Efficacy of Sildenafil Citrate on Female Sexual Dysfunction in A Sample of Egyptian Females, A Prospective Placebo Controlled Study
Mohamed Alhefnawy1*, Abdulla Esawy2, Mohamed Abdelazeem1, Mohamed Elnamoury3, Ahmed Eissa4, Ahmed Zoair4, Ahmed Ghaith4, Ayman Hagras4 and Khaled Almekaty4
1Urology department, Benha University, Egypt
2Dermatology department, Zagazig University, Egypt
3Gynecology department, Tanta University, Egypt
4Urology department, Tanta University, Egypt
Submission: October 15, 2021; Published: February 28, 2022
*Corresponding author: Mohamed Alhefnawy, Urology department, Benha University, Egypt
How to cite this article: Mohamed A, Abdulla E, Mohamed A, Mohamed E, Ahmed E, et al. Efficacy of Sildenafil Citrate on Female Sexual Dysfunction in A Sample of Egyptian Females, A Prospective Placebo Controlled Study. J Gynecol Women’s Health 2022: 23(1): 556105. DOI: 10.19080/JGWH.2022.23.556105
Abstract
Background: Sexual dysfunction is a problem that occurs during the sexual response cycle that prevents the individual from experiencing satisfaction from sexual activity. The assessment of sexual function in women is frequently confounded by many factors, including depressed mood and other comorbid medical and psychiatric disorders. Sildenafil is selective type 5 phosphodiesterase (PDE5) inhibitors, taken orally and effective for men with erectile dysfunction. Previous studies suggested that sildenafil may improve the sexual health of women affected by sexual difficulties such as arousal disorders and may indirectly improve other aspects of sexual life. Sildenafil was effective and well tolerated in postmenopausal women with sexual arousal disorder without concomitant hypoactive sexual desire disorder or contributory emotional relationship or historical abuse issues.
Objective: This study aimed to evaluate the effect of sildenafil citrate on female sexual dysfunction.
Subjects and methods: The study was conducted in the Andrology and Gynecology departments of Zagazig and Tanta University Hospitals during the period from April 2017 to August 2020. Fifty-two married female patients were included in this study. Patients were divided into 2 groups. Group 1 included 26 patients, all received 50mg sildenafil on demand and group 2 included 26 patients who took placebo tablets.
Results: There was no significant difference between the studied groups regarding the demographic data, and FSFI. There was significant difference between pre and post treatment of sexual dysfunction regarding the Sildenafil arm. There was no significant difference in post treatment results between the two studied groups as regard sexual dysfunction except in orgasm which showed superior improvement in the Sildenafil group.
Conclusions: Sildenafil citrate seems to be effective in treating women who could not achieve orgasm.
Keywords: Female; Sexual Dysfunction; Sildenafil
Abbreviations: FSD: Female Sexual Dysfunction; IRB: Institutional Review Board; FSFI: female sexual function index; SPSS: Statistical Package for Social Science
Introduction
Female Sexual Dysfunction (FSD) is a disturbance or dysfunction in the process of desire, arousal or orgasm, which can be a symptom of a biological condition, a psychological problem, an interpersonal issue or a combination of these factors [1]. Female Sexual Dysfunction is a multi-causal and a multi- dimensional medical problem that adversely affects physical health & emotional wellbeing. Also impaired sexual function can have damaging effects on the self-esteem, sense of wholeness and interpersonal relationships of women. It is often emotionally distressing and can affect reproduction or even end up with separation or divorce [2].
Selective type 5 phosphodiesterase (PDE5) inhibitors as sildenafil, which acts by inhibiting cyclic GMP specific PDE5 may improve the sexual health of women affected by sexual difficulties such as arousal disorders and may indirectly improve other aspects of sexual life [3]. Sildenafil was effective and well-tolerated in post-menopausal women with sexual arousal disorder without concomitant hypoactive sexual desire disorder or contributory emotional relationship or historical abuse issues [4]. However, studying FSD is lacking in the literature especially in the Arab and middle east region. In this study, we tried to prospectively assess safety and efficacy of sildenafil citrate in treating FSD.
Patients and Methods
The study was conducted in the Andrology and gynecology departments of Zagazig and Tanta University Hospitals during the period from April 2017 to August 2020. Fifty-two married female patients were included in this study. Informed consents were taken from all participants. Patients were randomized into 2 groups. Group A contained 26 patients who received 50mg sildenafil on demand. Group B received placebo tablets and also included 26 patients. The study was prospective, double-blinded and placebo controlled. The Institutional Review Board (IRB) provided ethical approval for this study (Institutional Review Board N° 1965) for Faculty of Medicine, Zagazig University, and Zagazig, Egypt on March 3, 2017.
