Detection of HPV E6/E7 Mrna Using Nuclisens Easyq HPV™ in AbnormalCytology Specimens
Ozer Birge*
Osmaniye state hospital, Turkey
Submission: June 01, 2018; Published: July 17, 2018
*Corresponding author: Ozer Birge, Osmaniye state hospital, Osmaniye, Turkey, Tel: 00905542267192; Email: ozbirge@gmail.com
How to cite this article: Ozer Birge. Detection of HPV E6/E7 Mrna Using Nuclisens Easyq HPV™ in AbnormalCytology Specimens. J Gynecol Women’s Health. 2018: 10(3): 555794. DOI: 10.19080/JGWH.2018.10.555794
Abstract
Objective: To analyze HPV E6/E7 mRNA (16, 18, 31, 33, 45) ratios in patients with abnormal smear cytology and to evaluate its efficiency in detecting CIN lesions.Material and method: All cases with abnormal cytologies described by Bethesda System and obtained via conventional pap smear in Celal Bayar University, Manisa maternity hospital and KETEM are included in this study. By evaluating these cases, Nuclisens EasyQ HPV E6/E7 mRNA (16, 18, 31, 33, 45) test is applied. This test is carried out in the microbiology laborotory of Celal Bayar University. The data concerning demographic and clinical features of the cases with HPV E6/E7 mRNA positivity and negativity are recorded. The factors affecting the positivity of HPV E6/E7 mRNA are evaluated. The cases with abnormal cytology are managed according to the ASCPP guideline. The sensitivity, specificity, positive and negative predictive values of HPV E6/E7 mRNA test are calculated after the diagnosis of CIN. Chisquare and Mc Nemar tests are used for the rest of statistical analyses.
Result:HPV E6/E7 mRNA was found to be positive in 55.3% of the cases with abnormal cytology. Furthermore, it was positive in 92.8% of HGSIL, 100% of ASC-H, 100% of AGC-NOS and 27.6% of ASC-US cases. In cases with abnormal cytology, HPV type 16 (%38.6) is isolated most commonly, HPV type 18 being the second (%24.6). Regarding the age, parity, number of sexual partners and contraceptive methods, there was no significant difference between HPV E6/E7 mRNA positive and negative cases, whereas positive HPV E6/E7 mRNA was significantly higher in smokers. In respect of detecting CIN, the sensitivity was found to be 100%, specificity 27%, positive predictive value 27% and negative predictive value 100%. Any case with CIN was established if there was negative result of HPV type 16, 18, 31, 33, 45 E6/E7 mRNA test with abnormal smear cytology.
Conclusion:approximately in half of cases with abnormal cytology, HPV E6/E7 mRNA was positive. Furthermore, it was more prominent with cases except ASC-US. The high sensitivity and low false negative ratios make the HPV E6/E7 mRNA test to become efficient in clinical use.
Keywords: Smear; Cytology; Human papilloma virus; mRNA; E6/E7 protein
Introduction
Cervical cancer is the third most common cancer in women worldwide. About 530.000 women get the diagnosis of cervical cancer each year and about 275.000 of them die because of the disease [1]. Infection with high-risk human papilloma virus (HPV) is the most important factor in the etiology of cervical cancer [2]. About 15HPV types are accepted to be high risk, however, HPV types 16,18,31,33 and 45 are most commonly detected in cervical cancer cases [3]. HPV causes infection in 75% of women during their life. Only 10-15% of HPV infections lead to cervical lesions. The factors affecting the HPV infection persistence are not exactly known, however, HPV type, smoking, concomitant sexually transmitted diseases, immune suppression may play important role [1,2].
At the present time, most commonly used HPV detection tests are DNA-based assays. They give data about the presence or absence of the high-risk virus. As all the infections with the high-risk types do not persist and do not cause cervical lesions progressing to cervical cancer, the problem is that we have higher sensitivity, lower specificity and lower positive predictive values for the prediction of cervical intraepithelial lesion with HPV DNA assays [3].
Viral oncoproteins E6 and E7 of HPV are the basic proteins responsible for the cellular transformation. E6 and E7 inactivate p53 and Rb tumor suppression genes, respectively. Disruption of p53 and Rb tumor suppressor pathways causes the loss of cell cycle growth control by the abnormal entry of S-phase [4]. Therefore, the detection of E6-E7 mRNA of high risk HPV types may be more reasonable to establish the associated cervical intraepithelial lesions with higher positive predictive values and higher specificity.In this study, we aimed to analyze HPV E6/E7 mRNA (16,18,31,33,45) ratios in patients with abnormal smear cytology with the use of NucliSENS Easy QHPV and to evaluate its efficiency in detecting CIN lesions.
