The Role of Soluble TNF-Like Weak Inducer of Apoptosis as A Predictor of Preeclampsia
Salah Ahmed Marzouk1, Tamer Mamdouh Abdel Dayem2, Eman Saad Nassar1 and Yasmin Khaled Wagih Elgezery1*
1Department of Clinical and Chemical pathology, Alexandria University, Egypt
Submission: January 22, 2019;Published: February 07, 2019
*Corresponding author: Yasmin Khaled Wagih Elgezery, Department of Clinical and Chemical pathology, Alexandria University, Egypt
How to cite this article: Salah A M, Tamer M A D, Eman S N, Yasmin K W E. The Role of Soluble TNF-Like Weak Inducer of Apoptosis as A Predictor of Preeclampsia . J Gynecol Women’s Health 2019: 14(1): 555879. DOI: 10.19080/JGWH.2019.14.555879
Abstract
It was proved that preeclampsia is closely related to endothelial dysfunction (ED). Soluble tumor necrosis factor-like weak inducer of apoptosis (sTWEAK) is a cytokine from the TNF superfamily found in inflammatory as well as non inflammatory conditions. It was found that sTWEAK is closely linked to ED in patients suffering from atherosclerosis, primary hypertension or chronic kidney disease. In this study our aim was to compare serum sTWEAK levels in Egyptian females suffering from preeclampsia to levels in gestational age-matched healthy pregnant females and to correlate these levels with maternal and fetal outcome. This study was performed on 40 preeclamptic females and 40 healthy pregnant females. The serum sTWEAK levels were measured by an enzyme linked immunosorbent assay (ELISA) kit. ALT, AST and urinary protein/creatinine ratio (uPCR) were significantly elevated in preeclamptic subjects than healthy pregnant subjects. sTWEAK concentrations were significantly decreased in the patient group (395.1±64.74pg/mL) than the control group (432.8±65.73pg/mL) (p=0.012). Our study showed that sTWEAK is lower in females suffering from preeclampsia than gestational age-matched healthy pregnant females. sTWEAK might play a role in preeclampsia development and could be considered as a promising predictor marker for preeclampsia diagnosis.
Keywords: Preeclampsia; sTWEAK; Endothelial dysfunction; Angiogenesis
Abbrevations: ED: Endothelial Dysfunction; sTWEAK: Soluble Tumor Necrosis Factor-Like Weak Inducer of Apoptosis; TNF: Tumor Necrosis Factor
Introduction
Preeclampsia (PE) is a syndrome specific to pregnancy. It complicates 2-8% of pregnancies. It is a main cause for maternal as well as fetal morbidity and mortality all around the world [1]. It classically appears around gestational age of 20 weeks with symptoms of hypertension and proteinuria [2]. PE is a multifactorial disease. PE was thought to be due to placental ischemia (The two-stage theory); it states that partial or lack of cytotrophoblastic invasion of spiral arteries causes poor placental blood supply, causing placental ischemia, which in turn, releases inflammatory substances that leads to endothelial dysfunction (ED). This leads to the manifestations of PE [3]. Also, PE was thought to be due to imbalance between antiangiogenic factors such as; soluble fms-like tyrosine kinase 1 (sFlt-1) as well as soluble endoglin (sEng), and pro-angiogenic factors such as; placental growth factor (PLGF) as well as vascular endothelial growth factor (VEGF). Increased antiangiogenic factors levels and decreased levels of pro-angiogenic factors lead to generalised ED of maternal blood vessels, hypertension, renal endotheliosis and coagulopathy [4].
Pregnant females suffering from PE have serious complications such as liver rupture, pulmonary edema, renal failure, eclampsia, or HELLP syndrome and death [5,6]. Moreover, PE may cause early rupture of membrane and preterm delivery causing cerebral palsy [7,8]. Offspring of preeclamptic mothers may suffer from premature delivery, low birth weight, IUGR or intrauterine fetal death [7].
Tumor necrosis factor super family (TNFSF) is a family of cytokines consisting of 19 ligands [9]. Tumor necrosis factor-like weak inducer of apoptosis (TWEAK, TNFSF12) is one of the TNSF. It is a 249-amino-acid (aa). It has two forms; membrane-bound protein (mTWEAK) and soluble form (sTWEAK). mTWEAK is processed proteolytically by furin, releasing a 156-aa, soluble form (sTWEAK) [10]. TWEAK binds to its receptor; fibroblast growth factor-inducible 14 (Fn14) [11]. Both mTWEAK and sTWEAK can bind to Fn14 [12]. It was discovered that CD163 is the scavenger receptor for TWEAK [13]. CD163 is expressed by macrophages. It can bind to TWEAK and allow the internalisation and production of sTWEAK. Hence, this mechanism represents a negative regulatory pathway of TWEAK/Fn14 [14]. The main source of sTWEAK in inflammatory conditions is macrophages [15-18]. Also, it is produced by non-immune cells, such as endothelial cells and renal cells [19].
TWEAK/Fn14 signaling is important in many biological activities such as angiogenesis and inflammatory responses [20,21]. Also, TWEAK/ Fn14 interaction was found to increase VEGF expression via the NF-κB pathway. TWEAK can cooperate with FGF-2 as well as VEGF-A in tumor angiogenesis [12]. It was discovered that sTWEAK is linked to ED in chronic kidney disease (CKD) patients. Soluble TWEAK is considered an independent predictor for ED in addition to its role in angiogenesis [22]. Moreover, it was discovered that in young patients suffering from primary hypertension, sTWEAK serum concentrations were decreased, than the non-hypertensive group [23].
