Cesarean Hysterectomy: A 10-Year Retrospective Review in Jeddah, Saudi Arabia
Abdulrahim Gari1,2*, Fadwah Tahir1, Hassan Latifah2, Bander Hafidh2, Afaf Tawfiq2 and Musab Almatrafi3
1Department of Obstetrics and Gynecology, Umm Al-Qura University, Saudi Arabia
2Department of Obstetrics and Gynecology, King Faisal Specialist Hospital and Research Centre, Saudi Arabia
3Department of Obstetrics and Gynecology, King Abdulaziz Medical City, Saudi Arabia
Submission: July 27, 2005-2011; Published: August 04, 2021
*Corresponding author: Abdulrahim Gari, Department of Obstetrics and Gynecology, Umm Al-Qura University and King Faisal Specialist Hospital and Research Centre, Saudi Arabia
How to cite this article: Abdulrahim G, Fadwah T, Hassan L, Bander H, Afaf T, et al. Cesarean Hysterectomy: A 10-Year Retrospective Review in Jeddah, Saudi Arabia. J Gynecol Women’s Health. 2021: 22(1): 556078. DOI: 10.19080/JGWH.2021.22.556078
Keywords: Vulnerability; COVID-19; Women; Geo-political; Gender diplomacy;
Abstract
Objectives: This study aimed to review the most significant obstetrical, gynecological, and surgical findings in the history of peripartum hysterectomy patients in the last 10 years at a tertiary care center in Saudi Arabia.
Methods: This is a 10-year retrospective review conducted at King Faisal Specialist Hospital & Research Centre, Jeddah, between 2009 and 2019, including 41 cases of cesarean hysterectomy among 10,752 deliveries.
Result: The mean age was 33.5 ± 5.6 years. Sixty-one percent of the patients were diagnosed with placenta accreta, followed by 22% with placenta increta, and the remaining 17.1% with placenta percreta. Of which, 31 (76%) women underwent total abdominal hysterectomy and the remainder underwent subtotal hysterectomy. No significant associations were observed between the 3 types of vascular ligation methods used and the risk of complications, except for intraoperative bleeding. Ultrasound (US) showed slightly greater odds at being consistent with histopathological findings compared to the combined methods of magnetic resonance imaging and US. Intravascular occlusive balloon was more effective in minimizing intraoperative blood loss compared to other vascular ligatures.
Conclusion: Peripartum cesarean section due to placenta accreta, increta, and percreta is an obstetrical emergency with high rates of operative morbidity and mortality. The cases should be referred to specialized centers experienced in those cases to minimize the perioperative complications and mortalities affecting the patient and the fetus.
Keywords: Cesarean section; C-section; Cesarean hysterectomy; Peripartum hysterectomy
Abbreviatations: US: Ultrasound; CS: Cesarean Section; KAMC: King Abdullah Medical City; CD: Cesarean Delivery; PH: Peripartum Hysterectomy; MRI: Magnetic Resonance Imaging; SDs: Standard Deviations
Introduction
The last decade witnessed a dramatic increase in the cesarean section (CS) rate worldwide, including Saudi Arabia. The Kingdom’s current estimation rate of CS is 45% in some centers [1]. A previous epidemiological report showed that the CS rate significantly increased by 80.2%, from 10.6% in 1997 to 19.1% in 2006 [2]. Moreover, the last 2 decades witnessed a significant increase in the CS birth rates in most of the centers, including King Abdullah Medical City (KAMC), Riyadh, Saudi Arabia. The increase at KAMC was from 8% to 21% between 1993 and 2013, and in 2016, the rate increased to 27% of all deliveries [3]. Another study conducted in late 2016, using the National In-patient Sample, reported an overall placenta accreta rate of 1/272 women who had a birth-related hospital discharge diagnosis in the United States, which is higher than any other published study. The increasing rate of placenta accreta over the past 4 decades is most likely due to the increase in its risk factors, mainly cesarean delivery (CD) rates [4]. Placenta accreta is an abnormal adherence of the placenta to the uterine wall, secondary to a defect in the decidua [5]. Placenta accreta spectrum, formerly known as morbidly adherent placenta, refers to the range of pathologic adherence of the placenta, including a) attaching too firmly into the uterus or placenta accreta, b) attaching more deeply into the muscle wall of the uterus or placenta increta, and c) even extending to nearby organs or placenta percreta. Due to these conditions, the placenta does not entirely separate from the uterus after birth, resulting in life-threatening bleeding and emergency hysterectomy, accounting for 51.1% of emergency hysterectomies [5]. The removal of the uterine corpus (alone or with the cervix) at the time of CS, or shortly after a vaginal delivery, is one of the high-risk and more critical operations in modern obstetrics [6]. Maternal morbidity and mortality have been reported to occur in up to 60% and 7%, respectively, in women with placenta accreta3. Furthermore, the incidence of perinatal complications has also increased mainly due to preterm birth and