Methods and Materials
The patients with abnormal cytology who were admitted to the department of gynecology at Celal Bayar University and Manisa Maternity Hospital between June 2011 and February 2012. Ethical approval for the study was obtained from the Research Ethics Committee at Celal Bayar University. All cytologic smears were evaluated by a specialised cytopathologist (ARK). The classification and diagnosis of cytology was made by Bethesda System. The cases with normal cytologic diagnosis were excluded from the study group. The abnormal cytological diagnosis were classified in atypical squamous cells of undetermined significance (ASC-US), low grade squamous intraepithelial lesion (LSIL), high grade squamous intraepithelial lesion (HSIL). Histological evaluation for the cases of abnormal cytologies except ASC-US lesions was also made following colposcopy and cervical biopsy.
The data including age, gravidity, parity, contraceptive methods, smoking, and number of sexual partners was recorded. The swab samplesfor HPV E6/E7 mRNA test were obtained from ecto- and endocervix of patients with abnormal cytologic results via cervibrush (SZ Wholesale Center,China). The brush was taken in viral transport liquid medium for one minute and thereafter they were sent to the laboratory of microbiology department for the evaluation of HPV E6/E7 mRNA testing. The samples were preserved at the temperature of -20°C until the test day. In order to detect high risk HPV E6/E7 mRNA, a Nucleic Acid Sequence Based Amplification system (NucliSENS EasyQ HPV™; bioMérieux, France) is used. In this system, single stranded oligonucleotide probes with 3’-5’ endings having fluorophore and inhibitor molecules and being complemantory to each other and with the remaining parts complementory to the amplified target are used. By the hybridization with the target molecule, the secondary structure of the probe opens and the signal of the fluorophore is detected by the system via elimination of the inhibitor effect. According to the producter’s comments, for each sample, three different mixture was prepared with each of them containing 2 primary and 1 probe (U1A/HPV16, HPV 33/45 and HPV 18/31) and the amplification signals were being detected simultaneously for 2.5 hours at 41°C. The results were evaluated by EasyQ™ analysis software.
The women with abnormal cytological results except ASC-US were evaluated by colposcopy and cervical biopsy. The biopsy samples were analyzed in the pathology department. According the histopathological results, the treatment and follow-up modalities were determined. The data analysis was evaluated by SPSS (15.0 Statistical Package for Social Sciences). Chi-square and Mc Nemar tests are used for the statistical analyses. The sensitivity, specificity, positive and negative predictive values of HPV E6/E7 mRNA tests were calculated after the diagnosis of CIN.
Result
The study consists of 103 women with abnormal cervical cytologic diagnosis. The mean age of patients was 40.82 10.4 (range 21-67 years). Among the patients, 20(19.4%) were younger than 30 years of age. The mean gravidity and parity were 3.39 1.4 and 2.39 1.2, respectively. The ratio of women using combined oral contraceptives was 12.6%. Approximately 46% of the patients were smokers and 78.6% of them had single sexual partner. The main demographic findings are demonstrated in Table 1. The flow chart regarding the triage of the study population is shown in Figure 1. Most common abnormal cytology was ASC-US, followed by LSIL, HSIL, ASC-H and AGC-NOS (45.6%, 35.9%, 13.6%, 3.9% and 1%, respectively).

