The Association of Serum Lead Concentration in Pregnant Women and Risk for Preterm Delivery
Zahra Salehi*, Tayebeh Jahed, Saeideh Saedi and Zahra Naiiji
Department of Gynecology, Mahdie Hospital, Shahid Beheshti University of Medical Science, Iran
Submission: November 20, 2021; Published: December 03, 2021
*Corresponding author: Zahra Salehi, Department of Gynecology, Mahdie Hospital, Shahid Beheshti University of Medical Science, Iran
How to cite this article: Zahra S, Tayebeh J, Saeideh S, Zahra N. The Association of Serum Lead Concentration in Pregnant Women and Risk for Preterm Delivery. J Gynecol Women’s Health 2021: 22(4): 556093. DOI: 10.19080/JGWH.2021.22.556093
Abstract
Background: There are strong evidence for an association between lead exposure and an increased risk of adverse pregnancy outcomes such as preterm delivery. We assessed the association of lead levels with preterm delivery by assessing the blood level of lead in pregnant women.
Methods: This cross-sectional study was conducted on 240 pregnant women who referred to Mahdiyeh Hospital (Tehran, Iran) for child delivery or termination of pregnancy that were divided into two groups as the group with preterm delivery (before 28th week of pregnancy) (n=63) and the group experienced normal delivery (delivered after 37th week of pregnancy) (n=177). The value of lead in serum samples of both groups was measured and compared.
Results: The mean serum lead level in preterm delivery group was 8.75±2.6 μg/dl and in normal delivery group was 8.88±3.8μg/dl that was similar in both groups (p = 0.326). Adjusted for age, gestational age and BMI, no association could be found between serum lead level and likelihood of preterm delivery (OR=1.012, 95%CI: 0.789-1.782, P=0.574).
Conclusion: The relationship between exposure to lead and the risk of preterm delivery may be influenced by various environmental and demographic factors, as such a relationship has not been confirmed in our society. However, it is strongly recommended that pregnant women avoid exposure to air pollutants as much as possible to avoid the potential risk of this event.
Keywords: Lead; Preterm Labor; Outcome
Abbreviations: SD: Standard Deviation; IBM: International Business Machines; BMS: Body mass index; WHO: World Health Organization; SPSS: Statistical Package for the Social Sciences
Introduction
Premature delivery refers to the onset of labor prior to the completion of 37 weeks of gestation [1]. At present, preterm delivery is one of the main health problems and after congenital abnormalities, it is the main cause of morbidity and infant mortality. Premature birth is the cause of 28% of 4 million neonatal deaths each year [1,2]. In 2005, it was estimated that 12.9 million preterm births occurred, or 9.6% of all births were premature [3]. According to a study in Tehran, the rate of preterm birth is estimated at 7.8% [4].
Despite the increasing awareness of risk factors and related mechanisms and the identification of many medical and public health interventions designed to reduce preterm labor, the rate of this event has increased in many industrialized countries. In the United States, this rate increased from 9.5 percent in 1981 to 12.7 percent in 2005 [5,6]. The cause of preterm labor is not yet fully understood, although several factors appear to play a role in the incidence of preterm labor. Suggested causes include medical and obstetric complications, lifestyle factors, genetic factors, environmental exposures, infertility treatments, behavioral factors, socio-economic indicators, history of preterm delivery, poor cervix, periodontal disease, and identification of fetal fibronectin in cervical (vaginal discharge) [7]. In some studies, preterm birth has been associated with a number of chemical and environmental exposures [8].
Today, due to the expansion of industry and the increasing consumption of fossil fuels, environmental is directly and indirectly contaminated with chemical and industrial pollutants. One of the most important components of air pollution is lead, which is an incompatible element with body tissue and, contrary to the essential elements of body tissues; it is identified as a toxin [9]. Lead is a heavy, gray-colored metal with a blue color and high applicability in the industry. Lead is widely distributed in our environment so that there is always a small amount of lead in the blood of most people [10]. Lead is considered as one of the most common environmental pollutants in today’s world. Lead and its organic and inorganic compounds are easily absorbed through the skin, respiration, and digestion systems. After entering the blood plasma, it passes through the blood-brain barrier and placental membranes and accumulates in all soft and hard tissues [11]. This element is found in various organs including the heart, bones, intestine, kidneys, and nervous system and enters the body through polluted air, water, soil, and food [12,13]. The passage of lead from the placenta to fetus around the 12th week of pregnancy leads to an increment in the blood lead level of the fetus inflicting the central nervous system during fetal and neonatal development. There is no barrier for lead to cross the fetal placental barrier, and fetal and maternal blood lead levels are approximately the same, so the fetus is at high risk of exposure to lead [14]. According to the World Health Organization (WHO), the normal level of lead in the mother’s blood is less than 10μg/dl [15]. Several mechanisms have been implicated in the relationship between preeclampsia and high level of lead. These include the oxidation and inactivation of nitric oxide, increased activity of sympathetic system, elevation of blood norepinephrine level, upregulation of beta-adrenergic receptors, increased activity of Angiotensin converting enzyme, increased plasma levels of renin, angiotensin, and aldosterone, augmented kinase activity and finally higher thromboxane production [16].
