Common iliac Artery Pseudo Aneurysm as a Complication of Diagnostic Laparoscopy
Purohit P1*, Ramnarine R2, Evans D2 and Narvekar N1
1Department of Gynaecology, Kings College Hospital, London
2Department of Interventional Radiology, Kings College Hospital, London
Submission: March 13, 2017; Published: March 27, 2017
*Corresponding author: Purohit P, Department of Gynaecology, Kings College Hospital, London, Email: prashant.purohit@nhs.net
How to cite this article: Purohit P, Ramnarine R, Evans D, Narvekar N. Common Iliac Artery Pseudo Aneurysm as a Complication of Diagnostic Laparoscopy. J Gynecol Women's Health. 2017; 3(3): 555617. DOI: 10.19080/JGWH.2017.03.555617.
Keywords
Keywords: Veress needle; Aneurysm; Laparoscopy; Vascular injury; Stent
Introduction
In UK, a quarter of a million women undergo laparoscopic surgery each year most of which are without any serious complications [1]. Vascular injury, albeit rare, is a major life-threatening complication of laparoscopy and it is difficult to determine the exact incidence due to its rarity and possible under-reporting. The published rates vary between 0.1 to 1.05/1000 cases with maximum risk reported during e the phase of entry i.e from insertion of optical port until visualisation of the intrabdominal contents [2,3].
We report a case of Visceral Artery pseudo aneurysm (VAP) of the Right Common Iliac secondary due to Veress needle insertion during a gynaecological surgery.
Case Report
A 29 year female underwent diagnostic laparoscopy to manage uterine perforation during a hysteroscopic surgery. The laparoscopy was carried out by routine closed entry technique with single passage of Veress needle for pneumoperitoneum followed by 10mm intra-umbilical port and 5mm lateral accessory port. A small uterine fundal perforation was sutured with 2-0 Vicryl. The total procedure time was 90 minutes. The blood loss during the procedure was minimal.
The patient presented with severe abdominal pain and transient hypotension during the post-operative period. Her observations settled with fluid resuscitation and she was kept overnight for pain control. An urgent post-operative Hb showed a drop in Hb (pre-op=139g/L, post-op=88g/L). On examination, abdomen was soft with no guarding or rigidity. Due to persistent post-operative pain and disproportionate fall in Hb, an urgent CT scan was arranged.
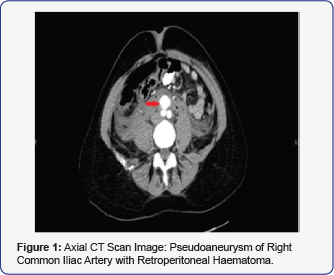
CT showed a large retro peritoneal haematoma extending from renal veins up to the pelvis with pseudo aneurysm of the Right Common Iliac Artery measuring 21x27x17mm just below the aortic bifurcation (Figure 1). Retrograde puncture of the ipsilateral common femoral artery was performed under ultrasound guidance followed by insertion of a 7 French sheath. A pigtail catheter was sited into the distal aorta, allowing for angiographic identification of the pseudoaneurysm origin. A 10 mm diameter balloon-mounted Advantage V12 covered stent (Atrium Medical, USA) was then deployed within the common iliac artery, excluding flow into the aneurysmal sac. A percutaneous 10mmx60mm Endovascular Stent graft was inserted in the Right Common Iliac Artery pseudo aneurysm (Figure 2). Post stent angiography demonstrated satisfactory flow within the vessel, with no filling of the pseudoaneurysm. The access site was sealed with deployment of an Angioseal collagen plug closure device. This procedure was uneventful. The patient was put on dual anti-platelet therapy (Aspirin+Clopidogrel) and LMW heparin.
