Placental Biomarkers and Uterine Doppler Indices Predictability Capacity for Preeclampsia and its Clinical Sequalae
Naglaa Hussien1* and Mohamed Hashem El Refaey2
1Department of Obstetrics and Gynecology, Tanta University, Egypt
2Department of Diagnostic Radiology, Tanta University, Egypt
Submission: September 13, 2019;Published: October 09, 2019
*Corresponding author: Naglaa Hussien, Department of Obstetrics and Gynecology, Tanta University, Egypt
Naglaa Hussien and Mohamed Hashem El Refaey. Placental Biomarkers and Uterine Doppler Indices Predictability Capacity for Preeclampsia and its Clinical Sequalae. J Gynecol Women’s Health. 2019: 16(5): 555949. DOI: 10.19080/JGWH.2019.16.555949
Abstract
Background: Maternal angiogenic biomarkers during gestation are considered the main reflectors of the possible triggering pathophysiological scenarios for preeclampsia. preeclampsia that is still considered the disease of theories is well recognized and established to be characterized by its systemic vascular pathology that is reprinted clinically in the form of raised maternal blood pressure especially after 20 gestational weeks besides the end organ damage.
Aim: to investigate the effectiveness of biomarkers, arteriography and uterine artery Doppler in predictability of hypertensive disorders of pregnancy, small for gestational age development.
Methodology: A prospective clinical research trial in which all research study subjects were fully assessed clinically by detailed history and examination within the first gestational trimester serum samples were obtained to assay the placental growth factor, alphafetoprotein pregnancy associated plasma protein A and human chorionic gonadotrophin, full clinical follow up for maternal, neonatal clinical outcomes was assessed to determine the correlation between hypertensive disease development and adverse perinatal outcomes such as SGA and IUFD.
Result: comparative statistical analysis between healthy cases and diseased cases regarding basal laboratory data, oocytes count, sperm count, fertilization rate and outcome in which there was no statistical significant difference basal AMH, FSH, LH, E2,TSH, Oocytes count per patient, Total sperm count (x106/ml), Fertilization rate per patients, (p values=0.093, 0.088, 0.367, 0.132, 0.338, 0.252, 0.739, 0.694 consecutively) however the Rate of clinical pregnancy and cycle cancelation was statistically significantly higher among the health research group(p values= 0.001). Statistical Logistic regression analysis for association between maternal morbid disease and IVF/ICSI outcome among the studied cases in which there was statistical significance as regards clinical pregnancy and cycle cancelation (p values =0.001, 0.003, 0.001, 0.005 consecutively)
Conclusion: The current study has revealed the cornerstone role of placental angiogenic factors and beta hcg hormones besides the mean arterial pressure and uterine Doppler indices in predictability of adverse clinical events and occurrence of preeclampsia.
Introduction
The best approach in recent research efforts is to consider the early detection of obstetric clinical challenges and adverse outcomes in order to upgrade the levels of management guidelines in order to reduce maternal and neonatal morbidity and mortality issues .the implementation of serum biomarkers in early detection of preeclampsia is global research interest particularly when integrated to clinical data that could be very useful to prevent and reduce the impact of adverse clinical outcomes by early prediction of pathological development of preeclampsia [1-3].
Maternal angiogenic biomarkers during gestation are considered the main reflectors of the possible triggering pathophysiological scenarios for preeclampsia. preeclampsia that is still considered the disease of theories is well recognized and established to be characterized by its systemic vascular pathology that is reprinted clinically in the form of raised maternal blood pressure especially after 20 gestational weeks besides the end organ damage that results, early detection of blood pressure changes particularly in large vessels could raise the clinician awareness of possible disease development [4-7].
The failure of proper trophoblastic invasion could be reflected in physiological imbalance of the normal blood pressure changes during the progression of pregnancy by complex interaction between the placental and maternal vascular systems at molecular and cellular levels and the cross talk that occurs due to changes in angiogenic factors among other numerous biomarkers well recognized and demonstrated during gestation. The aorta is affected by the neural and hormonal interactions of pregnancy all the way till delivery any changes in the integrity and harmony could be mirrored in the form of blood indices changes such as that well proven in the situation of uterine artery Doppler changes that could predict in an effective manner the possible development of preeclampsia [8-10].
Aim of the Work
To investigate the effectiveness of biomarkers, arteriography and uterine artery Doppler in predictability of hypertensive disorders of pregnancy, small for gestational age development.
