A Rare Ovarian Tumor: Granulocytic Sarcoma-Case Report
Funda Atalay1*, Nazan Bozdoğan2 and Hanife Sağlam3
1Department of Gynecological Oncology Surgery, Ankara Oncology Education and Resarch Hospital, Turkey
2Department of Pathology, Ankara Oncology Education and Resarch Hospital, Turkey
3Department of Gynecology, Ankara Oncology Education and Resarch Hospital, Turkey
Submission: July 27, 2018; Published: August 06, 2018
*Corresponding author:Funda Atalay, Department of Gynecological Oncology Surgery, Ankara Oncology Education and Resarch Hospital, Turkey, Email: atalayfundak@yahoo.com
How to cite this article: Salwa samir anter. Local Application of Propranolol and Treatment of Diabetic Vulovagnitis. J Gynecol Women’s Health. 2018: 11(1): 555802. DOI: 10.19080/JGWH.2018.11.555802
Abstract
Background:Granulocytic sarcoma is a hematological malignancy of myeloblasts or immature myeloid cells that hold an extramedullary anatomical region. Granulocytic sarcoma in the gynecologic tract is very rare.
Case report:At the age of 51 years, a left adnexial mass was detected during the follow-up of a patient who had no known hematologic disease story and who had breast cancer surgery and adjuvant treatment two years ago. Peritonitis carcinomatosis was observed during the operation and optimal debulking was performed. In the large immunohistochemical panel, tumoral cells were widely stained with myeloperoxidase, CD34, C-kit and CD43; was focally stained with CD68 and granulocytic sarcoma was diagnosed. The patient developed small bowel perforation in the early postoperative period and reoperated. Then she was diagnosed with acute myeloid leukemia (AML) by the hematologic department because of poor hematologic status postoperatively. Due to worsening of the general condition, the patient died before the planned bone marrow biopsy was performed.
Conclusion:In conclusion, primary ovarian granulocytic sarcoma is one of the rare presentation forms of AML. In order to distinguish ovarian granulocytic sarcoma from malignant lymphoma and granulosa cell tumor, it is first strongly suspected and appropriate immunohistochemical markers should be examined to confirm the diagnostic granulocytic sarcoma.
Keywords: Granulocytic sarcoma; Breast; Ovarian; Hematologic status
Abbrevations: AML: Acute Myeloid Leukemia
Introduction
Granulocytic sarcoma is a hematological malignancy of myeloblasts or immature myeloid cells that hold an extramedullary anatomical region. This neoplasm is in the literature; myeloid sarcoma, extramedullary myeloid cell tumor, myeloblastoma, chloroma. These tumors rarely occur in any anatomical region without known hematolymphoid disease. Granulocytic sarcoma in the gynecologic tract is very rare [1].
Case Presentation
In this presentation; we aimed to discuss the case of granulostatic sarcoma due to overt tumor, which is not a hematologic disease, in the context of literature information. At the age of 51 years, a left adnexial mass was detected during the follow-up of a patient who had no known hematologic disease story, who had two years ago breast cancer surgery and adjuvant treatment. The left adnexal area of the captured tomography showed a mass of 90 x 82 x 68mm and ascites in the abdomen [2]. Peritonitis carcinomatosis was observed during the operation and optimal debulking was performed. Total abdominal hysterectomy and left salfingooferectomy material, peritoneum, omentum, bilateral iliac, obturator, paraaortic lymph nodes and abdominal fluid were evaluated after the right salphingooferectomy material was sent to the frozen section. The typical macroscopic appearance was of the right salphingooferectomy material. On the macroscopic examination of this sample, oophorectomy material measuring 10x9.5x6.5cm containing tuba length of 9.5cm was observed. When the overlying tissue was cut, it was seen to be composed of a solid greenish color lesion. Other materials consisted of areas consistent with solid, irregular tumor infiltration. Microscopically, a solid diffuse tumoral lesion infiltrating bilateral ovaries, peritoneum and omentum and all pelviperitoneal lymph nodes was observed. Tumor cells were immature character with vesicle nucleus with narrow cytoplasm. In the large immunohistochemical panel, epithelial, melanocytic, lymphoid and plasmacytoid tumors were excluded because of the lack of staining with Pan CK, -S- 100, LCA, CD138. Tumoral cells were found to exhibit focal staining with CD68, widely stained with Myeloperoxidase, CD34, Ckit and CD43 (Figure1 & 2). On this basis, the specimens of the mammary tissue which had been previously diagnosed were examined again and it was seen that the hematoxylin & eosin and the immunohistochemical evaluation performed on the material were similar to the ovarian tumor. With these findings, it was decided that granulocytic sarcoma was present in the tumor of the breast that was previously diagnosed as invasive lobular carcinoma [3]. The patient developed small bowel perforation in the early postoperative period and reoperated. Hematology department was consulted for postoperative haematological problems. A peripheral-sided flow cytometry examination was performed on a patient suspected of acute myeloid leukemia (AML) in peripheral spread, and AML was diagnosed on detection of blast cells in flow cytometric examination. Due to worsening of the general condition, the patient died before the planned bone marrow biopsy was performed [4].