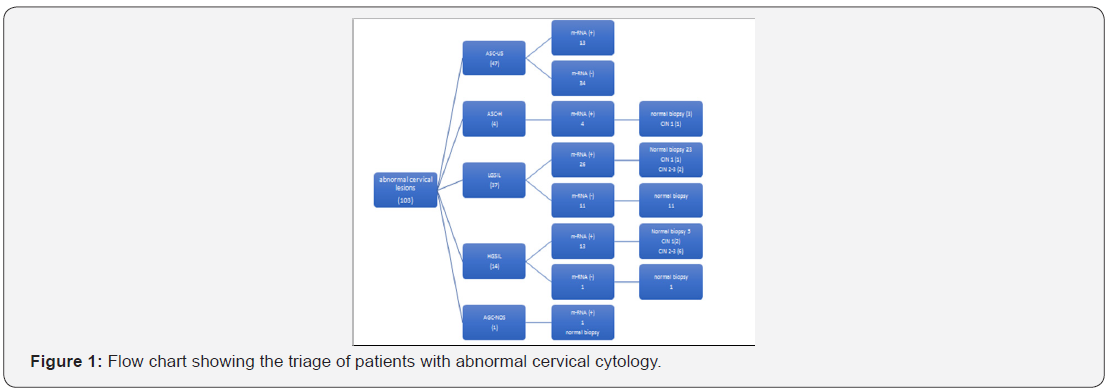
Fifty-seven (55.3%)of the patients with abnormal cytology had HPV E6/E7 mRNA positivity. HPV E6/E7 mRNA was found to be positive in 13 of 47 ASC-US cases (27.6%), 26 of 37 LGSIL cases (70.2%), 13 of 14 HGSIL cases (92.8%), 4 of 4 ASC-H cases (100%) and 1 case of AGC-NOS (100%) (Table 2). The rates of HPV E6/E7 mRNA positivity were significantly higher in ASC-H, LGSIL and HGSIL lesions compared that in ASC-US (p<0.05) (Table2).

Regarding all HPV E6/E7 mRNA positive cases (n=57), 38 of them (36.9%) had infection with single viral type, 14 of them (13.6%) infected with concomitant 2 viral types and 5 of them (4.9%) infected with concomitant 3 viral types. The most isolated viral type was HPV type 16 with 22 cases (38.6%), type 18 being the second most common with 14 cases (24.6%). HPV type 32 was only in 2 cases (3.5%) positive. HPV type 33 and 45 were not isolated as single etiologic factor. Regarding the concomitant infections, the most common form was with HPV type 16 and 18 in 17.5% of cases. Coexistence of type 16,18 and 31 was the second most common co-infection (Table 3).
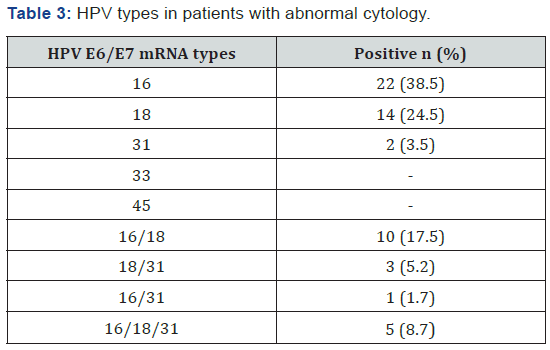
Twelve (92.3%) of 13 HPV E6/E7 mRNA positive cases among 47 ASC-US patients had type 16 and type 18 HPV. Only one of them was infected with type 31. HPV E6/E7 mRNA positivity was detected in all of the ASC-H cases, 2 of them had type 18 and the other 2 had type 16 and type 31 infection. Regarding HPV mRNA positive LGSIL cases, 11(42.3%) of them had type 16,5(19.2%) of them had type 18 infection. 5 patients (19.2%) had co-infection with type 16 and 18, 2(7.6%) patients had type 16,18 and 31 co-existence. One (3.8%) of them was co-infected with type 16 and 31. Regarding 13 HPV E6/E7 mRNA positive HGSIL patients, 3 of them (23%) had type 16 and 1(7.6%) of them had type 18 infection. 5 cases (38.4%) had co-infection with type 16 and 18, 3 cases (23%) type 16,18 and 31. Type 18 and 31 co-infection was found in one of HGSIL patients (Table 3).

