Trend and Timing of Maternal Death in Mizan-Aman and Gebretsadikshawo General Hospitals Ethiopia 2011 - 2015 Case Control Study
Tensay kahsay*, Tegene Legese and Kebadnew Mulatu
Department of Nursing, Mekelle University, Ethiopia
Submission: May 29, 2017; Published: July 18, 2017
*Corresponding author: Tensay kahsay, Department of Nursing, College of Health Sciences, Mekelle University, Ethiopia, Tel: +251912937986; Email: tensayl221@gmail.com
How to cite this article: Tensay k, Tegene L, Kebadnew M. Trend and Timing of Maternal Death in Mizan-Aman and Gebretsadikshawo General Hospitals Ethiopia 2011 � 2015 Case Control Study. J Gynecol Women's Health 2017; 6(1): 555678. DOI: 10.19080/JGWH.2017.06.555678.
Abstract
Background: The economic burden on family, total lost economic productivity and out of pocket expenditure of households with maternal death is 10 times higher than that in without maternal death. Even though our country reduces the maternal death from previous times as the report of international organizations, still the number of death that occurs currently is high as WHO maternal death classification.
Objective: To identify the trend and timing of maternal death in Mizan -Amanand Gebretsadikshawo general hospitals Ethiopia 2011-2015 a five years retrospective analysis
Methods: Institution based retrospective case control study design was conducted to investigate the trend and time of maternal death. A total of 595 samples, 119 cases and 476 controls were included from the maternal logbooks of the hospitals based on proportional allocation to patient flow of the hospitals. The collected data was entered into Epi Data version 3.1 and then exported for analysis to STATA version 13.1.
Result: Most death (74.8%) occurred during post-partum period. From post-partum period the first three days is crucial, which accounts 69(77.5%) of deaths occurred within 72 hours of delivery. Only 17.6% of women died in Intrapartum period. The maternal mortality was higher in 2013 and lower in 2015.
Conclusion: The number of maternal death has a fluctuation pattern. MMR is high as compared to national figure and it is in range of very high maternal death classification as per WHO classification. Most of the women died in post-partum period particularly within three days.
Keywords: Trend; Timing; Maternal death; Ethiopia
Introduction
Women shoulder a double burden of helping to support the family by working outside the home and taking full responsibility for household duties and child care. Yet, despite this vital role played by women in society, the health needs of a women is neglected which is evidenced by high level of maternal mortality in many poor countries [1,2].
Globally maternal mortality rate (MMR) has fallen by 45% from 523,000 (380/100,000) in 1990 to 289,000 (210/100,000) in 2013 yielding an average annual decline of 2.6%. In 2013, developing countries account for 99% (286 000) of the global maternal deaths with sub-Saharan Africa (SSA) region alone accounting for 62% (179 000) followed by Southern Asia (69 000). Based on this, the MMR in developing regions was 14 times higher than in developed regions [3,4].
In general in SSA there is 49% reduction from 990 to 510 per 100,000 but eastern Africa reduces MMR by 57% from 1000 to 440 per 100,000 which are highest in SSA. Ethiopia decreased maternal death from 1400 to 420 per 100,000 MMR between 1990 and 2013 which is making progress to achieve MDG 5 by 2015 [2,4,5]. Even though our country reduces the maternal death from previous times as the report of international organizations, still the number of death that occurs currently is high as world health organization (WHO) maternal death classification. In contrary, some hospital based study in our country shows inconsistency in death trend. So the need of further study is unquestionable to identify trend and time maternal death. Particularly health institutions based study is important to observe the trend, time of maternal death.
Methods
The study was conducted at Mizan-Aman & Gebretsadikshawo general hospitals, which are located around 568Km and 440Km respectively in south western of Addis Abeba the capital city of Ethiopia. Institution based retrospective case control study design was conducted to investigate the trend and time of maternal death. Sample size was determined using STATA version 13.1 by taking the following assumptions 95% CI, and 90% power, odds ratio of 0.27 (odds of women having less than 24 labour length over odds of women having greater than 24hr labour length) from study done in Tigray region, case to control ratio of 1:4 and the prevalence of exposure among controls were 97.6% (proportion of controls delivered in less than 24hr) taken from unmatched case control study done in Tigray regional state [6]. A total of 975 charts, 195 cases and 780 controls were planned to include in the study. But due to poor registration and shortage of sample we included a total of 595 samples, 119 cases and 476 controls (Figure 1).
