Traumatic Dreams in a Women’s Prison Setting: Probable Under-Treatment
Burr S Eichelman1* and Anne Dorava2
1Wisconsin Department of Corrections and Emeritus Professor of Psychiatry, University of Wisconsin-Madison, USA
2Wisconsin Department of Corrections Psychiatric Nurse, Taycheedah Correctional Institution, USA
Submission: July 23, 2019;Published:August 22, 2019
*Corresponding author: Burr S Eichelman, Wisconsin Department of Corrections, University of Wisconsin-Madison, USA
How to cite this article:Burr S Eichelman, Anne Dorava. Traumatic Dreams in a Women’s Prison Setting: Probable Under-Treatment. J Gynecol Women’s 002 Health. 2019: 16(1): 555932. DOI: 10.19080/JGWH.2019.16.555932
Abstract
Post-traumatic stress disorder (PTSD) is a diagnosis of high frequency for incarcerated women. Recurrent traumatic dreams are one symptom of this disorder; such dreams may be present in individuals who do not fully meet the diagnostic criteria for full-blown PTSD. Despite substantial efficacy of prazosin in reducing the frequency and intensity of traumatic dreams, this medication appears to be under-utilized as evidenced within is the facility of investigation - a large women’s state correctional institution’s population where a high frequency of traumatic dreams has been reported.
Keywords:PTSD; Traumatic dreams; Women; Prisoners; Prazosin; Trauma dream treatment
Introduction
Post-traumatic stress disorder is diagnosed in the Diagnostic and Statistical Manual of Mental Disorder, Fifth Edition (DSM 5) [1] as a consequence of exposure to trauma one or more of the following elements: recurrent, involuntary, and intrusive distressing memories of the traumatic event (s); recurrent distressing dreams in which the content and/or affect of the dream are related to the traumatic event (s); dissociative reactions; intense or prolonged psychological distress at exposure to internal or external cues that symbolize or resemble an aspect of the traumatic event (s); marked physiological reactions to internal or external cues that symbolize or resemble an aspect of the traumatic event (s). Forensic clinicians are aware of the high incidence of PTSD as a full disorder, but also PTSD symptoms, within prison populations, particularly female prison inmates. Cook et al. [2] reported 99% of female inmate respondents reporting some form of abuse prior to incarceration. Earlier studies [3,4] have also reported significant victimization. PTSD in female prisoners has been reported at an incidence of 48% current with incarceration and plus an additional 20% prior to incarceration [5]. In an Illinois prison sample of 163 inmates (non-segregation inmates), 40% were experiencing repeated, disturbing dreams of a stressful experience and 38% were having difficulty falling or staying asleep. Sixty per cent (60%) were thought to be diagnosed with PTSD [6].
Coupled to this high prison incidence of PTSD and concomitant symptoms is the question of whether PTSD is recognized by clinicians within the prison setting and whether its symptom elements are being treated. This is particularly critical given the efficacy of prazosin in the treatment of one symptom of PTSD, namely recurrent traumatic dreams. Traumatic dreams are defined as frightening dreams which include “videotape” replaying of elements of precise trauma which an individual has experienced. These are very unique, although widespread, dreams. They are not general nightmares or night terrors. Traumatic dreams have been argued as contributing factors to alcoholism and substance abuse, as well as suicidal ideation and completed suicides [7].
Prazosin is an alpha1 adrenergic receptor antagonist. It is exceptionally effective in suppressing recurrent traumatic dreams. In three open-label trials 94.4% (17 of 18 patients) experienced a 50% reduction in the occurrences of their nightmares [8-10]. In an open comparison between prazosin and quetiapine 61.3% of patients acutely experienced efficacy in traumatic dream suppression and 48.4% had prolonged effectiveness [11].
Based upon the above information, this study was designed from a quality assurance perspective to ask the following questions:
a) what is the incidence of traumatic dreams within a female prison setting?
b) Is traumatic dreaming being detected by the prison psychologists and psychiatrists?
c) Are the traumatic dreams being treated by the prison psychiatric prescribers?