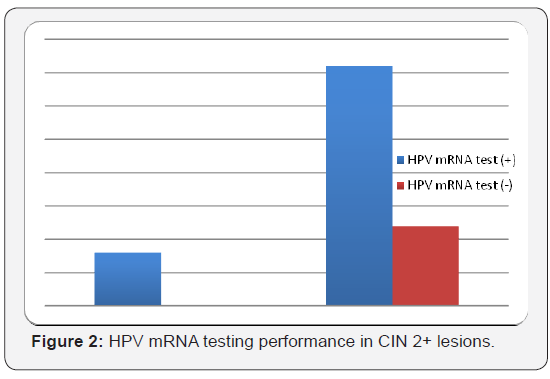
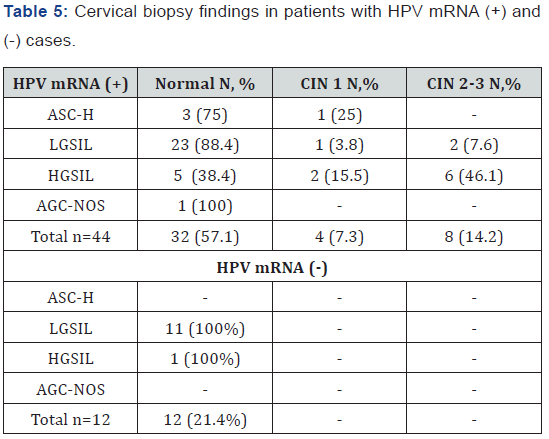
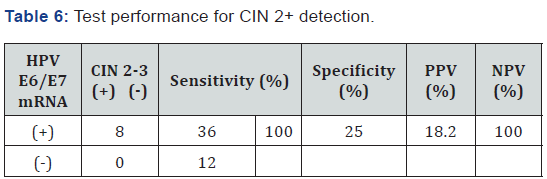
The colposcopy-guided cervical biopsy findings of HPV E6/ E7 mRNA positive cases that have cervical lesions higher than ASC-US are shown in Table 4. CIN was detected in 12(21.4%) of 56 cases. Among 44 patients with HPV E6/E7 mRNA positive results, 8(18.2%) had high grade cervical lesions such as CIN 2 and CIN 3 (Figure 2). However, in HPV mRNA negative cases, there was not any abnormal biopsy findings. Regarding these findings, the sensitivity, specificity, positive predictive value (PPV) and negative predictive value (NPV) of the HPV E6/E7 mRNA NucliSENS EasyQ HPV™ testing of CIN 2+ lesions are calculated (Table 5 & 6). The sensitivity of the test for CIN 2+ lesions was 100%, the specificity 25%, PPV 18.2% and accuracy was 35.7%.
Discussion
Cervical cancer is still a major health problem with being second most common cancer among women in undeveloped countries without any national screening program. Unfortunately, 500.000 women die because of cervical cancer worldwide every year [5]. With regular screening programs, cervical cancer has been the 6th most common cancer in women in developed countries.
Cervical cancer is still a major health problem with being second most common cancer among women in undeveloped countries without any national screening program. Unfortunately, 500.000 women die because of cervical cancer worldwide every year [5]. With regular screening programs, cervical cancer has been the 6th most common cancer in women in developed countries.
Pap smear has been used for the detection of preinvasive lesions. However, false negative values of 20-50% of a pap smear lead the researchers to find supplementary methods to increase the accuracy [8]. In recent years, screening for HPV virus has become the interest of investigations. HPV DNA tests show the presence or absence of the virus; however, the potential of progression to invasive cancer, the probability of concomitant preinvasive lesion can not be predicted by the viral DNA assays. Furthermore, lesions that will regress spontaneously are diagnosed and ‘over-treatment’ is made. By this way, the detection of HPV E6/E7 mRNA proteins seems to be more reasonable, as the E6/E7 proteins are responsible for oncogenic transformation [9,10].
In present study, the overall high risk HPV mRNA positivity rate in patients with abnormal cervical cytology was 55.3%. The ratio of positive HPV E6/E7 mRNA results was evaluated in a study by Halfon consisting of 140 abnormal cytology results revealing that 46% of abnormal smears had positive HPV E6/ E7 mRNA [11]. A greater study by Sorbye from north Norway including 1798 minor cervical lesions concluded that 18% of patients (n=327) had positive HPV E6/E7 mRNA [12].
The analysis of 3085 invasive cervical carcinomas by the International Agency for Research on Cancer (IARC) showed that the most common HPV genotypes were HPV 16, 18, 45, 31 and 33 [11]. In our study, these genotypes were found in 55.3% of cases. Similarly, the most common HPV type was HPV 16, with HPV 18 being the second most common (Table 3). HPV 33 and 45 genotypes were not detected in our study.
HPV E6/E7 mRNA levels are well matched to the clinical manifestations compared to HPV DNA and viral load detection [9]. High HPV E6/E7 mRNA levels are found to be correlated to the bad prognosis in patients with cervical invasive cancer. However, there was no correlation between HPV E6/E7 mRNA levels and viral load [10,13]. Regarding these results, it can be postulated that the tests for detection of HPV E6/E7 mRNA levels are well correlated with the severity of cervical abnormality with great potential of cervical cancer prediction [14].
