Determinants of Skilled Birth Attendance Utilization Among Mothers Who Gave Birth in The Last 24 Months in Kembata Tembaro Zone
Eyassu Mathewos Oridanigo*
Department of Nursing, College of Medical and Health Sciences, Wachamo University, Ethiopia
Submission: February 22, 2021; Published: May 16, 2022
*Corresponding author: Eyassu Mathewos Oridanigo, Department of Nursing, College of Medical and Health Sciences, Wachamo University, Ethiopia
How to cite this article: Eyassu Mathewos O. Determinants of Skilled Birth Attendance Utilization Among Mothers Who Gave Birth in The Last 24 Months in Kembata Tembaro Zone. J Gynecol Women’s Health 2022: 23(3): 556113. DOI: 10.19080/JGWH.2022.23.556113
Abstract
Background: Skilled delivery is considered the single most important strategy in preventing maternal and neonatal morbidity and mortality. It ensures safe birth, reduces actual and potential complications and increases the survival of most mothers and newborns.
Objective: To identify determinants of the utilization of skilled birth attendance among women who gave birth in the last 24 months in the Kembata Tembaro zone, Southern Ethiopia, 2020.
Methods: A community-based cross-sectional study was employed from April 1 to 30, 2020 among women who gave birth in the last 24 months in Kembata Tembaro zone. Six hundred and twenty-four mothers were recruited for the study as eligible participants. Multi-stage stratified sampling was used to select three districts and one town administrative unit of the study area. The data were collected and verified for their completeness, followed by editing and coding. Multivariate analysis was performed using the back ward LR method to identify factors independently associated with the dependent variable. Statistical significance was declared at a p-value of less than 0.05 and the strength of statistical association was measured by adjusted odds ratio and 95% confidence interval.
Result: Of 624 study subjects sampled, 607 provided information with a response rate of 97.3%. In this study, 309(50.9%) women had their last birth at health facilities attended by skilled birth attendants. Place of residence [AOR (95% CI)=0.33(0.22,0.58)]; age at interview [AOR (95% CI=3.41(1.57,5.45)]; maternal education [AOR (95% CI)=1.50(1.34, 4.19)]; history of still birth [AOR (95% CI)=3.85(2.14,6.91)]; maternal occupation [AOR (95% CI)=3.35(1.79,6.27)]; husband occupation [AOR (95% CI)=2.69(1.70,7.09)]; ANC visit [AOR (95% CI) =4.62(3.12,7.32)]; knowledge of obstetric complications [AOR (95% CI) =3.10(1.37,5.21)]; and final decision-making about place of delivery [AOR (95% CI)=3.64(1.70,7.99)] were significantly associated with the use of skilled birth attendance.
Conclusion: In this study, nearly half of the mothers used skilled birth attendance. Place of residence, age at interview, maternal education, history of still birth, maternal occupation, husband occupation, antenatal visit, knowledge about obstetric complications and final decision maker about place of delivery were determinants of the use of skilled attendance delivery.
Keywords: Skilled birth attendance; Utilization; Kembata Tembaro zone
Abbreviations: WHO: World Health Organization; MMR: Maternal Mortality Ratio; SBA: Skilled birth attendance; SDGs: Sustainable Development Goals; EDHS: Ethiopian Demographic and Health Survey; SNNPR: Southern Nations, Nationalities and People republic
Background
According to the World Health Organization (WHO), “skilled birth attendants are accredited health professionals (such as midwives, doctors, or nurses) who have been educated and trained to proficiently manage normal (i.e., uncomplicated) pregnancies, childbirths and the immediate postnatal period, as well as handle the identification, management and referral of complications in women and newborns” [1]. To reduce maternal mortality, the indicators of progress are proportion of births attended by skilled attendants and Maternal Mortality Ratio (MMR) [2]. Skilled birth attendance (SBA) during labor, delivery and early post-partum period can significantly reduce both maternal and newborn morbidity and mortality by preventing or managing most obstetric complications [3]. Providing skilled care at birth goes hand in hand with the Sustainable Development Goals (SDGs) to reduce child mortality, particularly neonatal mortality [4]. Since 2000, the United Nations’ MDGs, which included a goal to improve maternal health by the end of 2015, has facilitated significant reductions in maternal morbidity and mortality worldwide [5].
Despite more focused efforts made especially by low- and middle-income countries, targets were largely unmet in sub- Saharan Africa, where women are plagued by many challenges in seeking obstetric care. Maternal mortality is unacceptably high and every day approximately 810 women died from preventable causes related to pregnancy and childbirth in 2017 [6]. Sub- Saharan Africa and Southern Asia accounted for approximately 86% (254 000) of the estimated global maternal deaths in 2017 with sub-Saharan Africa alone accounting for roughly 66% (196 000) [7]. Nearly 42.5% of infant deaths each year occur within the first week of life and are often due to a lack of or inappropriate care during pregnancy, delivery and the post-partum period [8]. One third of nearly one million stillbirths occur during labour, and approximately 280,000 babies die of birth asphyxia soon after birth. Approximately 60% of African women and their babies do not receive skilled care during childbirth and fewer receive effective postnatal care [9]. This is also the crucial time for other interventions, especially prevention of mother-to-child transmission of HIV and initiation of breastfeeding [10].