Inclusion Criteria
Married female patients complaining of sexual dysfunction for at least 6 months and not on drug therapy for the treatment of FSD.
Exclusion Criteria
Patients with sexual dysfunction caused by local genital disorder, patients with retinal problem, patients with chronic debilitating diseases or hormonal disturbance, patients who cannot be treated with PDEs inhibitors type 5(sildenafil) as: Major hematological, renal or hepatic abnormalities, patients with major psychological disorders including major depression or psychosis, a history of stroke or myocardial infarction or any significant cardiovascular disease within the last 6 months, or concomitant treatment with nitrates.
Methods and Objectives
All patients in the 2 groups were subjected to: Complete history taking: age, education, occupation, residence, age of marriage, special habits, history of medical diseases, surgical history and sexual history in the previous 6 months. Thorough general and local examination was also done. Routine laboratory investigations including complete blood count liver function tests renal function tests, blood sugar and lipid profiles; were done. Evaluation questionnaire used included 25 items designed by the investigators. Only some items selected from the female sexual function index (FSFI) [5], other questions were added to suit the purpose of study.
The FSFI domain has maximum possible total scores of 36 as in (Table 1). The FSFI, a 19-item questionnaire, has been developed as a brief, multidimensional self-report instrument for assessing the key dimensions of sexual function in women. It is psychometrically sound, easy to administer, and has demonstrated ability to discriminate between clinical and nonclinical populations. The questionnaire described was designed and validated for assessment of female sexual function and quality of life in clinical trials or epidemiological studies. In addition, depression questionnaire was added to exclude the major psychological depressive disorder and its result put with the evaluation questionnaire as one item only (Table 2).
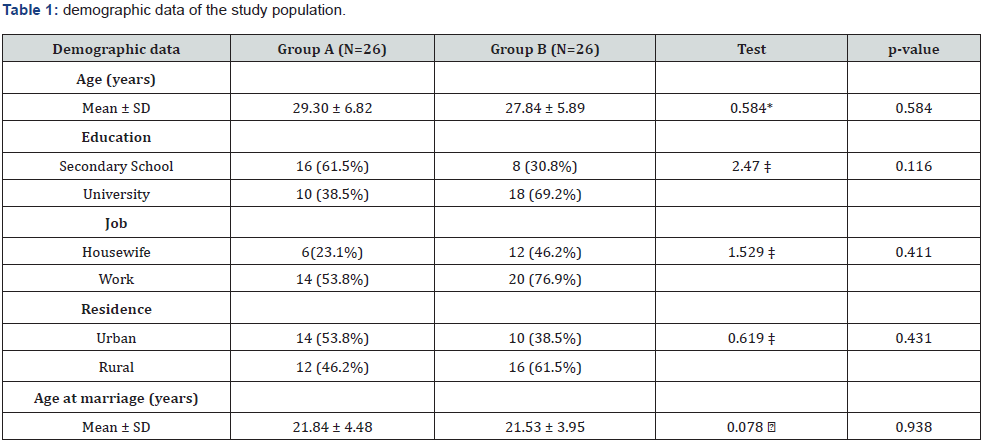
* Independent samples Student’s t-test. Mann Whitney U test. ‡ Chi-square test. P< 0.05 is significant.