Regarding the follow-up period after the treatment of cervical preinvasive lesions, Trope at all performed a study with patients having CIN 2 or more severe lesions treated with coldknife conisation. To detect the residual lesion after conisation, HPV E6/E7 mRNA test with a sensitivity of 45% (95% CI, 26.8- 65.5%) was found to be unsuitable in the follow-up management [15]. However, more studies are needed for accurate data.
We found the sensitivity of the HPV E6/E7 mRNA test 100%, specificity 25%, positive predictive value 18.2% and negative predictive value 100%. Regarding Halfon`s study, the sensitivity was 76% with a specificity 63%, positive predictive value 50% and negative predictive value 84% [11]. Similarly, Sorbye’s study suggested the sensitivity of the HPV mRNA test for moderate to severe dysplasia as 81%. The specificity was 91%. The sensitivity and specificity regarding CIN 3 lesions were 84% and 88%, respectively [12]. The sensitivity level seems to be high in both studies. All of the patients having CIN lesions in our study had positive HPV E6/E7 mRNA test and none of the patients having negative HPV E6/E7 mRNA test had any CIN lesions. The negative test result for the HPV E6/E7 mRNA seems to be more precious.
Conclusion
our preliminary results show that mRNA testing may be a good marker for the prediction of high grade cervical preinvasive lesions and cervical cancer, however further data are needed to confirm these results.
References
- Arbyn M, Raifu AO, Autier P, Ferlay J (1904) Source Scientific Institute of Public Health, Brussels, Belgium.
- Chen HC, Schiffman M, Lin CY, Pan MH, You SL, et al. (2011) Persistence of type-specific human papillomavirus infection and increased longterm risk of cervical cancer. J Natl Cancer Inst 103(18): 1387-1396.
- Dixon EP, King LM, Adams MD, Grønn P, Murphy PG, et al. (2008) Isolation of RNA from residual BD SurePathTM liquid-based cytology specimens and detection of HPV E6/E7 mRNA using the PreTect TM HPV-Proofer assay. J Virol Methods 154 (1-2): 220-222.
- Malinowski DP (2005) Molecular diagnostic assays for cervical neoplasia: emerging markers for the detection of high-grade cervical disease. Biotechniques 38(Suppl 1): S17-S23.
- Franco EL, Duarte-Franco E, Ferenczy A (2001) Cervical cancer: epidemiology, prevention and the role of human papillomavirus infection. Can Med Assoc J 164(7): 1017-1025.
- McMeekin DS, McGonigle KF, Vasilev SA (1997) Cervical cancer prevention: Toward cost-effective screening. 1(2): (13 screens).
- Andersson S, Hansson B, Norman I, Gaberi V, Mints M, et al. (2006) Expression of E6/E7 mRNA from ‘high risk’ human papillomavirus in relation to CIN grade, viral load and p16INK4a. Int J Oncol 29(3): 705- 711.
- Boer DMA, Jordanova ES, Kenter GG, Peters AA, Corver WE, et al. (2007) High human papillomavirus oncogene mRNA expression and not viral DNA load is associated with poor prognosis in cervical cancer patients. Clin Cancer Res 13(1): 132-138.
- Halfon P, Benmoura D, Agostini A, Khiri H, Martineau A, et al. (2010) Relevance of HPV mRNA detection in a population of ASCUS plus women using the NucliSENS EasyQ HPV assay. J Clin Virol 47(2): 177- 181.
- Sorbye SW, Fismen S, Gutteberg TJ, Mortensen ES (2010) HPV mRNA test in women with minor cervical lesions: experience of the University Hospital of North Norway. J Virol Methods 169(1): 219-222.
- Wang-Johanning F, Lu DW, Wang Y, Johnson MR, Johanning GL, et al. (2002) Quantitation of human papillomavirus 16 E6 and E7 DNA and RNA in residual material from Thin Prep Papanicolaou tests using realtime polymerase chain reaction analysis. Cancer 94(8): 2199-2210.
- Lie AK, Kristensen G (2008) Human papillomavirus E6/E7 mRNA testing as a predictive marker for cervical carcinoma. Expert Rev Mol Diagn 8(4): 405-415.
- Tropé A, Jonassen CM, Sjøborg KD, Nygård M, Dahl FA, et al. (2011) Role of high-risk human papillomavirus (HPV) mRNA testing in the prediction of residual disease after conisation for high-grade cervical intraepithelial neoplasia. Gynecol Oncol 123(2): 257-262.






