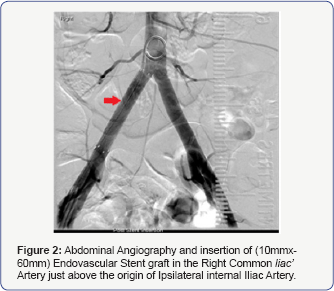
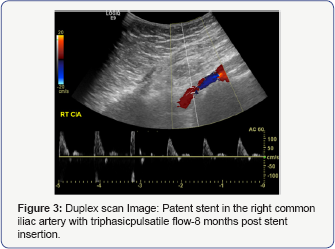
She was transfused 2 units of blood and then discharged a week later after her original procedure. She was jointly followed up by the gynaecology and vascular team. A duplex scan done 8 months post stenting showed a well embedded and patent stent in the right common iliac artery with triphasic pulsatile flow and no stenosis. No pseudo aneurysm was seen during this examination (Figure 3).
Discussion
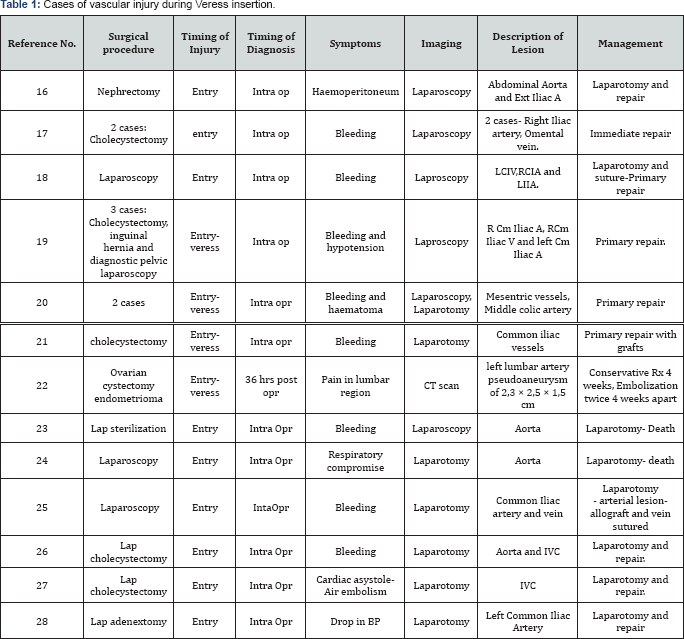
Visceral artery psuedoaneurysms (VAP) can develop as a result of blunt or penetrating trauma, inflammation, infection, vasculitis, and iatrogenic trauma secondary to surgical, endoscopic, and radiologic procedures. In traumatic VAPs, the pathologic feature is deficiency of the arterial media with loss and/or fragmentation of the connective tissue and smooth muscle. The VAP in this case was attributed to the blind technique of Veress needle insertion. Alternative to the blind Veress needle insertion technique is the open Hasson’s technique. However, based on the available evidence there is no consensus in regards to the superiority of one technique over the other [4]. The open technique is associated higher bowel injuries as compared to the closed technique. However, quality of evidence in this regards is poor [5]. The risk of vessel damage was so low in both groups that no statistical difference was observed (Table 1).
This procedure was performed by an experienced laparoscopic surgeon. As per the analysis done by Schäfer et al. [6] 85% of the major vascular injuries caused either by experienced surgeons (those who had performed between 51 and 100 procedures) or very experienced surgeons (over 100 procedures performed). Thus, it is essential that the position of the needle tip after insertion be determined as accurately as possible and with great care.
Complications of VAPs can be life threating which include early rupture, compression of adjacent structures, thromboembolism and a higher frequency of aneurysm infection. Lack of an intact vessel wall leads to continued enlargement and subsequent rupture in nearly all cases of visceral pseudo aneurysms necessitating prompt and accurate treatment. In this particular case, post-operative pain and drop in haemoglobin level were the symptoms which prompted further investigations to diagnose the VAP. The mainstay for diagnosis of VAPs is the conventional angiography but is an invasive procedure and non-invasive diagnostic modalities like CT scan, MRI both combined with Angiography and colour Doppler Ultrasound study should be included in the initial work-up if possible [7]. In our case, the VAP was diagnosed on a contrast CT scan.
