An Endometriosis Invading Uterus that Mimics a Degenerating Uterine Leiomyoma
Sul Lee, Byung Kyoo Park and Jong Kil Joo*
Department of Obstetrics & Gynecology, Pusan National university Hospital, Korea
Submission: September 17, 2017 ; Published: October 02, 2017
*Corresponding author: : Jong Kil Joo, Department of Obstetrics and Gynecology, Pusan National University School of Medicine, 179 Gudeko-ro, Seo- Gu, Busan-si, 49241 Korea, Tel : +82-51-240-7287; Fax: +82-51-248-2384; Email: jongkilj@hanmail.net
How to cite this article: Sul L, Byung K P, Jong K J. An Endometriosis Invading Uterus that Mimics a Degenerating Uterine Leiomyoma. J Gynecol Women's Health 2017; 7(1): 555705. DOI: 10.19080/JGWH.2017.6.555705
Abstract
Endometrioma is usually easily detected by ultrasound. In this case, women who were suffering from severe abdominal pain were diagnosed with secondary degeneration of uterine leiomyoma with ultrasound and computed tomography. Endometriosis was confirmed after histopathological examination from diagnostic surgery. Magnetic resonance imaging has a role in differentiation of leiomyoma second degeneration and endometriomas
Keywords: Endometriosis; Leiomyomas; Ultrasound; Magnetic resonance imaging
Introduction
Endometriosis is defined as the presence of endometrial tissue outside uterus. The most common sites of implantation are the pelvic viscera and peritoneum. Endometriosis should be suspected in women with subfertility, dysmenorrhea, dyspareunia, or chronic pelvic pain. The diagnosis should be confirmed by visual inspection during laparoscopy and by histologic confirmation of endometriosis in biopsied lesion [1]. Some patients with endometriosis will form cysts, termed endometriomas, which are found in up to 44% of women with endometriosis [2]. Endometriomas are usually readily detectable by ultrasound (USG). Cystic lesion with diffuse low- level internal echoes, sometimes described as "ground glass”, are characteristic, with 95% of endometriomas having this appearance [3]. However, in case of distorted pelvic anatomy or accompanying with infection, it could be misdiagnosed by conventional radiologic diagnostic method. We report a case of endometriosis that treatment was delayed due to misdiagnosed as leiomyoma after USG and computed tomography (CT) examination.
Case Report
A 27-year-old nulliparous woman was transferred to our hospital with severe chronic pelvic pain after several weeks of symptomatic treatment at local hospital.
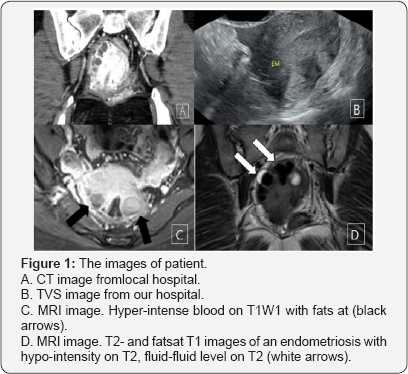
Three month ago the patient visited local hospital due to abnormal uterine bleeding (AUB) and underwent dilation and curettage (D&C). After D&C, she took oral contraceptives (OCs) for control AUB. During OCs medication, severe pain was occurred and she was admitted to the hospital. The laboratory finding shows elevated C-reactive protein (CRP), leukocytosis, and contrast-enhanced CT scan of the chest and abdomen revealed enteritis, and inflammatory lesions and leiomyoma with secondary degeneration in posterior wall of uterus (Figure 1A). The size of leiomyomas was up to 4.3cm. Antibiotics and non-steroid anti-inflammatory drug (NSAID) were administered. However, pelvic pain was not improved and she was transferred to our hospital.
Five years ago, she underwent a laparoscopic surgery due to ovarian endometrioma and no other specific medical, surgical or familial history was identified. She has regular menstrual cycle with severe dysmenorrhea.
The laboratory findings of our hospital were as following. A blood test showed the white blood cell was 6,460/uL and the hemoglobin and hematocrit level were 10.7g/dL and 30.7%, respectively. The CRP was 2.20mg/dL and the cancer antigen 125 was 146.8U/mL. The blood cultures for bacterial growth showed nothing. All other laboratory finding was within normal range.
Transvaginal ultrasound (TVS) showed multiple hypoechoic lesions in the posterior surface of uterus (Figure 1B). Despite the use of antibiotics, symptom did not improve. So Contrast- enhanced magnetic resonance image (MRI) of the pelvis was checked and radiologist reported an endometriosis involving uterus with combined infection (Figure 1C & 1D).
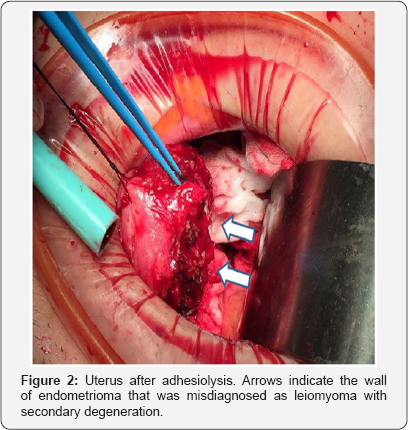
Explolaparotomy was done (Figure 2). Cul-de-sac was unable to be spotted because of severe adhesion between posterior uterus wall and pelvis. After adhesiolysis, a typical form of endometriosis, chocolate fluid trapped in adhesion, came out on such spot. Also, we could find multiple endometriotic spots in the pelvis. After complete adhesiolysis, uterus was repaired to normal shape. All of the excised parts were diagnosed to an endometriosis by histological examination. After the surgery, the patient recovered well and was discharged without pain and treated by a gonadotropin-releasing hormone agonist for 6 months. Endometriosis was not observed in the follow-up ultrasound performed in the outpatient clinic. She is currently doing well.