Up till now, few data is known on the function of sTWEAK in PE, whose pathogenesis was proved to be linked to angiogenesis and ED. Our aim in this study was to compare sTWEAK concentrations in Egyptian women with PE to sTWEAK concentrations in gestational age-matched healthy pregnant women and to correlate its levels with maternal and fetal outcome.
Materials and Methods
Patients
This study was made on eighty pregnant females in the 3rd trimester of pregnancy; forty pregnant females with preeclampsia and forty gestational age-matched females without preeclampsia. All subjects were recruited from the Obstetrics and Preeclampsia units of the Department of Obstetrics and Gynecology at El-Shatby Maternity University Hospital. Approval of the ethics committee was obtained and a written informed consent was taken from each patient. The criteria for diagnosis of preeclampsia were; newly developed hypertension (blood pressure≥140mmHg systolic and ≥90mmHg diastolic at least 4 hours apart) after 20 weeks gestation, with or without newly developed proteinuria (≥0.3 grams in a 24 hour specimen of urine or urinary protein/creatinine ratio ≥0.3). Exclusion criteria were; twin or multiple pregnancies, diabetes mellitus (DM), previous renal disease, chronic hypertension and receiving medications for any disease. All participants were subjected to detailed history taking regarding demographic data such as age, gravidity, parity and last menstrual period (LMP) as well as medical history including hypertension, DM, hepatic and renal diseases.
Routine laboratory measurements
Venous blood samples from participants were obtained. Hemoglobin, platelet count and white blood cell count, were measured using 3 part differential automated cell counter Sysmex, Sysmex, Kobe, Japan KX-21N. Alanine transaminase (ALT), aspartate transaminase (AST), serum creatinine and serum urea were assessed by standard laboratory methods using RxL dimension autoanalyser. A random urine sample was also collected from the participants and urinary protein was measured by turbidimetric method while urinary creatinine was measured by RxL dimension autoanalyser. Then, urinary protein/creatinine ratio (uPCR) was calculated.
Measurement of Serum sTWEAK
Blood samples were collected, samples were allowed to clot for 30 minutes before centrifugation for 15 minutes at about 1000×g. Serum was removed, aliquot was prepared and samples were stored at -80 ℃ until the time of analysis. The concentrations of sTWEAK in serum were determined by an enzyme-linked immunosorbent assay (ELISA) kit (Human Tumor necrosis factor ligand superfamily member 12, ELISA Kit. catalog No.: E1883h. Wuhan EIAab® Science Co., Ltd. Wuhan, CHINA). A microplate photometer was used for readings at a wave length of 450nm. The results were expressed as pg/mL.
Ultrasonographic examination for biometry, liquor, movements and flow resistance in the umbilical artery was done using Voluson P8 ultrasound machine; GE®. Follow up was done till delivery as well as correlation of sTWEAK levels with maternal and fetal outcome.
Statistical analysis
Data were fed to the computer and analyzed using IBM SPSS software package version 20.0 (Armonk, NY: IBM Corp). Number and percent were used to describe qualitative data. Verification of the normality of distribution was done using the Kolmogorov- Smirnov test. Range (minimum and maximum), mean, standard deviation and median were used to describe quantitative data. Significance of the obtained results was judged at the 5% level (variables expressed as mean±SD. were statistically significant at p≤0.05). The used tests were; Chi-square test used for categorical variables, to compare between different groups. Also, Fisher’s Exact or Monte Carlo correction test was used for the correction for chi-square when more than 20% of the cells have expected count less than 5. Moreover, Student t-test was used for normally distributed quantitative variables, to compare between the two groups. In addition, Mann Whitney test was used for abnormally distributed quantitative variables, to compare between the two groups. Also, regression analysis was used to detect the most independent/affecting factor for the parameters that affect sTWEAK.
Result
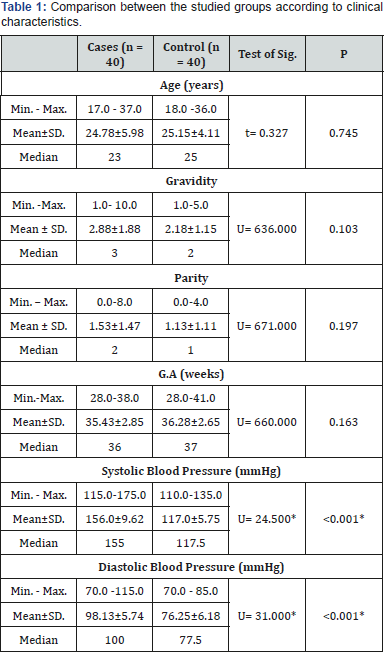
U, p: U and p values for Mann Whitney test for comparing between the two groups
t, p: t and p values for Student t-test for comparing between the two groups
*: Statistically significant at p ≤ 0.05
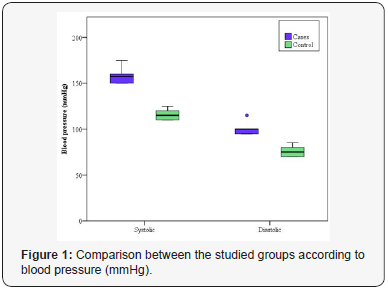
Clinical characteristics of preeclamptic females and the healthy controls are shown in Table 1. There was no significant difference discovered between the two groups regarding age, gravidity, parity and gestational age (GA). The mean systolic blood pressure was 156.0±9.62 and 117.0±5.75mmHg for PE group and control one, respectively. We discovered a statistically significant difference between the studied groups concerning systolic blood pressure (p<0.001) (Figure 1), while, the mean diastolic blood pressure was 98.13±5.74 and 76.25±6.18mmHg for patients with PE and healthy pregnant group, respectively. A significant difference was discovered between the studied groups regarding diastolic blood pressure (p<0.001) (Figure 1).