small for gestational age fetuses [7]. Regarding management, peripartum hysterectomy (PH) is an emergency procedure performed to prevent maternal mortality [8]. PH may be performed after CD whereas postpartum hysterectomies are performed after vaginal delivery [9]. The incidence of PH is less than 1/1000 deliveries in developed countries and 11/1000 deliveries in developing countries [9]. Hemorrhage from placenta accreta spectrum carries a higher risk of hysterectomy than surgical trauma/tears or uterine atony. Subsequently, cesarean hysterectomy has become a common procedure, carrying significant morbidity and even mortality when performed in a hospital without experienced personnel or high-level supportive care, such as anesthesia, blood bank, and ICU. This could potentially result in a hysterectomy at the time of delivery or during the postpartum period with a longer hospital stay [4,10,11]. The main obstetric complications associated with CS/CD include maternal mortality, postpartum infection, uterine rupture, bladder injury, abnormal placentation, ectopic pregnancy, stillbirth, preterm birth, and others [12-14]. In addition, evidence suggested the role of CS in altering the hormonal and microbiological physiology of the infant as compared to vaginal delivery [1]. The conventional alternatives include leaving the placenta in situ at the time of CD and allowing later reabsorption or expulsion to occur [15]. Furthermore, methotrexate may be administered to enhance the resolution and has been reported to reduce the size of retained placenta and serum beta-human chorionic gonadotropin to an undetectable level [15]. In general, conservative surgical approaches must be improved to increase the longevity of pregnant women undergoing CS with possible peripartum hysterectomies and lower premature fetal-related complications [16,17]. This study aimed to review the most significant obstetrical, gynecological, and surgical findings in the history of PH patients in the last 10 years at a tertiary care center in Saudi Arabia.
Methods
Study design
This is a 10-year retrospective review conducted at King Faisal Specialist Hospital & Research Centre (KFSH&RC) in Jeddah, including 41 cases of cesarean hysterectomy among 10,752 deliveries, between 2009 and 2019. Cesarean hysterectomy was identified as the removal of the uterus at the time of the planned or unplanned (emergency) cesarean delivery. Most of the patients suspected or at risk of peripartum hysterectomy were referred from a secondary care hospital to King Faisal Specialist Hospital and Research Center or other tertiary center.
Procedure
Patients were admitted and assessed by a maternal-fetal medicine specialist, and in cases where abnormal placentation was the reason for referral, Doppler ultrasound (US) and magnetic resonance imaging (MRI) was obtained. Patients were either booked electively and taken to the operating room in conjunction with a gynecologic oncologist. Blood tests were requested in advance and patients were assessed preoperatively using anesthesia. ICU was reserved for such cases. The surgery was performed via a midline incision in the lithotomy position. There was a trend to insert intravascular occlusion (by an interventional radiologist) in the first 5 years, but this has changed once data became available showing a high incidence of complications than previously known. The placenta was not removed, except in few cases, to save the uterus. In addition, data summery sheet was developed to extract relevant information from the patient history, preoperative investigation, operative record, postoperative care plus complication, and neonatal outcomes.
Ethical consent
The study was approved by the ethical committee at KFSH&RC. Informed consent was obtained from participants before the commencement of the study and we followed the principles of Helsinki declarations in our research.
Statistical Analysis
Reports were collected, coded, and revised. The data were analyzed using the Statistical Package for Social Sciences logistic, version 20 (IBM Corp., Armonk, NY, USA). Since this was a descriptive study, the normality of continuous variables was tested using the Shapiro-Wilk test. All statistical analyses were conducted using 2-tailed tests with an alpha error of 0.05. P-value less than 0.05 was considered to be statistically significant. Frequencies and percentages were used to describe the categorical variables whereas means ± standard deviations (SDs) were used to express continuous variables. Differences in categorical variables were analyzed using the Pearson chi-square test or Fisher’s exact test when conditions were not fulfilled. Mean differences were analyzed using independen samples t-test or non-parametric Mann-Whitney U tests. The logistic regression model was used to explain the association between the initial diagnostic imaging method used, the postoperative total complications, and the odds of having a consistent diagnosis using histopathological studies.