Methodology
A prospective clinical research trial held in department of obstetrics and complemented in department of radio-diagnosis in Tanta university hospitals in a period from May 2018 till April 2019, in which all research study subjects were fully assessed clinically by detailed history and examination within the first gestational trimester serum samples were obtained to assay the placental growth factor, alpha feto protein pregnancy associated plasma protein A and human chorionic gonadotrophin, full clinical follow up for maternal, neonatal clinical outcomes was assessed to determine the correlation between hypertensive disease development and adverse perinatal outcomes such as SGA and IUFD. Placental growth factor, alphafetoprotein pregnancy associated plasma protein A and human chorionic gonadotrophin have been assayed by using ELISA technique and samples have been stored at minus 40 degree Celsius till time of assay.
Statistical Analysis
Data were collected, revised, coded and entered to the Statistical Package for Social Science (SPSS) version 23. The qualitative data were presented as numbers and percentages and compared between groups using Chi-square test and/or Fisher exact test while quantitative data were presented as means and standard deviations and compared between groups using Independent t-test and One Way ANOVA test. Receiver operating characteristic curve (ROC) was used to assess the diagnostic accuracy of serum biomarkers and uterine artery Doppler in prediction of outcome groups. The confidence interval was set to 95%. So, the p-value was considered significant at the level of < 0.05.
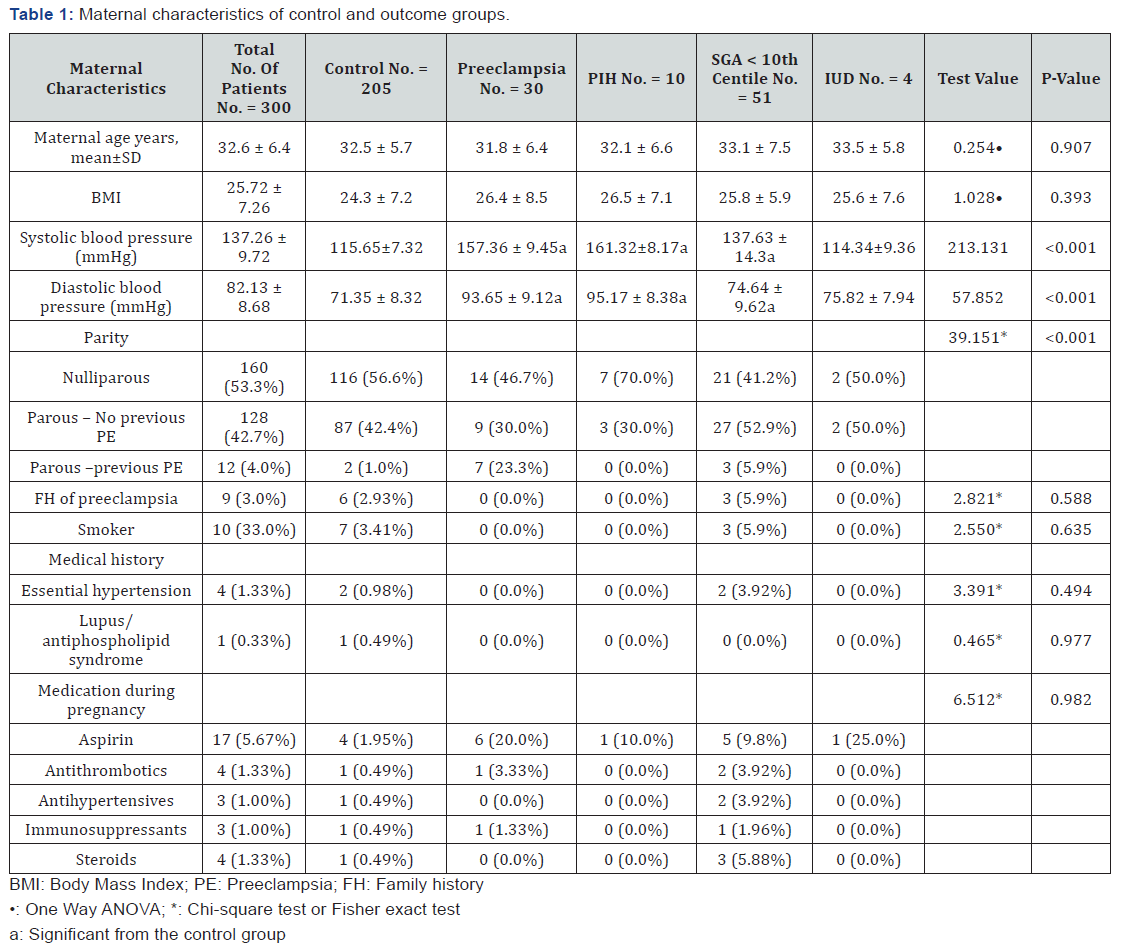
Table 1 reveals and displays the maternal characteristics among the research study cohort in which there was no statistical significant difference between the research categorial groups (total number of cases, control, preeclampsia, PIH, SGA <10th centile, IUD) as regards Maternal age years, mean±SD, BMI, FH of preeclampsia, Smoker, Medical history (Essential hypertension, Lupus/antiphospholipid syndrome) Medication during pregnancy (p values=0.907, 0.393, 0.588, 0.635, 0.494, 0.977, 0.982 consecutively), however there was statically significant difference as regards Systolic blood pressure (mmHg), Diastolic blood pressure (mmHg), Parity (p values <0.001).