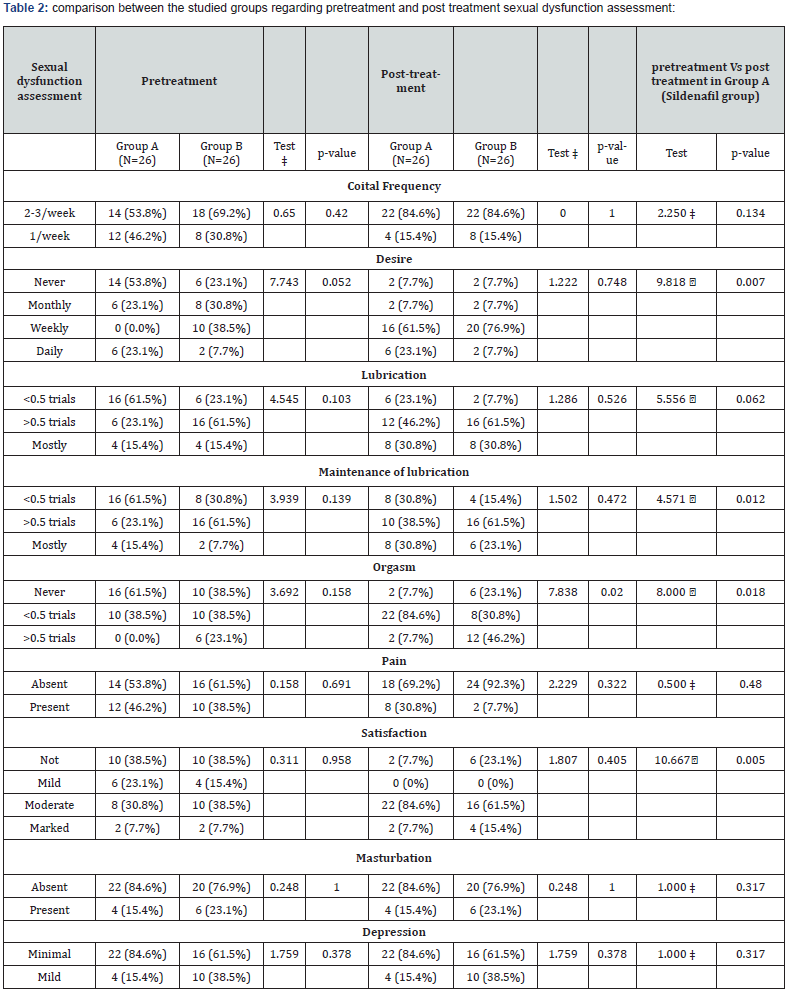
‡ Mc Nemar’s test. Stuart-Maxwell test. P< 0.05 is significant. Sig.: significance.
Statistical Analysis
The collected data were statistically analyzed using SPSS program (Statistical Package for Social Science) version 18.0.SPSS Inc., Chicago, IL, US.
Result
No significant differences were found between both studied groups regarding the demographic data (Table1). Also, the pretreatment baseline sexual function domains were comparable between both arms as shown in Table1. There were significant improvements in group A (the sildenafil group) particularly in the desire, lubrication, orgasm and the overall satisfaction domains (Table2).When compared to the placebo group, the treatment group was superior only in the post-treatment orgasm domain (Table 2).
Discussion
Sexual dysfunction is any disturbance in sexual response cycle [6].The family as the center and core of all human societies is based on the sexual instinct [7]. Female sexual problems have not received much attention as men’s sexual problems especially in Arab countries [8].
The current study was conducted to evaluate the effect of sildenafil citrate on the female sexual dysfunction. The included sample was composed of 52 women complaining of sexual dysfunction. They were randomized into 2 equal groups “sildenafil group and placebo group” as mentioned in the methodology section.
Overall, most of patients who received sildenafil were living in urban areas (53%). All patients of this study were educated, varying between secondary and university levels. Well-educated women from urban areas gave accurate answers as compared to those from conservative families, rural areas with lower education because the latter suffers from lack of access to information and lower level of awareness. As El-Gelany and Moussa. [9] concluded that high education level, exposure to the media, and living in modernized cities were the main contributing factors to a high awareness of reproductive health issues.
Both studied groups were comparable regarding the pretreatment FSFI with its all domains. As for the unprovoked desire to have sex, no statistically significant difference between both groups was found. This means that the demographic data has no particular effect on the female sexuality and both groups were at the same baseline pretreatment parameters. This agrees with the conclusion of Spector et al. [10] who stated that the sexual desire, which is an aspect of a person’s sexuality, varies significantly from one person to another, and varies depending on the surrounding circumstances at a particular time.
Comparing the effect of residence on female sexuality, the study showed higher figures in urban areas regarding coital frequency, ability to reach orgasm, overall satisfaction with sexual life, practice of premarital masturbation and knowledge about it. However, frequency of experiencing unprovoked desire seemed to be unaffected by residence. These results mean that sexual function of women resident in cities is better than those living in villages. This may be due to better level of education, sexual knowledge or socioeconomic factors.
Christensen et al. [11] concluded that men and women who had trouble in paying their bills were twice as likely to report sexual dysfunctions compared with peers without such economic troubles. In women, there was also a statistically significant trend of increasing sexual dysfunction prevalence with decreasing income. As regard masturbation practice before marriage, it was more common among participants living in cities.