Result
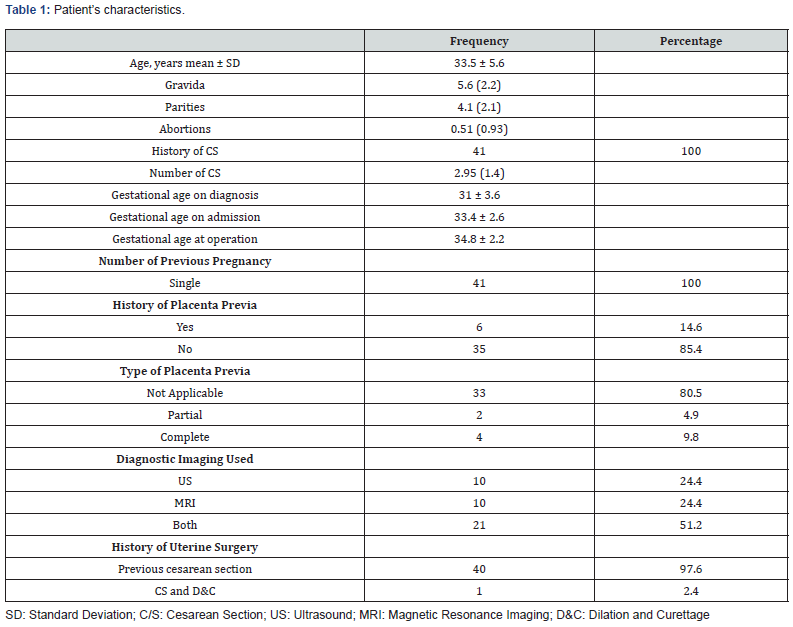
Table 1 shows participants’ characteristics. Their mean age was 33.5±5.6 years, ranging between 22 and 47. The pregnancy history revealed 5.6±2.2 pregnancies, and their complete pregnancies or full-term pregnancies were on average equal to 4.1+2.1 pregnancies. The abortion history showed that these women underwent 0.51±0.93 abortions on average, and all of them had a history of CS with a mean of 2.95 (approximately 3 abortions) on average. The mean gestational age at the time of diagnosis was 31±3.6 weeks, and their gestational age at the time of admission was 33.4±2.6 weeks. However, their gestational age at the time of operation was approximately higher, 34.8±2.2 weeks. All of them had singletone pregnancies, and none of them had twins or higher. Moreover, their gynecological history showed that only 6 of them (14.6%) had a history of placenta previa, whereas the remaining (majority) did not. The types of placenta previa observed in the 6 women were distributed as follows: 2 (4.9%) partial placenta previa and 4 (9.8%) complete placenta previa.
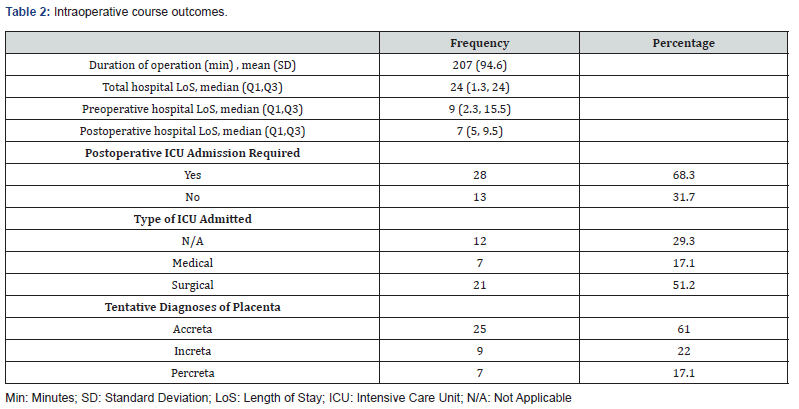
All of the patients underwent operative intervention, with an overall operative time of 207 + 94.6 minutes and a median in-hospital length of stay of 24 days. In brief, the total in-hospital stay was 24 days or less for 75% of them, whereas a quarter of them stayed 1.3 days or less. The majority required an immediate ICU admission after the surgery (68.3%), and the remaining (31.7%) were transferred to the general hospital obstetric postpartum floors. Sixty-one percent were diagnosed with placenta accreta, followed by 22% diagnosed with increta (22%), and the remaining 17.1% with Percreta (Table 2).
Overall, 33 women required vascular occlusive interventions (Table 3). The most employed vascular ligation method was internal iliac ligation (51.2%), followed by uterine artery ligation (22%) and internal iliac balloons (7.3%). Of these women, only 4(9.8%) required intra-abdominal packing, in which 3 (7.3%) of them had their abdominal packing kept for 24-hours and only one (2.4%) had her abdominal pack past 72 hours. The mean total intraoperative blood loss for these women was estimated to be equal to 1891.5 ±1319 cubic centimetre (cc) and the majority (n = 35, 85.4%) had blood loss >=1000 cc. Accordingly, 78% required blood transfusion: 33 (61%) required Packed Red Blood Cells “PRBCs,” 14 (25.9%) required Fresh Frozen Plasmas “FFPs,” and 7 (13%) required Platelets.
