Deceptive Appearance of Pelvic Actinomycosis in a Middle Aged Woman with Diabetes Mellitus and Long Standing Intra-Uterine Device: Mimicking an Ovarian Carcinoma
Dodampahala SH1*, De Silva MCV2 Dodampahala SK3 and Rahubaddha AN4
1Department of Obstetrics and Gynecology, University of Colombo, Sri Lanka
2Facu!ty of Medicine, University of Colombo, Sri Lanka
3Undergraduate Research Student, Sri Lanka
4Department of Obstetrics and Gynecology, University of Colombo, Sri Lanka
Submission: September 07, 2017 ; Published: September 18, 2017
*Corresponding author: Dodampahala SH, Department of Obstetrics and Gynecology, Faculty of Medicine, University of Colombo, Sri Lanka, Email: hemdodam@gmail.com
How to cite this article: Dodampahala S, D Silva M, Dodampahala S, Rahubaddha A. Deceptive Appearance of Pelvic Actinomycosis in a Middle Aged Woman with Diabetes Mellitus and Long Standing Intra-Uterine Device: Mimicking an Ovarian Carcinoma. J Gynecol Women's Health 2017; 7(1): 555702. DOI: 10.19080/JGWH.2017.6.555702
Abstract
Actinomycosis is a chronic granulomatous infection caused by filamentous, gram positive, anaerobic bacteria from the genus Actinomyces. The disease is characterized by variable presentations, including disease states that can mimic neoplastic disease. A case is presented of actinomycosis associated with long standing usage of intra-uterine device, which resembled an ovarian neoplasm. A 47 year old lady with a background history of type 2 diabetes mellitus presented with lower abdominal pain and a non-offensive vaginal discharge for the duration of one year. She also complained of episodes of fever and sweating. Abdominal and pelvic examination revealed an irregular, tender pelvic mass, the size of which corresponded to an 18 week uterus. Subsequent imaging studies deceptively pointed towards the diagnosis of a pelvic neoplasm. The histological samples acquired through a laparotomy, confirmed the diagnosis of actinomycosis and with an appropriate antibiotic course, she made a full recovery.
Introduction
Actinomycosis is a chronic granulomatous disease caused by filamentous, gram positive, anaerobic bacteria from the genus Actinomyces which are usually commensalism of the oral cavity and less prominently of the lower gastrointestinal and female genital tracts. Although pelvic actinomycosis accounts for only 3% of all actinomycotic infections in humans [1], it can cause significant diagnostic confusion leading to extensive investigations and surgical procedures. Abdominal surgery, ruptured viscus, tubo-ovarian abscess and intra-uterine devices (IUD) are recognized risk factors for abdominal and pelvic actinomycosis [2]. Here we present a case of a woman who had an IUD in-situ for 14 years, presented with abdominal pain and vaginal discharge and was diagnosed to have actinomycosis post-operatively.
Case Report
A 47 year old mother of 2, with a background history of type 2 diabetes mellitus presented to the gynecology clinic with lower abdominal pain and whitish non-offensive vaginal discharge for the duration of one year. Abdominal pain was dragging in nature, persistent and was present most of the time of the day. It was accompanied by episodes of pyrexia and sweating. She claimed the pyrexia was of low grade and was associated with malaise, lethargy and loss of appetite. There was increased frequency of urination with occasional episodes of dysuria. She had undergone two Caesarean sections (CS). Following the last CS, she was inserted with an IUD in 2001 which was subsequently removed in 2015. She had not had any past cervical smear examinations. Her last menstrual period was a week ago. There was no positive family history of ovarian or uterine malignancies. She did not hypoglycemic agents for diabetes mellitus and there was no have a positive contact history of tuberculosis. She was on oral evidence of macro or micro vascular disease (Figure 1).