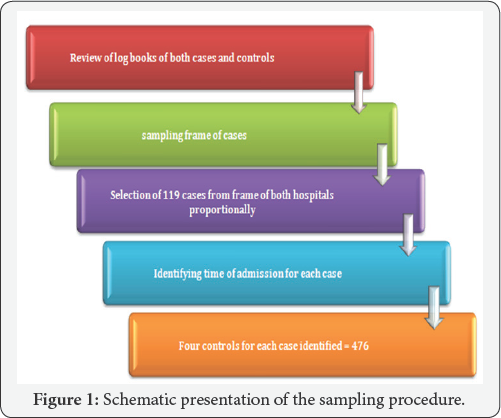
To access the number of cases and controls in the study the following short description of sampling procedures was used. Data collection instrument was adapted from Maternal Death Surveillance and Response Technical Guideline of Ethiopia [7]. The checklist consists of socio-demographic data, obstetric and delivery history, time of death, antenatal and intranatal risks and presence of complications. The collected data was entered into Epi Data version 3.1 and then exported for analysis to STATA version 13.1. The data was cleaned for inconsistencies and missing values. Graphical presentation such as tables, line graphs and bar graph was used to present the result findings of the study. Maternal mortality trend was done using the total number of cases occurred in the study period. Trend is shown using MM Ratio. The total MM Ratio in 5 year and each year MMR was calculated using the following formula
MMR = totalnumberofmaternaldeathinthestudyperiod/ Totalnumberoflivebirthsinthestudyperiod x100,000
Prior to data collection, ethical clearance was obtained from Research and Ethics committee of the College of Health sciences of Mizan-Tepi University. Written permission letter will also be received from Mizan-Aman general hospital & Gebretsadikshawo general hospital CEO and other concerned bodies in the study set up. In order to establish anonymous linkage only the codes, not the names of the participant from the chart, was registered on the questionnaire. During the training of data collectors and supervisor, ethical issues was addressed as important component of the research.
Result
A total of 119 cases (dead women) and 476 controls (survived women) were included in the study. Majority of the women age was with 20-34 years which were 397(66.7%). The other sociodemographic data were including in the analysis due to poor registration or 99% were not included in the maternal charts.
Obstetric and delivery history
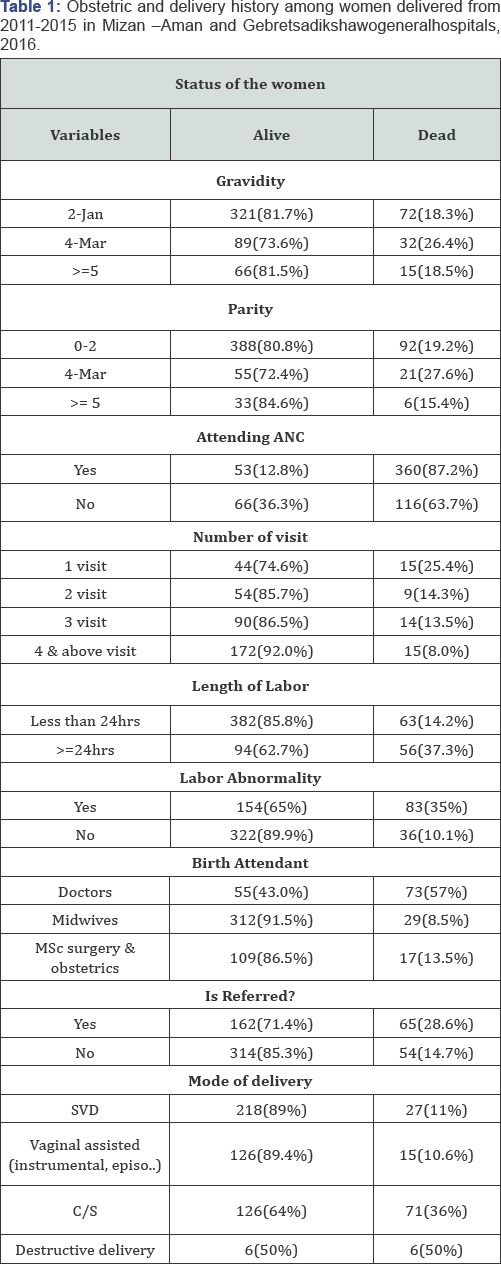
Regarding the women obstetric and delivery history around 393(66.1%) were gravid 1-2 and 480(80.7%) were in parity 0-2. Majority 413(69.4%) were attending ANC, of those 187(45.2%) were attended 4 times and more. From the total women 227(38.2%) were come to the hospitals by referral due to different complication. And 237(39.8%) of the women were developed labor abnormality. From the women who had 3-4 gravidity more than 26% of them are died. Likewise from women who had 3-4 parity more than 27% of them are died. More than 63% of women who don't have ANC are died. From women who had only one visit more than 25% of them are died (Table 1).
