Vaginal Delivery and Postpartum Hemorrhage Simulation Skills and Confidence Level of Skilled-Birth Attendants in Rural Rwanda
Verόnica Maria Pimentel1*, Denis Rwabizi2, John Gahima2, Stephen Rulisa3, Xianhong Xie4, Peter S Bernstein1 and Lisa M Nathan1
1 Department of Obstetrics & Gynecology and Women’s Health, Albert Einstein College of Medicine, USA
2 Department of Obstetrics and Gynecology, University Teaching Hospital of Kigali, Rwanda
3 College of Medicine and Health Sciences, University of Kigali, Rwanda
4 Department of Epidemiology and Population Health, Albert Einstein College of Medicine, USA
Submission: August 01, 2018; Published: August 20, 2018
*Corresponding author: Veronica Maria Pimentel, Department of Obstetrics & Gynecology and Women’s Health, Albert Einstein College of Medicine, Bronx, NY, USA, Email:vonypimentel@gmail.com
How to cite this article: Verόnica M P, Denis R, John G, Stephen R, Xianhong X, Peter S B, et.al. Vaginal Delivery and Postpartum Hemorrhage Simulation Skills and Confidence Level of Skilled-Birth Attendants in Rural Rwanda. J Gynecol Women’s Health. 2018: 11(2): 555809. DOI: 10.19080/JGWH.2018.11.555809
Abstract
Objectives: To evaluate and compare the vaginal delivery (VD) and postpartum hemorrhage (PPH) skills of skilled-birth attendants (SBAs).
Methods:? A post-intervention simulation study was conducted in rural Rwanda with two separate groups of SBAs 30 months (Group 1) and 18 months (Group 2) after the initial simulation training. Participants were scored on communication, evaluation, and management skills. SBA-confidence levels were assessed using a survey. Two-sample t-test was used to compare total skills scores and confidence levels. Pearson’s chi-square was used to compare passing scores ≥ 60% correct.
Results: Twenty-six SBAs participated in the study; 14 in Group 1 and 12 in Group 2. The overall mean score was 72.9% for VD and 57.7% for PPH. Group 2 scored higher than Group 1 on VD simulation skills (84.5% vs. 59.6%, p= 0.03). Overall, pass rate was 62% for VD and 33% for PPH. VD simulation pass rate was higher for Group 2 than Group 1 (80% vs. 33%, p=0.04). There was no difference in the PPH simulation pass rate and in confidence levels. Conclusion: Passing rates were low. VD performance was greater 18 months after initial training compared to 30 months later while confidence levels were similar
SynopsisSkilled-birth attendants’ postpartum hemorrhage skill simulation pass rate was low. Vaginal delivery performance was greater one year compared to two years after training.
Keywords: Simulation training; Skilled-birth attendants; Rwanda; Vaginal delivery; Postpartum Hemorrhage
Abbrevations:WHO: World Health Organization; ICM: International Confederation of Midwives; FIGO: Federation of Gynecology and Obstetrics; SBAs: Skilled Birth Attendants; PPH: Postpartum Hemorrhage; VD: Vaginal Delivery
Introduction
The World Health Organization (WHO), International Confederation of Midwives (ICM) and International Federation of Gynecology and Obstetrics (FIGO) advocate for the presence of skilled birth attendants (SBAs) at every birth with the goal of reducing both maternal and newborn morbidity and mortality [1]. SBA is a healthcare professional proficiently trained “to manage normal (uncomplicated) pregnancies, childbirth and the immediate postnatal period, and in the identification, management and referral of complications in women and newborns” [1]. In developing countries, SBA-attended deliveries increased from 56% in 1990 to 68% in 2012 [2]. Despite this effort, maternal mortality remains high, with an estimated 303 000 women dying in 2015. Most of these deaths are preventable and the majority occurred in low-resource settings [3].