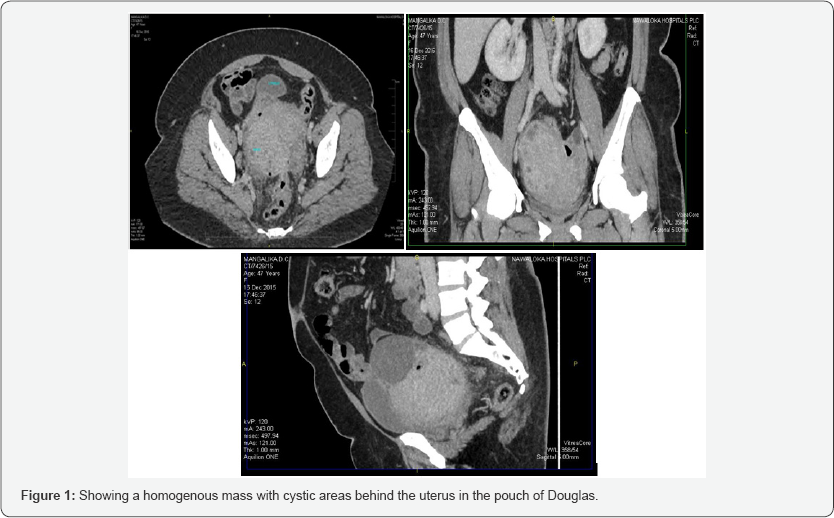
Her body mass index was 32. Weight was 89kgs. She had pallor and bilateral ankle oedema. There was no generalized lymphadenopathy. Abdominal examination revealed attended vague pelvic mass with irregular margins. There was no free fluid. Vaginal examination revealed a tender pelvic mass of 18 week size, with restricted mobility. Vaginal examination was extremely painful. Hence it was decided to proceed with an ultra sound examination which revealed a homogenous pelvic mass and an ill-defined uterus. Subsequent CT scan showed a clear homogenous mass with cystic areas posterior to the uterus in the pouch of Douglas.
Her full blood count showed Hb of 9.5g/dl. Since patient continued to suffer from pain and fever, it was decided to proceed with an exploratory laparotomy. The laparotomy revealed hyperemic pelvic organs. There was a bluish purple mass containing a white coloured homogenous material which seeped through the mass during mobilization. After a difficult dissection, the mass along with both ovaries and the uterus were removed without any bladder, bowel or urethra injuries. Two pints of blood were transfused during the procedure. A drain was placed during the post-operative period. There was a provisional diagnosis of pelvic abscess during the surgery and the relevant samples were sent for cytological and microbial analysis. Specimen was sent for histopathological evaluation. The peritoneal fluid and the material that seeped through the mass did not contain any cells of malignancy of malignant potential and the ABST was sensitive for Pivmecillinam. Although not in agreement with the antibiotic sensitivity, the patient was treated with Meropanam and Metronidazole intravenously for four days. Patient made a dramatic recovery and was discharged on Pivmecillinam, iron and nutritional supplements. The histology revealed the mass containing sulfur granules indicative of Actinomycosis infection. Patient was recalled and a multidisciplinary opinion was obtained including the histopathologist and microbiologist to manage the said condition. She received intravenous Benzyl penicillin for five days and was discharged on oral penicillin for the period of one month. Patient was recalled after one month and she was clinically normal with her CRP level less than 6mg/dl.
Discussion
Actinomycosis is a rare disease characterized by contiguous spread, suppurative and granulomatous inflammation, and formation of multiple abscesses and sinus tracts that may discharge sulfur granules. Although it's a rare disorder the resemblance of clinical presentation and the radiological appearance to an ovarian malignancy may lead to misdiagnose of the condition especially by a young gynecologist. It's caused by Actinomyces species which are among the normal flora of the oral cavity and less prominently in the lower gastro intestinal and female genital tracts. Because these microorganisms are not virulent, they require a break in the integrity of the mucous membranes [1]. Furthermore, actinomycosis is mostly a polymicrobial infection, with isolates numbering as many as 10 bacterial species. These co-pathogens may play a role in enhancing the relatively low invasiveness of actinomycetes [1]. In this particular case we believe that diabetes mellitus played a role in increasing the susceptibility by reducing the immunity in our patient. Once infection is established, the host mounts an intense inflammatory response which manifests as granulomatous or suppurative inflammation and fibrosis may then follow. Infection typically spreads contiguously, ignoring tissue planes and invading surrounding tissues and organs eventually resulting in sinus tract formation. Typically sulfur granules can drain from these tracts. Hematogenous dissemination to distant organs is also a known sequale of actinomycosis.Actinomycosis has a predilection to occur in young to middle aged adults. For unknown reasons it is three times commoner in males with the exception of pelvic actinomycosis [1].
Actinomycosis is divided into three forms: cervicofacial, thoracic, and abdominopelvic. The most frequent site of human infection is the cervicofacial area, accounting for 40 to 50% of cases. Pelvic actinomycosis accounts for only about 3% of all human actinomycocyte infections [2,3]. Abdominal disease is usually a result of disruption of bowel mucosa. It often occurs as a firm mass that appears fixed to the surrounding tissue and often is mistaken for a tumor [4,5]. Abdominal surgery, ruptured viscus, tubo-ovarian abscess and IUDs are recognized risk factors for abdominal and pelvic actinomycosis [2,5]. Actinomycesisraelii infects 1.65% to 11.6% of IUD users, and infection is more common in women who have had an IUD in situ longer than four years. In females, Actinomyces is thought to be originated fromoro-genital contact [3].
