Different Etiological Aspects of Diminished Ovarian Reserve Impact on Clinical Outcomes of ICSI Cycles
Ahmed Hagras1*, Maha Mahmoud Hagras2 and Mohamed Elzayat3
1Department of Obstetrics and Gynecology, Tanta University, Egypt
2Department of Clinical Pathology, Tanta University, Egypt
3genetic engineering and biotechnology, Head of royal fertility center, Egypt
Submission: September 13, 2019;Published: October 03, 2019
*Corresponding author: OAAMJ Timmermans, Professorship Healthy Region, HZ University of Applied Sciences, Netherlands
Ahmed Hagras, Maha Mahmoud Hagras, Mohamed Elzayat. Different Etiological Aspects of Diminished Ovarian Reserve Impact on Clinical Outcomes of ICSI Cycles. J Gynecol Women’s Health. 2019: 16(5): 555947. DOI: 10.19080/JGWH.2019.16.555947
Abstract
Background: Reduced ovarian reserve have been featured from prior research efforts to cause unfavorable fertility clinical outcomes. The pathophysiological origin and etiologic aspects causing decreased ovarian reserve to reveal a broad spectrum of causes from idiopathic, prior ovarian surgery to chemotherapy.
Aim: Is to compare the rates of clinical pregnancy in intracytoplasmic sperm injection-embryo transfer management cycles in different clinical scenarios of diminished ovarian reserve etiologies.
Methodology: A retrospective clinical research trial conducted on 500 consecutive cases having diminished ovarian reserve scheduled for their first ICSI-ET cycles, Cases have been categorized in three research categorial groups: research group A, idiopathic diminished ovarian reserve (age <35 years and no clinical history of ovarian surgery or chemotherapy); research Group B, cases above 35 years old without any surgical history; and research Group C, cases having diminished ovarian reserve after ovarian surgery for endometrioma.
Result: Multivariate statistical logistic regression analysis for factors affecting clinical pregnancy among DOR patients in which there was statistical significance as regards age, number of oocytes retrieved, transferred embryos (p values <0.001, 0.032, 0.041 consecutively).
Conclusion: Responsiveness to ovarian stimulation, rates of clinical pregnancy, and live birth rates didn’t differ in a statistically significant fashion in cases of diminished ovarian reserve with various etiological factors, young aged cases having diminished ovarian reserve with could benefit from ART management.
Keywords: Fertility clinical outcomes; Intracytoplasmic sperm; Idiopathic; Surgery; ICSI-ET cycles; Endometrioma; Logistic regression; Pregnancy; Fertility
Introduction
Fertility management protocols are almost always tailored according to the ovarian reserve of the case after assessment of the full fertility aspect of both couple’s quality of oocytes and ovarian responsiveness are affected by the ovarian reserve and fertility capacity [1,2]. Diminished ovarian reserve is a major clinical challenge to all reproductive physicians all over the globe. The complexity of the ovarian histological and physiological ovarian systems makes reduced ovarian reserve a great issue of concern that requires tailored induction protocols since the ovarian responsiveness is not the only concern, but the quality of oocytes retrieved could affect the gestational outcomes [3,4].
The pathophysiological origin and etiologic aspects causing decreased ovarian reserve to reveal a broad spectrum of causes from idiopathic, prior ovarian surgery to chemotherapy [5]. Reduced ovarian reserve have been featured from prior research efforts to cause unfavorable fertility clinical outcomes with high rates of cancellation of IVF-ET cycles, and a considerable reduction in rates of pregnancy [6]. The three chief causes of poor ovarian responsiveness revealed and displayed by different research groups of investigators is advanced maternal age (above 40 years) a prior poor ovarian responsiveness incident, a reduced ovarian reserve test parameter or indices e.g. AMH and antral follicle count [7,8].
Aim of the Work
Is to compare the rates of clinical pregnancy in intracytoplasmic sperm injection-embryo transfer management cycles in different clinical scenarios of diminished ovarian reserve etiologies.
