Fatal Manual Strangulation: A Brief Overview
Kenrick Berend1* and Guido Reijnen2,3
1 Curacao Medical Centre, Curaçao
2 Pulmonary department, Bravis hospital, Netherlands
3 Department of Forensic Medicine, Public Health Service of Eindhoven, Netherlands
Submission:August 20, 2023;Published:September 11, 2023
*Corresponding author: Kenrick Berend, Curacao Medical Centre, JHJ Hamelbergweg, Willemstad, Curaçao , Email: kenber2@me.com
How to cite this article: Berend K, Reijnen G. Fatal Manual Strangulation: A Brief Overview. J Forensic Sci & Criminal Inves. 2023; 17(5): 555973 DOI:10.19080/JFSCI.2023.17.555973.
Abstract
Up to ten percent of homicide deaths among women in North America involve strangulation and many of them involve domestic violence against women [1,2]. The covid pandemic catalyzed the incidence of domestic violence making it a worldwide problem. Most healthcare professionals will encounter domestic violence cases in their career, including manual strangulation. Strangulation related deaths are the result of applied external manual forces to the neck that may rapidly lead to death often after compression of cervical blood vessels, or tracheal occlusion. Symptoms and physical findings after manual strangulation pose a challenge for those without specific training. This paper gives an overview on aspects of fatal manual strangulation. New, largely unknown developments that may help to make a proper postmortem diagnosis are discussed in this paper.
Keywords: Strangulation; Manual; Postmortem evaluation; Autopsy; CT scan
Introduction
Prosecution in fatal manual strangulation cases may be extremely difficult as fatal manual strangulation may lack an obvious external trace in up to 40 percent of cases [1]. The statistics for domestic violence related strangulation cases, especially those that lead to homicides, are alarming [2]. Domestic violence is a worldwide problem, and most healthcare professionals will encounter victims of domestic violence [3]. Domestic violence is assumed to be underreported, but each year in the United States about 1.3 million women and 835,000 men are victims of physical assaults committed by an intimate partner. Moreover, 8% of men and 25% of women will be assaulted by an intimate partner in their lifetime. Annually, over 1,500 deaths in the United States are the result of domestic violence [3].
Domestic Homicide Victims
The covid pandemic catalyzed the incidence of domestic violence, creating an additional global problem, as stay-at-home policies to reduce the spread of the SARS-CoV-2 virus increased violence against women [4-8]. The term “intimate partner” includes actual and former spouses or dating partners. Intimate partner homicides make up almost 50 percent of all murders involving female victims in the United States [9]. It is estimated that there are about 20 physically assaults by an intimate partner committed per minute in the United States [10]. The Centers for Disease Control and Prevention report that about 1 in 6 homicide victims are killed by an intimate partner [11]. About 40% of homicide victims have been strangled by their offender within the previous year. Surviving victims of strangulation are eight times more likely to be a homicide victim thereafter [12]. Deaths due to strangulation account for 10% of violent deaths in North America [13], and of these, about ninety percent are related to domestic violence [14]. “Strangulation” is defined by Minnesota Criminal Statue §609.2247 as “intentionally impeding normal breathing or circulation of the blood by applying pressure on the throat or neck or by blocking the nose or mouth of another person” [15]. Manual strangulation is a overwhelming devastating form of domestic violence because no extra weapon is needed and the victim can be unconsciousness in seconds and dead within minutes [10,16]. According to one study, the lethality was 4.8% in 289 incidents in which an intimate partner strangled a woman, compared to 1.0% in 4,722 cases where other types of violence were used [17]. The human neck is vulnerable because of its small diameter and lack of bones protecting major vessels and trachea which are fundamental for life [18]. Strangulation injuries include hanging, manual strangulation, and ligature injuries when an object is used around the neck [19]. Postural strangulation occurs when pressure on the neck results in asphyxia caused by an unusual head down position often against an object. This is often associated with alcohol and drug intoxications [20]. Accidental self- strangulation and sex-associated asphyxias have been reported, but these cases remain a challenge for forensic medicine [21]. The most likely cause of death is either anoxia from occlusion of the arteries, venous occlusion of the major neck veins followed by congestion or anoxia, and occlusion of the trachea [1].
Disinformation by assassin
A realistic scenario for fatal manual strangulation is that the victim is reported by the attacker, claiming suicide or substance abuse. As no evident injury can be seen, an autopsy is performed with the suspicion of drug abuse, and the signs of strangulation may only be found if neck dissection is performed. In these cases, the suspect will not be examined properly, and crucial photographs and other evidence collection is not made [22]. The intent in cases of strangulation may be homicidal, suicidal, accidental, or autoerotic. Autoerotic hypoxia, which is practiced mostly by men, involves strangulation to increase orgasmic pleasure. These people usually hang themselves so that their feet can just reach the floor to ensure they will survive; however, consciousness may be lost within 10 seconds, leaving the victims incapable of releasing themselves [20,23,24]. The criminal justice system faces many legal challenges for successful prosecution in manual strangulation cases as merely fifteen percent of these victims present crucial evidence for manual strangulation [25]. Therefore, this review will focus on manual strangulation resulting in death where homicide may be extremely difficult to prove.
Pathophysiology of Strangulation
There are several anatomic neck structures that can cause morbidity and mortality in manual strangulation within minutes. These structures include the jugular veins which can resist merely 2 kg of manual force, the carotid arteries which collapse under 2.5 to 10 kg of pressure, the vertebral arteries which need 8 to 30 kg of pressure to collapse, and the trachea which will constrict completely under about 15 kg of pressure. The cricoid cartilage may fracture with 9 kg of force [19]. The grip strength with two hands in young women is about 28 kg and for men upto 45 kg. The “tip pinch” of thumb and other fingers is most used in manual strangulation from the front, using one hand. The grip strength with one hand is about half of that with two hands [26, 27]. However, these data may be incorrect in vivo as they are based on cadaver studies published in 1897 [28].