Discussion
Endometriosis is a common benign disease that can develop anywhere, especially pelvic cavity.
The classic sonographic appearance of an endometrioma is a homogeneous hypoechoic lesion with low to medium level echoes and no internal vascularity [4]. This had often been referred to as a “ground glass” appearance and is highly predictive of an endometrioma [3]. Due to such characteristics, sensitivity of USG for endometrioma ranged from 64% to 89% with a specificity of 80% to 100% [5].
Characteristic finding of endometrioma for MRI is increased signal intensity on T1-weighted images and decreased signal on T2-weighted images, sometimes referred to as “shading”. MRI has a greater than 90% sensitivity and specificity for endometrioma [6]. CT does not use for diagnosis of endometriosis due to lack both sensitivity and specificity, and a variety of nonspecific radiologic findings may be seen [7].
Uterine leiomyoma is a common benign disease, and it has different characteristics than endometriosis. The characteristics of a leiomyoma appear as a well-defined hypoechoic solid mass arising from the myometrium with a well-defined border or pseudocapsule resulting from compression of the adjacent myometrium [8]. Specificity of USG for leiomyoma is 91% and for sensitivity is 99% [9]. Characteristic finding of MRI appears as sharply margined areas of low to intermediate signal intensity on T1 and T2. Sensitivity and specificity are 99%, 86% respectively [9]. Even though MRI has high sensitivity and specificity secondary degenerations make it difficult to differentiate from other diseases. In CT scan, leiomyoma is usually indistinguishable from healthy myometrium unless they are calcified or necrotic. Therefore, CT scan is usually not the first-line imaging study for diagnosing and mapping uterine leiomyomas [10].
Even though, the role of CT scan in diagnosis of endometriosis and leiomyoma is limited, CT scans have been widely used due to relatively low costs and short scan time. Beside these reasons, CT can check the pelvis and abdomen with high accuracy on variable abdominal diseases. Moreover, technologic advances in CT have improved its ability to differentiate leiomyomas from normal myometrium. Therefore, CT scan may reduce the need for ultrasound or MRI when CT has been performed for other indications [8].
In this case, CT examination was thought to be done due to variable symptoms.Therefore, accurate diagnosis and treatment was delayed due to difficulties in differentiating between second degeneration of uterine leiomyoma and endometrioma.
Ultrasound examination is used as a first line in the diagnosis of abdominal and pelvic pain. Because USG is limited in viewing the entire abdomen, not the narrow range, CT is commonly used when there are various symptoms. Although MRI is better for differential diagnosis of endometriosis and uterine leiomyoma, which is a common pelvic disease, CT is often used because of cost-effectiveness. Therefore, for patients who have already taken CT, it is not an easy decision to take a MRI. Therefore, determining case which MRI scans should be performed is important in preventing delays in diagnosis and selecting appropriate therapy To date, no literature or guidelines have been identified about it.
Conclusion
Considering this case, even though severe pelvic pain was thought to cause by second degeneration of leiomyoma, considering MRI scan as additional imaging test should be helpful if patient has dysmenorrhea or history of endometriosis or the results of ultrasound or CT scan are not consistent with clinical symptoms.
Acknowledgement
This work was supported by clinical research grant from Pusan National University Hospital in 2016.
References
- Wolman I (2014) Berek Novak's Gynecology (15th edn). Journal of Obstetrics and Gynaecology of India 64(2): 150-151.
- Busacca M, Vignali M (2003) Ovarian endometriosis: from pathogenesis to surgical treatment. Curr Opin Obstet Gynecol 15(4): 321-326.
- Valentin L (2004) Use of morphology to characterize and manage common adnexal masses. Best Pract Res Clin Obstet Gynaecol 18(1): 71-89.
- Bhatt S, Kocakoc E, Dogra VS (2006) Endometriosis: sonographic spectrum. Ultrasound Q 22(4): 273-280.
- Moore J, Copley S, Morris J, Lindsell D, Golding S, et al. (2002) A systematic review of the accuracy of ultrasound in the diagnosis of endometriosis. Ultrasound Obstet Gynecol 20(6): 630-634.
- Togashi K, Nishimura K, Kimura I, Tsuda Y, Yamashita K, et al. (1991) Endometrial cysts: diagnosis with MR imaging. Radiology 180(1): 7378.
- Woodward PJ, Sohaey R, Mezzetti TP (2001) Endometriosis: Radiologic- Pathologic Correlation 1. Radiographics 21(1): 193-216.
- Shwayder J, Sakhel K (2014) Imaging for uterine myomas and adenomyosis. J Minim Invasive Gynecol 21(3): 362-376.
- Dueholm M, Lundorf E, Hansen ES, Ledertoug S, Olesen F (2002) Accuracy of magnetic resonance imaging and transvaginal ultrasonography in the diagnosis, mapping, and measurement of uterine myomas. Am J Obstet Gynecol 186(3): 409-415.
- Karasick S, Lev-TAS, Toaff ME (1992) Imaging of uterine leiomyomas. AJR American journal of roentgenology 158(4): 799-805.






