In both high- and low-resource settings, simulation-based training is becoming a useful method of training healthcare providers in obstetrics and might prevent many of the maternal deaths [4]. “Helping Mothers Survive Bleeding After Birth” validated the use of a simulation training and showed immediate increase in knowledge, skills and confidence of healthcare workers in Tanzania [5]. Simulation training has successfully been used to train healthcare providers in Rwanda in obstetric emergencies. Homaifar et al. [6] showed practical skills retention by medical students in Rwanda after training. Nathan et al. [7] showed immediate improvement and subsequent retention of postpartum hemorrhage skills by generalist physicians in rural Rwanda. However, in rural Rwanda, nurses are frontline in the management of vaginal deliveries. They are essential in recognizing obstetrical complications, such us obstructed labor and postpartum hemorrhage.
Rwanda has made tremendous progress in maternal health with a decrease in maternal mortality ratio from 567 in 2005 to 290 per 100 000 live births in 2015, corresponding to a 6.7% annual rate of reduction. Post-partum hemorrhage and obstructed labor are the leading direct causes of maternal death in Rwanda, accounting for 22.7% and 12.3%, respectively, of all cases [8]. Additionally, hemorrhage accounts for 57% of maternal near misses at the district level in Rwanda [9]. Rwanda has 1 midwife per 8,600 births, a ratio far below the WHO recommendation of 1 SBA to every 175 pregnant women [10]. Their ability to quickly escalate care and provide the necessary prompt interventions is paramount to preventing mortality. For such reason, periodic skills evaluation with subsequent relevant education and training is necessary to maintain and enhance their skill set. Thus, the primary objective of this study was to evaluate the vaginal delivery (VD) and postpartum hemorrhage (PPH) skills of rural skilled-birth attendants (SBAs). The secondary objectives were to compare the VD and PPH skills of SBAs who previously participated in a simulation training in 2013 versus those who participated in 2014.
Materials and Methods
A simulation-based study was conducted in the Western Province of Rwanda with two convenient groups of SBAs who previously underwent a didactic and simulation training. The initial education training program, composed of didactics on normal labor and delivery and obstetric hemorrhage, was immediately followed by a simulation-based training of vaginal delivery (VD) and postpartum hemorrhage (PPH) utilizing the same scenario used in this study. A repeat simulation exercise to assess their communication, evaluation, and management skills in VD and PPH was conducted in September of 2015. The time to follow-up was 30 months for Group 1 and 18 months for Group.
The study protocol was approved by the ethics committee of the University Teaching Hospital of Kigali, University of Rwanda. The research was deemed exempt from full review by the Institutional Review Board of the Albert Einstein College of Medicine, NY, USA. All participants provided written informed consent to participate before the study began. Prior to beginning the simulation exercises, the participants completed both demographic and confidence questionnaires. The confidence questionnaire used five-point Likert scale to assess the participants’ confidence in their own vaginal delivery and postpartum hemorrhage knowledge and management skills. The participants then individually completed a simulated vaginal delivery and postpartum hemorrhage exercise. A local actress portrayed a “patient,” a actor portrayed a “nurse,” and a Rwandan obstetrics and gynecology resident physician assessed each participant’s performance. The “patient” sat crossed-legged, fully clothed on the bed, and had a mannequin pelvis in front of her at her feet. The “patient” and the mannequin appeared to be one “person” as local fabric covered her waist down to the mannequin. The “patient” controlled the release of blood from under the fabric.
The rater completed a skills-based checklist that was used to assess the performance of each participant during the simulation while blinded to the participants’ group assignment. Simulation exercises were performed in Kinyarwanda, one of the official languages of Rwanda, which is spoken by most native Rwandan. Tasks completed during the exercise, such as “obtaining vital signs” or “placing an intravenous catheter” were verbalized while the participant acted as if they were performing such tasks. Bimanual compression and uterine massage were performed directly on the mannequin. After completing the hands-on simulation skills, each participant received relevant feedback and had the opportunity to practice and perfect targeted skills. Subsequently, all participants participated in a hands-on vaginal laceration repair workshop and a didactic session on postpartum hemorrhage.