In Ethiopia, poor access to SBA is reflected by its MMR [11]. According to the 2016 Ethiopian Demographic and Health Survey (EDHS), MMR was estimated to be 412 per 100,000 live births [12]. Major causes of maternal deaths in Ethiopia are like to most developing countries such as infection, hemorrhage, obstructed labor, abortion and hypertension that could be avoided if preventive measures were taken and adequate care is available particularly during pregnancy, childbirth, and postpartum period through obstetric care services [13]. Poor access to and use of skilled delivery services have been identified as a major contributory factor to high maternal and newborn mortality, which remains a major challenge to health systems and public health issue in the country [14].
Although skilled delivery has been promoted in Ethiopia, home delivery with TBAs is still common, primarily in rural areas that are hard-to-reach [15]. The 2016 EDHS showed that only 28% of live births in the 5 years before the survey were delivered by a skilled provider, 26% in the health facility whereas home delivery was 73% and 1% in other places. For rural women, the report showed that 80 percent of births to urban mothers were assisted by a skilled provider as compared with 21 percent in rural area. 80% of them delivered at home [16].
Based on the National Reproductive Health Strategy (NRHS), the country planned to increase the proportion of births attended by skilled health personnel either at home or in the facility to 60% [5]. Despite the efforts being made by the government and other stakeholders to mitigate the problems and subsequent consequences posed by SBA delivery, studies in different parts of the country are showing that most Ethiopian women are giving birth at home and SBA remains low [17,18]. To enhance use of SBA in the country, barriers during delivery among women need to be identified across the regions. Little is known about the current magnitude of use of SBA and its determinants in the study area. Therefore, this study aimed to assess extent of SBA utilization and attempts to explore its determinant that are assumed to be barriers among mothers who gave birth in the past 24 months in Kembata Tembaro zone, Southern Ethiopia.
Methodology
Study area and period
A community-based cross-sectional study was conducted in the Kembata Tembaro Zone from April 1 to 30, 2020. The zone is located in the Southern Nations, Nationalities and People republic (SNNPR) of Ethiopia and its capital town, Durame, which is located 293 kilometers (km) south of Addis Ababa and 118 km west of Hawassa. In this zone, there are eight woreda health offices and three health administrative units, one general and four primary hospitals, 28 governmental and three non-governmental health centres, 136 health posts and 1,170 different types of health professionals.
Population
The source population consisted of all women who gave birth in the last 24 months prior to the survey in the study area while study population consisted of randomly selected women who gave birth in the last 24 months, irrespective of the outcome of the birth.
Sample size determination
To determine the sample size, two-population proportion formulas were used, and the following assumptions were made. The level of confidence=95% and power= 80%. Antenatal Care (ANC) visit during last the pregnancy was considered as predictor factor for the utilization of SBAs. Participants were categorized as women who visited or not ANC during last their pregnancy [19]. An ANC visit during the last pregnancy gives the maximum sample size among other predictor variables, such as having place of residence and educational status.
P1=Proportion of women who attended ANC during their last pregnancy= 57.9%
P2= Proportion of women who did not attend ANC during their last pregnancy= 42.1%
Based on the above assumptions, a design effect of 1.5 and a 5% non-response rate, 624 study participants who gave birth in the last 24 months were selected for the study.
Sampling procedures
Multi-stage stratified sampling was used to select three districts (Angacha, Doyogena and Kedida Gamela) and one administrative town, Durame, from a total of eight districts and three administrative towns in the zone. First, the zone was stratified into rural districts and urban administrative towns, and then 15 kebeles were chosen by lottery. House-to-house visits were carried out in selected kebeles to identify households with women who gave birth in the last 24 months prior to the survey, and 13,806 households were identified as fulfilling the eligibility criteria. By allocating the sample size proportionally to each kebele, systematic sampling was used to select study subjects. If the houses were closed or the mother was not present at the time of data collection, revisits were made until the data collectors were able to survey the women.
Variables
Dependent variable: Use of skilled birth attendance
Independent variables: Socioeconomic and demographic factors (education, age, marital status, education income, number of family members, residence, travel time to the nearest health facility within 30 minutes, exposure to the mass media), obstetric factors, parity, complications experienced (prolonged labour), history of stillbirth, history of ANC follow up), husband’s factors (occupation, education) and knowledge and attitude on key danger signs of pregnancy, labour/childbirth and delivery services.