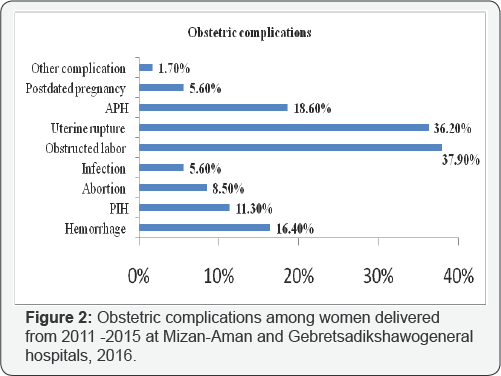
About obstetric complications of the women 177(29.7%) were developed different types of obstetric complications. The leading obstetric complications were obstructed labor, and uterine rupture which accounts 67(37.9%), and 64(36.2%) respectively (Figure 2).
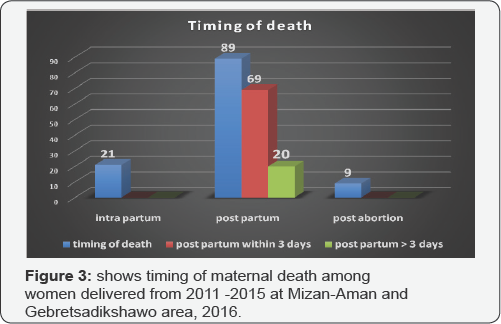
Timing of maternal death
Most death (74.8%) occurred during post-partum period. From post-partum period the first three days is crucial. From 89 deaths in post-partum period 69(77.5%) of deaths occurred within 72 hours of delivery. Only 17.6% of women died in Intrapartum period (Figure 3 & Table 2).
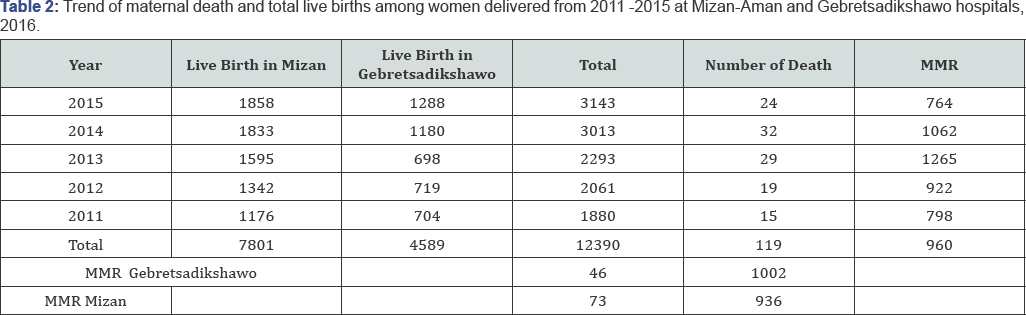
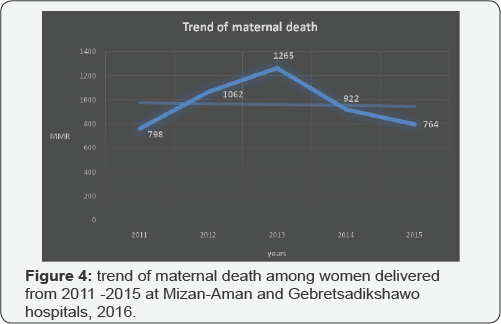
Trends of maternal death
The maternal mortality was higher in 2013 and lower in 2015. The number of live birth more or less has an increasing pattern which is having highest number of live births in 2015 and lowest number of live birth in 2011. The maternal mortality was higher in Mizanaman hospital 1002/105. The number of live births is higher in Mizan than Gebretsadikshawo (Figure 4).