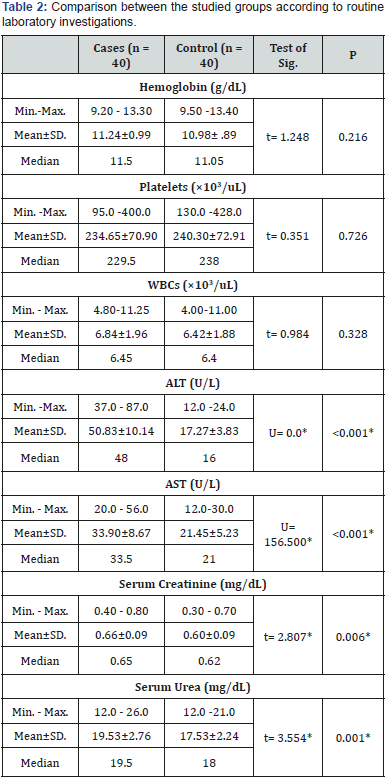
t, p: t and p values for Student t-test for comparing between the two groups
U, p: U and p values for Mann Whitney test for comparing between the two groups
*: Statistically significant at p ≤ 0.05
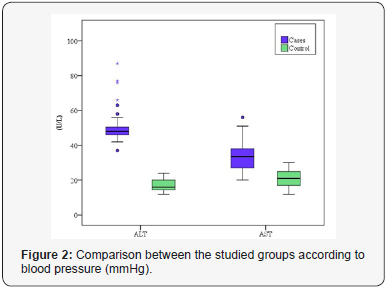
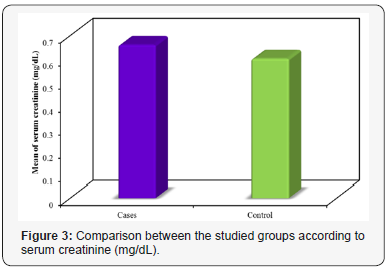
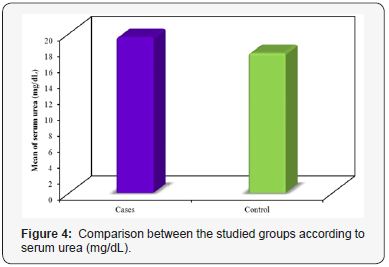
The routine laboratory investigations of both groups are shown in Table 2. There was no statistically significant difference discovered between the studied groups concerning the hemoglobin, the platelet count and the white blood cell count. The mean ALT was 50.83±10.14 and 17.27±3.83U/L for patients with PE and healthy pregnant group, respectively. We discovered a statistically significant difference between the two groups concerning ALT (p<0.001) (Figure 2). The mean AST was 33.90±8.67 and 21.45±5.23 U/L for patients with PE and healthy pregnant group, respectively. There was a statistically significant difference discovered between the two groups (p<0.001) regarding AST. The mean serum creatinine was 0.66±0.09 and 0.60±0.09 mg/dL for PE group and control one, respectively. A statistically significant difference was discovered between the studied groups concerning serum creatinine (p=0.006) (Figure 3). The mean serum urea was 19.53±2.76 and 17.53±2.24mg/dL for patients with PE group and control one, respectively. A statistically significant difference was discovered between the studied groups regarding serum urea (p=0.001) (Figure 4).
U, p: U and p values for Mann Whitney test for comparing between the two groups
t, p: t and p values for Student t-test for comparing between the two groups
*: Statistically significant at p ≤ 0.05
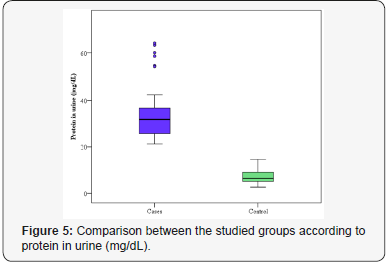
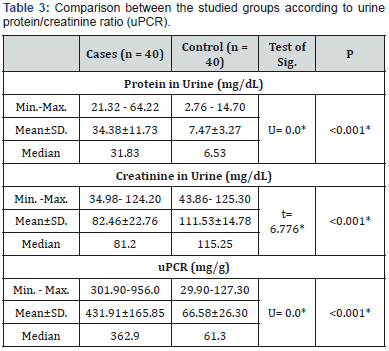
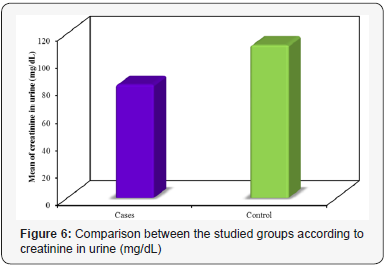
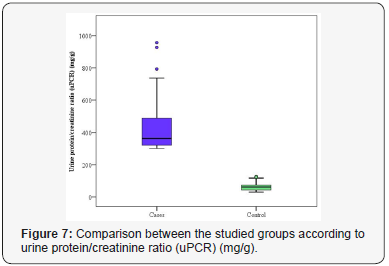
Urinary protein, urinary creatinine and urinary protein/ creatinine ratio (uPCR) are shown in Table 3. The mean protein in urine was 34.38±11.73 and 7.47±3.27mg/dL for patients with PE group and control one, respectively. A statistically significant difference was proved between the studied groups concerning protein in urine (p<0.001) (Figure 5). The mean creatinine in urine was 82.46±22.76 and 111.53±14.78 mg/dL for patients with PE and healthy pregnant group, respectively. There was a significant difference proved between the different studied groups regarding creatinine in urine (p<0.001) (Figure 6). The mean uPCR was 431.91±165.85 and 66.58±26.30mg/g for PE group and control one, respectively. There was a statistically significant difference discovered between the studied groups concerning uPCR ratio (p<0.001) (Figure 7).