Data collection procedures
Data were collected using interviewer-administered, structured questionnaires that were developed after reviewing relevant studies [17,19-22]. Six BSc nurses and one health officer were recruited to collect the data and supervise the data collection process respectively. Data collectors were selected from outside the study area to minimize interviewer bias and selected based on the ability to speak both Kambatissa and Amharic (local languages). Two days of training were provided concerning the purpose of the study and the methods of data collection. The supervisors were informed about the strict supervision and crosschecking procedures for data abstraction forms and completeness at the end of each day. The principal investigator supervised the overall activities.
Data quality control
The quality of the data was assured via proper questionnaire design and training of data collectors and supervisors for two days before the data collection. Every day after the data collection, the questionnaires were reviewed and checked by the supervisors to maintain accuracy and completeness by the supervisors. The English versions of the questionnaires were translated into local languages (Kambatissa and Amharic) and back-translated translated to English and comparisons were made to ensure the consistency of these versions. Data collection tools were pretested at 5% of the sample and to identify any weaknesses in the structuring of the research instruments prior to their use in data collection. Following the pre-test, the tools were improved in terms of their clarity and simplicity.
Data management and statistical analysis
Data was checked for its completeness; edited, coded and cleaned then it was entered into Epidata 3.1 and exported to SPSS version 23 for analysis. Descriptive statistics was computed and results were presented by tables, graphs and numerical summary was used to present the quantitative results. Before bivariate analysis, all variables were checked by cross tabulation for fulfilling chi-squared test assumptions of 80% expected frequency greater than five and all cells expected frequency greater than one. Variables with p<0.25 in bivariate analysis were considered as candidates for multivariate analysis. Multivariate analysis was performed using back ward LR method to identify factors independently associated with dependent variable. Statistical significance was declared with p<0.05 and the strength of statistical association was measured by adjusted odds ratio and 95% confidence intervals. Hosmer-Lemeshow goodness-of-fit statistics were used to check the goodness of fit of the model with a p-value of 10%.
Operational definitions