Materials and Methods
The population for study was the full inmate population of Taycheedah Correctional Institution (TCI), namely the State of Wisconsin’s female correctional facility for maximum and medium security inmates. This prison’s total inmate population was surveyed using all inmates incarcerated at TCI on January 26, 2015. The survey and the method of survey were approved by the Department of Corrections’ Institutional Review Board even though this was designed with the primary purpose of quality improvement of mental health care. On the day of the sample, there were 791 inmates. Inmates all received a questionnaire approved by the Department of Corrections IRB. This questionnaire queried the inmates about the frequency and character of trauma and the presence or absence of traumatic dreams, asking about their frequency and their intensity. The questions asked were abstracted from The Clinician- Administered PTSD Scale (CAPS) [12] which has been used to research PTSD within other populations [13,14]. Inmates identified as having traumatic dreams were asked whether they were interested in pharmacologic and/or non-pharmacologic treatment for their dreams. A follow-up questionnaire was sent 22 weeks later to the non-responders [15].
Result
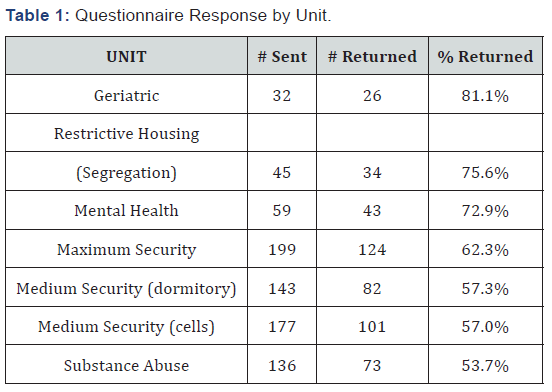
In the first mailing, 791 questionnaires were sent (1/26/15). Three hundred twenty-one were returned with a response rate of 40.6%. A second mailing was sent (6/30/15) to the nonresponders still remaining at TCI (317 of the 470 non-responders). For this population, 162 questionnaires were returned. This provided a response rate of 61.1% of the total initial population or 75.7% of the total “available” sample population. Response rates (calculated with the initial denominator of 791) varied from 75.6% for the restrictive housing unit to 53.7% for the unit housing substance abuse special programs. The MMHU (the mental health residential unit) responded at 72.9% (Table 1).
Characteristics and Frequency of Trauma
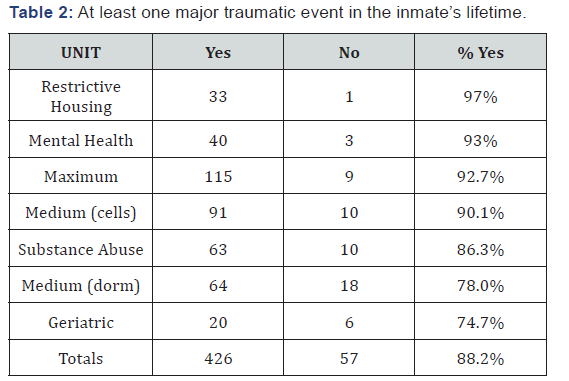
Inmates were asked if they had experienced at least one major traumatic event in their lifetime, defined as witnessing something violent such as a shooting, a beating, a traffic accident with injuries, or experiencing such things including sexual or physical abuse or rape. The response percentage for the responding population was 88.2%. From those who responded (426 out of 483 questionnaires returned) the highest affirmative response was received from the restricted housing unit (segregation) were the affirmative response was 97% (Table 2).
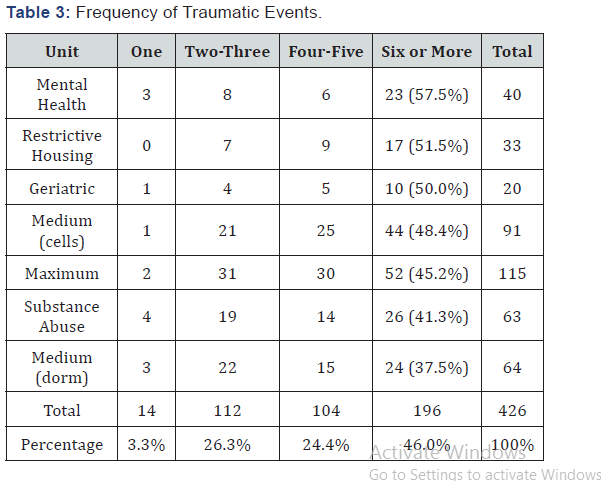
When inmates answered in the affirmative about experiencing a traumatic event, they were then asked about the frequency of traumatic events experienced in their lifetime to date. Forty-six percent of the respondents reported having experienced six or more such events. Only 3% reported only one such traumatic event (Table 3).
