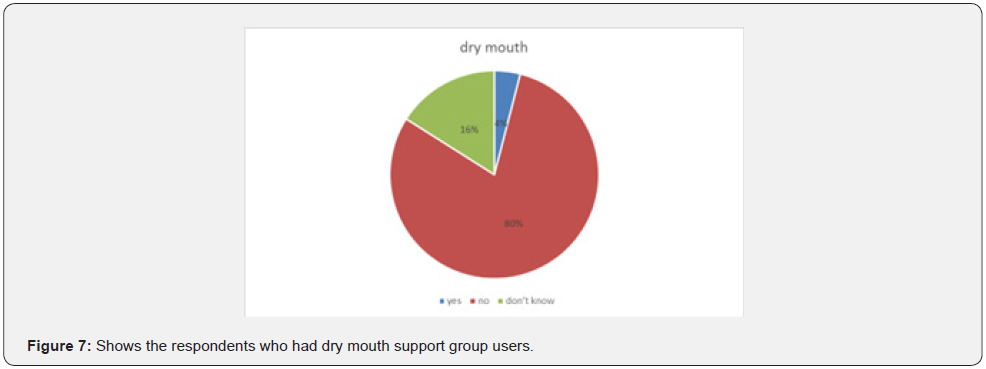
General health and diabetes symptoms (Figure 5-7).
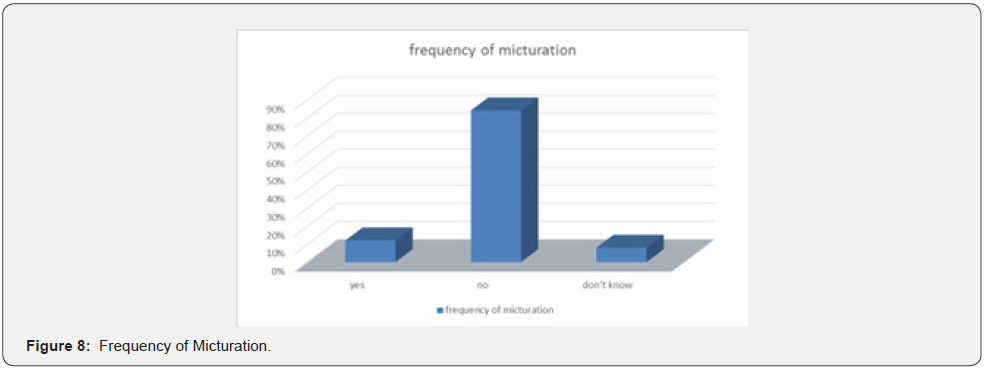
Majority of the respondents didn’t have dry mouth 80% 4 % had dry mouth and 16% didn’t know if they had a dry mouth (Figure 8).
Discussion of Results
The present study contributes to a better understanding of the role of patient support groups in the self-management of type 2 diabetes. The concept of identity has often been used to understand goal behaviours in the workplace and has been slowly introduced into the healthcare environment to understand how individuals cope with chronic illness. Healthcare providers are in a unique position to implement theory-based interventions or strategies to improve patient-reported outcomes.This study examines how individuals identify with and behave as part of, social groups. Within this theoretical framework, group identification has been found to be positively related to improved effort and motivation of the individual to attain goals. Individuals in the study could identify with a specific support group, or a more abstract collectivity of all individuals with type 2 diabetes in Bomet County.
Discussion of the Demographic Results
When we look at the demographic data we see that type 2 diabetes impacts men and women proportionately. The demographic characteristics of the participants completing both versions of the survey show that the majority of respondents in both populations (52% of non-support group users and 54% of support group users) were female (Tables 4.1 and 4.2). Our study sample had more females, which is not surprising because when we examine support group participants, we see that there tend to be more women than men in such groups. In a study conducted by the Pew Research Center on Internet use, it was found that over 90 million individuals have participated in an online group of some form. When we examine the results of support groups, the study reports that women tend to seek support for illness more so than men and are more likely than men to have more interactive relationships [1,2]. Such findings, with respect to participation and interaction, have also been observed within online social networking sites, such as Facebook ® and Linkedin ® [3]. Another study found evident differences between genders with respect to types of interactions in support groups; reporting that men tend to give and receive information related to their condition, while women tend to give and receive encouragement and support [4]. Other studies on self-help show that men are more likely than women to use self-help groups (i.e. Alcoholics Anonymous) [5]. This study by Davion and colleagues included other support groups, including those for chronic illness, however, the largest subset of the population was the substance abuse groups. Our findings suggest that both men and women in this particular study have the same level of need with respect to support groups as others [6-9].
When we compare the two study groups, we found the only statistically significant differences were age and sex. Respondents in the support group were significantly older than respondents in the non-support group; the majority of the support group respondents were 45 and older. The majority of the population had some high school education, and the support group participants were slightly more educated [10,11].
Health Impact on the Emotion
There are many significant differences between support group users and those that are not in a support group. These differences are with respect to certain diabetes control attitudes, the support of family and friends, negative emotions related to or as a result of being a person with diabetes, the impact that diabetes has on one’s life (both present and future abilities), the strength of all lifestyle goals and related goal self-efficacy and achievement. Recommendations for care made by the provider may make the patient feel unable to exercise any control in their care. Examination of the types of topics that are posted within the support group community reveals that many members question the recommendations of their healthcare provider and seek confirmation or disconfirmation from other members, and the majority of these instances of doubt involve medication use.
