Mercurial Erythema in A Pregnant Woman : A Case Report And Review of the Literature
Olfa Zoukar1, Yosra Jemaa2*, Amal Bayar3, Rahma Issa1, Amina Mnajja2, Ghada Khouidi3, Dalel Naguez3, Amal Sebri1, Dhekra Toumi1, Anis Haddad1 and Raja Faleh1
1Service de Gynéco-obstétrique, Centre de maternité et de néonatologie, Monastir, Tunisia
2Service de Gynéco-obstétrique de Ksar Hlel, Tunisia
3Service de gynéco obstetrique de CHU Taher SFAR Mahdia, Tunisia
Submission: March 14, 2021; Published: March 18, 2022
*Corresponding author: Yosra Jemaa, Service de Gynéco-obstétrique de Ksar Hlel, Tunisia
How to cite this article: Olfa Z, Yosra J, Amal B, Rahma I, Amina M, et al. Mercurial Erythema in A Pregnant Woman : A Case Report And Review of the Literature. J Gynecol Women’s Health 2022: 23(2): 556107. DOI: 10.19080/JGWH.2022.23.556107
Abstract
Mercurial erythema is an erythematous rash related to mercury intake by oral, intravenous, and dermal application. The diagnosis is evoked by the appearance of a pruritic, intense, sometimes generalized erythema that predominates in the groin folds, armpits, flanks, lateral surfaces of the neck, umbilicus, and elbows. This erythema becomes covered with a characteristic sieve of pustules and is sometimes associated with general signs. The management of this condition is essentially based on local corticosteroid therapy combined with symptomatic treatment with antihistamines and antibiotics in case of superinfection. The evolution of mercurial erythema is usually favorable. This work, based on a case observed in our department and on a review of the literature, aims to present the main clinical manifestations of mercurial erythema and the characteristics of the management of this pathology.
Keywords: Erythema; Mercury ; Pruritic Maculo-Papular Lesions ; Skin Biopsy ; Local Corticotherapy
Abbreviations: CBC: Complete Blood Count
Introduction
Mercury is a silvery-white, shiny, very dense metal, a good conductor of heat and electricity, and a liquid at ordinary temperatures. Mercurial compounds are volatile at room temperature and soluble in water. Metallic mercury and its compounds are sensitizing. Mercurial erythema is a systemic contact dermatitis that occurs after inhalation of mercury vapors (usually from a broken mercury thermometer), transcutaneous absorption, or ingestion of a mercurial derivative in a patient previously sensitized to mercury.
We report the case of a mercurial erythema in a pregnant woman hospitalized in our department and with the help of a review of the literature, this work aims to present the main clinical manifestations of mercurial erythema and the particularities of the management of this pathology in pregnant women.
Case Report
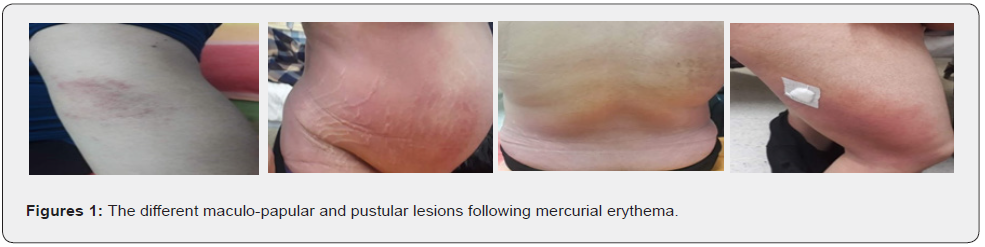
Mrs. Y.S, 31 years old, G1P1, pregnant at 29 days of age, type II diabetic. She was hospitalized in our department for glycemic cycle and presented a vaginal candidiasis, put under treatment. During her hospitalization, the patient presented with the sudden appearance of an erythema dotted with several maculo-papules covered in places with small whitish pustules located on the thigh, back, buttocks with absence of lesions on the face (Figures 1). Moreover, there was no notion of recent medication or arthralgia.
On further questioning, it was discovered that the patient had a history of mercury erythema not mentioned on admission and that these lesions appeared following recent exposure to mercury. A dermatological opinion was requested and the different diagnoses evoked in front of this clinical picture were: mercurial erythema; exanthematic pustulosis of pregnancy or pustular psoriasis.