As one focus of this study was to ascertain the frequency of traumatic dreaming in this population, the inmates were asked about experiencing recurring dreams about one or more of their traumatic events. Eighty-nine percent of those answering this question responded affirmatively that they had experienced such recurring dreams. When asked whether they were experiencing such traumatic dreams now, at the time of the survey, 74% of those answering this question responded in the affirmative (Tables 4&5).
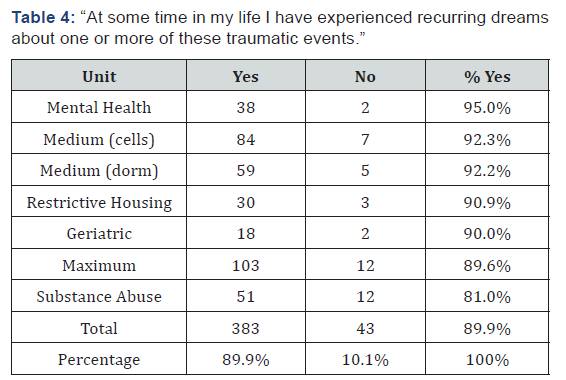
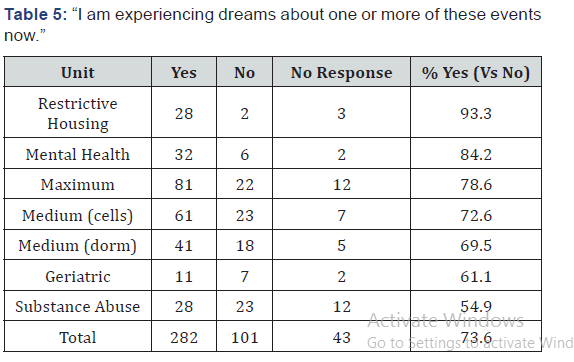
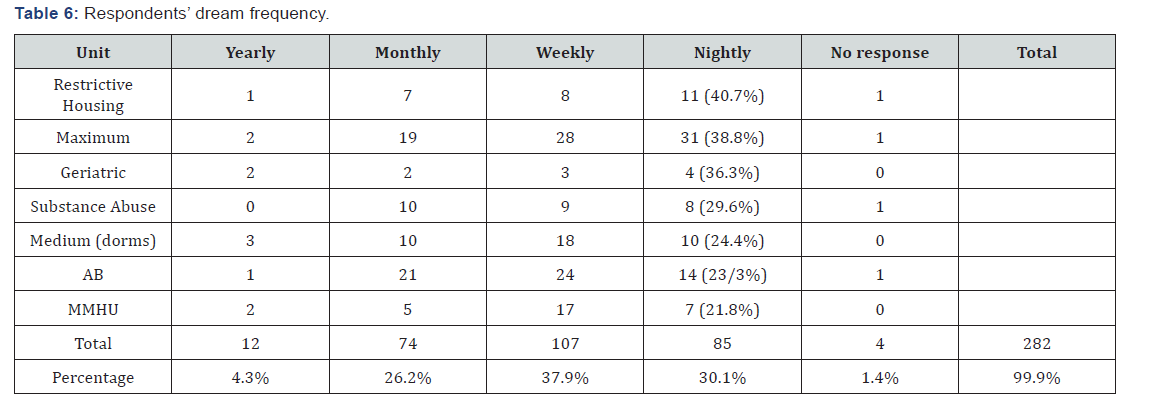
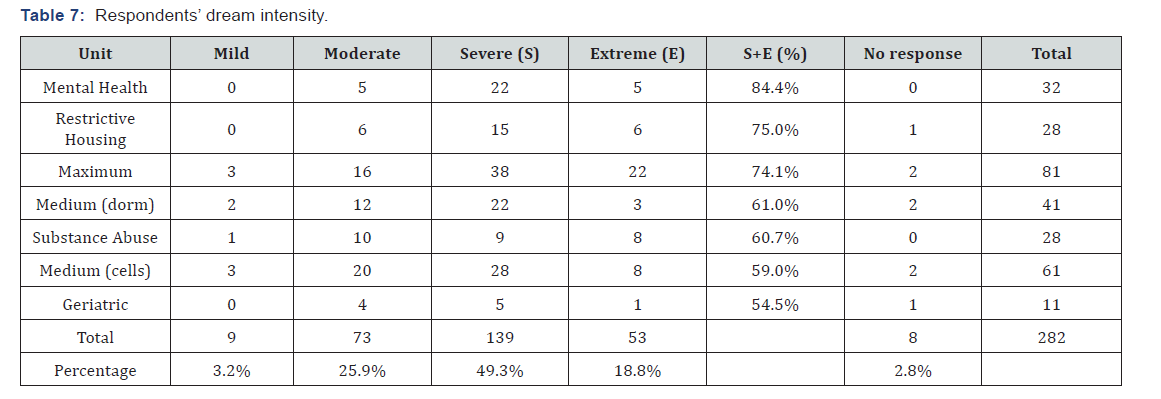
“At some time in my life I have experienced recurring dreams about one or more of these traumatic of the 282 respondents who reported experiencing dreams at the time of the survey, 85(30%) reported experiencing them nightly and 107(38%) reported experiencing them weekly. Fifty-three (19%) reported these as extreme. One hundred thirty-nine (49%) reported these dreams as severe in intensity. Extreme in the survey was defined as generating “overwhelming or incapacitating distress, could not return to sleep”. Severe was defined as generating “considerable distress, difficulty returning to sleep” (Tables 6&7).
Discussion
In response to treatment preferences of the inmates, one hundred eighty-seven (66%) affirmed they would like to receive treatment for these dreams. Of the 187 respondents to the question of medication and/or psychological treatment, 156 out of 187 inmates (84%) affirmed that they would like to receive medication for these dreams. One hundred forty (140) out of 187 (74.9%) affirmed that they would like to receive psychological treatment for these dreams.
In regards to an institutional awareness of PTSD and coincident traumatic dreams, two diagnostic databases were assessed in April of 2015 for the diagnosis of PTSD. Psychiatry had formally diagnosed 275 inmates with PTSD and psychology had diagnosed 328. In April of 2015, at the time of this treatment assessment, the psychiatry service had 103 patients on prazosin. However, cross-check with the inmates favoring medication treatment for traumatic dreams showed that only 39 of these inmates were already on prazosin, leaving 117 interested in treatment (14.8% of the total prison population), but not yet offered such by prison clinicians.