Skills were categorized into three performance areas: communication, evaluation, and management. Tasks completed correctly received one point each. Tasks not performed or performed incorrectly received zero points. The total skill scores were calculated by adding the points achieved during the exercises. A passing total skill score was set at ≥ 60% correct. Total skill scores were compared using two-sample t-test and passing skills cores were compared using Pearson’s chi-square test. SBA-confidence survey results were compared using twosample t-test. Statistical analyses were performed using SAS/ STAT version 9.3 (SAS Institute, Inc., Cary, NC) and p< 0.05 was considered statistically significant.
Result
A total of 26 SBAs participated in the study. Fourteen participants were in Group 1 (54%) and12 (46%) were in Group 2. Table 1 depicts the demographic characteristics and prior experience between the two groups of participants. The demographics and prior experience were statistically similar between the two groups, except that Group 2 reported working more years as a maternity ward nurse (p < 0.007).

aData are median (interquartile range) or n (%) unless otherwise specified
bA2 nurse completed seven years of secondary school training with a focus in nursing
cA1 nurse completed an additional three years of higher education.
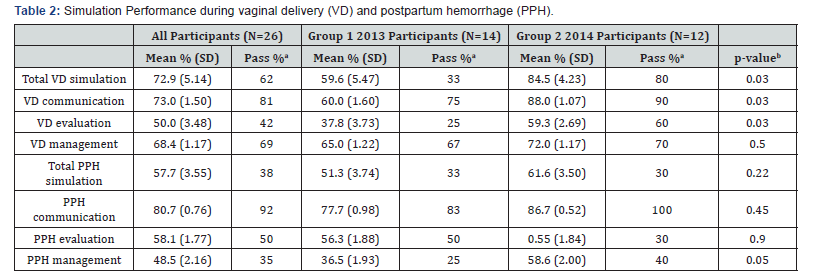
aCriterion reference pass score is ≥60% correct answers
bP-value for passing skills scores compared using Pearson’s chi-square test n, number; SD, Standard Deviation
The mean total skill score on the VD simulation was 72.9% for all participants (Table 2). Compared to Group 1, Group 2 obtained a significantly higher VD simulation skills mean score (84.5% vs. 59.6%, p = 0.03). The mean performance score for all participants was highest in the communication performance area (73.0%), followed by the management (68.4%) and evaluation (50.0%) areas. Sixty two percent of participants received a passing total skill score on the VD simulation exercise. Compared to Group 1, Group 2 obtained a statistically significant higher pass rate (80% vs. 33%, p=0.04).
The mean total score on the PPH simulation skills was 57.7% for all participants. Compared to Group 1, Group 2 had a higher PPH simulation skills mean score, but this was not statistically significant (61.6% vs. 51.3%, p=0.22). The mean performance score for all participants was highest in the communication performance area (80.7%), followed by the evaluation (58.1%) and management (48.5%) areas. The PPH simulation pass rate for all participants was 33%. There was no difference in the PPH simulation pass rate between the two groups (30% vs. 33%, p=1.00). The response rate for the confidence questionnaire was 100%. There was no difference in the mean SBA-confidence scores between the two groups (Table 3).