t, p: t and p values for Student t-test for comparing between the two groups
*: Statistically significant at p ≤ 0.05
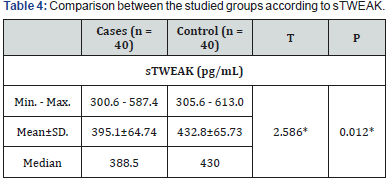
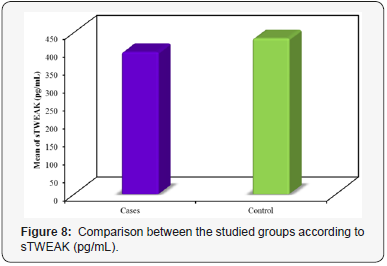
The sTWEAK levels of both groups are shown in Table 4. The mean sTWEAK was 395.1±64.74 and 432.8±65.73pg/mL for patients with PE and healthy pregnant group, respectively. A significant difference was discovered between the two studied groups concerning to sTWEAK (p=0.012) (Figure 8).
χ2, p: χ2 and p values for Chi square test for comparing between the two groups
FEp: p value for Fisher Exact for Chi square test for comparing between the two groups
U, p: U and p values for Mann Whitney test for comparing between the two groups
*: Statistically significant at p ≤ 0.05
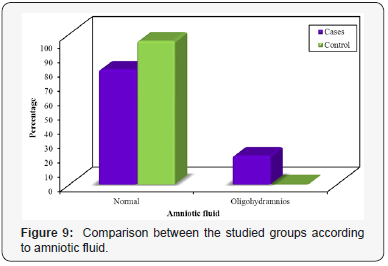
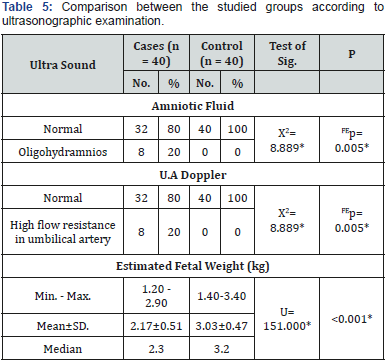
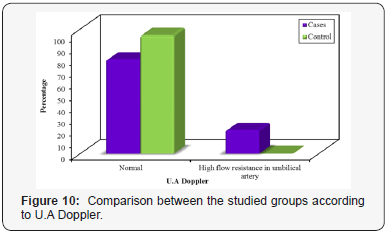
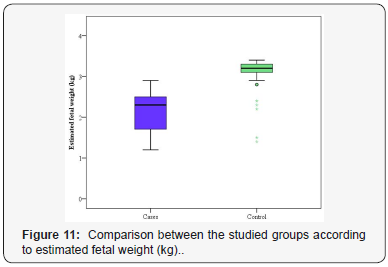
The ultrasonographic examination results of the studied groups are shown in Table 5. In the PE group, 80% had adequate amount of amniotic fluid. However, 20% of the PE group had oligohydramnios. While in the control group, 100% of the pregnant females had adequate amount of amniotic fluid. There was a significant difference proved between the studied groups (FEp=0.005) (Figure 9). In the PE group, 80% had normal flow resistance in the umbilical artery. However, 20% of the PE group had high flow resistance in the umbilical artery. While in the healthy pregnant group 100% of the pregnant females had normal flow resistance in the umbilical artery. There was a significant difference discovered between the two groups (FEp=0.005) (Figure 10). The mean estimated fetal weight was 2.17±0.51 and 3.03±0.47kg for PE group and control one, respectively. A significant statistical difference was proved between the two different groups was detected according to estimated fetal weight (p<0.001) (Figure 11).
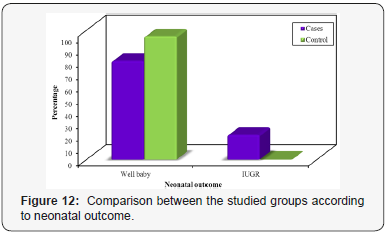
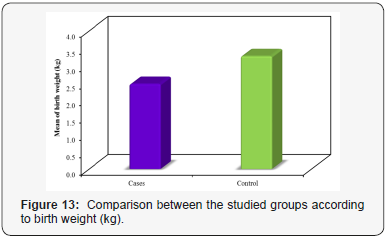
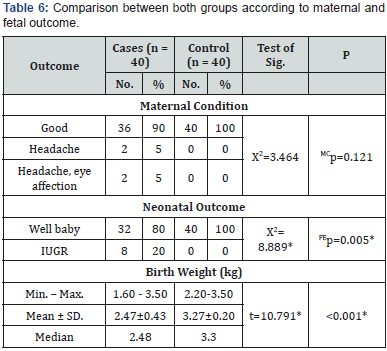
Maternal and fetal outcome of both groups is presented in Table 6. In the PE group, 90% had good maternal condition. However, 5% of the PE group had headache and 5% of the PE group had headache together with eye affection. While in the control group, 100% of the pregnant females had good maternal condition. No statistically significant difference was discovered between the studied groups (MCp=0.121). Regarding the neonatal outcome, in the PE group, 80% had well babies. However, 20% of the PE group had IUGR. While in the control group, 100% of the pregnant females had well babies. There was a statistically significant difference discovered between the two groups (FEp=0.005) (Figure 12). The mean birth weight was 2.47±0.43 and 3.27±0.20kg for patients with PE and healthy pregnant group, respectively. There was a significant statistical difference discovered between the different two groups concerning birth weight (p<0.001) (Figure 13).