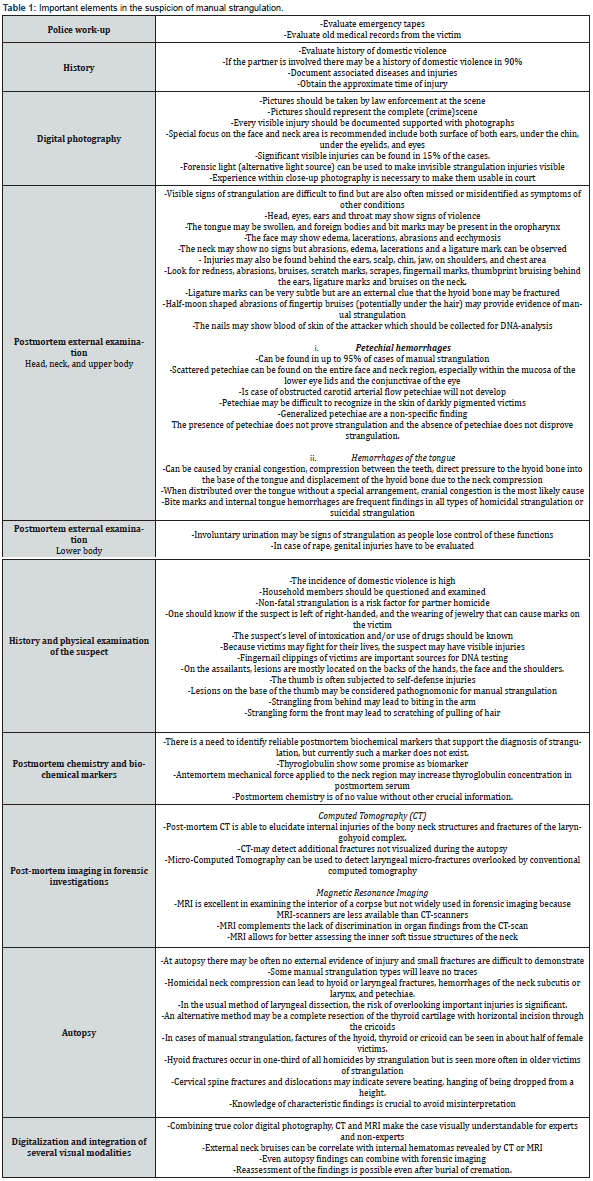
Manual strangulation options include strangulation with one or two hands constricting the larynx region facing the victim. From behind, the forearm or elbow is generally used to constrict the neck [29]. Several variables are involved in the fatal outcome: the quantity of pressure, the duration, the size of the area where the force is applied, and the location at the most vulnerable neck structures. The likelihood of a fatal outcome increases if the surface area is small when fingers are used, or if the duration of the force is longer. Even a relatively minor force by a small woman applied to a vital anatomic area may strangle a large man as has been showed by U.S. Army “close-range combative” training [22,30]. The likelihood of death increases with advanced age, heart disease, drug intoxications, or a vulnerable brain due to past injury [31]. About ten seconds of precise pressure on both carotid arteries may cause unconsciousness followed by brain death within five minutes [12]. Obviously, manual strangulation will primarily affect the jugular veins and/or carotid arteries. Pressure on the jugular veins with intact arterial flow prevents venous blood flow from the brain, resulting in congestion in the brain with unconsciousness, hypoventilation, and death within minutes. The fatal outcome is facilitated by cerebral hypoxia which will cause a loss of muscle tone. Once muscle tone is compromised, the pressure applied to carotid arteries or trachea will increase. Direct compression of the carotid arteries decreases cerebral blood flow which is a major cause of the loss of consciousness [19]. Choking is a technique used in martial arts [32] and in the past by police forces. In one study, twenty-four healthy police officers were studied during vascular neck restraint; carotid artery compression proved to be the most important cause of loss of consciousness, which started within 5-11 seconds [33,34]. It can be speculated that pressure on the carotid sinuses may cause a baroreceptor reflex with increased parasympathetic activation with sinus bradycardia or asystole together with the vasodepressor response, and hypotension due to decreased sympathetic activation will intensify hypoxic brain injury. Nevertheless, the risk of death caused by the cardioinhibitory reflex only is probably very small [35]. In recent decades, brochures, lists of questions, checklists and electronic applications have been developed to assist the investigation during cases of possible manual strangulation [22]. The Training Institute on Strangulation Prevention provides training, documentation, and electronic applications [36]. Evaluation of (suspected) strangulation is discussed below and outlined in table 1.
Police Work-up
Emergency (911) tapes should be evaluated to establish the suspect’s emotional state and statements. Additionally, the suspect’s cellular phones and computers should be confiscated and evaluated. Detailed police work-up is beyond the scope of this review. Evaluating old medical records from the victim can be vital in domestic violence prosecution because the recurrent rate of domestic violence is high and many survivors of manual strangulation do not provide this information to police authorities but may have discussed this with their physician [13,37].
History and physical examination of the suspect, household members/neighbors/bystanders
Because of the high incidence of domestic violence, household members should be questioned and examined. The decision whether a possible attacker has to be inspected, however, is made by police officers or the prosecutor. Non-fatal strangulation is an acknowledged risk factor for successive intimate partner homicide [17,38,39]. Therefore, certain information is required concerning domestic violence incidents in the past, pending criminal cases, and whether the suspect is currently on probation [22]. Detailed information should be obtained from the suspect, household members, neighbors, family or other relevant persons. One should know whether the suspect is left or righthanded and whether they wear jewelry, -in particular rings-that may have caused marks on the victim. The suspect’s level of intoxication and/or use of drugs and everything said must be electronically recorded [22]. Since victims often fight for their lives, defensive biting, scratching, or pulling of the suspect’s hair should be determined. Moreover, the suspect may be the only person with visible injuries. DNA evidence from bodily material, including fingernail clippings, blood, hair, or any other relevant material has become a major resource for solving crimes, in particular because DNA material can be stored for decades for later use [40-42]. The fingernail clippings of victims are important sources for forensic DNA testing, but although this foreign DNA may persist under fingernails for up to 48 hours, the signs of the scratched perpetrator are often no longer visible five hours after scratching [41].
Very often lesions on the assailants are located on the backs of the hands, the face, or the shoulders, but in many cases no injuries can be found. Because the thumb is the strongest part of the hand, it is often exposed to self-defense injuries. Specific lesions on the base of the thumb may be considered pathognomonic for manual strangulation [29]. Strangling from behind using a chokehold may lead to bitemarks on the hand or arm. Some bite areas may be found on biceps, forearms, shoulders, and upper chest [22]. The clothes of the suspect have to be examined by the forensic science laboratory. It remains imperative to investigate, photograph and interview all other household members and other possible bystanders. It is recommended that the forensic physician or forensic pathologist visit the place of incident to physically examine the suspect and his surroundings and to interview the household members and other bystanders.
History
History should be obtained from witnesses, family, friends, and professionals involved in the crime scene. If the partner is involved, there may be a history of domestic violence in up to 90 percent of the cases [12]; in other words, a victim of a prior strangulation is 800 percent more likely to become a homicide victim of that partner. In death investigations, a reasonable index of suspicion of a criminal offence is required to initiate further evaluation [22]. Associated diseases, injuries and substance ingestion need to be evaluated. Obtaining the approximate time of injury is also essential. The victim’s initial on-scene presentation and resuscitative efforts should be documented.