In the current study 53.85% of participants living in towns and 46.15% in villages; about 80.76% of them stated that they did not know what masturbation is. This can be attributed to customs and traditions which to some extent discourage sexual education especially among females.
Abdallah et al. [12] found that sexual satisfaction seemed to be associated with residence as (26.4%) and (39.1%) of participants living in town were very and moderately sexually satisfied compared to (18.2%) and (20.5%) of women living in villages who were very and moderately sexually satisfied. Regarding masturbation (17.3%) of town residents practiced it before marriage versus (11.4%) of those living in a village and (59%) of participants living in town and (54.5%) of participants living in rural areas stated that they did not know what masturbation is. This study revealed no significant differences between both groups regarding their baseline sexual desire or orgasm (Table 2). On the same side, the study carried by Omidi et al. [13] in Iran compared the two groups in terms of primary mean scores of sexual function, sexual satisfaction, and marital satisfaction showed similarities in terms of factors and prevalence of disorders at the beginning of the study.
In the treatment arm of the present study, there was improvement in sexual dysfunction particularly in sexual desire, maintenance of lubrication, orgasm and satisfaction. Regarding the desire, the obvious change was in patients with no desire weekly pretreatment to improve from zero to 61.5% post-treatment. The orgasm differences in women who achieved orgasm less than half the time were 38.5% versus 84.6% pre- and post-treatment respectively (Table 2).
Indeed these results were opposite to the study of Dasgupta et al. [14] which included 19 women completed the 2 arms of the double-blind phase and 12 completed the optional open label extension phase. Statistically significant improvement following sildenafil was only reported in the lubrication domain of sexual function during the double-blind phase. There was no overall change in quality of life after sildenafil.
On the other hand, Berman et al. [15] found that efficacy was shown on only one sexual function measure and only in a small subsample of women who had no associated hypoactive sexual desire disorder (HSDD) and had sufficient estradiol and free testosterone concentration or were receiving estrogen and/ or androgen replacement therapy. Proposed reasons for the unconvincing efficacy of sildenafil in women have included failure to adequately characterize the study populations, differences in the physiologic response to sildenafil in men and women, and the mechanism of action of the drug needing to be central and not peripheral. It is also possible that lack of concordance between physiological and subjective aspects of women’s sexual experiences need to be further investigated [16].
This study revealed no significant association between both groups in comparison of post treatment regarding sexual dysfunction assessment except in orgasm less than half times, which become (84.6%) versus (30.8%) in sildenafil group and placebo group respectively. These results can be supported by the study of Leddy et al. [17]; 13 of 19 (68%) subjects achieved a ≥50% increase in clitoral engorgement from baseline when administered sildenafil or placebo 30 minutes after dose administration. At 60 minutes after administration, 17/19 (89%) subjects receiving sildenafil and 16/19 (84%) subjects receiving placebo had responded (P value 0.3). Also Chiver et al. [16] used self-reported measures of sexual function which showed mixed results whereas studies examining physiological effects of PDE5i on genital vasocongestion consistently report significant effects on genital sexual response.
The improvnent in FSFI in-group A may be related to increase in androgen level as there might be a positive correlation between sildenafil intake and increase testosterone blood level [18]. Also it increases the pelvic blood flow which may give more improvement in lubrication and decrease pain during sexual act and increase overall sexual satisfaction. However Lo Monte et al. [19] stated that sildenafil citrate only acts on the physical phenomena of arousal and does not completely respond to the complexity of female sexual arousal disorders (FSADs). In fact, encouraging results were achieved in specific groups of patients affected by secondary FSADs (e.g., diabetes mellitus, multiple sclerosis, chronic antidepressant users) in which the genital arousal disorder is clearly connected with a neurological or vascular injury. [3]
Also Kaplan et al. [20] reported only lubrication changes in vaginal and clitoral sensitivity in patients treated with sildenafil. When examining the effects of sildenafil on female sexual dysfunction, it was found that sildenafil may increase congestion of the vagina, but it has no effect on excitement. This difference in results can be attributed to the manner and extent of drug administration, assessment of sexual status, and cultural status of the subjects in the study. Moreover, in most studies, the sample size has been very small, which makes their validity questionable.
The limitation of this study is that it was conducted on only Egyptian patients, so further well-designed studies are needed to see if the same conclusions apply to other races. On the other hand, points of strength include among others, the good sample size and the prospective randomized double-blinded study design.
Conclusion
Sildenafil citrate seems to improve orgasm in a sample of Egyptian females with sexual dysfunction.