Pelvic actinomycosis usually causes endometritis, salpingo- oophoritis, or tubo-ovarian abscess and a mass in the addenda may be palpable, indicating a pelvic malignancy. Subsequent extension to the abdominal wall or deep pelvic structures can occur. Pelvic actinomycosis can present with lower abdominal discomfort, abnormal vaginal bleeding or discharge. Examination may reveal a pelvic mass typically firm-to-hard in consistency, non-tender, often fixed to underlying tissue or less frequently sinus tracts with drainage from either the abdominal wall or the perianal region [6]. As pelvic actinomycosis causes symptoms and signs mimicking a pelvic abscess or a pelvic tumour, the initial investigations are directed towards these diagnoses leading to diagnostic confusion and more often than not missing the diagnosis of actinomycosis.
Because actinomycosis is difficult to diagnose based on the typical clinical features, direct identification of the infecting organisms from a specimen or sulfur granules is necessary for definitive diagnosis. Ultrasound-guided fine-needle aspiration or biopsy have been used successfully to obtain clinical material for diagnosis of actinomycosis [7]. However in a non-feasible site a laparotomy may be required to obtain the necessary samples. An exploratory laparotomy is warranted in the case of diagnostic uncertainty. Identification of sulfur granules is almost path gnomonic of actionomycosis [8]. A Gram-stained smear of the specimen may demonstrate the presence of beaded, branched, gram-positive filamentous rods, suggesting the diagnosis of actinomycosis. Isolation and definitive identification of actinomycetes via culturing may require 2-3 weeks [9].
In most cases of actinomycosis, antimicrobial therapy is the only treatment required, although surgery can be adjunctive in selected cases. Penicillin is the drug of choice for treating infections caused by actinomycetes and resistance is rare. Lack of a clinical response to penicillin usually indicates the presence of resistant companion bacteria. In those who are allergic to penicillin, erythromycin, doxycycline and clindamycin can be used [10]. Parenteral therapy might be required for severe infection before changing to the oral route. Generally, antibiotics are continued until there is evidence of complete resolution. Surgery is at times required to drain abscesses.
Conclusion
Pelvic actinomycosis should always be considered in patients presenting with a pelvic mass especially in those using or having had a history of using an IUD. Owing to the presentation with non-specific symptoms the accurate early diagnosis of actinomycosis is challenging and may necessitate the need for a laparotomy. Surgeons should be aware of this infection in order to avoid excessive surgical procedures. Diabetes mellitus can be a contributory fact in predisposing the patients for actinomycotic infection by reducing the host immunity [11].
References
- Hall V (2008) Actinomyces-gathering evidence of human colonization and infection. Anaerobe 14(1): 1-7.
- Schiffer MA, Elguezabal A, Sultana M, Allen AC (1975) Actinomycosis infections associated with intrauterine contraceptive devices. Obstet Gynecol 45(1): 67-72.
- McCormick JF, Scorgie RD (1977) unilateral tubo-ovarinactinomycosis in the presence of an intrauterine device. Am J Clin Pathol 68(5): 622626.
- Wagenlehner FM, Mohren B, Naber KG, Mannl HF (2003) Abdominal actinomycosis. Clin Microbiol Infect 9(8): 881-885.
- Sung HY, Lee IS, Kim SI, Jung SE, Kim SW, et al. (2011) Clinical Features of Abdominal Actinomycosis: A 15-year Experience of A Single Institute. J Korean Med Sci 26(7): 932-937.
- Hinnie J, Jaques BC, Bell E, Hansell DT, Milroy R (1995) Actinomycosis presenting as carcinoma. Postgrad Med J 71(842): 749-750.
- Wagenlehner FM, Mohren B, Naber KG, Mannl HF (2003) abdominal actinomycosis. Clin Microbiol Infect 9(8): 881-885.
- Abela J, Sciberras J, Meilak M, Felice AG, Degaetano J (2004) Omentalactinomycosis presenting with right lower quadrant abdominal pain. J Clin Pathol 57(6): 671.
- Schaal KP, Pape W (1980) Special methodological problems in antibiotic testing of fermentative actinomycetes. Infection 8(Suppl2): S176-182
- Smith AJ, Hall V, Thakker B, Gemmell CG (2005) Antimicrobial susceptibility testing of Actinomyces species with 12 antimicrobial agents. J Antimicrob Chemother 56(2): 407-409.
- Wong VK, Turmezei TD, Weston VC (2011) Actinomycosis. BMJ 343: d6099.






