Digital Photography
In any case of possible violence, pictures are one of the most important tools. As many pictures as possible should be taken by law enforcement at the scene. These pictures should include all areas of the (possible) crime scene. Pictures should be taken of the location, the surroundings, people at the scene, important areas like stairs, any potential weapon, traces of blood, and in fact, everything [14]. The digital photographs should include distant, full-body photographs of the victim to identify the injuries. Additionally, multiple total body close-up photographs should be taken with – in case of suspected strangulation – special focus on the head and neck area at different angles. All injuries, no matter how minor, should be photographed for both victims and suspects [14]. Photos should be taken with and without a ruler placed next to the injury to document the size of the injuries [13] Specific areas to photograph include the ears, the area below the chin, the inner side of the lips and cheeks, the soft palate, the eyes and inside the eyelids [22]. Nevertheless, injuries are often too minor to photograph in manual strangulation cases. Significant visible injuries, like marks and bruises, can be found in only 15 percent of the cases [43]. Unfortunately, photographs may be unusable in court as physical evidence of strangulation because they show nonspecific marks or are too unclear or details are blurred by the flash. Police officers are therefore trained in close-up photography [12,43].
Alternative light sources
A forensic light source or “Alternative Light Source” is a special lamp that releases ultraviolet and infrared wavelengths. It filters the light to enhance the visualization by light interaction methods: fluorescence will glow, absorption will darken evidence, and diagonal lighting may reveal small particles. These light sources enhance inspection of the skin, by revealing bruises or other details like fingerprints, body fluids and hair, which are invisible with normal light sources. Especially soft-tissue injuries can sometimes be adequately pictured. One study of 172 strangulation surviving victims reported that no visible evidence of external injury was seen in 93% of the strangulation victims, but with the use of alternative light sources there were dermal injuries visible in 98% of that group [44]. However, there is no literature available on the postmortem use of an “Alternative Light Source”. And even if there are no lesions seen with an “Alternative Light Source”, one cannot simply conclude that there is no injury.
Cross-polarized photography and parallel-polarized light
In cross-polarized photography and parallel-polarized, light from two polarizers has to pass through polarizing filters at a special angle. This may enhance visualization of bite marks, burns, and strangulation marks [45,46]. The efficacy of this technique in manual strangulation needs to be proven.
Postmortem external examination at the crime scene and at autopsy. Head, neck and upper body
Visible signs of manual strangulation may be difficult to find, but also may be misinterpreted as symptoms of other conditions [14]. In one study of 100 cases of strangulation, police officers could not report injuries in 62 percent of the cases. Minor injuries, like redness or scratch marks, were reported in 22 percent of the cases [12]. Head, eyes, ears, nose, and throat may show marks of violence. Edema of the tongue or oropharynx may be seen and blood, vomit, or tissue or bite marks may be present in the oropharynx. The face may show edema, bruises and ecchymosis. At first glance the neck may look normal, but thorough search may show scratches, edema, cuts or ligature marks. Injuries may also be found behind the ears, the scalp, under the chin, inside the mouth, on arms, shoulders and chest. There should be special focus on redness, abrasions, bruises, scratch marks, scrapes, fingernail marks, thumb-print bruising (especially behind the ears), ligature marks, and bruises on the neck [22]. Ligature marks may be difficult to notice, as they look like the natural folds of the neck. Ligature marks may be an indication that the hyoid bone is fractured [13]. Ear bleeding is an infrequent finding in fatal strangulation [47]. Forearm strangulation around the neck, known as the “carotid restraint hold” can leave marks on the shoulders.
Three types of nail mark abrasions are often seen: impression marks, claw marks, and scratches [29]. These types occur separately or in combination. Impression marks are often small marks due to the cutting of fingernails into the skin. They may be curved, exclamation mark-like but oval, triangular, or rectangular skin injuries may be found. The injury is the result of the angle between the finger and the skin, the shape of the nail and the flexibility of the skin. Claw marks occur when the skin is damaged. Because most victims are women, their longer nails often cause more damage than scratches caused by attackers. Claw marks are parallel markings often in the front of the neck but sometimes scattered randomly. The length varies between a few mm and a few centimeters and is caused by the nails cutting the skin. Blood and/or fragments of skin often remain under the nail. Scratch marks may look like parallel reddening or superficial marks on the skin [12,29]. Vertical fingernail scratch marks on the victim may be caused by the victim’s own fingernails. The victim, most often a woman, may have struggled to release the stranglehold and thereby injured herself. However, these marks may be a combination of lesions caused by the victim and the assailant’s fingernails [13]. Small half-moon shaped abrasions on the back of the victim’s neck (potentially under the hair) may provide evidence that the suspect’s hands were wrapped around the neck. Head injuries may be seen if the victim’s head was pushed onto the floor or wall during strangulation. There may be swelling of the neck due to internal hemorrhage, caused by injury of the underlying neck structures. Subcutaneous edema or crepitus may be a sign of trauma to the lungs or fracture of the larynx [13]. Swelling of the victim’s neck, lips and/or tongue have to be described because these may not be photographed well. A pressure point from the suspect’s thumb(s) on the neck or from a ligature often does not appear right away or may appear as redness on the neck [48]. Fingertip bruises are often difficult to see. A single mark on the victim’s neck is generally caused by the assailant’s thumb [13], but these fingerprints on the skin of the victim’s neck are rare [49, 50]. Chin abrasions may occur if the victim lowered the chin to protect the neck [13]. The nails may contain blood or skin of the attacker and if so, this should be collected for DNA analysis.
Petechial hemorrhages
The detection of typical hemorrhages in manual strangulation demonstrates that the victim was still alive at that time [51]. Petechial hemorrhages may be discovered at or above the level of compression on the skin, palate, the eyes and in the brain [1]. Special attention should be paid to conjunctival or facial petechial hemorrhages as these petechiae can be found in up to 95 percent of cases of manual strangulation [29]. Multiple areas of scattered hemorrhages (petechiae) of about 1 mm in size can be found on the entire face and neck region, in particular under the lower eyelids and the conjunctivae of the eyes. Petechiae are caused by increased intravascular pressure due to a combination of impaired venous return in the presence of persistent arterial flow. Anatomical features and perhaps hypoxia also play an important role [21, 52]. Less force is needed to occlude the venae jugulars compared to the carotid arteries and in continued arterial flow the venous vessel wall will be injured, resulting in many small petechias. The hemorrhages are mostly found in regions where the vessel walls consist of one layer of endothelial cells. The conjunctiva consists of a single-layer wall covered by loose connective tissue, and it cannot endure much pressure and together with a weak vessel wall, petechiae will be first created in the conjunctival parts connected to the tarsus. Microscopic evaluation will reveal vessels with ruptured walls and congestion.
Empty capillaries are also seen because the damaged endothelial will release vaso-active substances which decreases the blood flow and limit influx into the vessels. These hemorrhages, due to the rupture of a vessel wall, also called rhexis hemorrhages, may arise within seconds [52,53]. When the force obstructs carotid arterial flow simultaneously with the jugular veins, petechiae will not develop [54]. One should be aware of the fact that petechiae may be difficult to identify in darker skin [49], and the question remains if one or a combination of these signs can be predictive of strangulation.