Discussion
Maternal death in our country has a decreasing trend as depicted by different reports and reviews. As 2013 combined reports by WHO, UNICEF, the World Bank and UNFPD Ethiopia shows a decreasing pattern of maternal death. The general MMR in these hospitals is 960/105. It has a fluctuation pattern from 764 to 1265/105. It was highest in 2013 with 1265/105 and lowest in 2015 with 764/105 than other study periods in the study. Review of different community and hospital based studies by Ahmed Abdela shows a decreasing pattern of maternal death. Review made in jimma hospital before 15 years back and in Ambo hospital before 5 years back shows fluctuation of MMR from 671 -3986 per 105 but it is higher in general than the current of our finding. Review of maternal death from 2002-2006 in JUSH also shows a decreasing pattern with total MMR of 888/105 [4,8,911]. Decrease in occurrences of death from previous years in these hospitals particularly after 2010 might be because of increasing awareness of community about institutional delivery, organizational and policy factors. Organizational factors might be service expansion and human power expansion, increasing availability and accessibility of HI. The other factor might be after 2010 in our country there was country wide mobilization to decrease death of mother with slogan of "no mother should die while she gave birth.” In the other extreme it might be because of under reporting of death due to fear of bad criticism and captivity health professionals. These things might be the reason.
Most of death (74.8%) occurred during postpartum period. This study was consistent with study done in India, which revealed that postpartum deaths accounted for about 70% [12]. Which is higher than finding from south west Ethiopia in Bonkewereda in which 51% of maternal death occurred in postpartum period. This might be because of difference in number of maternal death included in the study, 49 deaths was included in Bonkewereda but in this research 119 maternal death were included in the study. The other reason might be because of recall bias introduced in south west Ethiopia study since it is retrospective cross sectional house hold survey. However study from maternity hospital of Nigeria shows about 61.9% of the maternal deaths occurred in post-partum period which is lower than this finding. This might be because of only 84 maternal deaths in two year study period were included. if it is data of five year it might be higher than this research finding [13,14]. Higher number of maternal death in post-partum period implies that the management following delivery and during delivery might be poor. Prolonged period of labour due to OL or due to not having timely intervention might contribute a lot for death occurring in post-partum period.
In the current study 21(17.6%) of maternal death occurred intra-partum. However lower than 37% from study done in Bonkewereda, Ethiopia. This difference might be because of difference in site of delivery, in Bonkewereda, south west Ethiopia 92% of delivery occurred in home so that in home delivery complications are not managed well so high number of death may occur in intra-partum period. But it is much higher than from findings of maternity hospital of Nigeria which is 13.1%. This difference might be because of high antepartum death (10.7%) and death because of post-abortion complications (14.3%). in maternity hospital of Nigeria in which 25% of women died before reaching to intra-partum period. post- abortion death accounts 7.6% of the death in this finding which is lower than study of Nigeria 14.3%. The reason might be absence of blood bank, difference in size and level of hospital and difference in the number of health professionals (low number) during the study period in maternity hospital of Nigeria might contribute to poor quality of abortion care. The other reason might be dramatic reduction of maternal death related with abortion due to the introduction of misoprostol or safe mother hood services or emergency contraception in our country [13,14].
None of the death in this study were not occurred in antepartum, but study done in Ethiopia and Nigeria showed that 12% and 10.7% death occurred at ante-partum respectively This might be due to high coverage of ANC in this study, which helps to prevent death during ante-partum. Ante partum death occurred in south west Ethiopia is 12% which is higher than this research finding 0%. There might be difference in awareness, this might create poor follow up of women during ante partum in south west Ethiopia study [13,14]. These imply that proper care during antenatal period, reduce home delivery, intra-partum period and after abortion save the lives of many women in antenatal and intra partum period. In general the major reason of inflated postpartum death and relative small number of death in intra-partum and post-partum in these hospitals as compared to Bonkewereda study is set up difference in which health institution death represents for 14% of females who utilize institutional delivery but the study of Bonkewereda represents 86% of females who did not utilize institutional delivery.