The course of action was to perform a blood calcium level, a complete blood count (CBC), a mycobacteriological sample from the pustule, viral serologies for CMC, EBV, Parvovirus B19 and to perform skin biopsies. The patient was put on local corticoids, antibiotics and antihistamines. The result of the anatomopathology examination concluded to a lesion complex compatible with a mercurial erythema. The evolution was favorable under local corticosteroid therapy with regression of the cutaneous lesions. The patient was discharged on the fifth day of hospitalization with an appointment at the dermatology outpatient clinic for further follow-up and at our outpatient clinic for pregnancy follow-up.
Discussion
Mercurial erythema is a pruritic maculo-papular rash of vermilion red or purplish hue, appearing abruptly in the major folds a few hours after exposure to mercury, then spreading diffusely, bilaterally and symmetrically within 3 to 5 days and gradually disappearing without sequelae [1-3]. The lesions remain more marked in the folds, particularly the inguinal folds. The secondary appearance of small amicrobial pustules is often observed. Localized contact dermatitis may be associated with the lesions previously described: pubic dermatitis (insecticide powder), foot dermatitis (plastic boots containing mercury chloride), periorbital dermatitis (ophthalmic cream).
Extensive vesiculo-bullous forms predominating in the folds have been reported, as well as erythema multiforme-like aspects [4]. General signs are frequent (fever over 39 °C, general malaise, axillary and inguinal adenopathies). On questioning, one should look for exposure to a mercury derivative a few hours or days before the appearance of the erythema and for a previously known contact allergy to mercury. The physical examination will find the lesions described above.
Complementary examinations in the acute phase may show a hyperleukocytosis with a predominance of eosinophils, an increase in CRP, transient proteinuria and sometimes a high level of mercury in the blood and urine. The skin biopsy will not show any specific elements. Epicutaneous tests performed secondarily will point more towards the diagnosis in case of positivity for mercurial compounds. However, these tests lack sensitivity because they may be spontaneously positive in some individuals [5-7]. Thus, a positive test will be an important but not sufficient element, in the absence of a suggestive clinical and anamnestic context, to make the diagnosis of mercurial erythema. Mercury vapor inhalation challenge tests are strongly discouraged because they are dangerous.
To date, the indications for treatment vary and there is no consensus [2]. Treatment in the acute phase is based on avoidance of the allergen and, symptomatically, on dermocorticoids and antihistamines. A short course of general corticosteroids has sometimes been proposed in severe cases. Subsequently, contact with mercury and its organic and inorganic compounds should be avoided [5,8].
Conclusion
Mercurial erythema is a pruritic maculo-papular rash, vermilion or purplish red in color, appearing suddenly in the major folds a few hours after exposure to mercury, then spreading diffusely, bilaterally and symmetrically in 3 to 5 days and gradually disappearing without sequelae. The lesions remain more pronounced in the folds, particularly the inguinal folds. The secondary appearance of small amicrobial pustules, 2 to 3 days after the onset of erythema, is frequently observed. Mercurial erythema in a pregnant woman poses the problem of diagnosis and treatment.
Author Contributions
All authors contributed to the conduct of this work. All authors also declare having read and approved the final version of the manuscript.
References
- Lauwerys RR, Haufroid V, Hoet P, Lison D (2007) Mercure. In: Toxicologie industrielle et intoxication professionnelle. Paris: Elsevier Masson, France, pp. 309-363.
- Kanerva L, Rantanen T, Aalto Korte K, Estlander T, Hannuksela M, et al. (2001) A multicenter study of patch test reactions with dental screening series. Am J Contact Dermat 12(2): 83-7.
- Nakayama H, Niki F, Shono M, Hada S. Mercury exanthem (1983) Contact Dermatitis 9: 411-7.
- Fuortes LJ, Weismann DN, Graeff ML, Bale Jr JF, Tannous R, et al. (1995) Immune thrombocytopenia and elemental mercury poisoning. J Toxicol Clin Toxicol 33(5): 449-55.
- World Health Organization (2003) Elementary mercury and inorganic mercury compounds: human health aspects. Concise International Chemical Assessment Document 50. Geneva, switzarland.
- Garnier R Mercure (2000) Toxicologie clinique. In: Bismuth C (Eds.), Flammarion Médecine Science, Paris, France, pp. 614-623.
- Cox C, Clarkson TW, Marsh DO, Amin Zaki L, Tikriti S, et al. (1989) Dose-response analysis of infants prenatally exposed to methyl mercury: an application of a single compartment model to single-strand hair analysis. Environ Res 49(2):318-32.
- Blanusa M, Varnai VM, Piasek M, Kostial K (2005) Chelators as antidotes of metal toxicity: therapeutic and experimental aspects. Curr Med Chem 12(23): 2771-94.






























