The Importance of Oral Health in the Management of the Pregnant Woman: A Case Report
Stefania Morittu1*, Stefania Barbieri2 and Manuela Simonini2
1Dental Hygienist Perinatal and Pedodontic, Perinatal educator, Private practice in Sardinia, Italy
2Dental Hygienist Perinatal and Pedodontic, Naturopath, Private practice in Calabria, Italy
3Dental Hygienist Perinatal and Pedodontic, psychologist and psychotherapist, Perinatal educator, Private practice in Bergamo, Italy
Submission: February 19, 2021; Published: February 23, 2022
*Corresponding author: Stefania Morittu, Dental Hygienist Perinatal and Pedodontic, Perinatal educator, Private practice in Sardinia, Italy
How to cite this article: Stefania Morittu, Dental Hygienist Perinatal and Pedodontic, Perinatal educator, Private practice in Sardinia, Italy. J Gynecol Women’s Health 2022: 23(1): 556104. DOI: 10.19080/JGWH.2022.23.556104
Keywords: Oral health; Oral health education; Pregnancy
Introduction
Pregnancy is a transient physiological condition which brings about different changes in all parts of woman’s body. These complex physiological changes can affect woman oral health and compromise that of the unborn child: the maintenance of optimal conditions of the oral cavity of the woman is crucial for the best outcome of pregnancy and for the promotion of the oral health of the unborn child [1].
In recent decades, many studies have shown the association between maternal oral infections and adverse pregnancy outcomes. Existing scientific evidence emphasizes the association between the presence and severity of gum infections and premature birth, fetal growth retardation, spontaneous abortion, preeclampsia [2].
The role of these infections as a possible risk factor or co-cause of adverse pregnancy outcomes has not, however, always been confirmed while the possibility of vertical transmission, from mother to child, of bacteria that cause tooth decay has been demonstrated. Gingival bleeding often causes the pregnant woman to decrease the brushing of teeth resulting in greater accumulation of bacterial plaque and further impairment of the general state [3-4].
Dietary and oral hygiene changes, morning gravidic hyperemesis, esophageal reflux disease can cause tooth tissue demineralisation with enamel erosion and increase the risk of tooth decay if appropriate preventive interventions are not planned [5-6].
Case Report
A 33-year-old woman, 3-month pregnancy, gravidic gingivitis, no systemic pathologies.
What She Referred
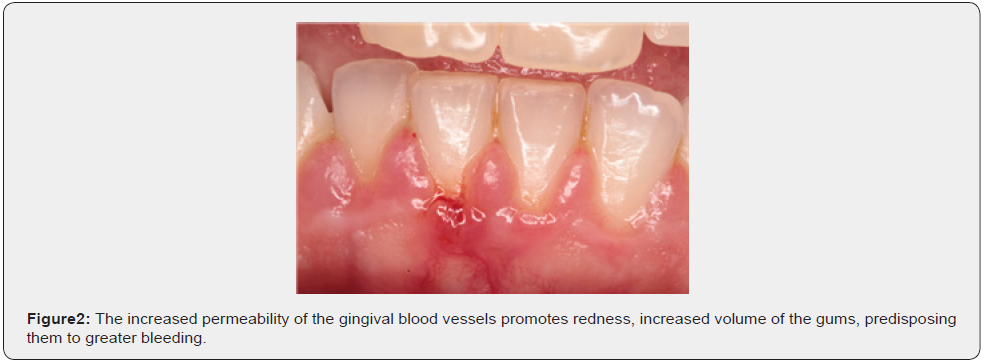
Pain in the gums, gums that bleed when brushing, swollen, tense gums, easily traumatizable, High estrogen levels, hyperemesis gravidarum. During the objective examination, we find what the patient said (Figure 1&2).