Another aspect highlighted through this case is the novel approach towards management of arterial aneurysms. Traditionally, internal iliac aneurysms have been repaired by surgical interposition of graft particularly in aneurysms >40mm to prevent rupture [8,9]. This approach is challenging due to the difficult dissection and surgical approach into the pelvis with high risk of visceral, genitourinary and pelvic venous injury with carries a significant morbidity and mortality of up to 10% [9].
With the advancement of endovascular techniques, effective alternative is now available. Particularly in our case as the aneurysm was close to the aortic bifurcation and minimally invasive repair played an important role. The technique of endovascular repair of a subclavian artery penetrating injury was first described in 1996 [10]. Similarly, Nyman et al. [11] presented three cases of iatrogenic iliac artery perforations treated by endovascular stent-grafting in 1999. There have been multiple subsequent reviews and case reports of endovascular techniques for arterial injuries throughout the body [12-14].
The mainstay of therapy is based on the use of stent-grafts. First developed for treating aneurysms, stent-grafts consist of a tubular metal scaffold covered with PTFE to create an artificial lumen through which blood can be diverted. The benefit of stent-grafts is that they can be packaged tightly within a small diameter delivery device and inserted endoluminally through an arterial puncture. They can be expanded in-situ, either by balloon inflation or self-expansion, the latter of which relies on the shape memory properties of the metal alloy Nitinol. With regards to focal penetrating arterial injury to a relatively large vessel such at the common iliac, stent-graft deployment can seal the point of haemorrhage without the need for open surgical repair, significantly reducing the morbidity and mortality associated with emergent laparotomy [15].
We would also like to stress here the need for appropriate counselling and consenting of all women before laparoscopic procedures. Women must be informed of the risks and potential complications associated with laparoscopy.
Conclusion
VAPs although life threating are extremely rare. All laparoscopic surgeons should be aware of the possibility of this complication which can happen even in the most experienced hands. High index of suspicion, early diagnosis and prompt treatment is the key towards minimizing the morbidity and mortality associated with these complications. This also depends on a great extent to the local availability of imaging modalities and interventional radiology services.
References
- Preventing Entry Related Gynaecological Laparoscopic Injuries: Royal College of Obstetricians and Gynaecologists Green-top Guideline No. 49 May 2008.
- Harkki-Siren P, Kurki T (1997) A nationwide analysis of laparoscopic complications. Obstet Gynecol 89(1): 108-112.
- Jansen FW, Kapiteyn K, Trimbos-Kemper T, Hermens J, Trimbos JB (1997) Complications of laparoscopy: a prospective multi-centre observational study. Br J Obstet Gynaecol 104(5): 595-600.
- Tinelli A, Malvasi A, Istre O, Keckstein J, Stark M, et al. (2010) Abdominal access in gynaecological laparoscopy: a comparison between direct optical and blind closed access by Verres needle. Eur J Obstet Gynecol Reprod Biol 148(2): 191-194.
- Ahmad G, Duffy JMN, Phillips K, Watson A (2008) Laparoscopic entry techniques. Cochrane Database of Systematic Reviews. Article ID CD006583.
- Schäfer M, Lauper M, Krähenbühl L (2001) Trocar and Veress needle injuries during laparoscopy. Surgical Endoscopy 15(3): 275-280.
- Saad NE, Saad WE, Davies MG (2005) Pseudoaneurysms and the role of minimally invasive techniques in their management. Radiographics 25(Suppl 1): S173-S189.
- Dix FP, Titi M, Al-Khaffaf H (2005) The isolated internal iliac artery aneurysm-a review. Eur J Vasc Endovasc Surg 30(2): 119-129.
- Patel NV, Long GW, Cheema ZF, Rimar K, Brown OW, et al. (2009) Open vs. endovascular repair of isolated iliac artery aneurysms: a 12-year experience. J Vasc Surg 49(5): 1147-1153.
- Patel AV, Marin ML, Veith FJ (1996) Endovascular graft repair of penetrating subclavian artery injuries. J Endovasc Surg 3(4): 382-388.