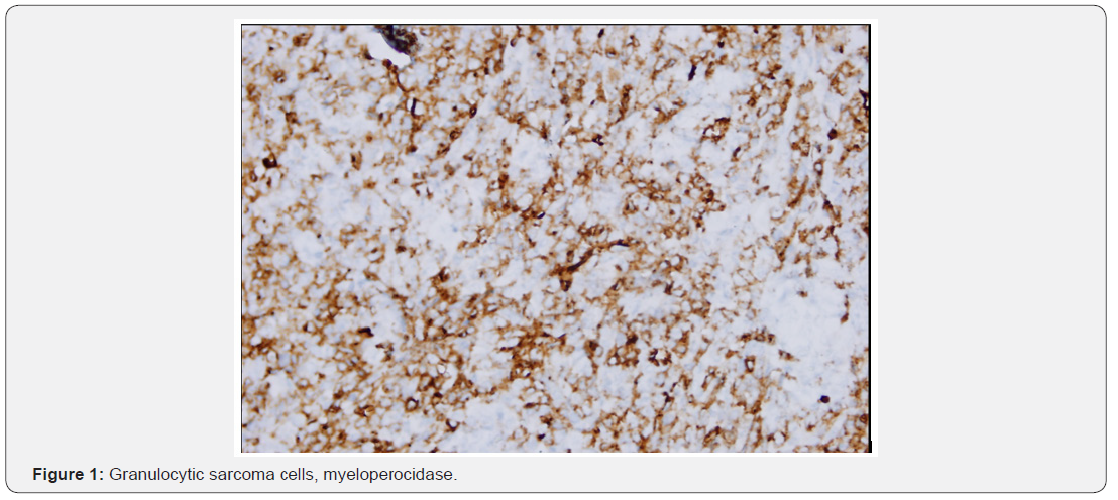
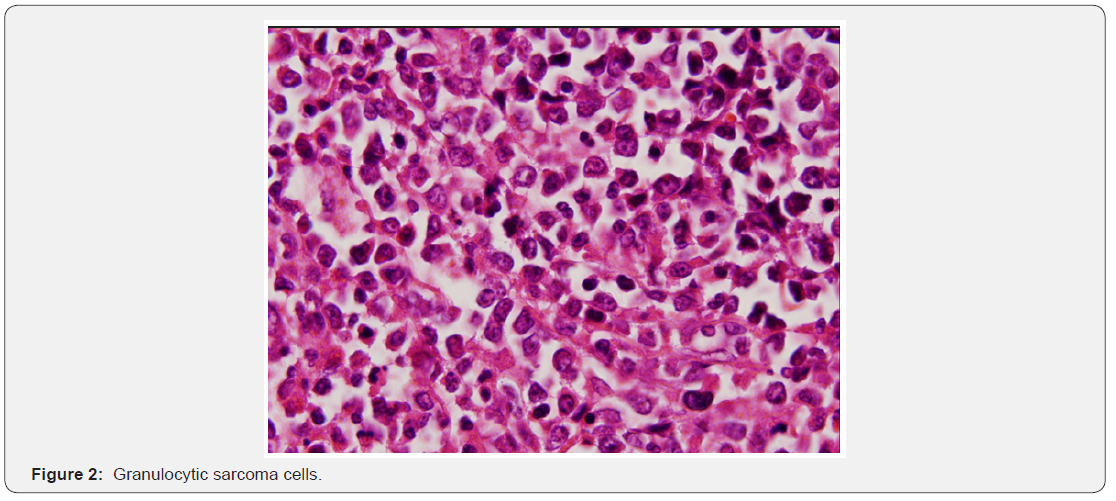
Discussion
Granulocytic sarcoma can be seen at any anatomic location. Gynecologic tract involvement is very rare and approximately 80 cases have been reported in different articles in the literature. Twenty-six cases were reported as isolated masses. AML development was reported between 8 days and 28 months (mean 7.4 months) in patients with granulocytic sarcoma without myeloid neoplasia [5].