Table 2 reveals and displays the statistical comparative analysis of the research categorial groups as regards the serum biomarkers, MAP and uterine artery Doppler indices in which there was statistical significance of MAP among the preeclampsia, PIH(p values < 0.001), Mean PI among the preeclampsia research group (p value <0.001), AFP (ng/ml) among preeclampsia and intrauterine death research groups (p values < 0.001), β-hCG (mIU/ ml) among Preeclampsia, PIH, SGA < 10th centile(p values <0.001), PAPP-A (ng/ml) among Preeclampsia, PIH, SGA < 10th centile(p values <0.001,0.031,<0.001 consecutively), PLGF (pg/ mL) among Preeclampsia, PIH, SGA<10th centile, intrauterine death (p values =0.004, 0.010, <0.001, 0.015 consecutively ).
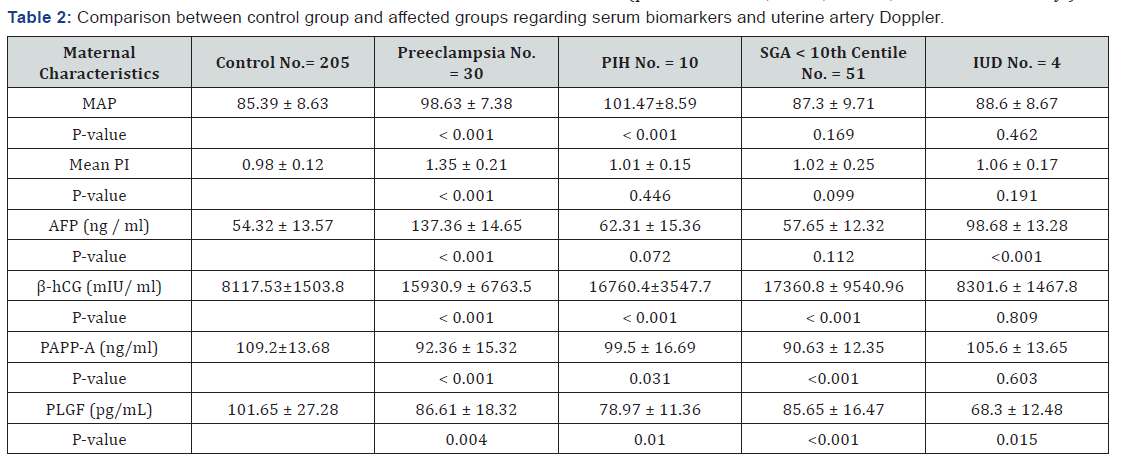
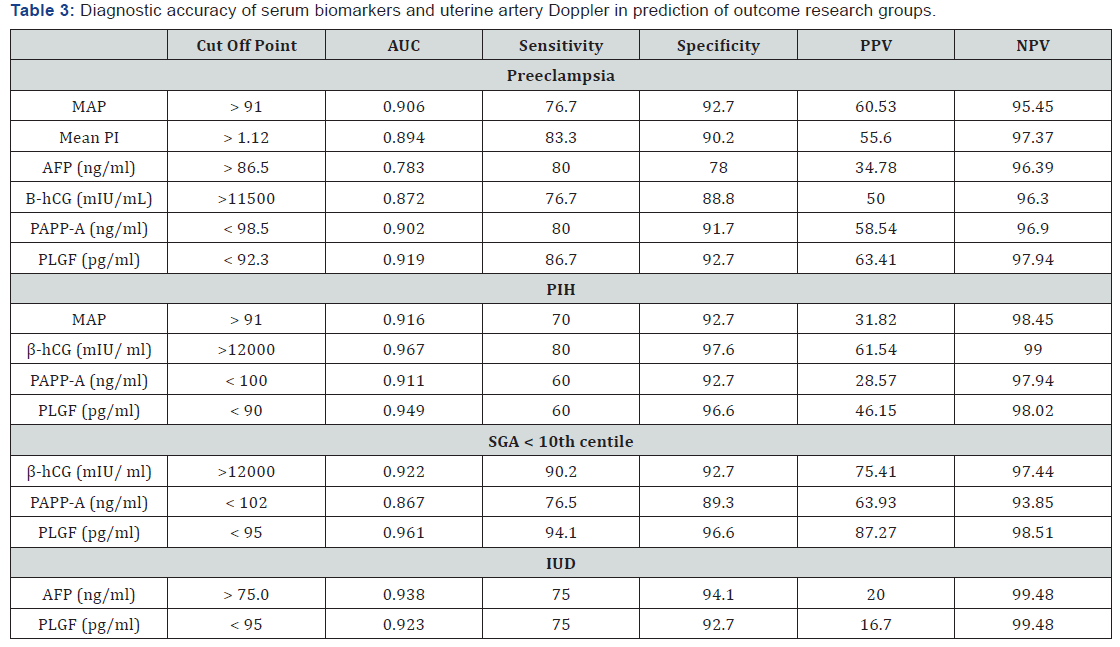
Table 3 reveals and displays the Diagnostic accuracy of serum biomarkers, MAP and uterine artery Doppler in predictability of outcome research groups as regards Preeclampsia, MAP, Mean PI, AFP (ng/ml), Β-hCG (mIU/mL), PAPP-A (ng/ml), PLGF (pg/ml) at cutoff points > 91,>1.12,>86.5,>11500,<98.5,< 92.3 consecutively had AUC(0.906,0.894,0.783,0.872,0.902,0.919consecutively) Sensitivity(76.7% ,83.3%,80.0% ,76.7% ,80.0%,86.7% consecutively)Specificity (92.7% ,90.2%% ,78.0 %,88.8% ,91.7% ,92.7% consecutively)PPV(60.53 ,55.6 ,34.78 ,50.0 ,58.54 ,63.41)NPV (95.45 ,97.37 ,96.39 ,96.3 ,96.9 ,97.94 consecutively ).concerning PIH, MAP,β-hCG (mIU/ ml),PAPP-A (ng/ml),, PLGF(pg/ml)) at cutoff points >91,>12000,<100,<90 consecutively AUC=0.916,0.967,0.911,0.949 consecutively, sensitivity=70.0, 80.0, 60.0 60.0 consecutively, specificity= PPV(31.82, 61.54, 28.57, 46.15 consecutively) NPV (98.45, 99.0, 97.94, 98.02 consecutively).
Discussion
A similar prior research study to the current study in approach and methodology have investigated the role of first trimetric placental growth factor, alpha feto protein, pregnancy associated plasma protein A and human chorionic gonadotrophin in predictability of preeclampsia besides usage of uterine Doppler indices have revealed that the integration of those biomarkers and sonographic indices of uterine artery have a cornerstone role in raising the predictability power for occurrence of preeclampsia that could be justified by the fact that poor placentation process in preeclampsia could disrupt the balance of hormones and