In some studies, the relationship between exposure to lead and spontaneous abortion, premature rupture of membranes, preeclampsia, fetal growth restriction, reported fetal weight loss, preterm delivery, preterm delivery has been revealed [17,18]. Therefore, preventing lead exposition in pregnant mothers is the most important way to reduce neural tube disorders and developmental abnormalities in neonatal and childhood periods. In this regard, measuring blood lead concentration in pregnant mothers and neonates may be useful to identify infants at the risk of lead poisoning. Overall, due to the wide range of adverse outcomes of preterm labor, prevention of this event and identification of its risk factors are very important. Since the increasing pollution of the environment has brought about the growth of industry in countries and among the types of pollutants, the harmful effects of lead on many aspects of human health have been well documented; we assessed the association of lead levels with preterm delivery by assessing the blood level of lead in pregnant women.
Materials and Methods
This cross-sectional study was conducted on 240 pregnant women who referred to Mahdiyeh Hospital (Tehran, Iran) for child delivery or termination of pregnancy that were divided into two groups as the group with preterm delivery (before 28th week of pregnancy) (n=63) and the group experienced normal delivery (delivered after 37th week of pregnancy) (n=177). The eligibility This cross-sectional study was conducted on 240 pregnant women who referred to Mahdiyeh Hospital (Tehran, Iran) for child delivery or termination of pregnancy that were divided into two groups as the group with preterm delivery (before 28th week of pregnancy) (n=63) and the group experienced normal delivery (delivered after 37th week of pregnancy) (n=177). The eligibility
After obtaining written informed consent, the baseline characteristics including demographics and clinical data were collected by interviewing. Then, 2ml of peripheral venous blood samples was taken via venipuncture and the collected samples were transferred to laboratory of our hospital to measure the serum level of lead. Agilent Atomic Absorption Spectrometer (Agilent Technology) was used to measure the value of lead in serum samples of pregnant women.
For statistical analysis, results were presented as mean ± standard deviation (SD) for quantitative variables and were summarized by frequency (percentage) for categorical variables. Continuous variables were compared using t test or Mann-Whitney test whenever the data did not appear to have normal distribution or when the assumption of equal variances was violated across the study groups. The categorical variables were compared using the Chi-Square test or Fisher’s exact test if required. The multivariate logistic regression modeling was used to assess the value of lead level and the risk for preterm delivery. P values of ≤ 0.05 were considered statistically significant. For the statistical analysis, the statistical software SPSS version 23.0 for windows (IBM, Armonk, New York) was used.
Result
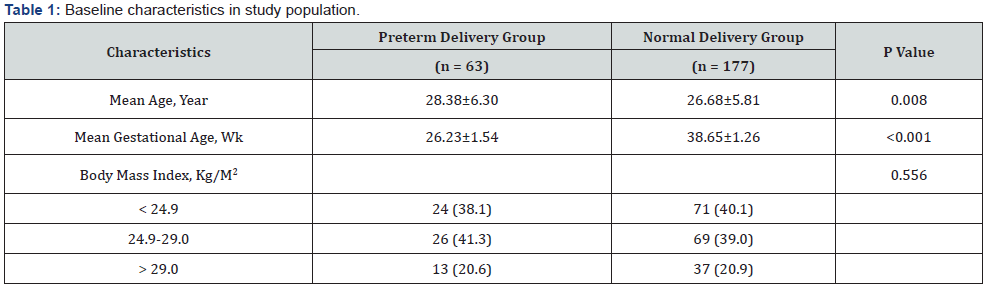
As summarized in Table 1 and with respect to baseline characteristics, those experienced preterm delivery had significantly lower average age (28.38±6.3 versus 26.68±5.8, p = 0.008). However, no difference was revealed in value of body mass index (BMI) between the two groups that the BMI values ranged 24.9-29 kg/m2 was found in 41.0% of women experienced preterm delivery while in 39.0% in those with normal delivery, while BMI higher than29kg/m2 was revealed in 21.0% and 21.0% of the women respectively.