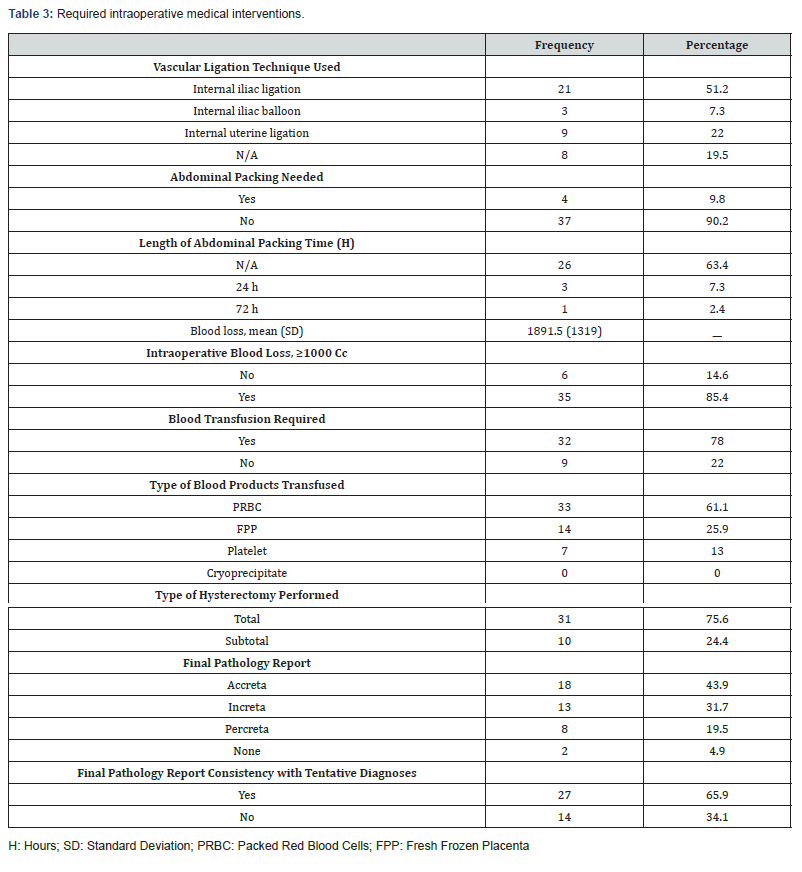
A total of 31 (76%) women underwent a total hysterectomy and the remainder underwent subtotal hysterectomy. Almost half of the patients (43.9%) had accreta, 31.7% had increta, 19.5% had percreta, and histopathological (4.9%) reports of 2 women were clear of any definitive diagnosis abnormal placentation. On the other hand, 27 (65.9%) had their final histopathological findings aligned with those found using medical imaging methods.
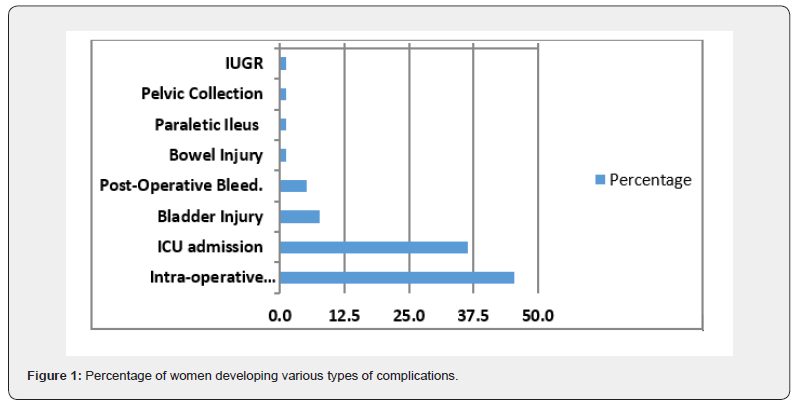
Figure 1 shows the percentage of each complication reported. The most frequent complication encountered by these women was the intraoperative hemorrhage with blood loss of more than 1000cc (n =35, 46%), followed by the intensive condition requiring admission to the critical care unit (n = 28, 36%), bladder injury (n =6, 8%), postoperative bleeding (n = 4, 5%), and the rest included bowel injury, paralytic ileus, pelvic collection, and a child with IUGR, (n = 1, 1.3% each).
Information on neonates are collected as well. The average weight for all the neonates was 2320.7± 712 gm, and their overall mean gestational age at birth time 34.1±6 weeks. Only one child was born with low birth weight for their gestational age, and 6 had a higher weight for their gestational age (14.6%). The Apgar score provides a convenient shorthand for reporting the status of the newborn infant and the response to resuscitation [15]. Their viability mean Apgar scores at 1 minute was 6.2 and at 5 minutes their overall mean Apgar score increased to 8.2 of 10 points.