Methodology
A retrospective clinical research trial was held in Tanta University teaching hospital at the assisted reproductive technology unit of obstetrics and gynecology department in the period from august 2017 till August 2019, conducted on 500 consecutive cases having diminished ovarian reserve scheduled for their first ICSI-ET cycles, exclusive research criteria involved criteria were undergoing a fertility preservation cycle or a frozenthawing embryo transfer cycle. Cases have been categorized in three research categorial groups: research group A, idiopathic diminished ovarian reserve (age <35 years and no clinical history of ovarian surgery or chemotherapy); research Group B, cases above 35 years old without any surgical history; and research Group C, cases having diminished ovarian reserve after ovarian surgery for endometrioma.
Cases have undergone controlled ovarian stimulation using conventional protocols antagonist protocol, the GnRH agonist long protocol, or GnRH agonist. The following agents were used involving recombinant FSH with or without human menopausal gonadotropin at dosages ranging from 150 IU/day to 450 IU/ day according to the BMI, age, and antral follicular number. research study subjects have been monitored every 2–4 days using transvaginal sonographic examination beginning on day 5 of the ovarian hyperstimulation, dosage of gonadotropin have been tailored according to the ovarian responsiveness. When at least 3 follicles reached a mean diameter of ≥18 mm, 10,000 IU human chorionic gonadotropin have been administered for trigger. The oocytes have been about 34 to 36 h after the hCG injection by transvaginal approach under sonographic guidance. The oocytes have been inseminated by using intracytoplasmic sperm injection. The embryos have transferred 3 or 5 days after the oocyte retrieval. All cases were administered luteal phase support beginning on the day of oocyte retrieval vaginal progesterone. Luteal support has been continued until the pregnancy test was conducted One positive hCG result have been accepted as a biochemical pregnancy. Visualization of the embryonic heartbeat by trans vaginal sonogram was defined as a clinical pregnancy.
Statistical Analysis
Data were collected, revised, coded and entered to the Statistical Package for Social Science (IBM SPSS) version 23. The quantitative data were presented as mean and standard deviations when parametric and median with inter-quartile range (IQR) when non parametric while qualitative variables were presented as number and percentages. The comparison between groups regarding qualitative data was done by using Chi-square test and/or Fisher exact test when the expected count in any cell found less than 5. The comparison between two independent groups with quantitative data and parametric distribution was done by using Independent t-test and more than two groups were done by One Way ANOVA followed by post hoc analysis using LSD test when significant while with nonparametric distribution was done by using Mann-Whitney test between two groups and Kruskall-Wallis test between more than two groups. Logistic regression analysis was used in the form of univariate and multivariate to assess the predictors of outcome of patients with DOR. The confidence interval was set to 95% and the margin of error accepted was set to 5%. So, the p-value was considered significant at the level of < 0.05.
Result
Table 1 reveals and displays the Demographic and clinical characteristics of patients with diminished ovarian reserve (idiopathic ,age related diminished ovarian reserve, previous ovarian surgery research groups) in which there was statistical significance as regards age (p value<0.001), whereas there was no statistical significant difference as regards BMI (kg/m2), mean±SD, Duration of infertility (months), AMH (ng/mL), FSH (IU/L), Estradiol (pg/mL), Antral follicle count, Stimulation days, Total FSH dose (IU) Peak estradiol (pg/mL), Endometrial thickness on hCG day (mm), Reached Oocyte retrieval stage, Number of oocyte retrieved, mature oocytes, top quality embryo, embryo transfer ,number of embryos transferred, Implantation rate, Clinical pregnancy n (%)ET cancelled n (%) (p values =0.337 , 0.986, 0.413, 0.830, 0.940, 0.969, 0.137, 0.850, 0.310, 0.087, 0.861, 0.306, 0.211, 0.651, 0.721, 0.150, 0.979, 0.556, 0.216 consecutively).