Many other causes of petechial hemorrhaging in the conjunctiva and other places have been reported in cases of external choking as well as in deaths due to natural causes, including sepsis and cardiac events, but also in other causes like electrocution, cerebral trauma, and intoxication. Petechiae in many parts of the body are mostly not specifically related to strangulation but caused by centrally elevated venous pressure in the chest. Increased intrathoracic or -abdominal pressure may produce congestion and may also be responsible for these petechiae in the head regions. Examples are epileptic seizures, asthma attack, sneezing, coughing, vomiting, giving birth, or other Valsalva maneuvers. In contrast, cardiopulmonary resuscitation does not seem to cause conjunctival petechiae [55]. Postmortem development of petechiae is also possible when the head is lying lower than the body [53,56]. In summary, the existence of petechiae does not prove strangulation, and the lack of petechiae does not exclude strangulation, but when found in combination with a history of strangulation, petechiae may be a sign of a deadly attack [20,21,52,53,55-58].
Hemorrhages of the tongue
Tongue hemorrhages can be caused by cranial congestion. This may be the result of compression by the teeth and neck compression that gives direct pressure on the hyoid bone into the base of the tongue by dislocation of the hyoid bone [59-62]. The bleeding must have happened while the victim was alive. Hemorrhages restricted to the margins of the tongue are mainly caused by the teeth. Central hemorrhages in the tongue are less common in forensic autopsy. When these bleedings are distributed over larger areas in the tongue without a special arrangement or if only a few small hemorrhages are present, cranial congestion is probably the cause [60,63]. Bite marks and internal tongue hemorrhages (often due to cranial congestion) are common findings in all types of homicidal and suicidal strangulation by ligature [60].
Lower body
Urinary sphincter incontinence resulting in an empty urinary bladder on catheterization may be an objective condition of danger to life. In one study urinary incontinence happened in only 4 of 79 survivors (5%) as compared with 22 of 37 victims of homicidal strangling (60%) [29]. Involuntary urination or defecation may be signs of manual strangulation as people lose control of these functions [1,25]. In the case of rape, genital injuries should be determined.
Postmortem chemistry and biochemical markers
Toxicology testing will ordinarily be done by medical examiners involved in homicide investigations [22]. Postmortem chemistry is essential in the forensic pathology routine and much progress has been made [64-69]. Biochemical markers often used include alcohol, drugs, markers of myocardial ischemia, inflammation, infection, sepsis, anaphylaxis, hormonal diseases, anemia, or hypoxia, and brain damage as circumstances of natural death have to be evaluated as well [66]. In some cases, the postmortem finding of drugs or intoxicants in bodily fluids have offered a tactical defense theory, to argue that death occurred by suicidal intoxication or overdose, and the assailant “merely” committed a physical assault, or even a consensual “asphyxophilic sexual injury” after which the victim supposedly committed suicide [22,70]. There is a need for reliable, postmortem biochemical markers of antemortem mechanical strangulation in fatal cases, but currently such a laboratory parameter does not exist. Thyroglobulin, however, shows some promise in this respect. The thyroid gland is situated in front of the neck and thyroglobulin is produced and stored only in the thyroid cells. Additionally, thyroglobulin is rarely secreted excessively in healthy individuals. The serum level is related to the size of the thyroid at 1 ng/mL per 1 g of thyroid mass. A thyroid gland weighs 20-25 g, so the reference range should be 20 to 25 ng/mL (20-25 μg/l) [71]. Consequently, mechanical force before death in the neck region may result in increased thyroglobulin levels in sampling sites close to the thyroid gland. In one postmortem study, thyroglobulin concentrations in serum from right heart blood in asphyxia cases (14 cases, including 10 suicidal hanging cases) ranged from 65 to 893 μg/l. In 11 out of these 14 cases, thyroglobulin levels were above 200 μg/l [68]. However, increased levels of thyroglobulin in cases without strangulation may exist but the authors of one study speculate that if the thyroglobulin concentration of both right heart blood and left heart blood are below 200 ng/ml, one can conclude that there was no antemortem strangulation causing damage to the thyroid tissue [72]. Nevertheless, postmortem chemistry is of no value without other crucial information including history, physical examination, radiological investigations, macroscopic findings, histology, and toxicology [72,73].
Post-mortem imaging in forensic investigations
Recently, modern imaging methods, like radiological crosssectional imaging, have become common forensic practice worldwide [74,75]. Although conventional radiography has been used in most countries in forensic imaging, the preferred method is multi-detector computed tomography, which allows 3D imaging of the total human body [74]. In addition, these imaging methods will help the pathologist decide on the optimal dissecting technique to avoid iatrogenic injuries [76]. In the case of manual strangulation, fractured laryngeal structures may be the only forensic finding. In the evaluation of strangulation deaths, post-mortem computed tomography is able to establish major injuries of the bony neck structures, in particular fractures of the laryngohyoid complex. Post-mortem computed tomography may be superior to autopsy-only examinations in the detection of small fractures. It may detect additional fractures that are difficult to visualize during autopsy. This is because the laryngohyoid complex has many muscles attached to it which cover a large part of the surfaces [77]. Fractures of the ventrolateral arch of the cricoid cartilage, along with hyoid and thyroid fractures or hemorrhages in these regions, should be looked for [51]. Hyoid fractures may be found in about 17 to 71 percent of fatal manual strangulation cases [1,78]. Unfortunately, the minimal slice thickness with multi-detector computed tomography is usually 0.6–1.2 mm and small tissue injuries may be missed or overlooked [79]. Micro-computed tomography is a new radiologic technique with a resolution of a few microns. It performs tridimensional investigations, showing micro-architecture which is very useful in detecting laryngeal micro-fractures overlooked by conventional computed tomography [79-81]. Unfortunately, the larynx has to be removed and scanned separately with this technique [51].
Magnetic resonance imaging (MRI)
Although MRI is a good technique to examine the internal corpse, it is limited because MRI scanners are less accessible than multi-detector computed tomography devices. MRI offers excellent soft-tissue evaluation, as it also distinguishes muscles, fat and neurological structures. It complements post-mortem computed tomography as MRI allows assessment of the inner soft- tissue structures of the neck, including vessels of the larynx [82-85]. Signs of manual strangulation include hemorrhage (e.g., subcutaneous, intramuscular, lymph node, submandibular glands), congestion, and also fractures of the laryngeal skeleton. However, small intramuscular hemorrhages of the sternohyoid muscle and substantial hemorrhage of the vocal cords may be missed by MRI. Compared to autopsy, postmortem MRI is almost as accurate in the detection of hemorrhages in the neck, but MRI is less accurate in the detection of fractures compared to postmortem CT and autopsy [51,84].