angiogenic factors produced by the placenta besides the uterine artery indices and blood pressure measurement determined by the mean arterial pressure .uterine artery abnormal indices was revealed and displayed by various prior research efforts to be a reflector of possible abnormal trophoblastic invasion process that is the main mechanism triggering the development of preeclampsia [11-13].
The free beta subunit of human chorionic gonadotrophin is secreted by the syncytiotrophoblastic tissue. Its main physiological function is to sustain the decidual spiral arteries and the vascular supply of the placenta during gestation .In normal gestations, the concentration levels of free beta hCG rises exponentially till 8 to 10 gestational weeks, falling afterward. In the gestational second-trimester, free beta hcg have been mentioned to be raised in females who later develop preeclampsia those research findings are in harmony with the current study results denoting that beta hch could be implemented as a biomarker for predictability of preeclampsia. Furthermore prior research studies that have retrospectively assessed have revealed and displayed that the free beta hCG have no for hypertensive disorders of gestation that contradicts with the current study findings however that could be due to lowered sensitivity and specificity of the biomarker when used alone since when integrated with other angiogenic biomarkers could raise the effectiveness of preeclampsia detection [14,15].
A disproportion between pro- and antiangiogenic factors before and after the onset of preeclampsia is suggested to play a crucial role in its pathophysiological development. It is thought that the poorly implanted placenta becomes ischemic and subsequently secretes antiangiogenic factors such as sFlt- 1 (soluble Fms-like Tyrosine Kinase-1) also known as soluble vascular endothelial growth factor receptor-1 and sEng (soluble endoglin) into the maternal circulation which later antagonize a number of proangiogenic factors, e,g placenta growth factor and vascular endothelial growth factor. Prior research studies in a manner similar to the current study in approach and methodology have revealed that a combination of serum bio makers, uterine artery Doppler indices, and maternal features could aid in identification of high-risk cases that are liable to develop preeclamptic toxemia [1,3,7,11].