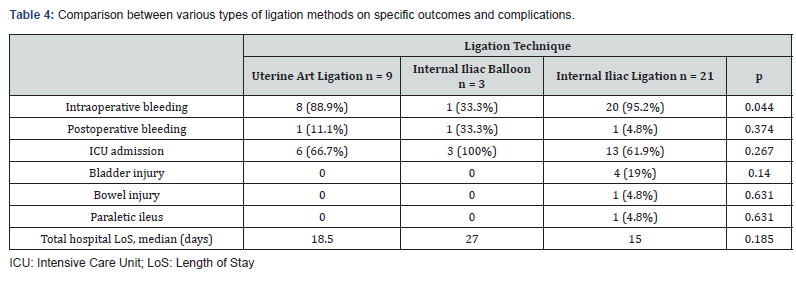
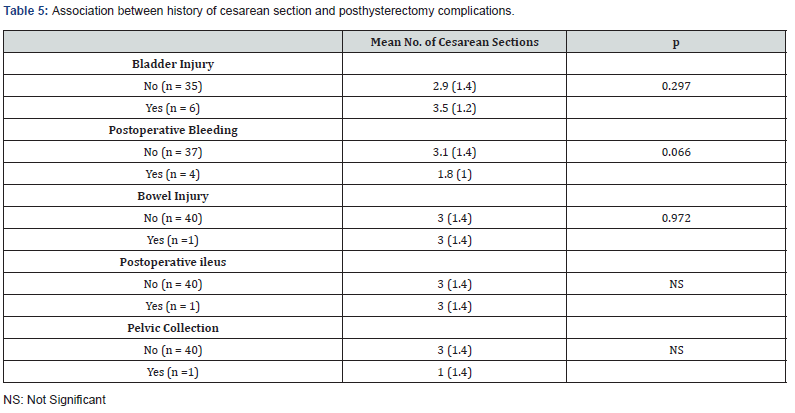
No significant associations between the 3 types of ligation methods used and the risk of complications except for intraoperative bleeding, with internal iliac balloon therapy being the least reporting bleeding whereas internal iliac ligation scoring the highest (95.2%) (Table 4). Women who developed postoperative bleeding (mean = 3.1, SD = 1.4) had slightly greater number of previous CS when compared to those who did not experience postoperative bleeding (mean = 1.8, SD = 1.4), p = 0.066. None of the other complications showed statistically significant differences in the mean number of previous CS (Table 5).
We found 65.9% (n = 27) of these women had antenatal imaging-based diagnoses in alignment with the final histopathological diagnoses. The overall reliability of the various medical imaging modalities in diagnosing placenta accreta was 88.9% and 46.5% at diagnosing placenta increta. However, their overall reliability in diagnosing placenta percerta was 62.5%. Women who underwent either total or subtotal hysterectomies do not differ statistically in their respective groups (obstetrics and gynecology history, parity, ICU admission, operative time, and the amounts of blood loss).
We compared 2 imaging modalities (US and MRI) to show the differential ability of each imaging technique in diagnosing the problems accurately and a multiple logistic regression model was applied. Despite that our sample size was too small in light of the multiple regression techniques, we used it to better understand the association and to produce a propensity score that will help us show visually how various medical imaging techniques employed by practitioners will demonstrate various inconsistency with those found with definitive laboratory findings using the histopathological tissue diagnosis. Our predictor to subject ratio was (1 predictor: 8.2 subjects). As such, we created a new binary dichotomous variable that showed whether a mismatch between interim diagnoses and the final definitive diagnoses was noted, which was coded as follows (0= an Inconsistent diagnosis, 1= consistent diagnoses) with consistent diagnoses denoting that both interim and definitive diagnoses are in agreement, regardless of what type of diagnoses was recorded, for example, increta, perecreta, and accreta. The model was not statistically significant, but it suggested that the US had slightly greater odds at being consistent with histopathological findings compared to the combined methods of (MRI and the US) when applied, those who undergo MRI alone are at odds equivalent to (1-0.764= 0.236 times) being less accurate in diagnosing these problems (or consistently matching with final histopathological findings) compared to using the combined methods of US and MRI.