Professional Treatment
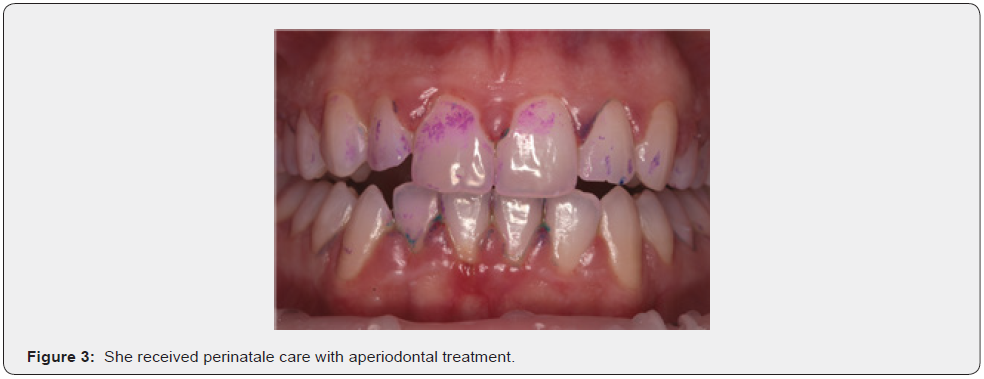
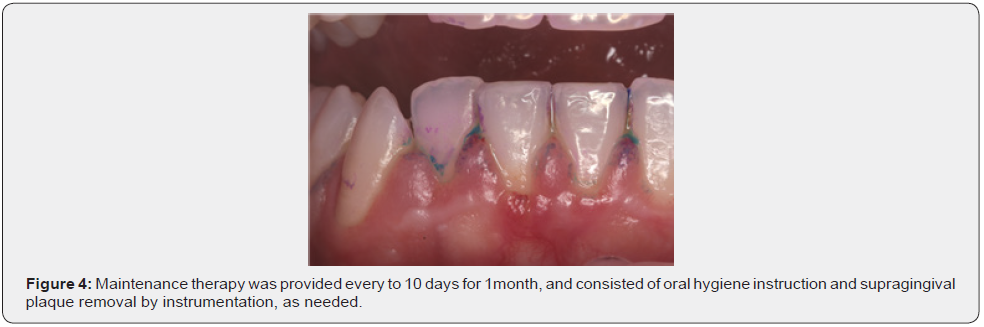
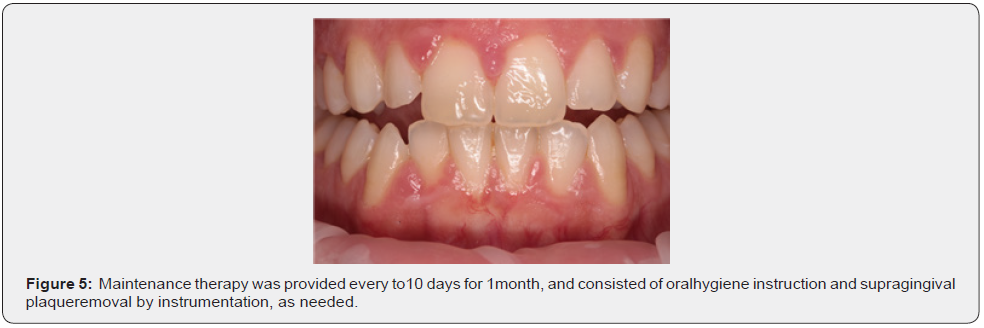
She received perinatale care with a periodontal treatment. Periodontal therapy consisted of plaque control with a tri-tone-plaque-detector, removing with airflow and scaling (Figure 3&4). Maintenance therapy was provided every to10 days for 1month, and consisted of oralhygiene instruction and supragingival plaqueremoval by instrumentation, as needed (Figure 5&6).
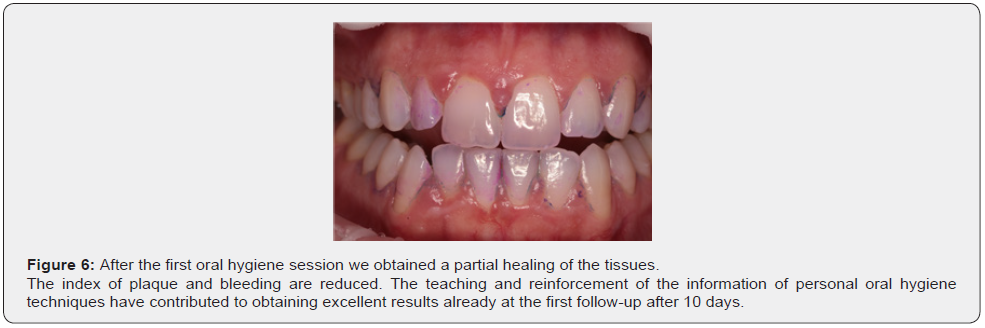
After the first oral hygiene session weobtained a partial healing of the tissues.
The index of plaque and bleeding arereduced.
The teaching and reinforcement of theinformation of personal oral hygienetechniques have contributed to obtainingexcellent results already at the first follow-upafter 10 days (Figure 7-9).