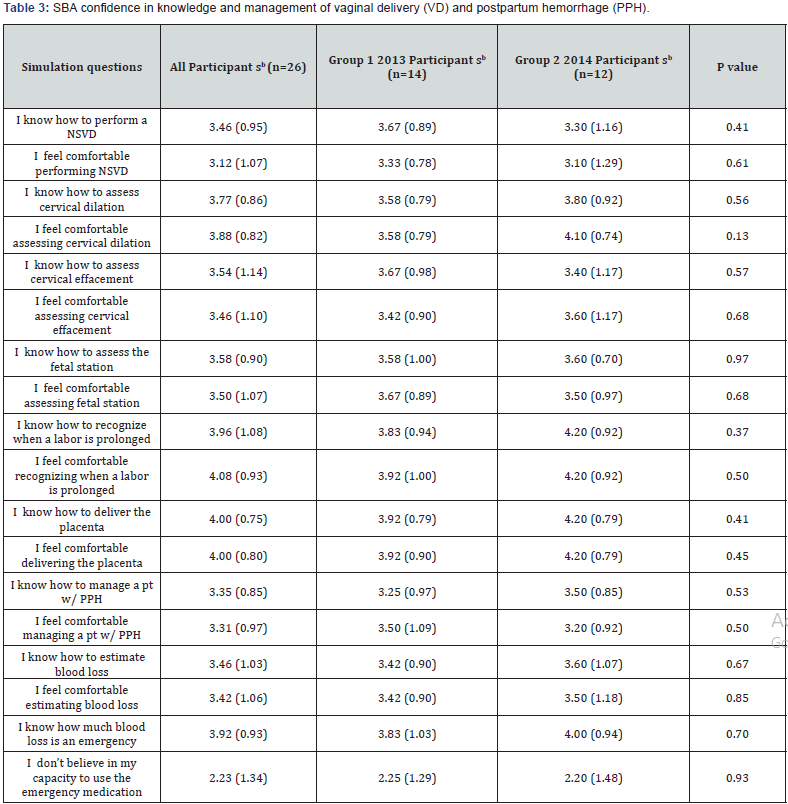
aValues are given as mean (SD) unless indicated otherwise
bConfidence measures were assessed using a 5-point Likert scale, where 1 = uncomfortable and 5 = extremely comfortable
Discussion
This follow-up simulation study conducted with SBAs in rural Rwanda showed that more recent training is associated with higher simulation scores. Overall, Group 2, with a follow-up time of 18 months, obtained higher simulation scores than Group 1, whose follow-up time was 30 months. To our knowledge, this is the first published practical simulation evaluation of SBA skills in the areas of vaginal delivery and postpartum hemorrhage in Rwanda that compares these skills based on two previous years of simulation training. Our study provides new insight on the effectiveness and optimal interval of simulation training in lowresource areas.
The SBAs obtained higher mean scores and passing rate during the vaginal delivery simulation skills than during the postpartum hemorrhage simulation exercise. The postpartum hemorrhage simulation passing rate was low, a result similar to those of Nelissen et al. [11] and Homaifar et al. [6] both of whom showed a low pass rate on a simulation skills test of learners after training. The pass rate likely reflects the level of competence of the participants. However, the ability of the skills checklist and the rater to accurately measure competency has not been studied. Other factors, such as timing between training sessions, limited experience with simulation, and the competency of previous facilitators could have influenced participant performance.
It is less likely that the participants confidence level affected their performance. They reported to be overall confident in and comfortable with both their VD and PPH knowledge and management skills. This study did not assess how their confidence changed overtime. Still, it found no statistically significant difference in confidence levels between those who previously underwent simulation training and education in 2013 versus those who participated in a similar training education in 2014. The study was not powered to assess the relationship between confidence levels and performance in the stimulation training. However, confidence levels do not appear to correlate with skills in obstetrics. Siassakos et al. [12] found no relationship between simulation performance and skill attitude. Nelissen et al. [11] showed that the increase in confidence of learners after training did not match the lack of improvement in their skills. Nathan et al. showed that confidence level decreased over time although skills were retained [7].
A strength of our study is that the participants were all nurses. They provide a good representation of the population of SBAs that manage labor and delivery and are first to encounter postpartum hemorrhage events in rural areas that necessitate prompt and appropriate management. Simulation participants of previously published studies in obstetrics have been either heterogeneous or focused on either generalist physicians or medical students. The nurses in our study possessed vast differences in clinical experience, volume and exposure to vaginal deliveries and postpartum hemorrhage, which likely are confounding variables in this study. However, such differences are inevitable and reflect the real world of SBAs. The fact that our study assessed competency long after the initial training is also a strength. This extended time period from training to repeat testing allowed SBAs to practice their skills and have more real-life experience with vaginal deliveries and postpartum hemorrhage.
Our study was limited by the number of participants, restricting the comparisons between groups. Without the participants’ baseline skills, we were neither able to assess skills retention nor determine if Group 2’s additional years as labor and delivery nurses provided the group with additional obstetrical skills, which could have led to better performance in the simulation. Moreover, this simulation was carried out in one region of Rwanda, limiting its generalizability. Importantly, our study was not randomized and instead was based on a convenient sample of willing participants who benefited from the education and training that followed the formal practical simulation evaluation.