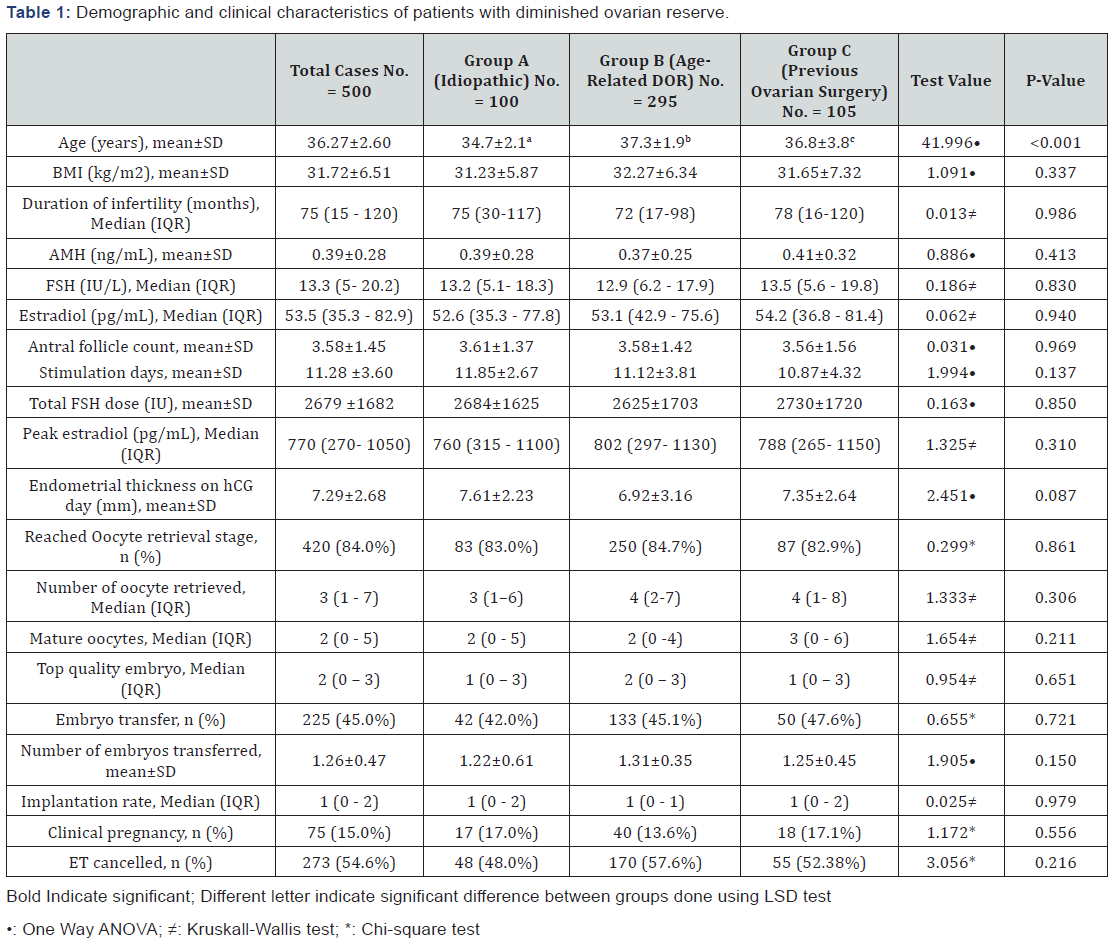
AMH: Anti-Mullerian hormone; FSH: follicle-stimulating hormone; hCG: human chorionic gonadotropin: ET: embryo transfer; SD: Standard deviations; IQR: Inter-quartile range
Table 2 reveals and displays the Demographic and clinical characteristics affecting embryo transfer rate among DOR patients(Patients with embryo transfer versus Patients without embryo transfer research groups ) in which there was no statistical significant difference as regards the Age (years), BMI (kg/m2), Duration of infertility (months), AMH (ng/mL), FSH (IU/L), Estradiol (pg/mL), Antral follicle count, Stimulation days, Total FSH dose (IU)(p values= 0.145, 0.306, 0.512, 0.691, 0.730, 0.543, 0.219, 0.424, 0.452 consecutively), however there was statistical significant difference as regards Peak estradiol (pg/mL), Endometrial thickness on hCG day (mm), Number of follicles > 17 on hCG day (p values =0.009, 0.017, 0.002 consecutively).