Discussion
The incidence of emergency Peripartum Hysterectomy (PH) varies from 0.24 to 5.09 per 1,000 deliveries in the literature [18]. Previous CS, advanced maternal age, and abnormal placentation (including placenta previa) were considered to be risk factors for peripartum hysterectomy [19]. Increased incidence of CS and placenta previa spectrum were found to play a role in the increasing number of peripartum or emergency hysterectomies [18-24]. Many previous studies suggested the association between previous CD and a higher risk of hysterectomy [8]. Thus, in this study, all the enrolled patients had undergone previous CS, and we evaluated the diagnostic tool used for the confirmation of clinical diagnosis [25,26]. It was found that only 65.9% had their final histopathological findings aligned with those found using imaging methods, whereas 34.1% had different definitive diagnoses using the histopathological findings that contradicted those found using imaging methods such as US, MRI or a combination of both. The most frequently reported complications in terms of occurrence were intraoperative hemorrhage (blood loss of more than 1000cc), followed by admission to the critical care unit, bladder injury, postoperative bleeding, bowel injury, and paralytic ileus. Despite significant advancements in medical technologies and sciences, these complications remain a contributing factors to maternal morbidity and mortality [27,28]. Women who underwent either total or subtotal hysterectomies do not differ statistically on their respective obstetrics and gynecology histories of gravidity and parity, the likelihood for ICU admission, or their gestational ages at admission, neither the operative time and the amounts of blood loss intraoperatively. In Nigeria, Obiechina et al. [29] reported postoperative morbidities in their patients included postoperative fever (37.9%), postoperative anemia (24.1%), wound infection (20.7%), disseminated intravascular coagulopathy (10.3%), and urinary tract infection (6.9%) [29]. These findings contradict the complications reported in our study where it was not common and we did not look at it in our study. These differences could be attributed to variations in the local health care system and probably difficult to find a justification for. The most frequent complications encountered in the present study were intraoperative hemorrhage with blood loss of more than 1000 cc (46%), followed by the intensive condition requiring admission to the critical care unit (36%), and bladder injury (6, 8%). Similar findings were reported by Choi et.al in his study [30]. In contrast, a recent retrospective study by Kang et al. [31] reported a lower rate of urinary tract injury after a hysterectomy of 1.1%, (bladder injury was accounted in 0.8%) compared to 8% in our study.
Considering neonatal evaluation, the findings of the study were similar to those reported in the previous literature by Rotem et al. [32] Though various attempts have been performed to assess the prevalence of peripartum hysterectomies, very few assessed the diagnostic efficiency of the tools considered [33-35]. This is quite alarming considering the treatment-associated changes in quality of life, even if for a temporary period. We found that the US had slightly greater odds of being consistent with histopathological findings compared to the combined methods of MRI and the US when applied well. No significant difference was observed between the 3 types of ligation methods used intraoperatively for these women nor their likelihood of either complication of postoperative bleeding or the need for ICU admission besides other types of injury, such as bladder and bowel wall injuries and paralytic ileus, as in the case of previous studies [36,37]. The operative time was not affected by the type of ligation used among all the patients in our study. Internal iliac ligation was used in 21 patients and scored the highest rate of intraoperative bleeding (95%) more than 1L compared to internal iliac occlusive balloon. A study by Camuzcuoglu et al. [38] reported that while evaluating the effect of internal iliac artery ligation in PH, the authors observed several complications such as bladder injury (3%), renal failure (12.1%), ovary removal (3%), and even maternal mortality (9.1%). Furthermore, internal iliac artery balloon occlusion catheter had the least reported bleeding among other techniques in our study (33.3%). There were only 3 cases managed with occlusive balloon in our study, and it is probably difficult to conclude the superiority. Chung et al. [39] reported that using the occlusive balloon immediately before CD could decrease perioperative blood loss in invasive placenta and placenta previa cases. Besides, recent evidence showed that uterine artery ligation prior to the delivery of the placenta in placenta accreta cases can effectively reduce the amount of intraoperative blood loss and postpartum hemorrhage and the risk of other complications [40]. In our study, there was no significant difference between internal iliac artery ligation and uterine artery ligation concerning intraoperative blood loss, although the number of patients was not equal on each arm (internal iliac artery and uterine artery ligation); probably having an equal number of patients may change the findings.
The current study has some limitations. First, this is a retrospective study with the risk of underreporting data, incomplete data collection, insufficient information on the possible confounder, and lack of data quality. Second, this is a single-center, small sample-sized study, thus limiting the generalizability of its findings. Nonetheless, the main strength of this study is the duration of the study (10 years) and all the studies were conducted by the same team, following the same accreta pathway. Emergency PH must be considered as a critical emergency hysterectomy and performed early in postpartum due to the possible relation with the delivery. More attention should be given to women with the risk of any placental pathology (history of CD or placenta previa) or those diagnosed by ultrasonography and MRI. It must be noted throughout this study the importance of avoiding unnecessary cesarean deliveries to avoid additional complications. Larger epidemiological investigations are warranted in the future to make a vigorous statement on these topics.
Conclusion
Peripartum Hysterectomy due to placenta accreta, increta, and percreta is an obstetrical emergency with high rates of operative morbidity and mortality. Precautions should be taken in cases of placenta previa and/or placenta accreta with previous CS, because special preparations, surgical skills, and experience are needed. These cases should be referred to a specialized center with experienced personnel staff (anesthesia, blood bank, vascular, and urology services, etc.) to minimize the perioperative complications and mortalities affecting the patient and fetus. However, further research is warranted to investigate the best technique to minimize blood loss and other transfusion-related complications.