Autopsy
Despite the above-mentioned signs, even an autopsy with detailed evaluation may show no external evidence of injury in strangulation. If the manual grip has been held in one place until circulation stops, no extravasation signs will be found from the pressured vessels. A broad soft ligature or forearm would apply force over a wide region, leaving a minimum of traces [86]. Special attention should be paid to external injury to skin, macroscopic hyoid or laryngeal fractures, hemorrhages of neck subcutis or strap muscles and subconjunctival or facial petechiae. A triad of hemorrhage may be found: subepithelial laryngeal, intralaryngeal muscular, and intracartilaginous laryngeal [87]. The diagnosis of manual strangulation at autopsy may be difficult as small fractures of neck structures without dislocation are difficult to establish also because of the risk of iatrogenic injuries [79,80]. Maxeiner postulated that the common method of laryngeal dissection carries a substantial risk of overseeing significant so-called “hidden” laryngeal injuries. The preferred dissection method in his view is a complete resection of the thyroid cartilage. Inspection of the laryngeal joints and laryngeal muscles should be carried out with the tongue attached [88]. Using this procedure, incomplete fractures and incomplete or non-dislocated fractures of the thyroid and cricoid cartilage may be better evaluated. In cases of manual strangulation, fractures of the hyoid, thyroid, or cricoid cartilage can be seen in about half of female victims. The hyoid is a U-shaped bone and because of its shape it is easily fractured by strangulation. These fractures occur in one-third of all fatal strangulation cases. Fracture of the hyoid occurs commonly in older victims of strangulation because of decreased elasticity and increased ossification or fusion of the hyoid synchondroses occurs with increasing age. The hyoid is fused in older persons whereas the unfused hyoids are found in younger persons. The hyoid bone is ossified or fused in about 70% of all fractured hyoids, compared with only 30% of fusion in unfractured hyoid cases of strangulation. Fractured hyoids are also longer and more steeply sloped when compared with unfractured hyoids [89-92]. Autopsy may reveal laryngeal muscle bleedings, principally of the vocal folds in manual strangulation [88]. The aspect of injury of the tissues of the neck may differentiate strangulation from other traumatic injuries like hanging or blowing to the neck, or artifacts of postmortem disintegration. Ligature marks related to the used object will often be horizontal in ligature strangulation and diagonal in cases of hanging [20]. Other bruises and scrapes are equally important. In the autopsy investigation, every injury on the body may be significant. For example, contusions of the chest, abdomen and extremities become valuable proof to establish the pattern of abuse [22]. In some cases, efforts to conceal the real cause of death are made, to give the impression that death was caused by an accident [18]. Cervical spine fractures and dislocations may indicate severe beating, hanging or being dropped from a height. [20] Knowledge of characteristic findings is crucial [93]. In busy routine medicolegal practice, subtle homicidal strangulation may remain unnoticed by the pathologist in some cases [94].
It remains a challenge to prove that observations made postmortem are a sufficient basis to conclude that death was caused by manual strangulation. Obviously, a wrong statement may lead to unjustified conviction. Pollanen described five main pitfalls and artifacts encountered in the neck at autopsy [91]. First, development differences of the hyoid may contain a flexible synchondrotic joint simulating a fracture. A fractured hyoid bone, however, will show discontinuity of the bone itself with traces of bleeding. Microscopic analysis after decalcification of the hyoid bone may -in theory- be helpful in these cases, to make the call of strangulation and homicide on the basis of such a microscopic evaluation would be at present irresponsible and nonscientific. Second, triticeous cartilage may appear as a fracture of the superior cornu of the thyroid cartilage. These small pieces of fibrocartilage are present in the fibrous connective tissues adjoining the hyoid bone. In the absence of fractures, there will be no hemorrhage, and careful macroscopic examination or histological examination is required for a proper conclusion. Third, a so-called Prinsloo-Gordon hemorrhage is an important pitfall in the search of hemorrhage due to strangulation. The veins of the posterior pharynx are a widespread anastomosing arrangement of small vessels known as the laryngo-pharyngeal venous plexus. In the agonal period, there may be congestion of the veins cranial to the heart, leading to rupture.
Fourth, postmortem hypostatic hemorrhage will follow in the combination of a congested venous plexus by gravitational effects of postmortem stasis and a loss of vascular integrity of the venous plexus due to autolysis or decomposition. If sudden death occurs with the body in the head down position, postmortem hypostasis in the head may give hypostatic hemorrhages in the soft tissues of the neck, which resemble strangulation injuries [91,95]. Fifth, resuscitation-related neck injuries that give the impression of strangulation injuries include sternomastoid muscle perforation due to placement of a catheter in the internal jugular vein. Iatrogenic injuries include esophageal or pharyngeal injuries caused by traumatic intubation, barotrauma due to mechanical ventilation and laryngeal fracture due to cricoid pressure during resuscitation and surgical tracheostomy or cricothyroidotomy to establish an open airway [91,96]. Pulmonary defects may be the result of hypopharyngeal injuries with pneumothorax, pneumopericardium, aspiration and pulmonary edema [97]. The cause of pulmonary edema may be neurogenic or due to large intrathoracic pressure differences [12,98,99]. Neurogenic pulmonary edema may be the result of a sympathetic hemodynamic effect leading to increased pulmonary hydrostatic pressure [100-103].
Digitalization and Integration of Several Visual Modalities
Recent promising technological developments combine truecolor digital photography with computed tomography and/or magnetic resonance imaging to produce three-dimensional (3D) documentation using 3D scanners [75,104,105]. This technique reveals correlations between external injuries and internal injuries, improving the understanding of a case. In addition, these images make the case visually understandable for experts as well as non-experts like jurors and judges. For example, external neck bruises documented using a digital camera have to correlate with internal hematomas of internal soft-tissue injuries of the neck revealed by computed tomography or magnetic resonance imaging that may show how the crime scene evolved. This may also provide insight into the way the neck was strangled. Since the illustrations are based on the visualization of real data, they increase objectivity [104]. Other techniques are even able to combine autopsy findings with forensic imaging by computed tomography, magnetic resonance tomography and 3D surface scanning. This makes reassessment possible even after burial or cremation of the corpse, thus leading to better court rulings. With a surface-scanning unit, a 3D image is constructed using special software. Together with digital photography, a truecolor 3D surface reconstruction can be created, documenting structures less than 1 mm in size [106]. This may support cases of manual strangulation and documentation will be objective and reproducible. Obviously, not all causes of death can be revealed by this technique. For example, rhythm disturbances cannot be diagnosed, but this is also the case in autopsy. Post-mortem imaging will be increasingly used with many opportunities in forensic imaging.