χ2, p: χ2 and p values for Chi square test for comparing between the two groups
MCp: p value for Monte Carlo for Chi square test for comparing between the two groups
FEp: p value for Fisher Exact for Chi square test for comparing between the two groups
t, p: t and p values for Student t-test for comparing between the two groups
*: Statistically significant at p ≤ 0.05
B: Unstandardized Coefficients
C.I: Confidence interval
#: All variables with p<0.05 was included in the multivariate
*: Statistically significant at p≤0.05
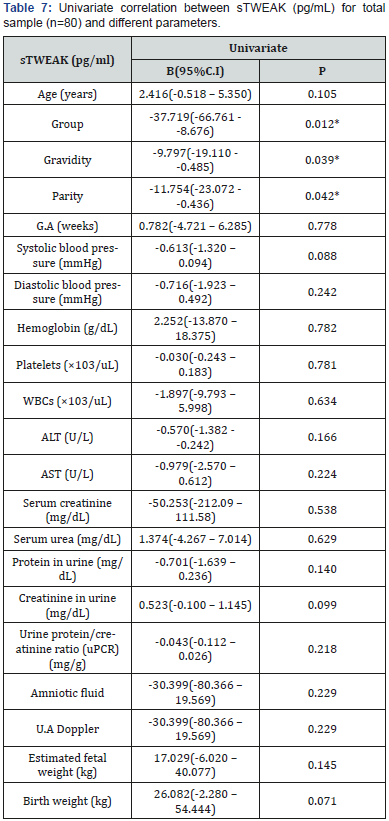
A positive correlation was found between sTWEAK and the study group (p=0.012), gravidity (p=0.039) and parity (p=0.042) in the total sample (Table 7). Moreover, multivariate linear regression analysis showed that the association between sTWEAK and the study group (β=-0.251, p=0.027) was still significant after adjusting for other parameters. Therefore, the study group was discovered to be the only strong independent factor affecting sTWEAK (Table 8).
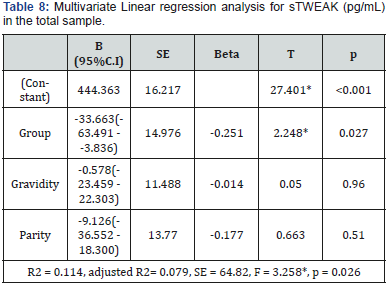
B: Unstandardized Coefficients
C.I: Confidence interval
SE: Standard error
Beta: standardized Coefficients
t: Student t-test
#: All variables with p<0.05 was included in the multivariate
*: Statistically significant at p ≤ 0.05
THMs (sTWEAK) = 444.363- (33.663* Group) - (0.578* Gravidity) - (9.126* Parity)
Discussion
In this study, a significant difference was discovered between the patient group and the control one regarding systolic blood pressure (SBP) and diastolic blood pressure (DBP) (p<0.001). This agrees with the standard criteria for diagnosing preeclampsia, as described by the American College of Obstetricians and Gynecologists. Similar to our findings, Yildirim ZK et al. [24] discovered that SBP and DBP showed a highly significant elevation in the preeclamptic females than the healthy pregnant females. In addition, Fasshauer M et al. [25] found that SBP and DBP were increased in preeclamptic females than healthy controls. Moreover, in our study we found a statistically significant difference between the different groups concerning routine laboratory investigations such as ALT, AST, serum creatinine and serum urea (p<0.001, p<0.001, p=0.006 and p=0.001, respectively). Mohsen M et al. [26] performed a study on 90 women; 60 with PE and 30 healthy pregnant controls. This study showed a highly statistically significant elevation in the preeclamptic group than the healthy pregnant group in ALT as well as AST levels. Similarly, Yildirim ZK and his colleagues [24] proved that serum creatinine levels were significantly higher in the patient group compared with the control group. This was reinforced by, Fasshauer M and his colleagues [25] who found that serum creatinine levels were elevated significantlyv in preeclamptic females than healthy pregnant females.
Also, in ours, we discovered a significant difference between the different groups as regards uPCR (p<0.001). In concordance with us, Yildirim ZK et al. [24] stated that uPCR increased significantly in the PE group than the healthy control group. This was reinforced by a study performed by Demirci O et al. [27] who found that uPCR had increased values in the preeclamptic group than the control one.
In our study, the mean sTWEAK was 395.1±64.74 and 432.8± 65.73pg/mL for patients with PE and healthy pregnant group, respectively. The maternal serum sTWEAK concentrations decreased significantly in PE patients than healthy controls (p=0.012). Our results may be attributed to the fact that in PE the antiangiogenic factors increase and the angiogenic factors decrease [28-31]. The imbalance between angiogenic and antiangiogenic factors, thus, causes endothelial dysfunction (ED), which has an important role in the clinical manifestations of PE [32]. ED was proved to be highly related to the decreased level of sTWEAK. Moreover, it was discovered that sTWEAK has an angiogenic effect [33]. Therefore, the decrease in sTWEAK levels that occur due to ED may lead to PE. Also, sustained increase of blood pressure leads to chronic inflammation, which in turn increases Fn14 level. Thus, binding of Fn14 to sTWEAK increases, causing a decrease of sTWEAK levels. In addition, CD163 expressing macrophages during inflammation are increased, causing breakdown of sTWEAK in addition to end organ damage.