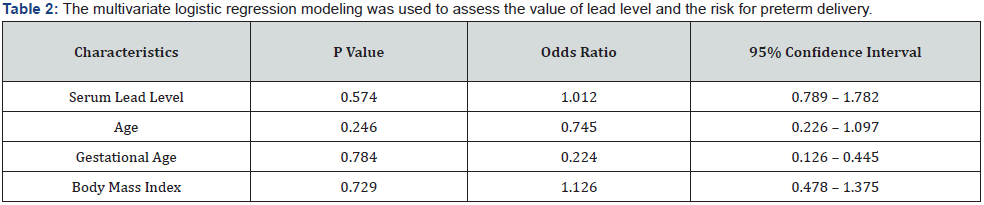
The mean serum lead level in preterm delivery group was 8.75±2.6 μg/dl and in normal delivery group was 8.88±3.8 μg/dl that was similar in both groups (p = 0.326). We found no association of serum lead level and baseline parameters of mother’s age (p = 0.556), BMI value (p = 0.249) and gestational age (p=0.283). Adjusted for age, gestational age and BMI, no association could be found between serum lead level and likelihood of preterm delivery (OR = 1.012, 95%CI: 0.789 -1.782, P=0.574) (Table 2).
Discussion
Contrary to some studies, we could not find significant association of serum lead level of mother and the risk for preterm delivery. Moreover, the serum lead level in our experience was also different as compared to some other investigations. In a study conducted by Mokhlesi et al [19], the mean blood lead level of pregnant mothers was 9.4μg/dL. A study performed by Vigeh et al [6] on 332 pregnant women at the 8-12th week of pregnancy showed that the mean blood lead level was 8.3±2μg/dL. It seems that the reason for such differences may be due to the precision of the laboratory method as well as the different living environments of the people leading different exposure position to lead poisoning. It is also noteworthy that the women in all the three mentioned studies had been in the first trimester of pregnancy while our samples were withdrawn in the third trimester. In accordance with this notion, Moura et al. [20] in their study in Brazil measured the blood lead level in 38 pregnant women during the first, second, and third trimesters and reported the levels of 8.5, 6.3, and 5.5μg/ dL respectively. Another reason for the differences observed in the blood lead level can be due to non-controllable factors such as climate, occupation, nutrition, and exposition to smoke (i.e., smoker relatives and neighbors). Studies have also shown that blood lead levels have been higher in immigrant than indigenous populations [21,22].
In the present study, there was no significant difference between the mean blood lead level comparing the preterm (75.8) and term (88.8) deliveries. In a study by Torres-Sánchez et al [23], lead levels were higher in primiparous women who had a preterm birth than in primiparous women with a fullterm birth (9.77±2.0 microgram/dl vs 8.24±2.15 microgram/ dl); this difference was marginally significant. After adjusting for other known preterm birth risk factors, the frequency of preterm birth was almost three times higher among women who had UCL levels greater or equal to 5.1 microgram/dl compared to those with lower than 5.1 microgram/dl. Contrary to the present study, Zang et al. [24] measured urine lead level in 408 pregnant women with either preterm or term deliveries. In their report, the mean level of urine lead was higher in women with preterm (6.10) than term (2.7) labor. Some other studies demonstrated a significant relationship between elevated blood lead level and preterm delivery which was inconsistent with our observation. The reason for this difference may be related to the method of lead measurement, as well as different study designs and sample sizes. Therefore, we may continue to see differences in findings related to the impact of elevated serum lead levels and the risk of preterm delivery in different communities because it seems that even with proper design and management of studies, due to the presence of multiple confounding factors associated with serum lead levels, the relationship between the two variables is greatly affected.
Conclusion
According to our results, initial assessment of serum lead poisoning may not be predictive for the likelihood of preterm delivery, meanwhile it is already recommended to prevent pregnant women’s exposure to pollutants during pregnancy by implementing comprehensive regional and national policies.
Ethics Approval and Consent to Participate
All participants signed the informed consent form. The project was approved by the Local Research Ethics Committee (Shahid Beheshti University of medical sciences, Iran).
References
- Lawn JE, Gravett MG, Nunes TM, Rubens C, Stanton C, et al. (2010) Global Report on Preterm Birth and Stillbirth (1 Of 7): Definitions, Description of The Burden and Opportunities to Improve Data. BMC Pregnancy and Childbirth 10(S1).
- Jeff AK, John PN (2017) Recent advances in the prevention of preterm birth. F1000Res 6.