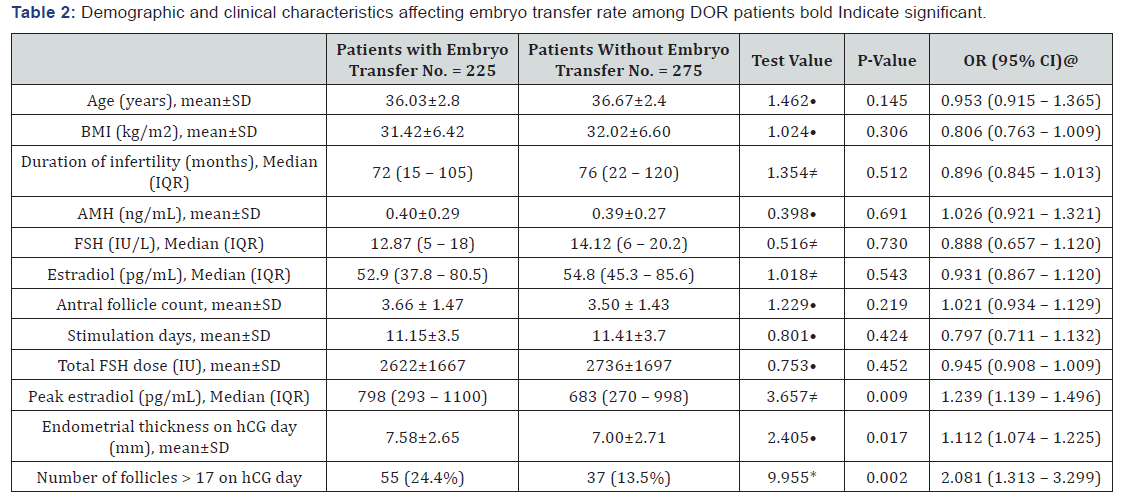
AMH: Anti-Mullerian hormone; FSH: follicle-stimulating hormone; hCG: human chorionic gonadotropin: SD: Standard deviations; IQR: Inter-quartile range; OR (95% CI): Odds ratio with 95% Confidence interval
@: Uni-variate logistic regression analysis
Table 3 reveals and displays the Demographic and clinical characteristics affecting clinical pregnancy rate among DOR patients (Patients with embryo transfer versus Patients without embryo transfer research groups) in which there was statistical significant difference as regards Age (years), FSH (IU/L), Antral follicle count , Number of oocyte retrieved, Number of transferred embryos (p values =0.002, 0.007, <0.001, <0.001, 0.021 consecutively) whereas there was no statistical significant difference as regards BMI (kg/m2), Duration of infertility (months), AMH (ng/mL), Estradiol (pg/mL), Stimulation days, Total FSH dose (IU), Peak estradiol (pg/mL), Endometrial thickness on hCG day (mm), Number of follicles > 17 on hCG day(p values =0.288,0.883, 0.683, 0.412, 0.898,0.865, 0.405 , 0.813, 0.174 consecutively).
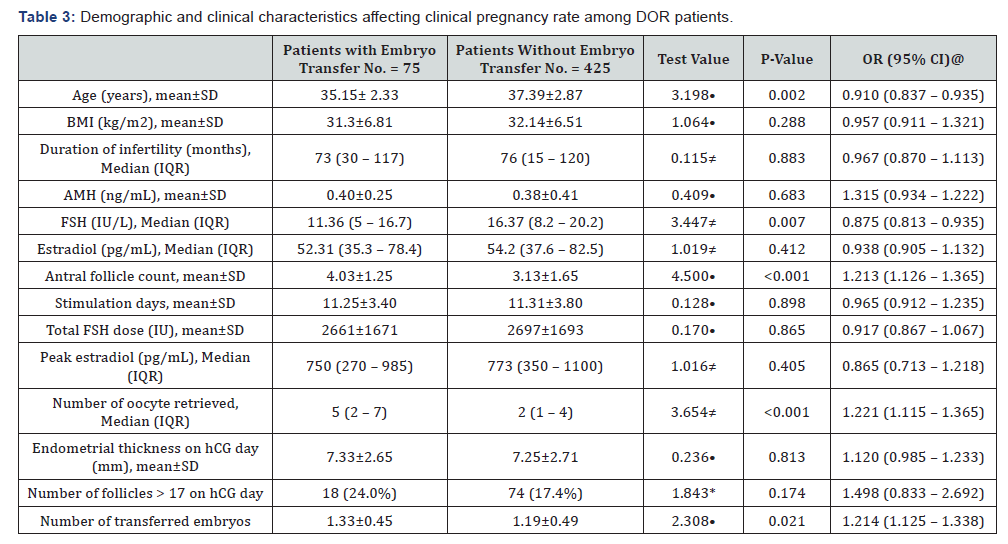
Table 4 reveals and displays the Multivariate statistical logistic regression analysis for factors affecting clinical pregnancy among DOR patients in which there was statistical significance as regards age ,number of oocyte retrieved, transferred embryos (p values <0.001, 0.032, 0.041 consecutively).