a) Utilization of skilled birth attendance: Use of skilled birth attendance delivery was assessed by asking the mother if she gave birth only in hospital or health center assisted with healthcare providers with midwifery skills or not for her recent delivery within the last 24 months.
b) Knowledgeable on danger signs of pregnancy: A woman was considered as knowledgeable if she could mention at least three danger signs that could occur during pregnancy [17,20]
c) Knowledgeable on danger signs of labour/ childbirth: A woman was considered as knowledgeable if she could mention at least three danger signs that could occur during Labor/childbirth and not knowledgeable if otherwise.
d) Knowledgeable on key danger signs of postpartum: A woman was considered as knowledgeable if she could mention at least the three danger signs that could occur during postpartum period /after delivery and not knowledgeable if otherwise.
Result
Socio-demographic and socio-economic characteristics of the respondents
In this study, out of 624 participants sampled, 607 of them provided information with a response rate of 97.3%. Approximately two third of the study subjects, 395(65.1%) were in the age range of 25-34 years with a mean and standard deviation age of 27.3 and 5.6 respectively and 479(68.6%) were residing in the rural area. Majority of the respondents, 446(73.5%) were Kembata in ethnicity. Regarding educational level of respondents, half, 306(50.5%) attended secondary and above school (Table 1).
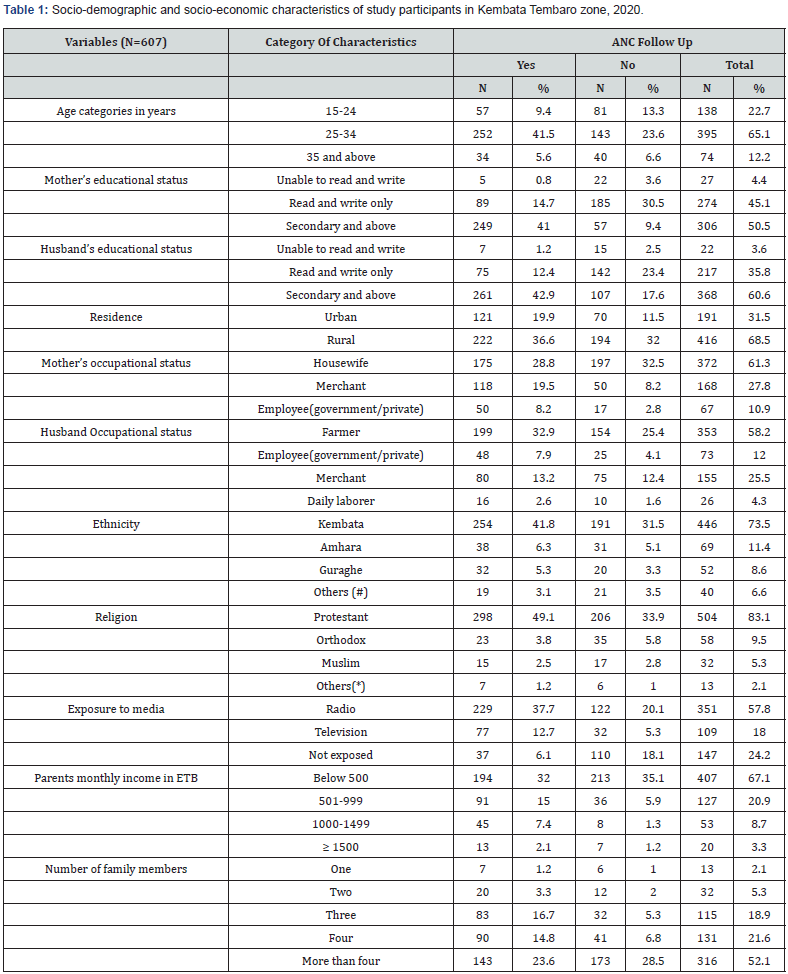
Note: Others (#) indicates Oromo, Tigre, Hadiya and Wolaita ethnicity and Others (*) indicates Adventist, Hawarat and catholic religion followers
Obstetric characteristics of the respondents
Among the respondents, 187(30.8%) [Rural, 133(21.9%) and urban, 54(8.9%)] married before the age of 18. Regarding age at first pregnancy, 181(29.8%) respondents [rural, 145(23.9%) and urban, 36(5.9%)] were pregnant before the age of 20. More than half, 354 (58.3%) did not follow up ANC during their last pregnancy and among those who had ANC follow up history, only 192(31.6%) had four visits and above. Among the respondents, approximately half, 232(49.1%) reported that they gave their last birth at home and more than half, 168 (56.4%) were attended by TBAs. (Table 2) Regarding the reason for home delivery, nearly three fourth, 232(77.9%) of the respondents reported that the main reason for home delivery was feeling of more comfortable. (Figure 1)
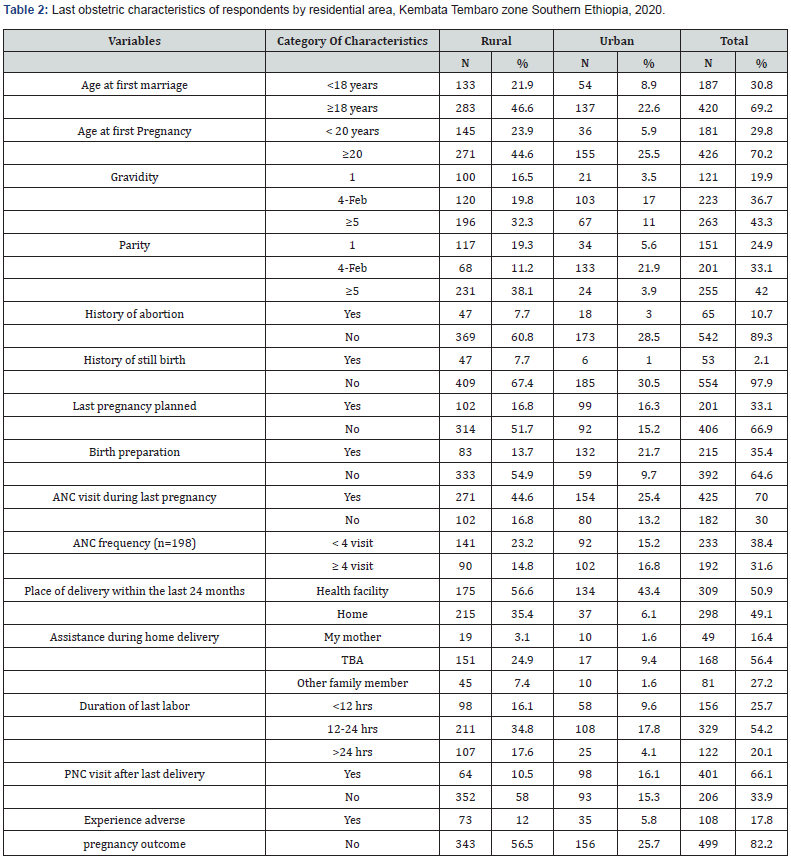

Accessibility characteristics of respondents
Approximately half of study participants, 305(50.2%) had health facility within 1 to 2 hours distance while 220(36.2%) and 82(13.5%) had health facility within one hour and less than one hour distance respectively. Regarding availability of functional media, 351(57.8%) and 109(18%) had functional media (radio and/or television) but 147(24.2%) had no functional media at all.