Conclusion
The passing rate for postpartum hemorrhage simulation was low, which may indicate a need for more education and training of SBAs. The practical vaginal delivery skill set of SBAs in rural Rwanda appear to be greater 18 months after initial training compared to 30 months later, but confidence levels were the same. In the future, attempts should be made to randomize subjects to sessions and determine the optimal interval training.
Author contributions
Verόnica Maria Pimentel was involved in the planning and execution of the study, performed data entry, assisted with the data analysis and drafted and revised the manuscript.
Denis Rwab, MD was involved in the planning and execution of the study and revising of the manuscript.
John Gahima, MD was involved in the planning and execution of the study and revising of the manuscript.
Stephen Rulisa was involved in the design, planning and execution of the study and revising of the manuscript.
Xianhong Xie performed the data analysis for the study and assisted with the data interpretation and preparation of the manuscript.
Peter S. Bernstein was involved in the design and planning of the study and assisted with the manuscript preparation.
Lisa M. Nathan was involved in the design, planning and execution of the study and assisted with the manuscript preparation.
Acknowledgment
This study was in part funded by the Global Health Center at the Albert Einstein College of Medicine, Bronx, NY, USA. The authors would like to thank Damien Nsabimana and Barbra Mutamba for their support.
References
- World Health Organization (2004) Department of Reproductive Health and Research. Making pregnancy safer: the critical role of the skilled attendant. A joint statement by WHO, ICM and FIGO. Geneva, Switzerland, pp. 1-18.
- World Health Organization (2016) Standards for improving quality of maternal and newborn care in health facilities. p. 73.
- Alkema L, Chou D, Hogan D (2017) Global, regional, and national levels and trends in maternal mortality between 1990 and 2015, with scenario-based projections to 2030: a systematic analysis by the UN Maternal Mortality Estimation Inter-Agency Group. Lancet 387(10017): 462-474.
- Crofts J, Winter C, Sowter M (2011) Practical simulation training for maternity care-where we are and where next. BJOG 118(suppl 3): 11- 16.
- Nelissen E, Ersdal H, Mduma E, Evjen-Olsen B, Jacqueline B, et al. (2015) Helping Mothers Survive Bleeding After Birth: retention of knowledge, skills, and confidence nine months after obstetric simulation-based training. BMC Pregnancy Childbirth 15(1): 190.
- Homaifar N, Mwesigye D, Tchwenko S, Worjoloh A, Joharifard S, et al. (2013) Emergency obstetrics knowledge and practical skills retention among medical students in Rwanda following a short training course. Int J Gynecol Obs 120(2): 195-199.
- Nathan LM, Patauli D, Nsabimana D, Bernstein PS, Rulisa S, et al. (2016) Retention of skills 2 years after completion of a postpartum hemorrhage simulation training program in rural Rwanda. Int J Gynecol Obstet 134(3): 350-353.
- Sayinzoga F, Bijlmakers L, Dillen JV, Mivumbi V, Ngabo F, et al. (2016) Maternal death audit in Rwanda 2009-2013: a nationwide facilitybased retrospective cohort study. BMJ Open 6(1): 1-8.
- Kalisa R, Rulisa S, Akker VDT, Roosmalen VJ (2016) Maternal Near Miss and quality of care in a rural Rwandan hospital. BMC Pregnancy Childbirth 16(1): 324.
- Black WHOC (2011) Save Lives: Invest in Midwives Knowledge Summary: Women’s and Children’s Health pp. 1-4.
- Nelissen E, Ersdal H, Østergaard D, Mduma E, Broerse J, et al. (2014) Helping mothers survive bleeding after birth: An evaluation of simulation-based training in a low-resource setting. Acta Obstet Gynecol Scand 93(3): 287-295.
- Sissako D, Draycott TJ, Crofts JF, Hunt LP, Winter C, et al. (2010) More to teamwork than knowledge, skill and attitude: General obstetrics. BJOG 117(10): 1262–1269.






