Conclusions and Recommendations for Future Research
The current study have revealed the cornerstone role of placental angiogenic factors and beta hcg hormones besides the mean arterial pressure and uterine Doppler indices in predictability of adverse clinical events and occurrence of preeclampsia ,however future research efforts are recommended to consider racial and ethnic differences that could affect the results, besides larger multicentric fashioned research studies are recommended in an effort to raise the ability to implement the usage of biomarkers in predictability of preeclampsia occurrence and its unfavorable outcomes.
s
References
- Cantwell R, Clutton-Brock T, Cooper G, Dawson A, Drife J, et al. (2011) Saving Mothers’ Lives: Reviewing maternal deaths to make motherhood safer: 2006-2008. The Eighth Report of the Confidential Enquiries into Maternal Deaths in the United BJOG 118 (Suppl): 1-203.
- Rolnik DL, Wright D, Poon LC, O’Gorman N, Syngelaki A, et al. (2017) Aspirin versus Placebo in Pregnancies at High Risk for Preterm N Engl J Med 377(7): 613-622.
- Verghese L, Alam S, Beski S, Thuraisingham R, Barnes I, et al. (2012) Antenatal screening for pre-eclampsia: evaluation of the NICE and pre-eclampsia community guidelines. J Obstet Gynaecol 32(2): 128-131.
- O’Gorman N, Wright D, Poon LC, Rolnik DL, Syngelaki A, et al. (2017) Multicenter screening for pre-eclampsia by maternal factors and biomarkers at 11-13 weeks’ gestation: comparison with NICE guidelines and ACOG recommendations. Ultrasound Obstet Gynecol 49(6): 756-760.
- Kleinrouweler CE, Cheong-See F, Collins G, Kwee A, Thangaratinam S, et al. (2016) Prognostic models in obstetrics: available, but far from applicable. Am J Obstet Gynecol 214(1): 79-90.
- Hayden JA, Windt VDA, Cartwright JL, Cote P, Bombardier C, et al. (2013) Assessing bias in studies of prognostic factors. Ann Intern Med 158(4): 280-286.
- Abou-nassar K, Carrier M, Ramsay T, Rodger MA (2011) The association between antiphospholipid antibodies and placenta mediated complications: A systematic review and meta-analysis. Thromb Res 128(1): 77-85.
- Adams JW, Watts DH, Phelps BR (2016) A systematic review of the effect of HIV infection and antiretroviral therapy on the risk of pre-eclampsia. Int J Gynecol Obstet 133(1): 17-21.
- Basaran A, Basaran M, Topatan B, Martin JN (2016) Effect of chorionic villu sampling on the occurrence of preeclampsia and gestational hypertension: An updated systematic review and meta-analysis. J Turk Ger Gynecol Assoc 17(2): 65-72.
- Wolf HT, Owe KM, Juhl M, Hegaard HK (2014) Leisure time physical activity and the risk of pre-eclampsia: a systematic review. Matern Child Health J 18(4): 899-910.
- Wotherspoon AC, Young IS, McCance DR, Holmes VA (2016) Evaluation of biomarkers for the prediction of pre-eclampsia in women with type 1 diabetes mellitus: A systematic review. J Diabetes Complications 30(5): 958-966.
- Wu P, Berg VDC, Alfirevic Z, Obrien S, Othlisberger RM, et al. (2015) Early pregnancy biomarkers in pre-eclampsia: A systematic review and meta-analysis. Int J Mol Sci 16(9): 23035-23056.
- Wu X, Yang K, Tang X, Sa Y, Zhou R, et al. (2015) Folate metabolism gene polymorphisms MTHFR C677T and A1298C and risk for preeclampsia: a meta-analysis. J Assist Reprod Genet 32(5): 797-805.
- Xia X, Chang W, Cao Y (2012) Meta-analysis of the methylenetetrahydrofolate reductase C677T polymorphism and susceptibility to pre-eclampsia. Hypertens Res 35(12): 1129-1134.
- Xu Y, Ren L, Zhai S, Luo X, Hong T, et al. (2016) Association Between Isolated Single Umbilical Artery and Perinatal Outcomes: A Meta-Analysis. Med Sci Monit 22(): 1451-1459.






