Knowledge on key obstetric danger signs during pregnancy, labor and childbirth, and after delivery
In this study, 289(47.6%), 498(82.0%), 326(53.7%), 252(41.5%), 208(34.3%) and 310(51.1%) mentioned Severe headache, blurred vision, Vaginal bleeding, Severe abdominal pain, Loss of consciousness and Convulsion during pregnancy respectively. Regarding danger signs during labour and childbirth, 421(69.4%), 539(88.8%), 559(92.1%), 425(70%) and 369(60.8%) mentioned severe vaginal bleeding, prolonged labor, retained placenta, loss of consciousness and convulsion respectively. Moreover, 538(88.6%), 460(75.8%), 424(69.9%), 325(53.5%) and 356(58.6%) mentioned retained placenta, excessive bleeding, abdominal pain, vaginal discharge and severe headache respectively. Based on above signs, about half, 315(51.9%) respondents were knowledgeable on obstetric complications related to Labor and childbirth. (Table 3)

Women’s, husbands’ and family related factors
Regarding decision on place of delivery, about two fifth of the respondents, 256(42.2%) reported that the decision was made by themselves [urban 75(39.3) and rural 181(43.5)]. Regarding mothers’ preferences about place and attendant of delivery, more than half, 347(57.2%) and 279(46%) preferred home delivery and SBAs respectively (Table 3).
Utilization of SBAs delivery
In this study, 309(50.9%) women gave their last birth at health institutions being attended by skilled birth attendants [Urban, 134(43.4%) and rural, 175(56.6%). (Figure 2).

Determinants of skilled birth attendance utilization
Among the variables in bivariate analysis, 14 of them had a p-value of less than 0.25; hence they were candidates for multivariate analysis. They were again entered in to multiple logistic regression models to obtain variables which were independently associated with outcome variable, use of skilled birth attendance. The variables with p-value of less than 0.05 in multivariate analysis were taken as significant predictors of outcome variable.

Therefore, the final model showed that there was statistically significant association between ANC follow up and utilization of SBA delivery (p-value< 0.001) so that, mothers who had at least four ANC visits were 4.62 times more likely to use skilled birth attendance than those who had less than four ANC visits during their last pregnancy [OR (95% CI) =4.62(3.12, 7.32)]. In this study, we found that there was negative association between place of residence and utilization of skilled birth attendance (p<0.001). Mothers who lived in rural area were 67% less likely to use skilled birth attendance than those who lived in urban area [OR (95% CI) = 0.33(0.22, 0.58)]. (Table 4&5).
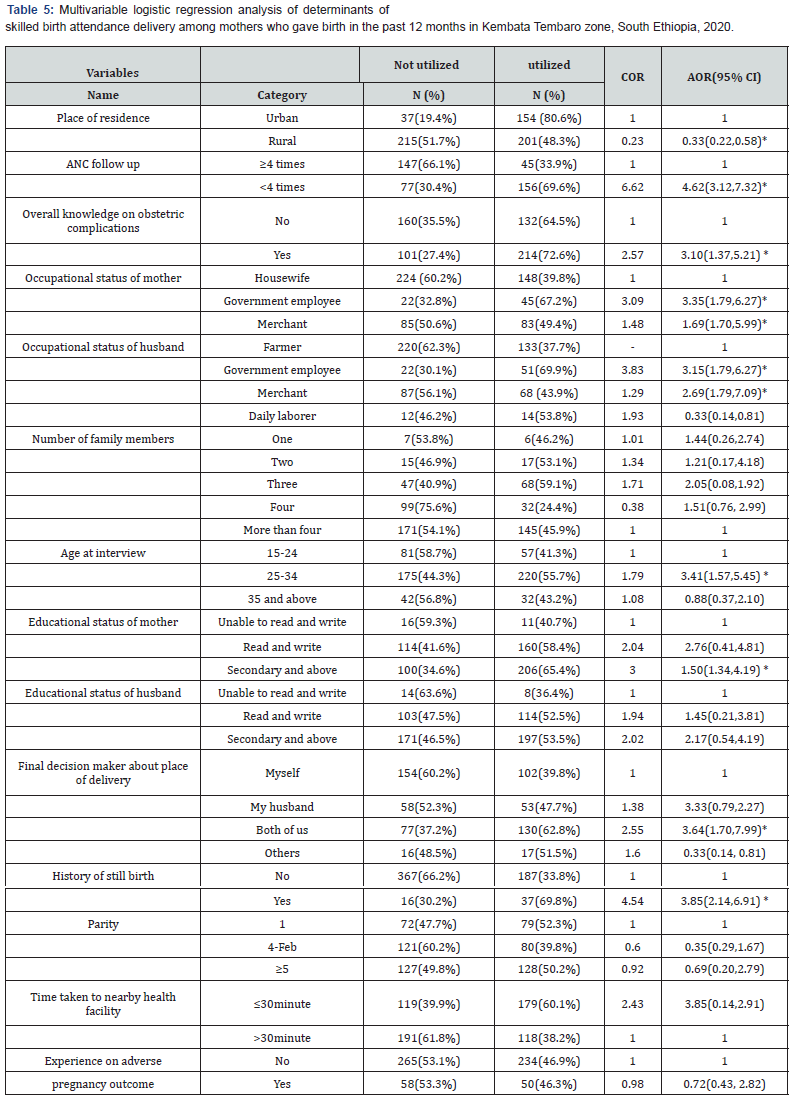
Note: * Indicates statistically significant at p<0.05
Hosmer and Lomeshow Test, p=0.407, the model was adequately fit the data
Discussion
Delivery assisted by skilled providers is the most proven intervention in reducing maternal mortality and one of the targets of United Nations’ (UN) Sustainable Development Goals (SDG) [23]. This community-based study identified very important determinants that are related to skilled birth attendant utilization among study subjects. The findings of the study revealed that the proportion of women who delivered in the facility assisted by skilled birth attendant was 51.8%. This finding is higher than study conducted in different parts of Ethiopia [17,19,24,25]. This might be because of increasing in functions of multipurpose health extension workers on improvements in ANC follow up and facilitating a referral services to HCs and hospitals for delivery service assisted by skilled healthcare provider. Health extension workers improved the utilization of maternal health services including skilled birth attendance delivery by bridging the gap between communities and health facilities [26]. However, it was lower than study conducted in rural southern Ghana where 68.8% mothers were assisted by skilled person during their last delivery [27]. The difference could be explained by the fact that women in those countries had better socio-economic status.