Special Case Situations
Several circumstances at the crime scene may exist that can either divert the attention from manual strangulation or give the impression of an accidental death. Postmortem stabbing with a knife or the use of other weapons can draw attention away from important signs of strangulation [29]. Death from positional or postural asphyxia occurs when the person’s position restricts breathing [107-117]. Fatal positional asphyxia is usually accidental and is associated with drunkenness or other intoxications. The diagnosis of positional asphyxia depends largely on circumstantial evidence. The accident must be established and moving to another position must have been impossible. However, even in the presence of a fatal position, other potential underlying causes of death, such as trauma, intoxication or exhaustion should be excluded because positional asphyxia remains a rare cause of death [107,108,110,113,115,116].
Discussion
Manual strangulation is a major cause of violent deaths. Symptoms and physical signs of manual strangulation may be absent or difficult to detect without specific training. Therefore, a low index of suspicion to initiate further investigation may be justified. The criminal justice system faces many legal challenges with regard to holding perpetrators criminally responsible, as manual strangulation resulting in death can be extremely difficult to prove. Manual strangulation is a well-known form of intimate partner violence, and most victims are females strangled by a male domestic member. Standard police work-up should include a special focus on repeated violence of the suspect and digital photography of the crime scene. Post-mortem imaging has become a major tool as the diagnosis of strangulation at autopsy may be difficult to prove. Conjunctival or facial petechial hemorrhages can be found in up to 95 percent of cases of manual strangulation but are no proof of strangulation. If possible, postmortem biochemical markers that help to evaluate manual strangulation in fatal cases would be helpful. Due to recent promising technological developments, it is possible to combine true-color digital photography with computed tomography, magnetic resonance imaging and autopsy to produce three-dimensional crime scene documentation using 3-dimensional scanners. Nevertheless, potential evidence of strangulation may be overlooked or not accurately documented. The crime scene, circumstances and history are crucial, and a comprehensive evaluation of all aspects is essential for adequate prosecution.
Conclusion
There are several anatomic neck structures that, when collapsed, can cause morbidity and mortality in strangulation within minutes, often without a trace. Post-mortem computed tomography elucidates major injuries of the bony neck structures and may be excellent in the detection of minor fractures. Diagnosing manual strangulation at autopsy may not be easy for forensic pathologists, as small fractures of neck structures without dislocation are difficult to find and introduces the risk of iatrogenic defects.
Conflict of interest
there are no potential conflicts of interest of the authors. No research involving human participants and/or animals. Informed consent: not applicable.
References
- De Boos J (2019) Review article: non-fatal strangulation: Hidden injuries, hidden risks. Emerg Med Australas 31(3): 302-308.
- Jacob B, Cullen N, Haag H (2020) Assault by strangulation: sex differences in patient profile and subsequent readmissions. Canadian Journal of Public Health 111: 492-501.
- Huecker MRW, Smock (2018) Florida Domestic Violence. In: StatPearls. Treasure Island (FL), USA.
- Agüero JM (2021) COVID-19 and the rise of intimate partner violence. World Dev 137: 105217.
- van Gelder NE (2021) Professionals' views on working in the field of domestic violence and abuse during the first wave of COVID-19: a qualitative study in the Netherlands. BMC Health Serv Res 21(1): 624.
- Sofer D (2022) The Top News Stories of 2021: The Hidden Toll of COVID-19. Am J Nurs 122(1): 14.
- Saleem GT (2021) COVID-19-induced surge in the severity of gender-based violence might increase the risk for acquired brain injuries. SAGE Open Med 9: 20503121211050197.
- Nair VS, D Banerjee (2021) "Crisis Within the Walls": Rise of Intimate Partner Violence During the Pandemic, Indian Perspectives. Front Glob Womens Health 2: 614310.
- How widespread is intimate partner violence? (2007) NIJ (National Institute of Justice).
- Jennings A (2016) Domestic Assault by Strangulation and Recantation of Victims in the Criminal Court System. Thomas and S. Paul (Eds) St. Catherine University, Minnesota United States. 1-72.
- (2018) Intimate Partner Violence: Consequences, C.f.D. C.a.P. National Center for Injury Prevention and Control Atlanta, USA.
- Strack GBMG (1999) How to Improve Your Investigation and Prosecution of Strangulation Cases. The Prosecutor’s Perspective. Justiuic (Edt.), United States.
- Funk M, Schuppel NJ (2003) Strangulation injuries. WMJ 102(3): 41-45.
- Walters ME (2016) Domestic Violence prosecution handbook: a quick reference guide to practical prosecution. Oklahoma, United States.
- Domestic Assault by Strangulation (2022) Revisor of Statutes, State of Minnesota, United States.
- Strack B, Gwinn CG (2011) On the edge of homicide. Strangulation as a prelude. Criminal Justice 26.
- Glass N (2008) Non-fatal strangulation is an important risk factor for homicide of women. J Emerg Med 35(3): 329-335.
- Wakde SD (2014) A Conflicting Case of Strangulation: A Case Report. J Indian Acad Forensic Med 36(3): 327-328.
- Dunn RJ, Sukhija K, Lopez RA (2023) Strangulation Injuries. In: StatPearls, StatPearls Publishing, United States.
- Armstrong M Jr, Strack GB (2016) Recognition and Documentation of Strangulation Crimes: A Review. JAMA Otolaryngol Head Neck Surg 142(9): 891-897.
- Lambe A, Puschel K, Anders S (2009) Extensive petechiae in attempted self- strangulation. J Forensic Sci 54(1): 212-215.
- Gwinn C, Strack GB (2013) The investigation and prosecution of strangulation cases.
- Egge MK (2010) The choking game: a cause of unintentional strangulation. Pediatr Emerg Care 26(3): 206-208.
- Sauvageau A, Ambrosi C, Kelly S (2012) Three nonlethal ligature strangulations filmed by an autoerotic practitioner: comparison of early agonal responses in strangulation by ligature, hanging, and manual strangulation. Am J Forensic Med Pathol 33(4): 339-340.
- Jennings A (2016) Domestic Assault by Strangulation and Recantation of Victims in the Criminal Court System.
- Peters MJ (2011) Revised normative values for grip strength with the Jamar dynamometer. J Peripher Nerv Syst 16(1): 47-50.
- Mathiowetz V (1985) Grip and pinch strength: normative data for adults. Arch Phys Med Rehabil 66(2): 69-74.
- Brouardel, P (1897) La pendaison, la strangulation, la suffocation, la submersion. Bailliere et Fils, IB 36-45.
- Harm T, Rajs J (1981) Types of injuries and interrelated conditions of victims and assailants in attempted and homicidal strangulation. Forensic Sci Int 18(2): 101-123.
- Army US, Field Manual 3-25.150 “Combatives,” U.S. Army Field Training Manual, D.o.t.A. Headquarters, Editor: Washington, D.C, United States.
- Reay DT JW Eisele (1982) Deaths from law enforcement neck holds. Am J Forens Med Pathol 3(3): 253-258.