The incidence of treatable traumatic dreams includes a clinical set of patients that exceeds those inmates diagnosed with PTSD. Of the 192 inmates reporting severe or extreme traumatic dreams, only 53% or 52% were formally diagnosed with PTSD by either the psychiatry or psychology services, respectively and, of these, only 36(18%) were medicated. Of the inmates reporting at least weekly trauma dreams, only 53% or 51% were diagnosed with PTSD by the psychiatry and psychology services, respectively, and only 43(22%) were medicated.
Of the 156 inmates wanting treatment for traumatic dreams, only 81(51.9%) had been diagnosed with PTSD by psychiatry and only 74(47.4%) had been diagnosed by psychology. However, of this population, 113(72.4%) had at least “weekly” traumatic dreams and 120(76.9%) had at least “severe” traumatic dreams. These findings, as part of Taycheedah’s continuous quality improvement effort, have been reported to both the psychology and psychiatry services for increased awareness of the issue and intervention options for traumatic dreaming. Both staffs have been encouraged to query inmates specifically about traumatic dreams. Psychology has been asked to consider a referral to psychiatry for prazosin treatment even without a formal diagnosis of PTSD; psychiatry has been asked to initiate treatment for traumatic dreams if there are no medical or psychiatric contraindications.
Conclusion
This survey of a women’s prison inmate population reaffirms the high incidence of trauma in the female inmate population. Eighty-eight per cent of inmates reported at least one major traumatic event with 46% reporting experiencing six or more such events. This is consistent with the high percentage of PTSD diagnoses in this prison population (328 for psychology or over 40% of the population and 275 for psychiatry or about 35% of the population). In looking at symptom relief for traumatized women, the institutional survey reported a high frequency (approximately 24% of the inmate population) experiencing nightly or weekly trauma dreams and a similar percentage experiencing severe or extreme dream intensity. Only 39 (of 156) inmates seeking somatic treatment were receiving prazosin; 117 (or 75%) were not. Similarly, of those reporting frequent, weekly to nightly traumatic dreams, or severe to extreme dream intensity, only 22% and 18%, respectively, were medicated with prazosin and the remainder was not. A corollary to these findings may be that female prisoner sleep disturbance and solicitation for sedative hypnotics may be related to the presence of traumatic dreams, a hypothesis which this study did not directly assess.