In agreement with our findings, Yildirim ZK et al. [24] performed a study aiming to test serum sTWEAK levels in preeclamptic females in addition to healthy pregnant females with similar gestational age. Maternal serum sTWEAK levels were measured in thirty three patients suffering from preeclampsia and thirty three healthy pregnant controls. The sTWEAK concentrations decreased significantly in patients suffering from preeclampsia (332±144pg/mL) than in normal pregnant controls (412±166pg/mL) (p=0.04). This was explained by the hypothesis that sTWEAK is decreased due ED or because of its role in the pathogenesis of PE via angiogenic imbalance.
Similarly, Karadurmus N et al. [23] found that serum sTWEAK concentrations decreased significantly in primary hypertensive group compared to control one. Moreover, the sTWEAK concentration in serum was negatively correlated with SBP as well as DBP. It was also found that the mean plasma asymmetrical dimethyl arginine (ADMA) levels increased significantly in the primary hypertensive group. High ADMA concentration in plasma is considered an indicator of ED [34]. ADMA was proved to be more in patients suffering from systemic atherosclerosis, hypercholesterolemia, essential hypertension and end-stage renal failure [35]. These diseases are related to an impairment of the NO-pathway as well as ED [34]. In concordance, Böger RH [36] discovered that ADMA levels were increased in plasma of hypertensive patients. These results were attributed to the presence of the scavenger receptor of sTWEAK; CD163, which can sequester and degrade sTWEAK under proinflammatory conditions [37,38].
This was supported by Ates I et al. [39] who performed a study on primary hypertensive (HT) patients with/without asymptomatic organ damage (AOD), aiming to measure sTWEAK as well as IL-17A serum concentrations in AOD. Also, they correlated sTWEAK and IL-17A levels with; carotid intima media thickness (CIMT), proteinuria, retinopathy as well as the left ventricle mass index (LVMI). The sTWEAK concentration decreased significantly in the hypertensive patients suffering from AOD compared to those not suffering from AOD. The sTWEAK concentration in serum negatively correlated with the microalbuminuria level, proteinuria level, LVMI, mean 24-h SBP and duration of hypertension. This was explained by the fact that, chronic increased blood pressure can cause chronic inflammation, during which, Fn14 concentration is increased, thus Fn14 binding to sTWEAK is increased, leading to a decrease in the sTWEAK concentration in serum [40]. Moreover, during inflammation, CD163 (the scavenger receptor of sTWEAK) expression is increased by inflammatory macrophages. Thus, the sTWEAK break down is increased causing a decrease of serum sTWEAK concentrations [37].
This was supported by, Yilmaz M I et al. [41] who reported that, in chronic kidney disease (CKD), sTWEAK concentrations decreased gradually with the decrease of estimated glomerular filtration rate (eGFR). Moreover, they discovered an independent relationship between sTWEAK levels and ED in subjects suffering from CKD. This was also explained by, increase the expression of TWEAK or its receptor; Fn-14, by endothelial cells [42,43] It was proved that during inflammation, the expression of Fn14 increases and vascular cells are sensitized to TWEAK, causing apoptosis and producing proinflammatory substances [44-46] Thus, in CKD patients decreased sTWEAK concentrations may be a compensatory mechanism to guard against the apoptotic complications resulting from increased Fn14 activation [46]. Also, it was reported that during inflammation, macrophages which express CD163 increase, therefore binding, internalization and degradation of sTWEAK increase as well [37]. Thus, the sTWEAK decrease in CKD patients may also be due to the CD163 increase, in patients suffering from late stage CKD [38,47]. Another explanation, is that sTWEAK concentrations in serum decrease in patients with CKD due to TWEAK defective shedding [41].
Moreover, Kralisch S et al. [48] stated that sTWEAK concentrations are lower in type two diabetes mellitus and endstage renal disease patients than control patients. The sTWEAK concentrations in plasma decrease with the increase of ED and increased mortality risk.
Also, in ours, we discovered a significant difference between the different groups as regards amniotic fluid and U.A Doppler (FEp=0.005) as well as fetal outcome such as neonatal outcome and fetal birth weight (FEp=0.005 and p<0.001 respectively). In another study, conducted by Yildirim ZK et al. [24] it was found that fetal birth weight increased significantly in the PE females than the healthy females.
Moreover, in our study, a positive correlation was found between sTWEAK and the study group (p=0.012), gravidity (p=0.039) and parity (p=0.042) in the total sample. Multivariate linear regression analysis showed that the association between sTWEAK and the study group (β=-0.251, p=0.027) was still significant after adjusting for other parameters. Therefore, the study group was the only strong independent factor affecting sTWEAK. Similar to us, Yildirim ZK et al. [24] discovered that, in the linear regression analysis model formed by parameters considered potentially related to sTWEAK levels (age, the study group, the level of proteinuria, serum uric acid levels and systolic blood pressure), the study group was proved to be the only independent variable related to sTWEAK level (β=0.663, p=0.009).
Conclusion
In our study we concluded that maternal serum sTWEAK concentrations decreased significantly in patients suffering from preeclampsia than healthy controls. The study group was proved to be the only strong independent predictor of circulating sTWEAK in preeclampsia patients. Further studies are needed to specify the exact role of sTWEAK in PE pathogenesis and state if sTWEAK can be considered as a promising predictor marker for preeclampsia diagnosis.
Acknowledgement
The authors would like to express their gratitude to the Department of Clinical and Chemical pathology, as well as, the Department of Obstetrics and Gynecology, Faculty of Medicine, Alexandria University for their continuous help, support and cooperation during this research.