Support group members may have different personalities than those that do not belong to support groups. Characteristics such as graciousness, holistic, and participative might be used to describe such patients. This perception of unease might be related to an individual’s rationale to join a support group and seek the support and understanding of other individuals that have diabetes. This finding may suggest that individuals who experience heightened negative emotions have an illness identity that is more salient and thus might affect their social relationships with others. These individuals might relate more with other persons with diabetes. These individuals might also identify themselves as belonging to a larger group of persons with diabetes because being one of many is deemed better than being alone. To preserve self-esteem this mentality is adopted.
Impact of the Health Problem on Social Interaction
The respondents were examined on the effect of diabetes type 2 on their ability to interact in various social activities as shown in the data collected in this study. Most non-support group users, 70%, were not able to comfortably interact in social events and to interact with others comfortably compared with support group users where the majority of the respondents had no problem participating in daily social events and interacting with others. Figure 4.6 in chapter 4 shows that most of the support group users 60% were able and happy to continue with their hobbies despite their health problems 34 % could not continue with their hobbies and 6 % were not sure if they could still participate in their hobbies. Concerning general health, 50% of support group users were in excellent health compared to 44% of nonsupport group users. The study also shows in Table 5.2 for support group users most support group users 60% had a glucometer machine and were able to measure their blood glucose at home compared to 40% of nonsupport group users.86% of support group users were adherent to their medication and 14% missed to take their medication in the past 1 month probably because of education in social support groups. most of the respondents were adherent to their medication at (n=43) 86% compared to (n=32) 64%in non-support group users Also, the act of taking medication, as described in other studies included in Chapter 2, is sometimes viewed as a failure, or an option of last resort when lifestyle changes are not effective. Therefore, patients might experience a decrease in self-efficacy when a particular medication they are on suddenly becomes ineffective or when they are switched from oral medications to insulin. In this particular study population, all subjects were on some form of medication.
Conclusion and Recommendation
Diabetes is a disease that can be very individualistic in the sense that it can differentially impact different individuals based on race, socioeconomic status, age and even gender. Illness severity, treatment strategies and comorbidities all contribute to a different experience for every patient. As such, using the experience of one patient to make assumptions about another with respect to treatment can be misinformed. That is why the information that is presented within support groups must be carefully reviewed by a healthcare professional and moderated so that it is not misconstrued. Peer information, while having an experiential component that family support lacks, is often provided from the viewpoint of one individual and his or her experience.
Without fully understanding how illness severity and comorbidities may play a role in determining treatment strategies, the individual may assert that because a particular treatment worked for them, it will work for others. The patient, then armed with this information, and perhaps more information (not always peer-reviewed) gleaned from an additional search, begins to question the recommendations of his or her healthcare provider. This questioning can result in two different scenarios: in one, the patient consults his or her healthcare provider with the information and dialogue about the information can occur. Oftentimes, the health care provider may spend an inordinate amount of time explaining why the particular treatment would not be effective for the patient when compared to what the patient is currently taking/doing to manage his or her diabetes, and thus can be viewed as an inefficient use of time in the health care encounter. In the second scenario, there is no communication between the patient and the provider and the patient may opt to stop following the healthcare provider’s recommendations and thus becomes non-compliant. This noncompliance may result in a multitude of adverse events for the patient, further jeopardizing his or her health.
Finally, this study sought to measure the influence of identity and support on one outcome: lifestyle and medication goal achievement. Future research should determine if support group participants are able to achieve benefits beyond goal achievement, such as quality of life, improved health and improved identity. More investigation is needed to determine if online support is effective in assisting people to achieve such outcomes and how to create interventions that supplement traditional healthcare provision for chronically ill patients that use online support to improve outcomes.
References
- American Association of Clinical Endocrinologists (2005) the State of Diabetes Complications in America.
- (2004) American Association of Diabetes Educators.
- Anderson BJ, Miller JP, Auslander WF, Santiago J (1981) Family characteristics of diabetic adolescents: Relations to metabolic control. Diabetes Care 4(6): 586-594.
- Anderson RM, Funnell MM, Fitzgerald JT, Marrero DG (2000) The diabetes empowerment scale: a measure of psychosocial self-efficacy. Diabetes Care 23(6): 739-743.
- Andrews KH, Kandel DB (1979) Attitude and behavior: A specification of the contingent consistency hypothesis. Am Social Rev 44(2): 298-310.
- Andrews D, Nonnecke B, Preece J (2003) Electronic survey methodology: A case study in reaching hard-to-involve Internet users. Int J Human-Computer Interaction 16(2): 185-210.
- Applebaum SH, Hare A (1996) Self-efficacy as a mediator of goal setting and performance: Some human resources applications. J Managerial Psych 11(3): 33-47.
- Azjen I (1991) The theory of planned behavior. Organizational Behavior and Human Performance 50(2): 179-211.
- Bagozzi RP, Dholakia UM (2002) Intentional social action in virtual communities. J Interactive Mktg 16(2): 2-21.
- Bandura A, Adams NE. Analysis of self-efficacy theory of behavioral change.
- Baron RM, Kenny DA (1986) The moderator-mediator variable distinction in social Psychological research: conceptual, strategic, and statistical considerations. J Personality Soc Psych 51(6): 1173-1182.
- Barrera M, Glasgow RE, McKay HG, Boles SM, Feil EG, et al. (2002) Do internet-based support interventions change perceptions of social support? An experimental trial of approaches for supporting diabetes self-management. Am J Comm Psych 30(5): 637-654.
- Baruch Y, Holtom BC (2008) Survey response rate levels and trends in organizational research. Human Relations 61(8): 1139-1160.
- Bradley E, Calvert E, Pitts MK, Redman CWE (2001) Illness Identity and the Self-Regulatory Model in recovery from early-stage gynaecological cancer. J Health Psychol 6(5): 511-521.






