The overall conclusion for this institution-where prazosin has been utilized and discussed for clinician awareness – is that there is an under-utilization of this agent for a population of inmates with symptoms suggested as potentially responsive to this agent. In an effort to further increase the prescribing practice for prazosin at this institution and other forensic institutions, a second “efficacy” study has been developed to affirm the benefit of this agent in reducing traumatic dreaming in this female inmate population.
Acknowledgement
We thank the inmates of Taycheedah Correctional Institution for their participation and candor in the completion of this study. We thank Ms. Katie Navarre for assistance in the preparation of this manuscript.
References
- (2013) American Psychiatric Association: Diagnostic and Statistical Manual of mental Disorders. In: (5th edn), American Psychiatric Association, Arlington VA, USA.
- Cook SL, Smith SG, Tusher CP (2005) Self-reports of traumatic events in a random sample of incarcerated women. Women & Criminal Justice 16 (1-2): 107-126.
- Browne A, Miller B, Maguin E (1999) Prevalence and severity of lifetime physical and sexual victimization among incarcerated women. Int J Law Psychiatry 22(3-4): 308-314.
- Lake ES (1993) An exploration of the violent victim experiences of female offenders. Violence Vict 8(1): 41-51.
- Zlotnick C (1997) Post traumatic stress disorder (PTSD), PTSD comorbidity, and childhood abuse among incarcerated women. J Nerv and Ment Dis 185(12): 761-763.
- Reichert J, Bostwick L (2010) Post-traumatic stress disorder and victimization among female prisoners in Illinois. Illinois Criminal Justice Information Authority, pp 1-23.
- Raskind MA, Peskind ER, Hoff DF, Hart KL, Holmes HA, et al. (2007) A parallel group placebo controlled study of prazosin for trauma nightmares and sleep disturbance in combat veterans with post-traumatic stress disorder. Biol Psychiatry 61(8): 928-934.
- Germaine A, Richardson R, Moul DE, Mammen O, Haas G, et al. (2012) Placebo-controlled comparison of prazosin and cognitive-behavioral treatments for sleep disturbances in US military veterans. J Psychosom Res 72(2): 89-96.
- Raskind MA, Dobie DF, Kanter ED, Petrie EC, Thompson CE , et al. (2000) The alpha-adrenergic antagonist prazosin ameliorates combat trauma nightmares in veterans with posttraumatic stress disorder: a report of 4 cases. J Clin Psychiatry 61(2): 129-133.
- Taylor F, Raskind MA (2002) The alpha-adrenergic antagonist prazosin improves sleep and nightmares in civilian posttraumatic stress disorder. J Clin Psychopharmacology 22(1): 82-85.
- Byers MG, Allison KM, Wendel CS, Lee JK (2010) Prazosin versus quetiapine for nighttime posttraumatic stress disorder symptoms in veterans: an assessment of long-term comparative effectiveness and safety. J Clin Psychopharmacology 30: 225-229.
- Blake DD, Weathers FW, Nagy LM, Kaloupek DG, Gusman FD, et al. (1995) The development of a clinician-administered PTSD scale. J Trauma Stress 8(1): 75-90.
- Beckham JC, Moore SD, Feldman ME, Hertzberg MA, Kirby AC, et al. (1998) Health status, somatization, and severity of posttraumatic stress disorder in Vietnam combat veterans with posttraumatic stress disorder. Am J Psychiatry 155(11): 1565-1569.
- Blanchard EB, Hickling EF, Taylor AE, Loos W (1995) Psychiatric morbidity associated with motor vehicle accidents. J Nerv Ment Dis 183(8): 495-504.
- Eichelman B, Dorava A (2012) Open outcome study of prazosin in a prison female population with traumatic dreams.






