- Brown K, Langston-Cox A, Unger HW (2021) A Better Start to Life: Risk Factors for, and Prevention of, Preterm Birth in Australian First Nations Women - A Narrative Review. Int J Gynaecol Obstet 155(2): 260-267.
- Nasibeh S, Somayyeh K, Reza P, Azita FK, Hashemmieh Ch, et al. (2017) Investigating the Prevalence of Preterm Birth in Iranian Population: A Systematic Review and Meta-Analysis. J Caring Sci 6(4): 371-380.
- Breslin N, Gyamfi-Bannerman C (2020) Current Preterm Birth Prevention Strategies. Clin Perinatol 47(4): 705-717.
- Vigeh M, Yokoyama K, Shinohara A, Afshinrokh M, Yunesian M, et al. (2010) Early pregnancy blood lead levels and the risk of premature rupture of the membranes. Reprod Toxicol 30(3): 477-480.
- Natalie S, Lisa S, Andrew S (2019) The prediction of preterm delivery: What is new? Semin Fetal Neonatal Med 24(1): 27-32.
- Fernandes JMPA, Aguiar PPY, Vaz JA, Pereira AR, Barbieri CLA, et al. (2021) Association between high-risk pregnancy and environmental contaminants in the Metropolitan Region of Baixada Santista, Brazil. Environ Sci Pollut Res Int.
- Zhang Y, Zhang W, Huang J, Zhong X, Liu Y, et al. (2021) Lead contamination status and assessment of potential risk to human health of commercial foods in Guangzhou City in 2017-2019. Wei Sheng Yan Jiu 50(5): 832-836.
- Muntner P, Menke A, DeSalvo K, Rabito F, Batuman V, et al. (2005) Continued decline in blood lead levels among adults in the United States: The National Health and Nutrition Examination Surveys. Arch Intern Med 165(18): 2155-2161.
- Flora G, Gupta D, Tiwari A (2012) Toxicity of lead: a review with recent updates. Interdiscip Toxicol 5(2): 47-58.
- Flora SJS, Flora G, Saxena G (2006) Environmental occurrence, health effects and management of lead poisoning. Amsterdam: Elsevier Publication, 158-228.
- Vij AG (2009) Hemopoietic, hemostatic and mutagenic effects of lead and possible prevention by zinc and vitamin C. Al Ameen J Med Sci 2(2): 27-36.
- Raymond LW, Ford MD, Porter WG, Saxe JS, Ullrich CG, et al. (2002) Maternal-fetal lead poisoning from a 15-year-old bullet. J Matern Fetal Neonatal Med 11(1): 63-66.
- Raymond LW (2009) Maternal-fetal lead poisoning from an old slug: 10-year follow-up. J Matern Fetal Neonatal Med 22(6): 543-544.
- Shannon M (2003) Severe lead poisoning in pregnancy. Ambul Pediatr 3(1): 37-39.
- La-Llave-León O, Salas PJM, Estrada MS, Esquivel RE, Castellanos JFX, et al. (2016) The Relationship Between Blood Lead Levels and Occupational Exposure in a Pregnant Population. BMC Public Health 16.
- Perkins M, Wright RO, Amarasiriwardena CJ, Jayawardene I, Rifas-Shiman SL, et al. (2014) Very low maternal lead level in pregnancy and birth outcomes in an eastern Massachusetts population. Ann Epidemiol 24(12): 915-919.
- Mokhlesi S, Moghaddam-Banaem L, Lamyian M, Alyianmoghadam N, Safari K, et al. (2013) Prediction of Preeclampsia Based on Blood Lead Levels in Early Pregnancy. J Shahrekord Univ Med Sci 15(6): 44-53.
- Moura M, Valente JG (2002) Blood Lead Levels During Pregnancy in Women Living in Rio De Janeiro, Brazil. Sci Total Environ 299(1-3): 123-129.
- Levin SM, Goldberg M (2000) Clinical evaluation and management of lead-exposed construction workers. Am J Ind Med 37(1): 23–43.
- Patrick L (2006) Lead toxicity, a review of the literature. Part 1: exposure, evaluation, and treatment. Altern Med Rev 11(1): 2-22.
- Torres-Sánchez LE, Berkowitz G, López-Carrillo L, Torres-Arreola L, Ríos C, et al. (1999) Intrauterine lead exposure and preterm birth. Environ Res 81(4): 297-301.
- Bin Z, Wei X, Yuanyuan L, Bryan AB, Aifen Z, et al. (2015) Prenatal exposure to lead in relation to risk of preterm low birth weight: A matched case-control study in China. Reprod Toxicol 57: 190-195.






