In this study, place of residence was statistically significant and negatively associated with outcome variable. The result showed that mothers who lived in rural area were less likely to use SBA than those who lived in urban area. This finding is supported with studies conducted in different regions of the country [17,19,22,25,28-30]. The possible reason might be prevailing of traditional thinking/views, presence of low education and income, lack of awareness on maternal health services like ANC, birth preparedness and complication readiness, remoteness/ lack of transportation to the health facility for mothers in rural than urban area [31]. History of still birth was another predictor of utilization of SBA. This study revealed that mothers who had previous history of still birth were more likely to utilize SBAs than mothers who did not have still birth. The finding from crosssectional survey conducted in Dembecha district of Northwest Ethiopia shows the negative association [24]. The possible reason might be the fact that ladies who had still birth in their lifetime may have a fear to develop the complication during the delivering of their child and prefer skilled provider to give birth in the health facility.
Older women were more likely to give birth assisted by skilled birth attendants than young women. This finding is similar with study done in rural residents of Southern Ghana [27]. However, the finding opposes other studies conducted in Raya district of North Ethiopia and Ghana which found as young women were more likely to use SBA than older women [19,32]. This might be older women were able to consider that giving birth at home is risky as they had experienced previously and they might get additional information regarding risk of home delivery with TBAs during different visits (childcare, immunization services and etc) to health facilities. The higher age of women can influence their status in the society which has been found to increases the ability of decision making [33].
Mothers’ educational status was other predictor of utilization of skilled birth attendant which was statistically significant. Mothers who had ability to read and write as well as mothers who learned secondary and above were more likely to use SBA than those who were unable to read and write. This finding is consistent with report from EDHS 2016 which found strong correlation between mothers’ educational status and skilled birth attendant delivery. EDHS 2016 found 17% of births to mothers with no education were assisted by a skilled provider as compared to 93% and 92%, respectively of births to mothers with more than a secondary education [16]. This might be because of educated women are likely to make their own healthcare decisions more and seek proper health care than their counterparts. In this study, parity was negatively associated with SBA utilization.
Maternal occupation is an important predictor of utilization of SBA. The study showed that both the government employees and merchants were more likely to use skilled birth attendance delivery than housewives. It was supported by study conducted in Northern Ethiopia and rural area of southern Ghana, which showed an important association between occupational status of mothers and utilization of SBA delivery [19,21]. Mothers with government employed husband were also more likely to utilize skilled birth attendance delivery than farmers. This finding was supported with study done in Gamo Gofa zone, southern Ethiopia [20]. The possible reason might be because those government employee and merchant ladies and their husbands might have more income and awareness for identifying skilled provider and place of delivery, searching for money for incurred costs, finding transportation, and other things which may contribute to home delivery.
In this study, we found that ANC visit during last pregnancy of the respondents was significant with use of skilled birth attendance delivery. Women who had ANC visit with skilled professional during their last pregnancy were more likely to deliver in health facility with skilled birth attendant than those who had no visit. This finding was also supported with the report from EDHS of 2011 and other studies conducted in different part of Ethiopia [17,19,28,34]. This might be women during Antenatal care (ANC) follow up can obtain counseling services on birth preparedness including place of delivery and selection of birth attendant and complication readiness. Antenatal care (ANC) from a skilled provider is important to monitor pregnancy and reduce morbidity and mortality risks for both the mother and child during pregnancy, delivery, and the postnatal period so that those mothers who had history of ANC follow up can easily give attention to deliver in the HF with SBA [16].
Knowledge regarding health problems during pregnancy and childbirth was other important predictor of skilled birth attendance delivery. Those respondents who had knowledge were more likely to utilize SBA delivery as compared to those who didn’t have knowledge on danger sign of pregnancy and childbirth. It is consistent with studies conducted Raya district of North Ethiopia and Gura Dhamole Woreda, Bale zone, southeast Ethiopia [17,19]. Women can take action by seeking appropriate health care by recognizing danger signs during pregnancy which can help them to deliver in the health facility with skilled birth attendant [35].