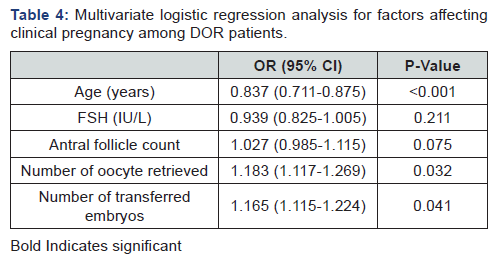
FSH: follicle-stimulating hormone; OR (95% CI): Odds ratio with 95% Confidence interval.
Discussion
Highly complex paracrine and autocrine pathways within the oocyte-cumulus complex are responsible the structural and functional integrity of the pre-ovulatory follicle prior research studies displayed that the disruption of those delicate and complex pathways are present in cases having low ovarian reserve and ageing oocytes issues [9,10]. Decreased ovarian reserve, is great clinical challenge in reproductive medicine everyday practice of assisted reproduction. Cases suffering from reduced ovarian reserve however different etiologies could have various impact and influences on the IVF/ ICSI clinical outcomes [11-13].
A prior research effort conducted with the aim of investigating factors influencing vitro fertilization clinical outcomes in cases with reduced ovarian reserve. Investigators Defined the diminished ovarian reserve as anti-Müllerian hormone serum level of <1.1ng/dL or serum follicle-stimulating hormone level of ≥20 mIU/mL. Among their research data analysis, they have shown that the Rate of clinical pregnancy have been 11.5% per management cycle, and rate of cancellation have been 34.4%. Clinical pregnancy rate has been statistically significantly correlated to the antral follicle count and the etiology of diminished ovarian reserve. Furthermore, they have revealed that the previous history of ovarian surgery was considered a statistically significant factor affecting the rates of clinical pregnancy. The research team of investigators concluded that the reduced ovarian reserve caused by Prior ovarian surgery could have better pregnancy clinical outcomes, whereas that triggered by chemotherapy could statistically significantly raise the rate of cycle cancellation. Additionally, cases having reduced ovarian reserve issues with history of gonadotoxic agent’s administration could have reduced effectiveness and raised clinical risk of IVF management cycle cancellation [1,3,9].
A prior research meta-analysis revealed the privilege of using growth hormone as an adjunct agent in diminished ovarian reserve cases with decreased ovarian stimulation duration needed before oocyte retrieval, with a larger oocytes number collected, and enhancements in various clinical outcomes with the usage of growth hormone agent [2,5,7].
A prior research study like the current research in approach and methodology have revealed that young cases having diminished ovarian reserve issues could have a higher clinical probability of clinical pregnancy achievement than those with other etiologies. Furthermore in a similar manner to the current research study results they have shown that the serum FSH concentration levels in young aged diminished ovarian reserve cases was relatively lower than in other research groups and they had higher rates of implantation and pregnancy in comparison and contrast to other research groups those results verify the current research study results in those aspects an interesting fact was observed at molecular and cellular levels of research that justifies most of the current research study findings that ovarian biological aging could occur independent of chronological age [8,11].