Conflict of Interest
The authors report no conflict of interests. The authors alone are responsible for the content and writing of the paper.
References
- Cerdeira AS, Agrawal S, Staff AC, Redman CW, Vatish M, et al. (2017) Angiogenic factors: potential to change clinical practice in preeclampsia? BJOG 125(11): 1389-1395.
- Townsend R, Obrien P, Khalil A (2016) Current best practice in the management of hypertensive disorders in pregnancy. Integr Blood Press Control 9: 79-94.
- Roberts JM (2014) Pathophysiology of ischemic placental disease. Semin Perinatol 38(3): 139-145.
- Gathiram P, Moodley J (2016) Pre-eclampsia: its pathogenesis and pathophysiolgy. Cardiovasc J Afr 27(2): 71-78.
- Souza JP, Gulmezoglu AM, Vogel J, Carroli G, Lumbiganon P, et al. (2013) Moving beyond essential interventions for reduction of maternal mortality (the WHO Multicountry Survey on Maternal and Newborn Health): a cross-sectional study. Lancet 381(9879): 1747-1755.
- Mohammedseid S, Megersa T, Kumbi S, Ayalew M (2017) Maternal Outcomes of Preeclampsia in an Ethiopian Gynecologic Hospital. Ann Med Health Sci Res 7: 16-21.
- Pokharel N, Shrestha M, Regmi M (2015) Maternal, fetal and new born outcomes in pre-eclampsia and eclampsia: a hospital based study. Health Renaissance12 (2): 106-110.
- Strand KM, Heimstad R, Iversen AC, Austgulen R, Lydersen S, et al. (2013) Mediators of the association between pre-eclampsia and cerebral palsy: population based cohort study. Bmj 347: f4089.
- Sonar S, Lal G (2015) Role of Tumor Necrosis Factor Superfamily in Neuroinflammation and Autoimmunity. Front Immunol 6: 364.
- Blanco-Colio LM (2014) TWEAK/Fn14 Axis: A Promising Target for the Treatment of Cardiovascular Diseases. Front Immunol, 5: 3.
- Wang X, Xiao S, Xia Y (2017) Tumor Necrosis Factor Receptor Mediates Fibroblast Growth Factor-Inducible 14 Signaling. Cell Physiol Biochem 43(2): 579-588.
- Hu G, Zeng W, Xia Y (2017) TWEAK/Fn14 signaling in tumors. Tumour Biol 39(6): 1010428317714624.
- Balaban YF, Orem A, Aksu AD, Altinkaynak B, Aksan B, et al. (2017) Soluble tumor necrosis factor-like weak inducer of apoptosis and soluble CD163 levels in patients with behcet’s disease. Atherosclerosis 263: e140-e141.
- Sanz AB, Izquierdo MC, Sanchez-Nino MD, Ucero AC, Egido J, et al. (2014) TWEAK and the progression of renal disease: clinical translation. Nephrol Dial Transplant, 29 (Suppl 1): i54-i62.
- Bird TG, Lu WY, Boulter L, Gordon-Keylock S, Ridgway RA, et al. (2013) Bone marrow injection stimulates hepatic ductular reactions in the absence of injury via macrophage-mediated TWEAK signaling. Proc Natl Acad Sci USA 110(16): 6542-6547.
- Madrigal-Matute J, Fernandez-Laso V, Sastre C, Llamas-Granda P, Egido J, et al. (2015) TWEAK/Fn14 interaction promotes oxidative stress through NADPH oxidase activation in macrophages. Cardiovasc Res 108(1): 139-147.
- Sharif MN, Campanholle G, Nagiec EE, Wang J, Syed J, et al. (2016) Soluble Fn14 Is Detected and Elevated in Mouse and Human Kidney Disease. PLoS One 11(5): e0155368.
- Liu Q, Xiao S, Xia Y (2017) TWEAK/Fn14 Activation Participates in Skin Inflammation. Mediators Inflamm 2017: 6746870.
- Xu WD, Zhao Y, Liu Y (2016) Role of the TWEAK/Fn14 pathway in autoimmune diseases. Immunol Res 64(1): 44-50.
- Ameri H, Liu H, Liu R, Ha Y, Paulucci-Holthauzen AA, et al. (2014) TWEAK/Fn14 pathway is a novel mediator of retinal neovascularization. Invest Ophthalmol Vis Sci 55(2): 801-813.
- Martino DL, Dave M, Menghini P, Xin W, Arseneau KO, et al. (2016) Protective Role for TWEAK/Fn14 in Regulating Acute Intestinal Inflammation and Colitis-Associated Tumorigenesis. Cancer Res 76(22): 6533-6542.
- Turkmen K, Tonbul HZ, Erdur FM, Toker A, Biyik Z, et al. (2013) Soluble TWEAK independently predicts atherosclerosis in renal transplant patients. BMC Nephrol 14: 144.
- Karadurmus N, Tapan S, Cakar M, Naharci I, Celik T, et al. (2012) Lower plasma soluble TWEAK concentration in patients with newly diagnosed hypertension. Clin Invest Med 35(1): E20-26.
- Yildirim ZK, Sumnu A, Bademler N, Kilic E, Sumnu G, et al. (2016) Soluble TNF-Like Weak Inducer of Apoptosis as a New Marker in Preeclampsia: A Pilot Clinical Study. Dis Markers, 5930589.
- Fasshauer M, Seeger J, Waldeyer T, Schrey S, Ebert, T. et al. (2008) Serum levels of the adipokine adipocyte fatty acid-binding protein are increased in preeclampsia. Am J Hypertens 21(5): 582-586.