Moreover, the final decision maker about place of delivery in last pregnancy was another important predictor which is significantly associated with utilization of skilled attendant delivery. Respondents who jointly (both wife and husband) decided about place of delivery were more likely to use SBA delivery as compared to respondents who decided herself about place of delivery. This finding is supported with different studies conducted [17,19,24,28,36]. If women are encouraged by husbands, they would also get financial and other social supports to go to health facility which will allow them to have health provider assisted delivery [37]. In contrast to this, studies conducted in western Ethiopia have showed that women whom the decision on place of delivery made by themselves were two times more likely gave birth in health institution with SBA compared to mothers whom decision made by others on place of delivery [38].
Conclusion
In this study, about half of the study subjects were utilizing SBA. Women’s place of residence was negatively associated while maternal education, maternal occupation, husband occupation, Age at interview, ANC visit, knowledge about obstetric complications, during and after childbirth, final decision maker about place of delivery and history of still birth were positively associated with outcome variable, utilization of SBA.
Ethical Approval
Ethical approval of this study was obtained from the institutional review board of Pharma College Hawassa campus and SNNPR health bureau research and technology core process. The support letter was written from Kembeta Tembero Zone health department. After clear discussion about the actual study or explaining of purpose of the study, verbal informed consent was obtained from each study subjects and privacy was maintained during data collection.
Acknowledgements
It gives our pleasure to express our heartfelt gratitude to Pharma College, Hawassa Campus and SNNPR health bureau research and technology core process for approval of ethical clearance and technical support. We wish to express our appreciation to all who made their effort for the accomplishment of this research project possible. We also acknowledge our study participants for providing the necessary information and the data collectors for collecting the data carefully [39].
References
- WHO, UNICEF, UNFPA, The World Bank the United Nations Population Division. Trends in Maternal Mortality: 1990 to 2013.
- UNITED NATIONS. The Millennium Development Goals Report.2007.
- Graham WJ, Bell JS (2018) Can Skilled Attendance at Delivery Reduce Maternal Mortality in Developing Countries?.
- World Health Organization (2016) Monitoring Health for the Sustainable Development Goals (SDGs).
- IEG World Bank/IFC/MIGA (2016) Delivering the Millennium Development Goals To Reduce Maternal and Child Mortality: A Systematic Review of Impact Evaluation Evidence.
- World Health Organization (2019) Maternal mortality.
- WHO, UNICEF, UNIFPA, World Bank Group UN. Trends in Maternal Mortality 2000 TO 2017.
- Darmstadt GL, CCL Anee, Cousens S, Sibley L, Bhutta ZA, et al. (2012) 60 million non-facility births: Who can deliver in community settings to reduce intrapartum-related deaths? Int J Gynaecol Obstet 107(Suppl 1): S89-112.
- Pearson L, Larsson M, Fauveau V, Standley J (2020) Opportunities for Africa’s Newborns Pp: 64-75.
- The Partnership for Maternal, Newborn and Child Health (2018) Opportunities for Africa’s Newborns: Practical data, policy and programmatic support for newborn care in Africa. Joy Lawn, Save the Children, and Kate Kerber, Save the Children and BASICS WHO on behalf of The Partnership for Maternal Newborn and Child Health Pp: 250.
- Yifru B, Berhan Y, Berhan A (2014) Review of maternal mortality in Ethiopia: A story of the past 30 years. Ethiop J Heal Sci 24 Suppl (0 Suppl): 3-14.
- Central Statistical Agency (CSA) [Ethiopia] and ICF (2016) Ethiopia Demographic and Health Survey 2016. Addis Ababa, Ethiopia, and Rockville, Maryland, USA: CSA and ICF.
- Sageer R, Kongnyuy E, Adebimpe WO, Omosehin O, & Elijah AO, et al. (2017) Causes and contributory factors of maternal mortality: evidence from maternal and perinatal death surveillance and response in Ogun state, Southwest Nigeria. BMC Pregnancy Childbirth: 17(160).
- Africa Progress Panel (2010) Maternal Health: Investing in the Lifeline of Healthy Societies & Economies.
- Mekdes G, Kristel M , Yves J , Jean-Pierre V Geertruyden , et al. (2020) Traditional birth attenndants’ roles and homebirth choices in Ethiopia. Women Birth 33(5): e464–e472.
- Central Statistical Agency (CSA) [Ethiopia] and ICF, Addis Ababa E (2016) Ethiopian Demographic and Health Survey: Key Indicators.
- Ayele GS, Melku AT, Semere SB (2019) Utilization of skilled birth attendant at birth and associated factors among women who gave birth in the last 24 months preceding the survey in Gura Dhamole Woreda, Bale zone, southeast Ethiopia. BMC Public Health 19(1501): 1–14.