A prior research team of investigators have compared in analytical manner the IVF live birth rates in cases having diminished ovarian reserve issues after performance of ovarian cystectomy for endometrioma with cases having idiopathic issues of diminished ovarian reserve revealing a statistically significantly higher rate of fertilization rate and mean number of embryos but a reduced rates of clinical pregnancy in cases that had an endometrioma excision operative procedure [10,12,13].
Conclusions and Recommendations for Future Research
Responsiveness to ovarian stimulation, rates of clinical pregnancy, and live birth rates didn’t differ in a statistically significant fashion in cases of diminished ovarian reserve with various etiological factors, young aged cases having diminished ovarian reserve with could benefit from ART management, however the current research study results should be verified in future research efforts in a multicentric fashion taking in consideration racial and ethnic differences that could affect the ovarian responsiveness and reserve due to variability in genetic makeup.
References
- Cohen J, Chabbert-Buffet N, Darai E (2015) Diminished ovarian reserve, premature ovarian failure, poor ovarian responder-a plea for universal definitions. J Assist Reprod Genet 32(12): 1709-1712.
- Regan SLP, Knight PG, Yovich JL, Arfuso F, Dharmarajan A, et al. (2018) Growth hormone during invitro fertilization in older women modulates the density of receptors in granulosa cells, with improved pregnancy outcomes. Fertil Steril 110(7): 1298-1310.
- Humaidan P, Alviggi C, Fischer R, Esteves SC (2016) The novel POSEIDON stratification of ‘Low prognosis patients in Assisted Reproductive Technology’ and its proposed marker of successful outcome. F1000Research 5: 2911.
- Yun BH, Kim G, Park SH, Noe EB, Seo SK et al. (2017) Invitro fertilization outcome in women with diminished ovarian reserve. Obstet Gynecol Sci 60(1): 46-52.
- Roustan A, Perrin J, Debals-Gonthier M, Paulmyer-Lacroix O, Agostini A, et al. (2015) Surgical diminished ovarian reserve after endometrioma cystectomy versus idiopathic DOR: comparison of invitro fertilization outcome. Hum Reprod 30(4): 840-847.
- Güvenir HA, Misirli G, Dilbaz S, Ozdegirmenci O, Demir B, et al. (2015) Estimating the chance of success in IVF treatment using a ranking algorithm. Med Biol Eng Comput 53(9): 911-920.
- Norman R, Alvino H, Hart R, Rumbauts L (2016) LIGHT Study Investigators. A randomised double blind placebo controlled study of recombinant human growth hormone (h-GH) on live birth rates in women who are poor responders. Hum Reprod 31(Suppl. 1): i37.
- Papathanasiou A, Searle BJ, King NM, Bhattacharya S (2016) Trends in ‘poor responder’ research: lessons learned from RCTs in assisted conception. Hum Reprod Update 22(3): 306-319.
- Polyzos NP, Sunkara SK (2015) Sub-optimal responders following controlled ovarian stimulation: an overlooked group? Hum Reprod 30(9): 2005-2008.
- Bassiouny YA, Dakhly DM, Bayoumi YA, Hashish NM (2016) Does the addition of growth hormone to the invitro fertilization/intracytoplasmic sperm injection antagonist protocol improve outcomes in poor responders? A randomized, controlled trial. Fertil Steril 105(3): 697-702.
- Mutlu MF, Erdem M, Erdem A, Yıldız S, Mutlu I, et al. (2013) Antral follicle count determines poor ovarian response better than anti-Mullerian hormone, but age is the only predictor for live birth in invitro fertilization cycles. J Assist Reprod Genet 30(5): 657-665.
- Nelson SM, Telfer EE, Anderson RA (2013) The ageing ovary and uterus: new biological insights. Hum Reprod Update 19(1): 67-83.
- Guler I, Erdem A, Oguz Y, Cevher F, Mutlu MF, et al. (2017) The impact of laparoscopic surgery of peritoneal endometriosis and endometrioma on the outcome of ICSI cycles. Syst Biol Reprod Med 63(5): 324-330.






