- Mohsen M, Algohary EA, Hassan SH, El-Sherbeny AA, El-Hadi EAA, et al. (2015) Study of possible relation between maternal serum resistin and insulin resistance in patients with preeclampsia. Egypt J Obes Diab Endocrinol 1(2): 77.
- Demirci O, Kumru P, Arinkan A, Ardic C, Arisoy R, et al. (2015) Spot protein/creatinine ratio in preeclampsia as an alternative for 24-hour urine protein. Balkan Med J 32(1): 51-55.
- Maynard S, Epstein FH, Karumanchi SA (2008) Preeclampsia and angiogenic imbalance. Annu Rev Med 59: 61-78.
- Maynard SE, Min JY, Merchan J, Lim KH, Li J, et al. (2003) Excess placental soluble fms-like tyrosine kinase 1 (sFlt1) may contribute to endothelial dysfunction, hypertension, and proteinuria in preeclampsia. J Clin Invest 111(5): 649-658.
- Venkatesha S, Toporsian M, Lam C, Hanai J, Mammoto T, et al. (2006) Soluble endoglin contributes to the pathogenesis of preeclampsia. Nat Med 12(6): 642-649.
- Levine RJ, Lam C, Qian C, Yu KF, Maynard SE, et al. (2006) Soluble endoglin and other circulating antiangiogenic factors in preeclampsia. N Engl J Med 355(10): 992-1005.
- Heidema WM, Scholten RR, Lotgering FK, Spaanderman ME (2015) History of preeclampsia is more predictive of cardiometabolic and cardiovascular risk factors than obesity. Eur J Obstet Gynecol Reprod Biol 194: 189-193.
- El-Asrar AAM, Hertogh DG, Nawaz MI, Siddiquei MM, Eynde VDK, et al. (2015) The tumor necrosis factor superfamily members TWEAK, TNFSF15 and fibroblast growth factor-inducible protein 14 are upregulated in proliferative diabetic retinopathy. Ophthalmic Res 53(3): 122-130.
- Landim MB, Casella FA, Chagas AC (2009) Asymmetric dimethylarginine (ADMA) and endothelial dysfunction: implications for atherogenesis. Clinics (Sao Paulo), 64(5): 471-478.
- Kielstein JT, Fliser D (2007) The past, presence and future of ADMA in nephrology. Nephrol Ther 3(2): 47-54.
- Boger RH (2003) The emerging role of asymmetric dimethylarginine as a novel cardiovascular risk factor. Cardiovasc Res 59(4): 824-833.
- Moreno JA, Munoz-Garcia B, Martin-Ventura JL, Madrigal-Matute J, Orbe J, et al. (2009) The CD163-expressing macrophages recognize and internalize TWEAK: potential consequences in atherosclerosis. Atherosclerosis 207(1): 103-110.
- Axelsson J, Moller HJ, Witasp A, Qureshi AR, Carrero JJ, et al. (2006) Changes in fat mass correlate with changes in soluble sCD163, a marker of mature macrophages, in patients with CKD. Am J Kidney Dis 48(6): 916-925.
- Ates I, Ozkayar N, Akyel F, Topcuoglu C, Akyel S, et al. (2014) The relationship between asymptomatic organ damage, and serum soluble tumor necrosis factor-like weak inducer of apoptosis (sTWEAK) and Interleukin-17A (IL-17A) levels in non-diabetic hypertensive patients. BMC Nephrol 15: 159.
- Vendrell J, Chacon MR (2013) TWEAK: A New Player in Obesity and Diabetes. Front Immunol 4: 488.
- Yilmaz MI, Carrero JJ, Ortiz A, Martin-Ventura JL, Sonmez A, et al. (2009) Soluble TWEAK plasma levels as a novel biomarker of endothelial function in patients with chronic kidney disease. Clin J Am Soc Nephrol 4(11): 1716-1723.
- Harada N, Nakayama M, Nakano H, Fukuchi Y, Yagita H, et al. (2002) Proinflammatory effect of TWEAK/Fn14 interaction on human umbilical vein endothelial cells. Biochem Biophys Res Commun 299(3): 488-493.
- Donohue PJ, Richards CM, Brown SA, Hanscom HN, Buschman J, et al. (2003) TWEAK is an endothelial cell growth and chemotactic factor that also potentiates FGF-2 and VEGF-A mitogenic activity. Arterioscler Thromb Vasc Biol 23(4): 594-600.
- Sanz AB, Justo P, Sanchez-Nino MD, Blanco-Colio LM, Winkles JA, et al. (2008) The cytokine TWEAK modulates renal tubulointerstitial inflammation. J Am Soc Nephrol 19(4): 695-703.
- Munoz-Garcia B, Martin-Ventura JL, Martinez E, Sanchez S, Hernandez G, et al. (2006) Fn14 is upregulated in cytokine-stimulated vascular smooth muscle cells and is expressed in human carotid atherosclerotic plaques: modulation by atorvastatin. Stroke 37(8): 2044-2053.
- Winkles JA (2008) The TWEAK–Fn14 cytokine–receptor axis: discovery, biology and therapeutic targeting. Nat Rev Drug Discov 7(5): 411-425.
- Bover LC, Cardo-Vila M, Kuniyasu A, Sun J, Rangel R, et al. (2007) A previously unrecognized protein-protein interaction between TWEAK and CD163: potential biological implications. J Immunol 178(12): 8183-8194.






