- Kea AZ, Tulloch O, Datiko DG, Theobald S, Kok MC (2018) Exploring barriers to the use of formal maternal health services and priority areas for action in Sidama zone, southern Ethiopia. BMC Pregnancy Childbirth 18: 1–12.
- Tadese F, Ali A (2014) Determinants of Use of Skilled Birth Attendance among Mothers Who Gave Birth in the Past 12 months in Raya Alamata District, North East Ethiopia Clinics in Mother and Child Health. Clin Mother Child Heal Tadese 11(2): 9–15.
- Mensa M, Belijo MN. Status of Skilled Birth Attendance Utilization and Determinants Among Women of Child Bearing Age in Chencha Woreda, Gamo Gofa Zone, Southern. Junier Online J Case Stud 4(3).
- Manyeh AK, Akpakli DE, Kukula V, Ekey RA Solomon N-B, et al. (2017) Socio ‑ demographic determinants of skilled birth attendant at delivery in rural southern Ghana. BMC Res Notes 10(1): 268.
- Markos D, Odo DB, Shifti DM (2014) Institutional Delivery Service Utilization and Associated Factors among Child Bearing Age Women in Goba Woreda, Ethiopia Institutional delivery service utilization and associated factors among child bearing age women in Goba Woreda, Ethiopia.
- WHO, UNFPA, UNICEF, ICM, ICN, et al. (2018) Definition of skilled health personnel providing care during childbirth : the 2018 joint statement by WHO, UNFPA, UNICEF, ICM, ICN, FIGO, IPA Pp:4.
- Kidanu S, Degu G, Tiruye TY (2017) Factors influencing institutional delivery service utilization in Dembecha district , Northwest Ethiopia : A community based cross sectional study. BMC Reprod Heal Pp: 1–8.
- Abdella Amano, Abebaw Gebeyehu, Zelalem Birhanu (2012) Institutional delivery service utilization in Munisa Woreda South East Ethiopia: a community based cross-sectional study. BMC Pregnancy and Childbirth.
- Jackson R, Hailemariam A (2016) The Role of Health Extension Workers in Linking Pregnant Women With Health Facilities for Delivery in Rural and Pastoralist Areas of Ethiopia. Ethiop J Health Sci 26(5): 471-478.
- Manyeh AK, Akpakli DE, Kukula V, Ekey RA, Bana SN, et al. (2017) Socio ‑ demographic determinants of skilled birth attendant at delivery in rural southern Ghana. BMC Res Notes Pp: 1–7.
- Fekadu M, Regassa N (2014) Skilled delivery care service utilization in Ethiopia: analysis of rural-urban differentials based on national demographic and health survey ( DHS ) data. Afr Health Sci 14(4): 974-984.
- Ayele DZ, Belayihun B, Teji K, Ayana DA (2014) Factors Affecting Utilization of Maternal Health Care Services in Kombolcha District, Eastern Hararghe Zone, Oromia Regional State , Eastern Ethiopia. Hindawi.
- Addis AF, Meaza D (2012) Prevalence of institutional delivery and associated factors in Dodota Woreda(district), Oromia regional state, Ethiopia. Reprod Health.
- Mulder S (1995) Midwifery in Rural India: A study of traditional birth attendants in Tamil Nadu, India. Aust coll midwives Inc J 8(1): 24-30.
- Dickson KS, Amu H (2017) Determinants of Skilled Birth Attendance in the Northern Parts of Ghana.
- ekonnen, Yared, AM (2002) Utilization of Maternal Health Care Services in Ethiopia. Calverton, Maryland, USA: ORC Macro.
- Central Statistical Agency (CSA) [Ethiopia] and ICF, Addis Ababa E (2011) Ethiopian Demographic and Health Survey 2011: Key Indicators.
- Mwilike B, Nalwadda G, Kagawa M, Malima K, Mselle L, et al. (2018) Knowledge of danger signs during pregnancy and subsequent healthcare seeking actions among women in Urban Tanzania: a cross-sectional study. BMC Pregnancy Childbirth. 18(4): 1–8.
- Soe M, Chamroonsawasdi K, Phitaya C, Suwat S (2015) Rate of Utilization of Skilled Birth Attendant and the Influencing Factors in an Urban Myanmar Population. Asia-Pac J Public Health 27(5): 521-530.
- Bernis L De, Sherratt DR, Abouzahr C, Lerberghe WV (2003) Skilled attendants for pregnancy, childbirth and postnatal care. Br Med Bull 67: 39–57.
- Tekelab T, Yadecha B, Melka AS (2015) Antenatal care and women’s decision making power as determinants of institutional delivery in rural area of Western Ethiopia. BMC Res Notes 8: 1–8.
- Kassa EM, kassa B (2021) Determinants of Skilled Birth Attendance Utilization Among Mothers Who Gave Birth in the Past 24 Months in Kembata Tembaro Zone.






