- Buse GJ (2006) No holds barred sport fighting: a 10-year review of mixed martial arts competition. Br J Sports Med 40: 169-172.
- Mitchell JR (2012) Mechanism of loss of consciousness during vascular neck restraint. J Appl Physiol 112(3): 396-402.
- Reay DT, Holloway GA Jr (1982) Changes in carotid blood flow produced by neck compression. Am J Forensic Med Pathol 3(3): 199-202.
- Leth PM (2016) The risk of death caused by cardioinhibitory reflex mechanism is very small. Ugeskr Laeger. 178(8): V08150644.
- Prevention, T.I.o.S. Strangulation (2022).
- Miller, E, B. McCaw (2019) Intimate Partner Violence. N Engl J Med 380(9): 850- 857.
- Campbell J, Messing JT (2017) Assessing dangerousness: domestic violence offenders and child abusers. (3rd), Springer Publishing Company, LLC, United States, pp. 220.
- Laughon K (2008) Revision of the Abuse Assessment Screen to address nonlethal strangulation. J Obstet Gynecol Neonatal Nurs 37(4): 502-527.
- Kettner M (2015) IPV--bridging the juridical gap between scratches and DNA detection under fingernails of cohabitating partners. Forensic Sci Int Genet 14: 110-115.
- Iuvaro A (2018) Male DNA under female fingernails after scratching: transfer and persistence evaluation by RT-PCR analysis and Y-STR typing. Int J Legal Med 132(6): 1603-1609.
- Matte M (2012) Prevalence and persistence of foreign DNA beneath fingernails. Forensic Sci Int Genet 6(2): 236-243.
- Strack GB, McClane GE, Hawley D (2001) A review of 300 attempted strangulation cases. Part I: criminal legal issues. J Emerg Med 21(3): 303-309.
- Holbrook DS, Jackson MC (2013) Use of an alternative light source to assess strangulation victims. J Forensic Nurs 9(3): 140-145.
- Marsh N (2014) Forensic Photograph. A practitioner's guide. West Sussex, JohnWiley & Sons, Ltd, United Kingdom.
- Hanlon KL (2018) Cross-polarised and parallel-polarised light: Viewing and photography for examination and documentation of biological materials in medicine and forensics. J Vis Commun Med 41(1): 3-8.
- Miles SH (2009) Autopsy findings in asphyxia in medical bed rails. Am J Forensic Med Pathol 30(3): 256-261.
- Koenig KL (2017) San Diego County Strangulation protocol, S. Approved by the Chiefs of Police, San Diego, D.A.a.S.D.C.A. San Diego, United States.
- Hawley DA, McClane GE, Strack GB (2001) A review of 300 attempted strangulation cases Part III: injuries in fatal cases. J Emerg Med 21(3): 317-322.
- Hammer HJ (1980) Methods for detection of latent fingerprints from human skin. Forens Sci Intl 16: 35-41.
- Gascho D (2019) Relevant findings on postmortem CT and postmortem MRI in hanging, ligature strangulation and manual strangulation and their additional value compared to autopsy - a systematic review. Forensic Sci Med Pathol 15(1): 84-92.
- Ely SF, Hirsch CF (2000) Asphyxial deaths and petechiae: a review. J Forensic Sci 45(6): 1274-1277.
- Lasczkowski G (2005) Pathogenesis of conjunctival petechiae. Forensic Sci Int 147(1): 25-29.
- Duband S (2009) Ear bleeding: A sign not to be underestimated in cases of strangulation. Am J Forensic Med Pathol 30(2): 175-176.
- Maxeiner HR, Jekat (2010) Resuscitation and conjunctival petechial hemorrhages. J Forensic Leg Med 17(2): 87-91.
- Schroder AS (2012) Post-mortem development of conjunctival petechiae following temporary prone position. Forensic Sci Int 223(1-3): e53-e55.
- Zivkovic VS, Nikolic (2018) Petechial haemorrhages as a consequence of very short- term strangulation during suicidal fall from a height: Case reconstruction. Med Sci Law 58(1): 62-66.
- Asamura H (2010) Unusual body posture after death leading to signs of strangulation. Am J Forensic Med Pathol 31(2): 195-197.
- Simonsen J (1989) Discussion of "An Unusual, Deep Lingual Hemorrhage as a Consequence of Ligature Strangulation". J Forensic Sci 34(3): 529-531.
- Bockholdt BH, Maxeiner (2002) Hemorrhages of the tongue in the postmortem diagnostics of strangulation. Forensic Sci Int 126(3): 214-220.
- Ishikawa N (2018) The relationship between the intramuscular bleeding of the tongue and cause of death. J Forensic Leg Med 59: 50-55.
- Sperry K (1988) An unusual, deep lingual hemorrhage as a consequence of ligature strangulation. J Forensic Sci 33(3): 806-811.
- Suyama H (1982) Significance of hemorrhages in central parts of the tongue found in medicolegal autopsy. J Forensic Sci int 20: 265-268.
- Chandrakanth HV (2013) Postmortem vitreous chemistry--an evaluation of sodium, potassium, and chloride levels in estimation of time since death (during the first 36 h after death). J Forensic Leg Med 20(4): 211-216.
- Fancher JP (2017) An evaluation of soil chemistry in human cadaver decomposition islands: Potential for estimating postmortem interval (PMI). Forensic Sci Int 279: 130-139.
- Palmiere, Mangin CP (2012) Postmortem chemistry update part II. Int J Legal Med 126(2): 199-215.
- Palmiere, Mangin CP (2012) Postmortem chemistry update part I. Int J Legal Med 126(2): 187-198.
- Palmiere (2018) Postmortem biochemical investigation results in situations of fatal mechanical compression of the neck region. Leg Med (Tokyo) 30: 59-63.
- Vass AA (2002) Decomposition chemistry of human remains: a new methodology for determining the postmortem interval. J Forensic Sci 47(3): 542-553.
- Dettling A, Haffner, HT, Wehner HD (2009) The evaluation of doxepin concentrations in postmortem blood as optional cause of death. Am J Forensic Med Pathol 30(3): 298-300.
- Idrasena BSH (2017) Use of thyroglobulin as a tumour marker. World J Biol Chem 8(1): 81-5.
- Hayakawa A (2014) Unreliability of the use of thyroglobulin concentration in postmortem blood samples in forensic diagnosis. Leg Med (Tokyo) 16(3): 164-167.
- Takaso M (2018) Value of the serum thyroglobulin level for diagnosing neck compression in postmortem cases. J Forensic Leg Med 58: 126-129.
- Grabherr S (2016) Post-mortem imaging in forensic investigations: current utility, limitations, and ongoing developments. Research and Reports in Forensic Medical Science 6: 25-37.
- Grabherr S (2017) Modern post-mortem imaging: an update on recent developments. Forensic Sci Res 2(2): 52-64.