- Nyman U, Uher P, Lindh M, Lindblad B, Brunkwall J, et al. (1999) Stent-graft treatment of iatrogenic iliac artery perforations: Report of three cases. Eur J Vas Endovasc Surg 17: 259-263.
- Baltacioglu F, Cimsit, NC, Cil B, Cekirge S, Ispir S (2003) Endovascular stent-graft applications in iatrogenic vascular injuries. Cardiovasc Intervent Radiol 26(5): 434-439.
- Heye S, Vanbeckevoort D, Blockmans D, Nevelsteen A, Maleux G (2005) Iatrogenic main renal artery injury: treatment by endovascular stent-graft placement. Cardioasc Intervent Radiol 28: 93-94.
- DuBose J, Recinos G, Teixeira PJ, Inaba K, Demetriades D (2008) Endovascular stenting for the treatment of traumatic internal carotid arteries: expanding experience. Journal of Trauma 65(6): 1561-1566.
- White R, Krajcer Z, Johnson M, Williams D, Bacharach M, et al. (2006) Results of a multicentre trial for the treatment of traumatic vascular injury with a covered stent. Journal of Trauma 60(6): L1189-L1195.
- Simforoosh N, Basiri A, Ziaee SAM, Tabibi A, Nouralizadeh A, et al. (2014) Major Vascular Injury in Laparoscopic Urology. JSLS: Journal of the Society of Laparoendoscopic Surgeons 18(3): e2014.00283.
- Schäfer M, Lauper M, Krähenbähl L (2001) Trocar and Veress needle injuries during laparoscopy. Surg Endosc 15(3): 275-280.
- Geers J, Holden C (1996) Major vascular injury as a complication of laparoscopic surgery: a report of three cases and review of the literature. Am Surg 62(5): 377-379.
- Dixon M, Carrillo E (1999) Iliac vascular injuries during elective laparoscopic surger. Surg Endosc 13(12): 1230.
- Roviaro G, Varoli F, Saguatti L, Vergani C, Maciocco M, et al. (2002) Major vascular injuries in laparoscopic surgery. Surg Endosc 16(8): 1192-1196.
- Guloglu R, Dilege S, Aksoy M, Alimoglu O, Yavuz N, et al. (2004) Major Retroperitoneal Vascular Injuries During Laparoscopic Cholecystectomy and Appendectomy. Journal of Laparoendoscopic& Advanced Surgical Techniques 14(2): 73-76.
- Alcázar GD, Chapinal GB, Badia BE, Jesús SJL, Muñoz-Hernando L, et al. (2014) Psoas haematoma as a complication of Veress needle insertion: description of a case and literature review. BMC Surgery 14: 104.
- Peterson HB, Greenspan JR, Ory HW (1982) Death following puncture of the aorta during laparoscopic sterilization. Obstet Gynecol 59(1): 133-134.
- Hanney RM, Alle KM, Cregan PC (1995) Major Vascular Injury and Laparoscopy. Australian and New Zealand Journal of Surgery 65: 533-535.
- Baadsgaard SE, Bille S, Egeblad K (1989) Major Vascular Injury during Gynecologic Laparoscopy: Report of a case and review of published cases. Acta Obstetriciaet Gynecologica Scandinavica 68(3): 283-285.
- Battaglia L, Bartolucci R, Berni A, Leo E, De Antoni E (2003) Major vessel injuries during laparoscopic cholecystectomy: a case report. Chir Ital 55(2): 291-294.
- Benítez Pacheco OR, Serra E, Jara L, Buzzi JC (2003) Heart arrest caused by CO2embolism during a laparoscopic cholecystectomy. Rev Esp Anestesiol Reanim 50: 295-298.
- Chapron CM, Pierre F, Lacroix S, Querleu D, Lansac J, et al. (1997) Major Vascular Injuries during Gynecologic Laparoscopy. J Am Coll Surg 185(5): 461-465.






