Acknowledgment
KFSH anaesthesia department and Operating room staff
References
- Cegolon L, Mastrangelo G, Maso G, Pozzo G, Ronfani L, et al. (2020) Understanding factors leading to primary cesarean section and vaginal birth after cesarean delivery in the friuli-venezia giulia region (North-Eastern Italy), 2005-2015. Sci Rep 10: 380.
- Ba’aqeel HS (2009) Cesarean delivery rates in Saudi Arabia: A ten-year review. Ann Saudi Med 29(3): 179-183.
- Ahmed AE, Mohammad RS (2018) Cesarean Sections. Associated factors and frequency at king abdulaziz medical city in the central region of the kingdom of Saudi Arabia. Saudi Med J 39(11): 1154-1157.
- Cahill AG, Beigi R, Heine RP, Silver RM, Wax JR, et al. (2018) Placenta Accreta Spectrum. Am J Obstet Gynecol 219(6): B2-B16.
- Ballas J, Hull AD, Saenz C, Warshak CR, Roberts AC, et al. (2012) Preoperative intravascular balloon catheters and surgical outcomes in pregnancies complicated by placenta accreta: a management paradox. Am J Obstet Gynecol 207(3): 216.e1-5.
- Castaneda S, Karrison T, Cibils LA (2000) Peripartum Hysterectomy. J Perinat Med 28(6): 472-481.
- Eshkoli T, Weintraub AY, Sergienko R, Sheiner E (2013) Placenta Accreta: Risk factors, perinatal outcomes, and consequences for subsequent births. Am J Obstet Gynecol 208(3): 219.e1-7.
- Van den Akker T, Brobbel C, Dekkers OM, Bloemenkamp KWM (2016) Prevalence, Indications, Risk Indicators, and Outcomes of Emergency Peripartum Hysterectomy Worldwide: A Systematic Review and Meta-Analysis. Obstet Gynecol 128(6): 1281-1294.
- Rossi AC, Lee RH, Chmait RH (2010) Emergency postpartum hysterectomy for uncontrolled postpartum bleeding: A systematic review. Obstet Gynecol 115(3): 637-644.
- Usta IM, Hobeika EM, Musa AAA, Gabriel GE, Nassar AH, et al. (2005) Placenta Previa-Accreta: Risk Factors and Complications. Am J Obstet Gynecol 193(3 pt 2): 1045-1049.
- Marshall NE, Fu R, Guise JM (2011) Impact of multiple cesarean deliveries on maternal morbidity: A systematic review. Am J Obstet Gynecol 205(3): 262.e1-262.e8.
- Mascarello KC, Horta BL, Silveira MF (2017) Maternal complications and cesarean section without indication: Systematic review and meta-analysis. Rev Saude Publica 51: 105.
- Franchi M, Raffaelli R, Baggio S, Scollo M, Garzon S, et al. (2019) Unintentional Transvesical caesarean section: incidence, risk factors, surgical technique and post-operative management. Eur J Obstet Gynecol Reprod Biol 236: 26-31.
- Sandall J, Tribe RM, Avery L, Mola G, Visser GH, et al. (2018) Short-Term and Long-Term effects of caesarean section on the health of women and children. Lancet 392(10155): 1349-1357.
- Grace Tan SE, Jobling TW, Wallace EM, McNeilage LJ, Manolitsas T, et al. (2013) Surgical management of placenta accreta: a 10-year experience. Acta Obstet Gynecol Scand 92(4): 445-450.
- ElkhoulyNI, Solyman AE, Anter ME, Sanad ZF, El Ghazaly AN, et al. (2020) A new conservative surgical approach for placenta accreta spectrum in a low-resource setting. J Matern Fetal Neonatal Med, pp. 1-7.
- Uysal D, Cokmez H, Aydin C, Ciftpinar T (2018) Emergency peripartum hysterectomy: A retrospective study in a tertiary care hospital in Turkey from 2007 to 2015. JPMA J Pak Med Assoc 68(3): 487-489.
- Carvalho J, Cubal A, Torres S (2021) Emergency peripartum hysterectomy: A 10-Year Review.
- Yoong W, Massiah N, Oluwu A (2006) Obstetric hysterectomy: changing trends over 20 years in a multiethnic high risk population. Arch Gynecol Obstet 274(1): 37-40.
- Lau WC, Fung H (1997) Ten years experience of caesarean and postpartum hysterectomy in a teaching hospital in Hong Kong. European Journal of Obstetrics and Gynecology and Reproductive Biology 74(2): 133-137.
- Yildirim GY, Koroglu N, Akca A, Talmac M, Dikmen S, et al. (2021) What is new in peripartum hysterectomy? A seventeen year experience in a tertiary hospital. Taiwan J Obstet Gynecol 60(1): 95-98.