References
- Desilva P (1995) Sexual dysfunction in S.J.E Lindsay and G.E.Powell, The hand book of lineal and adult psychology. London and New York rout ledge (2): 199-288.
- Jaafapour M, Khani A, Khajavikhan J, Suhrabi Z (2013) Female sexual dysfunction, prevalence and risk factor and Journal of clinical and diagnostic research 7(12): 2877-2880.
- Caruso S, Rugolo S, Angello C, Intelisano G, Di Mari L, et al. (2006) Sildenafil improve sexual functioning in premenopausal women with type 1 diabetes who are affected by sexual arousal disorder. Fertil Steril 85(5): 1496-1501.
- Berman JR, Berman LA, Toler SM, Gill J, Haughie S, et al. (2003) Safety and efficacy of sildenafil citrate for the treatment of female sexual arousal disorder. Journal of Urology 170(6): 2333-2338.
- Rosen R, Brown J, Heiman J, Leiblum S, Meston C, et al. (2000) The Female Sexual Function Index (FSFI): a multidimensional self-report instrument for the assessment of female sexual function. J Sex Marital Ther 26(2): 191-208.
- Carl CB (1994) DSM-IV. Diagnostic and Statistical Manual of Mental Disorders. In: (4th edn), Washington DC: American Psychiatric Association 272(10): 828-829
- Amirkhan Z, Jangholi E, Ramezi P, Shafiei M, Saberi M, et al. (2014) Prevalence Survey of Sexual Dysfunction among Women in the Reproductive Age. Galen Medical Journal 3(1).
- Elnashar AM, El-Dien Ibrahim, El-Desoky MM, Ali OM, El-Sayd Mohamed Hassan M, et al. (2007) Female sexual dysfunction in Lower Egypt. BJOG 114(2): 201-206.
- El Gelany S, Moussa O (2013) Reproductive health awareness among educated young women in Egypt. Int J Gynecol Obestet 120: 23-26.
- Spector IP, Carey MP and Steinberg L (1996) The sexual desire inventory: Development factor, structure, and evidence of reliability. J Sex Marital Ther 22(3): 175-190.
- Christensen BS, Grønbæk M, Osler M, Pedersen BV, Graugaard C, et al. (2011) Sexual dysfunction and difficulties in Denemark: Prevelance and associated socio-demographic factors. Arch sex behave 40(1): 121-132.
- Abdallah I Y, AbdelrahmanSh (2014) female sexual dysfunction in relation to the age of marriage .thesis submitted for fulfillment of master degree in dermatology and Andrology in Banha city, Banha University, Egypt.
- Omidi A, Ahmedvand A, Najarzadan MR, Mehrzad F (2016) Compairing the effect of treatment with sildenafil and cognitive-behavioral therapy on treatment of sexual dysfunctioninwomen: arandomized controlled clinical trials. Electronic Phsicians 8(5): 2315-2324.
- Dasgupta R, Wiseman OJ, Kanabar G, Fowler CJ, Mikol D (2004) Efficacy of sildenafil in the treatment of female sexual dysfunction due to multiple sclerosis. J Urol 171(3): 1189-1193.
- Berman JR, Berman LA, Toler SM, Gill J, Haughie S, et al. (2003) Safety and efficacy of sildenafil citrate for the treatment of female sexual arousal disorder. Journal of Urology 170(6): 2333-2338.
- Chivers MI, Rosen RC (2010) Phosphodiesterase type 5 and female sexual response. Faulty protocols or paradigins? J Sex Med 7(2): 858-872.
- Leddy LS, Yang CC, Stuckey BG, Sudworth M, Haughie S, et al. (2012) Influence of sildenafil on genital engorgement in women with female sexual arousal disorder. J Sex Med 9(10): 2693-2697.
- Spitzer M, Bhasin S, Travison TG, Davda MN, Stroh H, et al. (2013). Sildenafil increases serum testosterone levels by a direct action on the testes. Andrology 1(6): 913-918.
- Lo Monte G, Graziano A, Piva I, Marci R (2014) Women taking the blue pill (sildenafil citrate) such big deal. Drug Design, Development and Therapy. Dove Press 8: 2251-2254.
- Kaplan SA, Reis RB, Kohn IJ, Ikeguchi EF, Laor E, et al. (1999) Safety and efficacy of sildenafil in postmenopausal women with female sexual dysfunction. Urology 53(3): 481-486.






