- Maiese A (2014) When the hidden features become evident: the usefulness of PMCT in a strangulation-related death. Leg Med (Tokyo) 16(6): 364-366.
- Decker LA (2018) The Role of Postmortem Computed Tomography in the Evaluation of Strangulation Deaths. J Forensic Sci 63(5): 1401-1405.
- Ubelaker DH (1992) Hyoid fracture and strangulation. J Forensic Sci 37(5): 1216-1222.
- Kettner M (2014) Analysis of laryngeal fractures in decomposed bodies using microfocus computed tomography (mfCT). Forensic Sci Med Pathol 10(4): 607-612.
- Fais P (2016) Micro computed tomography features of laryngeal fractures in a case of fatal manual strangulation. Leg Med (Tokyo) 18: 85-89.
- Longato S (2015) Post-mortem interval estimation of human skeletal remains by micro-computed tomography, mid-infrared microscopic imaging and energy dispersive X- ray mapping. Anal Methods 7(7): 2917-2927.
- Christe A (2010) Can MRI of the neck compete with clinical findings in assessing danger to life for survivors of manual strangulation? A statistical analysis. Leg Med (Tokyo)12(5): 228-232.
- Christe A (2009) Life-threatening versus non-life-threatening manual strangulation: are there appropriate criteria for MR imaging of the neck? Eur Radiol 19(8): 1882-1889.
- Yen K (2005) Strangulation signs: initial correlation of MRI, MSCT, and forensic neck findings. J Magn Reson Imaging 22(4): 501-510.
- Yen K (2007) Clinical forensic radiology in strangulation victims: forensic expertise based on magnetic resonance imaging (MRI) findings. Int J Legal Med 121(2): 115-123.
- Camps FE, Hunt AC (1959) Pressure on the neck. Y For Med 6: 116-135.
- Pollanen MS (2001) Subtle fatal manual neck compression. Med Sci Law 41(2): 135-140.
- Maxeiner H (1998) "Hidden" laryngeal injuries in homicidal strangulation: how to detect and interpret these findings. J Forensic Sci 43(4): 784-791.
- Pollanen MS, Chiasson DA (1996) Fracture of the hyoid bone in strangulation: comparison of fractured and unfractured hyoids from victims of strangulation. J Forensic Sci 41(1): 110-113.
- Pollanen MS, Bulger B, Chiasson DA (1995) The location of hyoid fractures in strangulation revealed by xeroradiography. J Forensic Sci 40(2): 303-305.
- Pollanen MS (2016) Pitfalls and Artifacts in the Neck at Autopsy. Acad Forensic Pathol 6(1): 45-62.
- Rayamane AP (2015) Pattern of Internal Neck Injuries in Strangulation Deaths with special reference to Laryngeal Fractures. J Indian Acad Forensic Med 37(2): 179-182.
- Cole SF, Massachusetts Continuing Legal Education Inc (1996) Child custody and domestic violence: strategies for advocacy when children witness violence. Massachusetts Continuing Legal Education, Boston, Massachusetts, USA, pp. 266.
- Sadler DW (1994) Concealed homicidal strangulation first discovered at necropsy. J Clin Pathol 47(7): 679-680.
- Bockholdt B, Maxeiner H, Hegenbarth W (2005) Factors and circumstances influencing the development of hemorrhages in livor mortis. Forensic Sci Int 149(2-3): 133-137.
- Stoppacher R, Teggatz JR, Jentzen JM (2004) Esophageal and pharyngeal injuries associated with the use of the esophageal-tracheal combitube. J Forensic Sci 49(3): 586- 591.
- Giger R (2004) Pneumopericardium after manual strangulation. Am J Med 116(11): 788-790.
- Grellner WB, Madea (1995) The value of various lung changes in death by strangulation. Arch Kriminol 196(1-2): 38-45.
- Kita TY Furuya (1989) Mechanisms of the pulmonary congestion in ligature strangulation (VIII). Igaku Kenkyu 59(3): 83-89.
- Bonello M, Pullicino R, Larner AJ (2017) Acute pulmonary oedema: not always cardiogenic. J R Coll Physicians Edinb 47(1): 57-59.
- Al-Dhahir MA, Sharma S (2019) Neurogenic Pulmonary Edema, in StatPearls. Treasure Island (FL).
- van Bussel B, Peters N, Aries M (2018) Neurogenic pulmonary oedema. BMJ Case Rep.
- Finsterer J (2019) Neurological Perspectives of Neurogenic Pulmonary Edema. Eur Neurol 81(1-2): 94-101.
- Bornik A (2018) Integrated computer-aided forensic case analysis, presentation, and documentation based on multimodal 3D data. Forensic Sci Int 287: 12-24.
- Campana L, (2016) 3D documentation and visualization of external injury findings by integration of simple photography in CT/MRI data sets (IprojeCT). Int J Legal Med 130(3): 787-797.
- Bolliger SA, Thali MJ (2015) Imaging and virtual autopsy: looking back and forward. Philos Trans R Soc Lond B Biol Sci 370(1674).
- Byard RW, Wick R, JD Gilbert (2008) Conditions and circumstances predisposing to death from positional asphyxia in adults. J Forensic Leg Med 15(7): 415-459.
- Padosch SA (2005) Death due to positional asphyxia under severe alcoholisation: pathophysiologic and forensic considerations. Forensic Sci Int 149(1): 67-73.
- Palmiere CP, Mangin (2012) Diabetic ketoacidosis or positional asphyxia? Leg Med (Tokyo) 14(4): 219-220.
- Hayashi T (2012) Fatal positional asphyxia. Forensic Sci Med Pathol 8(4): 470-472.
- Boghossian ES, Tambuscio, Sauvageau A (2010) Nonchemical suffocation deaths in forensic setting: a 6-year retrospective study of environmental suffocation, smothering, choking, and traumatic/positional asphyxia. J Forensic Sci 55(3): 646-651.
- Karch SB, Brave MA, Kroll MW (2016) On positional asphyxia and death in custody. Med Sci Law 56(1): 74-75.
- Chen L (2015) An overhung mute suspect died during restraint - Is this a case of positional asphyxia? J Forensic Leg Med 33: 98-100.
- Fernando T, Byard RW (2013) Positional asphyxia without active restraint following an assault. J Forensic Sci 58(6): 1633-1635.
- Chaudhari VA, Ghodake DG, Kharat RD (2016) Positional Asphyxia: Death Due to Unusual Head-Down Position in a Narrow Space. Am J Forensic Med Pathol 37(2): 51- 53.
- Chmieliauskas S (2018) Sudden deaths from positional asphyxia: A case report. Medicine (Baltimore) 97(24): e11041.
- Benomran FA, Hassan AI (2011) An unusual accidental death from positional asphyxia. Am J Forensic Med Pathol 32(1): 31-34.






