- Huque S, Roberts I, Fawole B, Chaudhri R, Arulkumaran S, et al. (2018) Risk factors for peripartum hysterectomy among women with postpartum haemorrhage: analysis of data from the woman trial. BMC Pregnancy Childbirth 18(1): 186.
- Sahin S, Guzin K, Eroğlu M, Kayabasoglu F, Yaşartekin MS, et al. (2014) Emergency peripartum hysterectomy: Our 12-Year Experience. Arch Gynecol Obstet 289(5): 953-958.
- Temizkan O, Angın D, Karakuş R, Şanverdi İ, Polat M, et al. (2016) Changing trends in emergency peripartum hysterectomy in a tertiary obstetric center in Turkey during 2000-2013. J Turk Ger Gynecol Assoc 17(1): 26-34.
- Wani RV, Abu-Hudra NMS, Al-Tahir SI (2014) Emergency peripartum hysterectomy: A 13-Year review at a tertiary center in Kuwait. J Obstet Gynaecol India 64(6): 403-408.
- Tapisiz OL, Altinbas SK, Yirci B, Cenksoy P, Kaya AE, et al. (2012) Emergency peripartum hysterectomy in a tertiary hospital in Ankara, Turkey: A 5-Year Review. Arch Gynecol Obstet 286(5): 1131-1134.
- Zaman BS, Sadaf J, Bhatti SZ, Shamas N (2016) Indications and complication of emergency peripartum hysterectomy in bahawal victoria hospital Bahawalpur. p. 4.
- Tokue H, Tokue A, Tsushima Y, Kameda T (2019) Risk factors for massive bleeding based on angiographic findings in patients with placenta previa and accreta who underwent balloon occlusion of the internal iliac artery during cesarean section. Br J Radiol 92(1102): 20190127.
- Obiechina NJA, Eleje GU, Ezebialu IU, Okeke CaF, Mbamara SU, et al. (2012) Emergency Peripartum Hysterectomy in Nnewi, Nigeria: A 10-Year Review. Niger J Clin Pract 15(2): 168-171.
- Choi SJ, Song SE, Jung KL, Oh SY, Kim JH, et al. (2008) Antepartum Risk Factors Associated with Peripartum Cesarean Hysterectomy in Women with Placenta Previa. Am J Perinatol 25(1): 37-41.
- Kang H, Lee ji, Kim H, Kim BW, Moon CS, et al. (2016) Total laparoscopic hysterectomy via suture and ligation technique. Obstet Gynecol Sci 59(1): 39-44.
- Rotem R, Sela HY, Hirsch A, Samueloff A, Grisaru-Granovsky S, et al. (2020) The use of a strict protocol in the trial of labor following two previous cesarean deliveries: maternal and neonatal results. Eur J Obstet Gynecol Reprod Biol 252: 387-392.
- Kallianidis AF, Maraschini A, Danis J, Colmorn LB, Deneux-Tharaux C, et al. (2020) Epidemiological analysis of peripartum hysterectomy across nine european countries. Acta Obstet Gynecol Scand 99(10): 1364-1373.
- Colmorn LB, Krebs L, Langhoff-Roos J, NOSS study group (2016) Potentially avoidable peripartum hysterectomies in denmark: a population based clinical audit. PloS One 11(8): e0161302.
- Vandenberghe G, Guisset M, Janssens I, Leeuw VV, Roelens K, et al. (2017) A Nationwide population-based cohort study of peripartum hysterectomy and arterial embolisation in belgium: results from the belgian obstetric surveillance system. BMJ Open 7(11): e016208.
- Shrivastava V, Nageotte M, Major C, Haydon M, Wing D, et al. (2007) Case-Control comparison of cesarean hysterectomy with and without prophylactic placement of intravascular balloon catheters for placenta accreta. Am J Obstet Gynecol 197(4): 402.e1-5.
- Amarin Z (2021) Approaches to Hysterectomy.
- Camuzcuoglu H, Toy H, Vural M, Yildiz F, Aydin H, et al. (2010) Internal iliac artery ligation for severe postpartum hemorrhage and severe hemorrhage after postpartum hysterectomy. J Obstet Gynaecol Res 36(3): 538-543.
- Chung M, Loudill C, Wieler M, Farnam J, Ahn SH, et al. (2017) Endovascular retrieval of nexplanon from the distal pulmonary artery. J Vasc Interv Radiol 28(3): 466-467.
- Lin J, Lin F, Zhang Y (2019) Uterine artery ligation before placental delivery during caesarean in patients with placenta previa accreta. Medicine (Baltimore) 98(36): e16780.






