Implications of these findings are
1. Management after terminating pregnancy might be poor or the women might not utilize postpartum care service.
2. The risk of death during intra-partum period is high when the delivery is at home.
Conclusion
The number of maternal death has a fluctuation pattern. MMR is high as compared to national figure and it is in range of very high maternal death classification as per WHO classification. Most of the women died in post-partum period particularly within three days.
Recommendation
To decrease the number of maternal death multi-sectorial collaboration is important. Everybody starting from a single individual to the higher officials and organizations has a responsibility to alleviate the problem.
Based on the findings from thisstudy the following recommendations are made:
I. To Bench Maji and Keffa zone health department
i. The zones should follow, monitor and evaluate IEC/ BCC provided by wereda health offices and health institutions to increase awareness of the community about complications of pregnancy and strengthen the referral system to avoid delay in intervention or to avoid prolonged labour
II. To gebretsadikshawogeneral and mizan -aman hospitals
i. They should strengthen service provision to reduce death in intra-partum period and post-partum period (particularly after operative delivery) and to avoid prolonged labour.
ii. They should improve the registration system of events and place for the placement of patient charts.
III. To health professionals
i. Health professionals should have to improve timely intervention to avoid delayed intervention.
IV. To HEWs:
i. They should have to improve awareness of the community about pregnancy complications and simultaneous comorbidities.
V. To academicians and researchers:
i. They should dig out associated socio-economic factors for maternal death
ii. Why most women would die in post-partum period?
Funding
This study was funded by Mizan-Tepi University.
Authors� Contribution
TG, KM and TK conceived the study, involved in the study design, data analysis, drafted the manuscript and critically reviewed the manuscript. All authors read and approved the final manuscript.
Acknowledgement
We are grateful to Mizan-Tepi University for funding the study and other supports. We would like to acknowledge Bench Maji, and Kefa Zonal Health Office for their cooperation in conducting this study. We would like to express our deepest gratitude for field data collectors for their hard work and sincere contribution.
References
- Divya A Patel, MPH Nancy M, Burnett, BS Kathryn M, Curtis P (2003) Maternal Health Epidemiology.
- World Health Organisation (2010) International statistical classification of diseases and related health problems. (10th revision), Instruction Manual. WHO, Geneva, Switzerland.
- Kassebaum NJ, Bertozzi-villa A, Coggeshall MS, Shackelford KA, Steiner C, et al. (2014) Global, regional, and national levels and causes of maternal mortality during 1990-2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet 6736(14): 1-25.
- WHO (2013) World bank, UNFPA U and U. Trends in Maternal Mortality: 1990 to 2013.
- Baden S (1996) Challenges to women ' s reproductive health: maternal mortality. 44(38).
- Gidey G (2013) Patterns of maternal mortality and associated factors; a case-control study at public hospitals in tigray region, ethiopia. Int J Pharm Sci Res 4(5): 1918-1929.
- Federal Democratic Republic of Ethiopia Ministry of Health (2012) Maternal Death Surveillance and Response (MDSR) Technical Guideline.
- Garomssa H, ADD (2008) Maternal mortality in Ambo Hospital: a five year retrospective review. Ethiop J Reprod Heal 2(1): 2-13.
- Abdella A (2010) Maternal Mortality Trend in Ethiopia. Ethiop J Heal dev 24(1): 115-122.
- Berhan Y, Berhan A (2014) Review of maternal mortality in ethiopia : a story of the past 30 years. Ethiop J Heal Sci 3-4.
- Negussie D, Mesfin N (2009) Review of maternal death in jimma univeristy specialized hospital. Ethiop J Heal Sci 19(1): 9-12.
- Devi K, Singh SR (2012) Maternal Mortality and Its Causes in a Tertiary Center. J Obstet Gynecol India 62(2): 168-171.
- Olopade FE, Lawoyin T (2008) Maternal Mortality in a Nigerian Maternity Hospital. African J Biomed Res 11: 267-273.
- Yaya Y, Eide KT, Norheim OF, Lindtj0rn B (2014) Maternal and Neonatal Mortality in South-West Ethiopia: Estimates and Socio-Economic Inequality. PLoS One 9(4): e06294.






