In our case, although the diagnosis was made within 1 month after the operation, the general condition of the patient was poor and the patient died before the hematologic medical treatment started. However, when the patient’s ovarian mass was identified as granulocytic sarcoma, the time between the first operation and the detection of AML was over two years when the previous breast operation was reassessed pathology and it was originally thought to be granulostatic sarcoma. The fact that granulostatic sarcoma can occur in any anatomic localization in the form of an isolated mass without primary myeloid neoplasia or a history of the tumor makes it very important to perform differential diagnosis with tumors with similar histomorphologic features. Neiman and colleagues reported that only 44% of these cases were correctly diagnosed at the time of 61-year GS series, especially malignant lymphoma or sarcoma in cases of only isolated tumoral mass before leukemia [6,7].
Conclusion
primary ovarian GS is one of the rare presentation types of AML and can be easily misdiagnosed when examining H&E based sections. In order to distinguish ovarian granulostatic sarcoma from malignant lymphoma and granulosa cell tumor, it is first strongly suspected and appropriate immunohistochemical markers should be examined to confirm the diagnostic granulocytic sarcoma.
References
- Oliva E, Ferry JA, Young RH, Prat J, Srigley JR, et al. (1997) Granulocytic sarcoma of the female genital tract: a clinicopathologic study of 11 cases. Am J Surg Pathol 21(10): 1156-1165.
- Ding J, Li H, Qi YK, Wu J, Liu ZB, et al. (2015) Case Report: Ovarian granulocytic sarcoma as the primary manifestation of acute myelogenous leukemia. Int J Clin Exp Pathol 8(10): 13552-13556.
- Nigam JS, Misra V, Kumar V, Varma k (2012) Aleukemic granulocytic sarcoma presenting at multiple sites: ovary, breast and soft issue. Rare Tumors 4(3): e36.
- Garcia MG, Deavers MT, Knoblok RJ, Chen W, Tsimberidou AM, et al. (2006) Myeloid sarcoma involving the gynecologic tract: a report of 11 cases and review of the literature. Am J Clin Pathol 125(5): 783-790.
- Açıkalın A, Bağır E, Karabağ S, Gümürdülü D, Ergin M, et al. (2014) Cervical Granulocytic Sarcoma Without Bone Marrow Infiltration. Cukurova Medical Journal 39(1): 169-174.
- Neiman RS, Barcos M, Berard C, Bonner H, Mann R, et al. (1981) Granulocytic sarcoma: a clinicopathologic study of 61 biopsied cases. Cancer 48(6): 1426-1437.
- Harris NL, Scully RE (1984) Malignant lymphoma and granulocytic sarcoma of the uterus and vagina. A clinicopathologic analysis of 27 cases. Cancer 53(11): 2530-2545.






