Follow-up 14 days
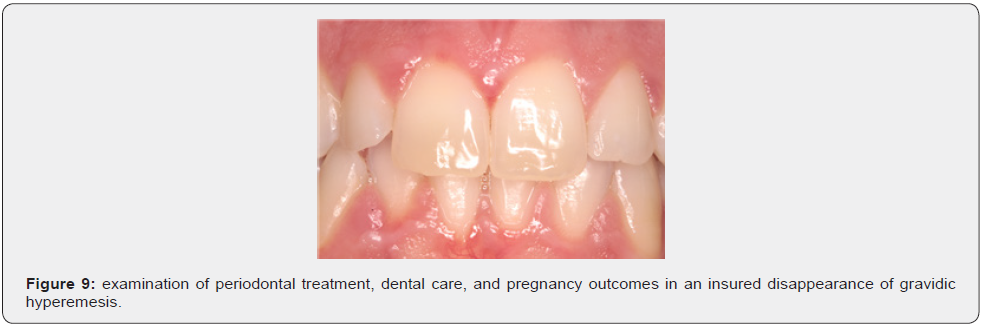
We have made dietary changes that have ledto the disappearance of gravidic hyperemesis.
Reduction of:
-plaque and bleeding index,
-gum edema,
-gums pain.
Professional perinatal treatment significantly reduced glum bleeding and inflammation.

Conclusion
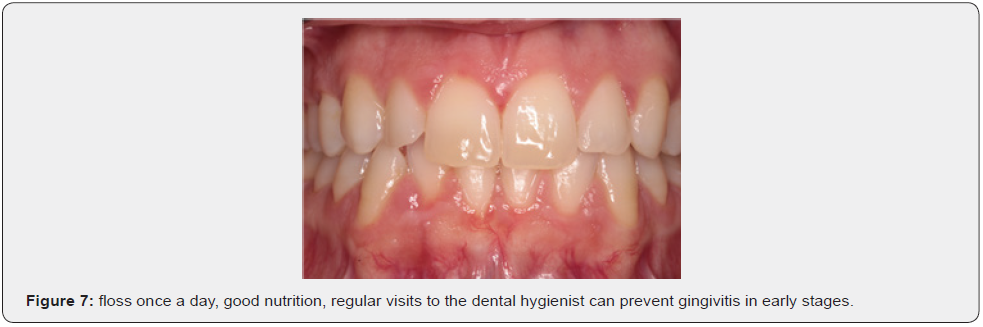
Dental procedures during pregnancy are safe and necessary: every pregnant woman should be assessed for dental hygiene habits and oral problems. The maintenance of optimal conditions of the oral cavity of the woman is crucial for the best outcome of pregnancy. Good oral hygiene, brush twice a day and floss once a day, good nutrition, regular visits to the dental hygienist can prevent gingivitisin early stages.
References
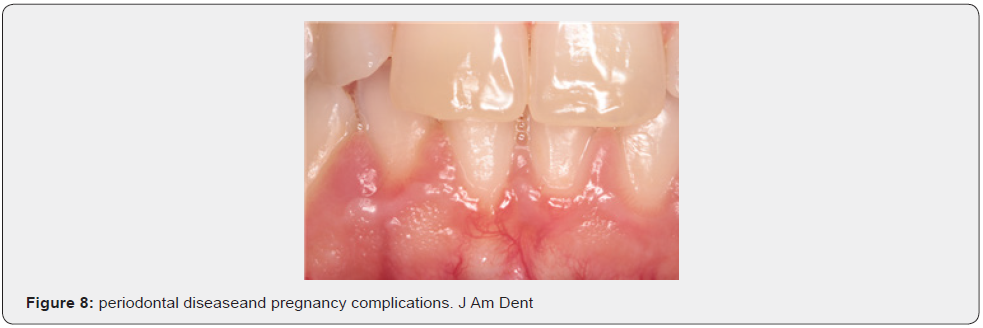
- Bobetsis YA, Barros SP, Offenbacher S (2006) Exploring the relationship between periodontal disease and pregnancy complications. J Am Dent Assoc 137 Suppl: 7S-13S.
- Gajendra S, Kumar JV (2004) Oral health and pregnancy: A review. N Y State Dent J 70(1):40-44.
- Dye BA, Vargas CM, Lee JJ, Magder L, Tinanoff N (2011) Assessing the relationship between children's oral health status and that of their mothers. J Am Dent Assoc 142:173-183.
- Albert DA, Begg MD, Andrews HF, Williams SZ, Ward A, et al. (2011) Andisappearance of gravidic hyperemesisReduction of:-plaque and bleeding index, -gum edema, -gums pain.Professional perinatal treatment significantly reduced glum bleeding and inflammation. Population in the United States. Am J Public Health 101(1): 151-156.
- Shrout MK, Comer RW, Powell BJ, Mccoy BP (1992) Treating the pregnant dental patient: four basic rules addressed. J Am Dent Asso 123(5): 75-80.
- Calabrese A, Nibali L, Rosati A, Fiengo S, Di Renzo GC, et al. (2010) Is there any association between periodontitis and preterm low birth weight? J Matern Fetal Neonatal Med 23(11): 1288-1293.






























